Epidemiological Characteristics and Spatial-Temporal Distribution of Hand, Foot, and Mouth Disease in Chongqing, China, 2009–2016
Abstract
:1. Introduction
2. Materials and Methods
2.1. Data Collection
2.2. Case Definitions
2.3. Specimen Collection and Laboratory Testing
2.4. Ethics Statement
2.5. Statistical Analysis
3. Results
3.1. Epidemiological Characteristics of HFMD Cases
3.2. Spatial–Temporal Clusters
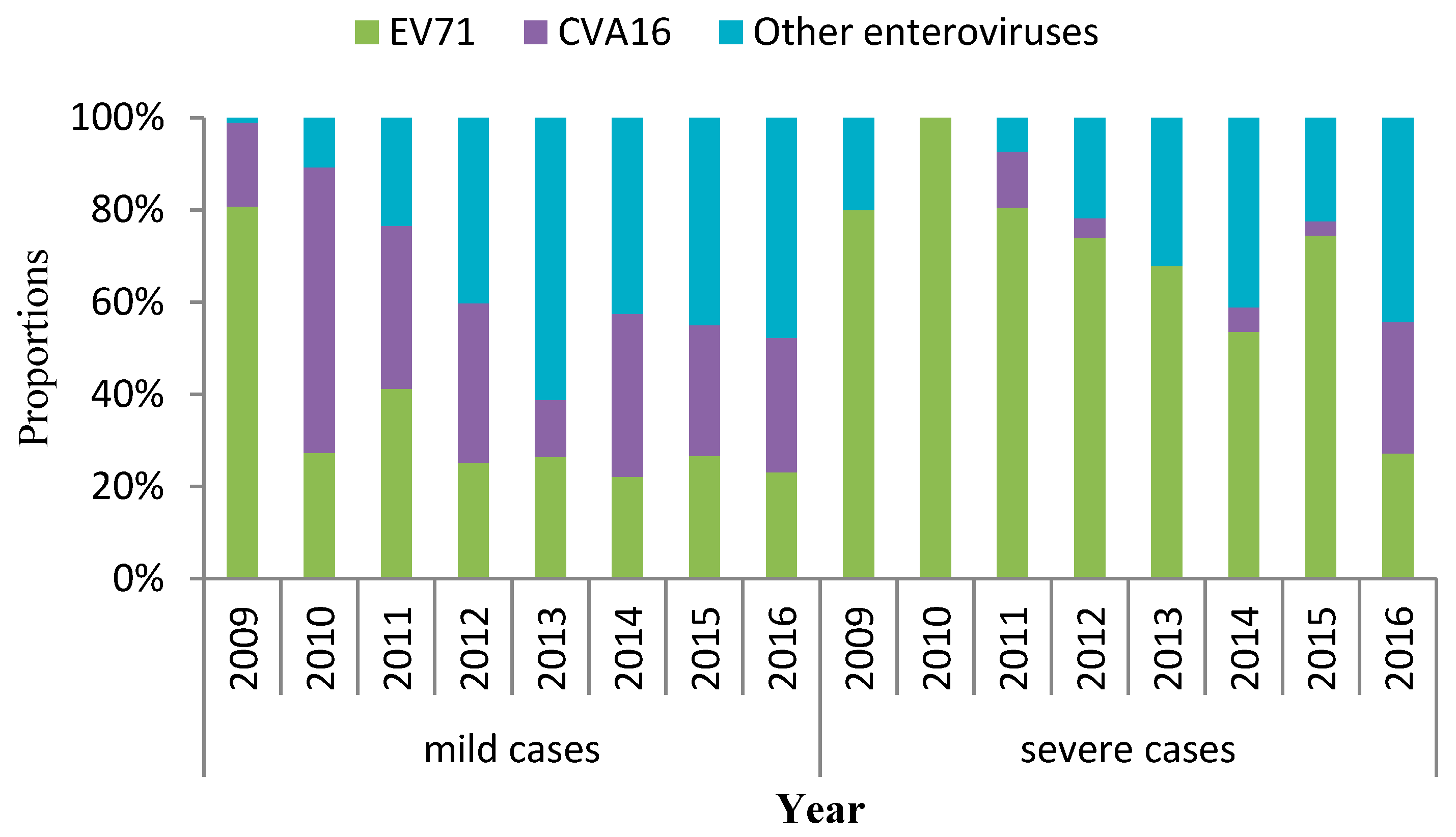
3.3. Distribution of Pathogens’ Serotypes
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Goksugur, N.; Goksugur, S. Images in clinical medicine. Hand, foot, and mouth disease. N. Engl. J. Med. 2010, 362, e49. [Google Scholar] [CrossRef] [PubMed]
- He, Y.Q.; Chen, L.; Xu, W.B.; Yang, H.; Wang, H.Z.; Zong, W.P.; Xian, H.X.; Chen, H.L.; Yao, X.J.; Hu, Z.L.; et al. Emergence, circulation, and spatiotemporal phylogenetic analysis of coxsackievirus a6- and coxsackievirus a10-associated hand, foot, and mouth disease infections from 2008 to 2012 in Shenzhen, China. J. Clin. Microbiol. 2013, 51, 3560–3566. [Google Scholar] [CrossRef] [PubMed]
