Insights on Allergic Rhinitis Management from a Northern Cyprus Perspective and Evaluation of the Impact of Pharmacist-Led Educational Intervention on Patients’ Outcomes
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Participants
2.2. Research Instruments
2.2.1. Development of the Questionnaires
2.2.2. Assessment Tools for Intervention Study
2.3. Data Collection
2.4. Ethical Considerations
2.5. Statistical Analysis
3. Results
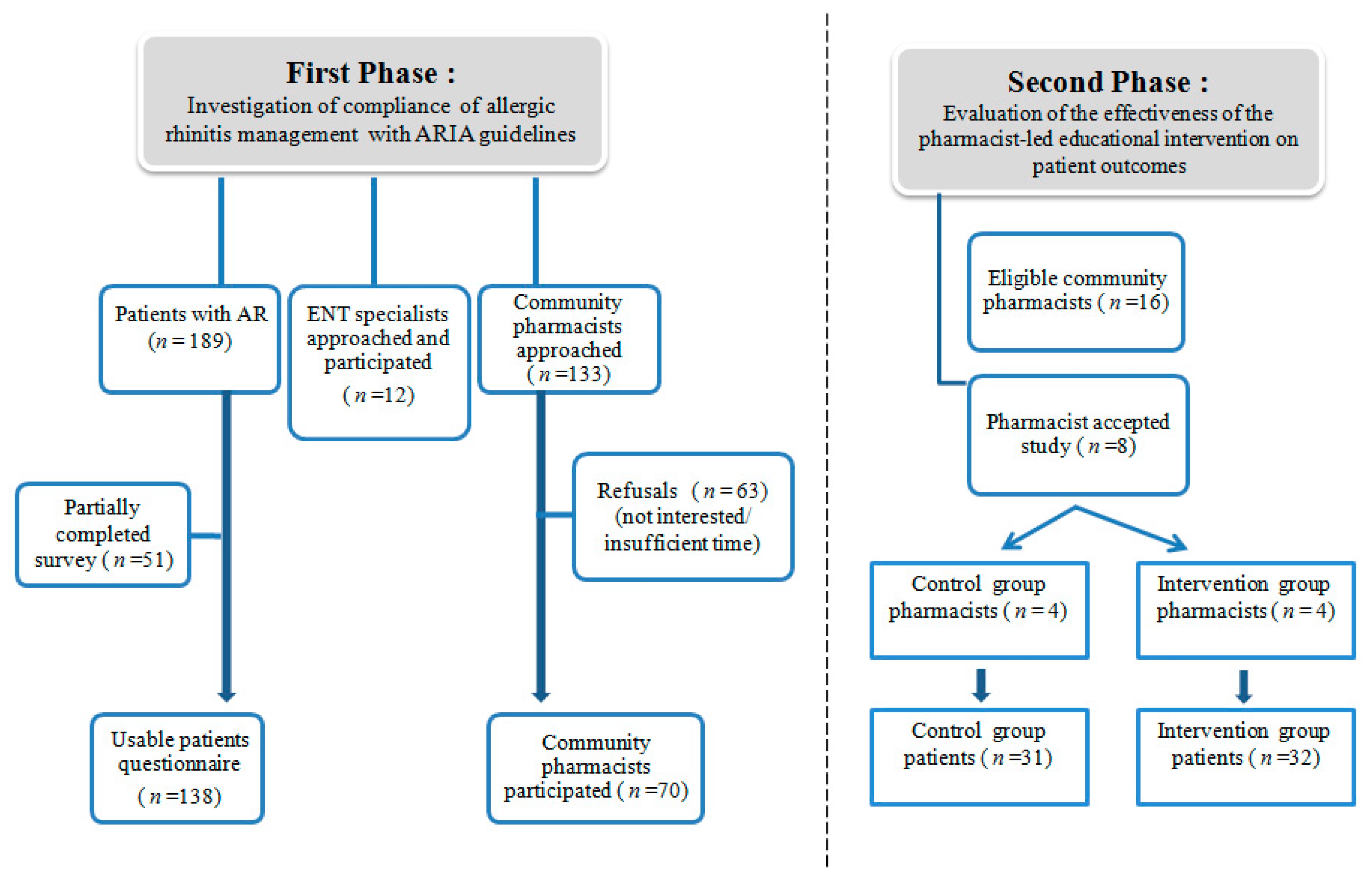
3.1. Response Rate and Participant Characteristics
3.2. First Phase Allergic Rhinitis (AR) Experiences and Management Questionnaire Responses
3.2.1. Data on Patients’ Experiences
3.2.2. Data on Pharmacists’ Practices
3.2.3. Data on Ear, Nose and Throat (ENT) Specialist’s Practice
3.3. Second Phase Controlled Interventional Study Data
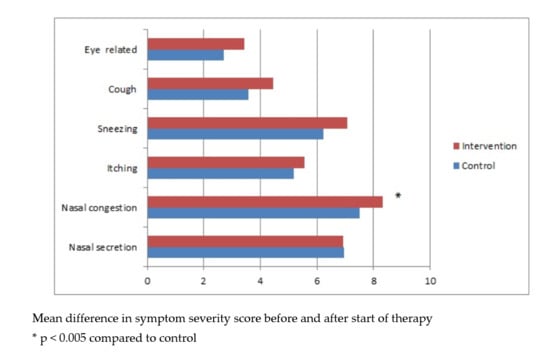
3.3.1. Patient Rated Symptom Severity
3.3.2. Quality of Life Measurements
4. Discussion
Limitations of the Study
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- May, J.R.; Dolen, W.K. Management of Allergic Rhinitis: A Review for the Community Pharmacist. Clin. Ther. 2017, 39, 2410–2419. [Google Scholar] [CrossRef] [PubMed]
- Bauchau, V.; Durham, S. Prevalence and rate of diagnosis of allergic rhinitis in Europe. Eur. Respir. J. 2004, 24, 758–764. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gerber, M.; Brignoli, R.; Canevascini, M.; Wuthrich, B. Epidemiological survey in hay fever patients. Allergy 1995, 50, 161–163. [Google Scholar]
- Tripathi, A.; Patterson, R. Impact of allergic rhinitis treatment on quality of life. Pharmacoeconomics 2001, 19, 891–899. [Google Scholar] [CrossRef] [PubMed]
- Simons, F.E. Learning impairment and allergic rhinitis. Allergy Asthma Proc. 1996, 17, 185–189. [Google Scholar] [CrossRef] [PubMed]
- Blanc, P.D.; Trupin, L.; Eisner, M.; Earnest, G.; Katz, P.P.; Israel, L.; Yelin, E.H. The work impact of asthma and rhinitis. Findings from a population-based survey. J. Clin. Epidemiol. 2001, 54, 610–618. [Google Scholar] [CrossRef]
- Bousquet, J.; Van Cauwenberge, P.; Khaltaev, N. ARIA in the pharmacy: Management of allergic rhinitis symptoms in the pharmacy. Allergy 2004, 59, 373–387. [Google Scholar]
- Van Cauwenberge, P.; Bachert, C.; Passalacqua, G.; Bousquet, J.; Canonica, G.W.; Durham, S.R.; Fokkens, W.J.; Howarth, P.H.; Lund, V.; Malling, H.J.; et al. Consensus statement on the treatment of allergic rhinitis. Allergy 2000, 55, 116–134. [Google Scholar] [CrossRef] [PubMed]