- Wong, S.S.; Yip, C.C.; Lau, S.K.; Yuen, K.Y. Human enterovirus 71 and hand, foot and mouth disease. Epidemiol. Infect. 2010, 138, 1071–1089. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Xing, W.; Liao, Q.; Viboud, C.; Zhang, J.; Sun, J.; Wu, J.T.; Chang, Z.; Liu, F.; Fang, V.J.; Zheng, Y.; et al. Hand, foot, and mouth disease in China, 2008–12: An epidemiological study. Lancet Infect. Dis. 2014, 14, 308–318. [Google Scholar] [CrossRef]
- Yan, X.; Zhang, Z.Z.; Yang, Z.H.; Zhu, C.M.; Hu, Y.G.; Liu, Q.B. Clinical and Etiological Characteristics of Atypical Hand-Foot-and-Mouth Disease in Children from Chongqing, China: A Retrospective Study. Biomed. Res. Int. 2015, 2015, 802046. [Google Scholar] [CrossRef] [PubMed]
- Lai, F.F.; Yan, Q.; Ge, S.X.; Tang, X.; Chen, R.J.; Xu, H.M. Epidemiologic and etiologic characteristics of hand, foot, and mouth disease in Chongqing, China between 2010 and 2013. J. Med. Virol. 2016, 88, 408–416. [Google Scholar] [CrossRef] [PubMed]
- Guideline for Diagnosis and Treatment of Hand, Foot and Mouth Disease 2010. Available online: http://www.nhfpc.gov.cn/zwgkzt/wsbysj/201004/46884.shtml (accessed on 20 April 2010).
- Protocol of Sample Collection and Laboratory Tests for HMD Cases. Available online: http://www.chinacdc.cn/jkzt/crb/szkb/jszl_2275/200906/t20090612_24707.htm (accessed on 12 June 2009).