- Georgalas, C.; Vlastos, I.; Picavet, V.; van Drunen, C.; Garas, G.; Prokopakis, E. Is chronic rhinosinusitis related to allergic rhinitis in adults and children? Applying epidemiological guidelines for causation. Allergy 2014, 69, 828–833. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bousquet, J.; Annesi-Maesano, I.; Carat, F.; Leger, D.; Rugina, M.; Pribil, C.; El Hasnaoui, A.; Chanal, I. Characteristics of intermittent and persistent allergic rhinitis: DREAMS study group. Clin. Exp. Allergy 2005, 35, 728–732. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lourenço, O.; Calado, S.; Sá-Sousa, A.; Fonseca, J. Evaluation of allergic rhinitis and asthma control in a Portuguese community pharmacy setting. J. Manag. Care Pharm. 2014, 20, 513–522. [Google Scholar] [CrossRef] [PubMed]
- Pawanker, R.; Canonica, G.W.; Holgate, S.T.; Lockey, R.F. (Eds.) World Allergy Organization (WAO) White Book on Allergy 2011–2020; World Allergy Organisation: Milwaukee, WI, USA, 2011; pp. 1–238. [Google Scholar]
- Bousquet, J.; Khaltaev, N.; Cruz, A.A.; Denburg, J.; Fokkens, W.J.; Togias, A.; Zuberbier, T.; Baena-Cagnani, C.E.; Canonica, G.W.; van Weel, C.; et al. Allergic Rhinitis and its Impact on Asthma (ARIA) 2008 update (in collaboration with the World Health Organization, GA(2)LEN and AllerGen). Allergy 2008, 63 (Suppl. 86), 8–160. [Google Scholar] [CrossRef] [PubMed]
- Lombardi, C.; Musicco, E.; Rastrelli, F.; Bettoncelli, G.; Passalacqua, G.; Canonica, G.W. The patient with rhinitis in the pharmacy. A cross-sectional study in real life. Asthma Res. Pract. 2015, 1, 4. [Google Scholar] [CrossRef] [PubMed]
- Smith, L.; Nguyen, T.; Seeto, C.; Saini, B.; Brown, L. The role of non-clinicians in a goal setting model for the management of allergic rhinitis in community pharmacy settings. Patient Educ. Couns. 2011, 85, e26–e32. [Google Scholar] [CrossRef] [PubMed]
- Baiardini, I.; Braido, F.; Tarantini, F.; Porcu, A.; Bonini, S.; Bousquet, P.J.; Zuberbier, T.; Demoly, P.; Canonica, G.W. ARIA-suggested drugs for allergic rhinitis: What impact on quality of life? A GA2LEN review. Allergy 2008, 63, 660–669. [Google Scholar] [CrossRef] [PubMed]
- Todorova, A.; Tsvetkova, A.; Mihaylova, S.; Andreevska, K.; Kondova, A.; Arnaoudova, M. The impact of pharmaceutical care on improving the quality of life in patients with allergic rhinitis. CBU Int. Conf. Proc. 2017, 5, 1022–1027. [Google Scholar] [CrossRef]
- Brozek, J.L.; Bousquet, J.; Baena-Cagnani, C.E.; Bonini, S.; Canonica, G.W.; Casale, T.B.; van Wijk, R.G.; Ohta, K.; Zuberbier, T.; Schünemann, H.J. Grading of Recommendations Assessment, Development and Evaluation Working Group. Allergic Rhinitis and its Impact on Asthma (ARIA) guidelines: 2010 revision. J. Allergy Clin. Immunol. 2010, 126, 466–476. [Google Scholar] [CrossRef] [PubMed]