- Xiao, X.; Liao, Q.; Kenward, M.G.; Zheng, Y.; Huang, J.; Yin, F.; Yu, H.; Li, X. Comparisons between mild and severe cases of hand, foot and mouth disease in temporal trends: A comparative time series study from mainland China. BMC Public Health 2016, 16, 1109. [Google Scholar] [CrossRef] [PubMed]
- Chen, S.C.; Chang, H.L.; Yan, T.R.; Cheng, Y.T.; Chen, K.T. An eight-year study of epidemiologic features of enterovirus 71 infection in Taiwan. Am. J. Trop. Med. Hyg. 2007, 77, 188–191. [Google Scholar] [PubMed]
- Ang, L.W.; Koh, B.K.; Chan, K.P.; Chua, L.T.; James, L.; Goh, K.T. Epidemiology and control of hand, foot and mouth disease in Singapore, 2001–2007. Ann. Acad. Med. Singap. 2009, 38, 106–112. [Google Scholar] [PubMed]
- Podin, Y.; Gias, E.L.; Ong, F.; Leong, Y.W.; Yee, S.F.; Yusof, M.A.; Perera, D.; Teo, B.; Wee, T.Y.; Yao, S.C.; et al. Sentinel surveillance for human enterovirus 71 in Sarawak, Malaysia: Lessons from the first 7 years. BMC Public Health 2006, 6, 180. [Google Scholar] [CrossRef] [PubMed]
- Report, I.A.S. Hand, foot and mouth disease in Japan, 2002–2011. IASR 2012, 33, 55–56. [Google Scholar]
- Chen, B.; Sumi, A.; Toyoda, S.; Hu, Q.; Zhou, D.; Mise, K.; Zhao, J.; Kobayashi, N. Time series analysis of reported cases of hand, foot, and mouth disease from 2010 to 2013 in Wuhan, China. BMC Infect. Dis. 2015, 15, 495. [Google Scholar] [CrossRef] [PubMed]
- Tu, P.V.; Thao, N.T.; Perera, D.; Huu, T.K.; Tien, N.T.; Thuong, T.C.; How, O.M.; Cardosa, M.J.; McMinn, P.C. Epidemiologic and virologic investigation of hand, foot, and mouth disease, southern Vietnam, 2005. Emerg. Infect. Dis. 2007, 13, 1733–1741. [Google Scholar] [PubMed]
- Liu, Y.; Wang, X.; Pang, C.; Yuan, Z.; Li, H.; Xue, F. Spatio-temporal analysis of the relationship between climate and hand, foot, and mouth disease in Shandong province, China, 2008–2012. BMC Infect. Dis. 2015, 15, 146. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.C.; Tang, J.H.; Hwang, J.S.; Shigematsu, M.; Chan, T.C. Effect of Meteorological and Geographical Factors on the Epidemics of Hand, Foot, and Mouth Disease in Island-Type Territory, East Asia. Biomed. Res. Int. 2015, 2015, 805039. [Google Scholar] [CrossRef] [PubMed]
- Onozuka, D.; Hashizume, M. The influence of temperature and humidity on the incidence of hand, foot, and mouth disease in Japan. Sci. Total Environ. 2011, 410–411, 119–125. [Google Scholar] [CrossRef] [PubMed]
- Wang, P.; Goggins, W.B.; Chan, E.Y. Hand, Foot and Mouth Disease in Hong Kong: A Time-Series Analysis on Its Relationship with Weather. PLoS ONE 2016, 11, e0161006. [Google Scholar] [CrossRef] [PubMed]
- Liao, Y.; Ouyang, R.; Wang, J.; Xu, B. A study of spatiotemporal delay in hand, foot and mouth disease in response to weather variations based on SVD: A case study in Shandong Province, China. BMC Public Health 2015, 15, 71. [Google Scholar] [CrossRef] [PubMed]
- Song, Y.; Wang, F.; Wang, B.; Tao, S.; Zhang, H.; Liu, S.; Ramirez, O.; Zeng, Q. Time series analyses of hand, foot and mouth disease integrating weather variables. PLoS ONE 2015, 10, e0117296. [Google Scholar] [CrossRef] [PubMed]
- Kim, B.I.; Ki, H.; Park, S.; Cho, E.; Chun, B.C. Effect of Climatic Factors on Hand, Foot, and Mouth Disease in South Korea, 2010–2013. PLoS ONE 2016, 11, e0157500. [Google Scholar] [CrossRef] [PubMed]
- Liao, J.; Yu, S.; Yang, F.; Yang, M.; Hu, Y.; Zhang, J. Short-Term Effects of Climatic Variables on Hand, Foot, and Mouth Disease in Mainland China, 2008–2013: A Multilevel Spatial Poisson Regression Model Accounting for Overdispersion. PLoS ONE 2016, 11, e0147054. [Google Scholar] [CrossRef] [PubMed]
- Guo, C.; Yang, J.; Guo, Y.; Ou, Q.Q.; Shen, S.Q.; Ou, C.Q.; Liu, Q.Y. Short-term effects of meteorological factors on pediatric hand, foot, and mouth disease in Guangdong, China: A multi-city time-series analysis. BMC Infect. Dis. 2016, 16, 524. [Google Scholar] [CrossRef] [PubMed]
- Huang, R.; Bian, G.; He, T.; Chen, L.; Xu, G. Effects of Meteorological Parameters and PM10 on the Incidence of Hand, Foot, and Mouth Disease in Children in China. Int. J. Environ. Res. Public Health 2016, 13, 481. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Du, Z.; Wang, X.; Liu, Y.; Yuan, Z.; Xue, F. Detecting the association between meteorological factors and hand, foot, and mouth disease using spatial panel data models. Int. J. Infect. Dis. 2015, 34, 66–70. [Google Scholar] [CrossRef] [PubMed]
- Gui, J.; Liu, Z.; Zhang, T.; Hua, Q.; Jiang, Z.; Chen, B.; Gu, H.; Lv, H.; Dong, C. Epidemiological Characteristics and Spatial-Temporal Clusters of Hand, Foot, and Mouth Disease in Zhejiang Province, China, 2008–2012. PLoS ONE 2015, 10, e0139109. [Google Scholar] [CrossRef] [PubMed]
- Lu, J.; Zeng, H.; Zheng, H.; Yi, L.; Guo, X.; Liu, L.; Sun, L.; Tan, X.; Li, H.; Ke, C.; et al. Hand, foot and mouth disease in Guangdong, China, in 2013: New trends in the continuing epidemic. Clin. Microbiol. Infect. 2014, 20, O442–O445. [Google Scholar] [CrossRef] [PubMed]
- Zhu, F.C.; Liang, Z.L.; Meng, F.Y.; Zeng, Y.; Mao, Q.Y.; Chu, K.; Song, X.F.; Yao, X.; Li, J.X.; Ji, H.; et al. Retrospective study of the incidence of HFMD and seroepidemiology of antibodies against EV71 and CoxA16 in prenatal women and their infants. PLoS ONE 2012, 7, e37206. [Google Scholar] [CrossRef] [PubMed]
- De, W.; Changwen, K.; Wei, L.; Monagin, C.; Jin, Y.; Cong, M.; Hanri, Z.; Jun, S. A large outbreak of hand, foot, and mouth disease caused by EV71 and CAV16 in Guangdong, China, 2009. Arch. Virol. 2011, 156, 945–953. [Google Scholar] [CrossRef] [PubMed]
- Luo, K.W.; Gao, L.D.; Hu, S.X.; Zhang, H.; Deng, Z.H.; Huang, W.; Sun, Q.L.; Zhang, F.; Zhang, S.Y.; Chen, Y. Hand, Foot, and Mouth Disease in Hunan Province, China, 2009–2014: Epidemiology and Death Risk Factors. PLoS ONE 2016, 11, e0167269. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, S.; Liao, Q.; Van Boeckel, T.P.; Xing, W.; Sun, J.; Hsiao, V.Y.; Metcalf, C.J.; Chang, Z.; Liu, F.; Zhang, J.; et al. Hand, Foot, and Mouth Disease in China: Modeling Epidemic Dynamics of Enterovirus Serotypes and Implications for Vaccination. PLoS Med. 2016, 13, e1001958. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Buttery, V.W.; Kenyon, C.; Grunewald, S.; Oberste, M.S.; Nix, W.A. Atypical Presentations of Hand, Foot, and Mouth Disease Caused by Coxsackievirus A6—Minnesota, 2014. MMWR Morb. Mortal. Wkly. Rep. 2015, 64, 805. [Google Scholar] [CrossRef] [PubMed]