- Seidman, M.D.; Gurgel, R.K.; Lin, S.Y.; Schwartz, S.R.; Baroody, F.M.; Bonner, J.R.; Dawson, D.E.; Dykewicz, M.S.; Hackell, J.M.; Han, J.K.; et al. Clinical practice guideline: Allergic rhinitis. Otolaryngol. Head Neck Surg. 2015, 152 (Suppl. 1), S1–S43. [Google Scholar] [CrossRef] [PubMed]
- Levin, M.E. Education for allergic rhinitis:original research. Curr. Allergy Clin. Immunol. 2014, 27, 101–106. [Google Scholar]
- ARIA Pocket Guide for Pharmacists. 2003. Available online: http://www.whiar.org/docs/ARIA_Pharm_PG.pdf (accessed on 21 November 2016).
- Natt, R.S.; Karkos, P.D.; Natt, D.K.; Theochari, E.G.; Karkanevatos, A. Treatment trends in allergic rhinitis and asthma: A British ENT survey. BMC Ear Nose Throat Disord. 2011, 11, 3. [Google Scholar] [CrossRef] [PubMed]
- Canonica, G.W.; Triggiani, M.; Senna, G. 360 degree perspective on allergic rhinitis management in Italy: A survey of GPs, pharmacists and patients. Clin. Mol. Allergy 2015, 13, 25. [Google Scholar] [CrossRef] [PubMed]
- Demoly, P.; Calderón, M.A.; Casale, T.; Annesi-Maesano, I.; Braun, J.J.; Delaisi, B.; Haddad, T.; Malard, O.; Trébuchon, F.; Serrano, E. Assessment of disease control in allergic rhinitis. Clin. Transl. Allergy 2013, 3, 7. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Juniper, E.F.; Thompson, A.K.; Ferrie, P.J.; Roberts, J.N. Development and validation of the mini Rhinoconjunctivitis Quality of Life Questionnaire. Clin. Exp. Allergy 2000, 30, 132–140. [Google Scholar] [CrossRef] [PubMed]
- De Marco, R.; Cappa, V.; Accordini, S.; Rava, M.; Antonicelli, L.; Bortolami, O.; Braggion, M.; Bugiani, M.; Casali, L.; Cazzoletti, L.; et al. Trends in the prevalence of asthma and allergic rhinitis in Italy between 1991 and 2010. Eur. Respir. J. 2012, 39, 883–892. [Google Scholar] [CrossRef] [PubMed]
- Recto, M.T.; Gabriel, M.T.; Kulthanan, K.; Tantilipikorn, P.; Aw, D.C.; Lee, T.H.; Chwen, C.C.; Mutusamy, S.; Hao, N.T.; Quang, V.T.; et al. Selecting optimal second-generation antihistamines for allergic rhinitis and urticaria in Asia. Clin. Mol. Allergy 2017, 15, 19. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Prepageran, N.; Wang, D.Y.; Nair, G.; Maurer, M. The status quo and unmet needs in the management of allergic rhinitis and chronic rhinosinusitis: A Malaysian perspective. Asia Pac. Allergy 2014, 4, 142–148. [Google Scholar] [CrossRef] [PubMed]
- Tan, R.; Cvetkovski, B.; Kritikos, V.; Price, D.; Yan, K.; Smith, P.; Bosnic-Anticevich, S. Identifying the hidden burden of allergic rhinitis (AR) in community pharmacy: A global phenomenon. Asthma Res. Pract. 2017, 3, 8. [Google Scholar] [CrossRef] [PubMed]
- Bousquet, J.; Reid, J.; van Weel, C.; BaenaCagnani, C.; Canonica, G.W.; Demoly, P.; Denburg, J.; Fokkens, W.J.; Grouse, L.; Mullol, K.; et al. Allergic rhinitis management pocket reference 2008. Allergy 2008, 63, 990–996. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bridgeman, M.B. Overcoming barriers to intranasal corticosteroid use in patients with uncontrolled allergic rhinitis. Integr. Pharm. Res. Pract. 2017, 6, 109. [Google Scholar] [CrossRef] [PubMed]
- O’Connor, J.; Seeto, C.; Saini, B.; BosnicAnticevich, S.; Krass, I.; Armour, C.; Smith, L. Health care professional versus patient goal setting in intermittent allergic rhinitis. Patient Educ. Couns. 2008, 70, 111–117. [Google Scholar] [CrossRef] [PubMed]
- Hammersley, V.S.; Elton, R.A.; Walker, S.; Hansen, C.H.; Sheikh, A. Adolescent seasonal allergic rhinitis and the impact of health-care professional training: Cluster randomized controlled trial of a complex intervention in primary care. NPJ Prim. Care Respir. Med. 2014, 24, 14012. [Google Scholar] [CrossRef] [PubMed]
- Gani, F.; Pozzi, E.; Crivearo, M.A.; Senna, G.; Landi, M.; Lombardi, C.; Canonica, G.W.; Passalacqua, G. The role of patient training in the management of seasonal rhinitis and asthma: Clinical implications. Allergy 2001, 56, 65–68. [Google Scholar] [CrossRef] [PubMed]
| Characteristic | Value |
|---|---|
| Key AR symptoms for physician diagnosis, n (%) | |
| Nasal congestion | 7 (58.3) |
| Rhinorrhea | 3 (25) |
| Sneezing | 1 (8.3) |
| Nasal itching | 2 (16.7) |
| Ocular symptoms | 1 (8.3) |
| Cough | 1 (8.3) |
| Most bothersome symptom motivating patients to visit the physician, n (%) | |
| Nasal congestion | 133 (96.4) |
| Sneezing | 116 (84.1) |
| Nasal itching | 112 (81.2) |
| Rhinorrhea | 121 (87.7) |
| Cough | 118 (85.5) |
| Ocular symptoms | 110 (79.7) |
| Chief symptoms that made pharmacist suspect AR, n (%) | |
| Nasal congestion | 29 (41.4) |
| Rhinorrhea | 30 (42.9) |
| Sneezing | 21 (30) |
| Nasal itching | 14 (20) |
| Cough | 9 (12.9) |
| Ocular symptoms | 10 (14.3) |
| Causes of symptoms according to patients, n (%) | |
| Animals | 9 (6.5) |
| Plants | 44 (31.9) |
| Seasonal changes | 63 (45.7) |
| Chemicals | 21(15.2) |
| Dust | 65 (41.7) |
| Others | 15 (10.9) |
| Impact on patients’ QoL, n (%) | |
| Impairment of daily activities | 24 (17.4) |
| Sleep disturbances | 23 (16.7) |
| Impairment of work or school | 12 (8.7) |
| Troublesome symptoms | 79 (57.2) |
| None | 0 (0) |
| Pharmacists | ENT Specialists | |||
|---|---|---|---|---|
| Medication | Median (IQR) | N (%) | Median (IQR) | N (%) |
| Oral antihistamine | 3.50 (1) | 35 (50) | 3 (0) | 8 (66.7) |
| Intranasal antihistamine | 2 (2) | 26 (37.1) | 1 (1) | 5 (41.7) |
| INCs | 1 (2) | 29 (41.4) | 4 (1) | 9 (75) |
| Oral corticosteroids | 0 (0) | 55 (78.6) | 1 (1) | 8 (66.7) |
| Oral decongestants | 2 (2) | 25 (35.7) | 1 (2) | 7 (58.3) |
| Intranasal decongestants | 2 (1) | 28 (40) | 1.50 (1) | 5 (41.7) |
| Anticholinergics | 0 (0) | 55 (78.6) | 1 (2) | 5 (41.7) |
| LTRAs | 0 (0) | 56 (80) | 0.50 (2) | 6 (50) |
| Nasal saline | 3 (1) | 22 (31.4) | 1(1) | 6 (50) |
| Symptom | Group | Baseline (V1) Median Score (IQR) | Final Visit (V2) Median Score (IQR) | Within Group Change Scores p-Value # | Between Group Change scores p-Value ^ |
|---|---|---|---|---|---|
| Nasal secretions | G1 | 8 (4) | 0 (0) | <0.05 | 0.23 |
| G2 | 8 (4) | 0 (0) | |||
| Nasal congestions | G1 | 9 (2) | 1 (0) | <0.05 | <0.05 |
| G2 | 9 (2) | 0 (0) | |||
| Nasal Itching | G1 | 5 (3) | 0 (0) | <0.05 | 0.65 |
| G2 | 5.50 (4.8) | 0 (0) | |||
| Sneezing | G1 | 7 (3) | 0 (0) | <0.05 | 0.35 |
| G2 | 8 (3) | 0 (0) | |||
| Cough | G1 | 3 (3) | 0 (0) | <0.05 | 0.35 |
| G2 | 4.5 (2.8) | 0 (0) | |||
| Eye related | G1 | 3 (1) | 0 (0) | <0.05 | 0.97 |
| G2 | 3 (2.8) | 0 (0) |
| Symptoms | Group | Baseline (V1) Median Score (IQR) | Final Visit (V2) Median Score (IQR) | Within Group Change Scores p-Value # | Between Group Change Scores p-Value ^ |
|---|---|---|---|---|---|
| Overall | G1 | 54 (13) | 7 (11) | <0.05 | <0.05 |
| G2 | 54.50 (13.75) | 0 (3) | |||
| Activity limitations | G1 | 16 (5) | 3 (4) | <0.05 | <0.05 |
| G2 | 16 (3) | 0 (0) | |||
| Practical problems | G1 | 8 (2) | 1 (2) | <0.05 | <0.05 |
| G2 | 8 (3) | 0 (0.75) | |||
| Nose symptoms | G1 | 13 (2) | 1 (2) | <0.05 | <0.05 |
| G2 | 13.5 (2.75) | 0 (0.75) | |||
| Eye symptoms | G1 | 3 (3) | 0 (0) | <0.05 | 0.52 |
| G2 | 3 (5.25) | 0 (0) | |||
| Other symptoms | G1 | 13 (3) | 2 (3) | <0.05 | <0.05 |
| G2 | 13 (3.75) | 0 (0.75) |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Arsoy, G.; Varış, A.; Saloumi, L.M.; Abdi, A.; Başgut, B. Insights on Allergic Rhinitis Management from a Northern Cyprus Perspective and Evaluation of the Impact of Pharmacist-Led Educational Intervention on Patients’ Outcomes. Medicina 2018, 54, 83. https://0-doi-org.brum.beds.ac.uk/10.3390/medicina54050083
Arsoy G, Varış A, Saloumi LM, Abdi A, Başgut B. Insights on Allergic Rhinitis Management from a Northern Cyprus Perspective and Evaluation of the Impact of Pharmacist-Led Educational Intervention on Patients’ Outcomes. Medicina. 2018; 54(5):83. https://0-doi-org.brum.beds.ac.uk/10.3390/medicina54050083
Chicago/Turabian StyleArsoy, Günay, Ahmet Varış, Louai M. Saloumi, Abdikarim Abdi, and Bilgen Başgut. 2018. "Insights on Allergic Rhinitis Management from a Northern Cyprus Perspective and Evaluation of the Impact of Pharmacist-Led Educational Intervention on Patients’ Outcomes" Medicina 54, no. 5: 83. https://0-doi-org.brum.beds.ac.uk/10.3390/medicina54050083