- Hongyan, G.; Chengjie, M.; Qiaozhi, Y.; Wenhao, H.; Juan, L.; Lin, P.; Yanli, X.; Hongshan, W.; Xingwang, L. Hand, foot and mouth disease caused by coxsackievirus A6, Beijing, 2013. Pediatr. Infect. Dis. J. 2014, 33, 1302–1303. [Google Scholar] [CrossRef] [PubMed]
- Zeng, H.; Lu, J.; Zheng, H.; Yi, L.; Guo, X.; Liu, L.; Rutherford, S.; Sun, L.; Tan, X.; Li, H.; et al. The Epidemiological Study of Coxsackievirus A6 revealing Hand, Foot and Mouth Disease Epidemic patterns in Guangdong, China. Sci. Rep. 2015, 5, 10550. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Sun, Y.; Du, Y.; Yan, Y.; Huo, D.; Liu, Y.; Peng, X.; Yang, Y.; Liu, F.; Lin, C.; et al. Characterization of Coxsackievirus A6- and Enterovirus 71-Associated Hand Foot and Mouth Disease in Beijing, China, from 2013 to 2015. Front. Microbiol. 2016, 7, 391. [Google Scholar] [CrossRef] [PubMed]





| Total | 2009 | 2010 | 2011 | 2012 | 2013 | 2014 | 2015 | 2016 | |
|---|---|---|---|---|---|---|---|---|---|
| (n = 276,207) | (n = 9558) | (n = 20,209) | (n = 20,641) | (n = 28,995) | (n = 29,883) | (n = 55,320) | (n = 46,757) | (n = 64,844) | |
| n (%) | n (%) | n (%) | n (%) | n (%) | n (%) | n (%) | n (%) | n (%) | |
| Age (year) | |||||||||
| less than 1 year | 25,929 (9.4) | 660 (6.91) | 1397 (6.9) | 1551 (7.5) | 2703 (9.3) | 3454 (11.6) | 4671 (8.4) | 4224 (9.0) | 7269 (11.2) |
| 1~ | 86,149 (31.2) | 1099 (11.5) | 5175 (25.6) | 5297 (25.7) | 8467 (29.2) | 10,413 (34.9) | 17,609 (31.8) | 14,628 (31.3) | 23,461 (36.2) |
| 2~ | 64,142 (23.2) | 2662 (27.9) | 5380 (26.6) | 5173 (25.1) | 7091 (24.5) | 6557 (21.9) | 13,410 (24.2) | 10,335 (22.1) | 13,534 (20.9) |
| 3~ | 53,560 (19.4) | 2437 (25.5) | 4445 (22.0) | 4483 (21.7) | 5910 (20.4) | 5120 (17.1) | 10,435 (18.9) | 9560 (20.5) | 11,170 (17.2) |
| 4~ | 24,049 (8.7) | 1399 (14.6) | 1870 (9.3) | 2110 (10.2) | 2608 (9.0) | 2226 (7.5) | 4784 (8.7) | 4084 (8.7) | 4968 (7.7) |
| 5~ | 10,022 (3.6) | 655 (6.9) | 690 (3.4) | 935 (4.5) | 1041 (3.6) | 962 (3.2) | 2013 (3.6) | 1845 (3.9) | 1881 (2.9) |
| more than 6 years | 12,356 (4.5) | 646 (6.8) | 1252 (6.2) | 1092 (5.3) | 1175 (4.1) | 1151 (3.9) | 2398 (4.3) | 2081 (4.5) | 2561 (3.9) |
| Gender | |||||||||
| Male | 162,934 (59.0) | 5739 (60.0) | 12,096 (59.9) | 12,612 (61.1) | 17,647 (60.9) | 17,792 (59.5) | 32,216 (58.2) | 27,309 (58.4) | 37,523 (57.9) |
| Female | 113,273 (41.0) | 3819 (40.0) | 8113 (40.1) | 8029 (38.9) | 11,348 (39.1) | 12,091 (40.5) | 23,104 (41.8) | 19,448 (41.6) | 27,321 (42.1) |
| Sex ratio | 1.44 | 1.50 | 1.49 | 1.57 | 1.56 | 1.47 | 1.39 | 1.40 | 1.37 |
| Population classification | |||||||||
| In kindergarten | 86,339 (31.2) | 3868 (40.5) | 8123 (40.2) | 7186 (34.8) | 9604 (33.1) | 8087 (27.1) | 17,053 (30.8) | 14,965 (32.0) | 17,453 (20.6) |
| Scatter children * | 176,858 (63.8) | 4920 (51.5) | 11,050 (54.7) | 12,088 (58.6) | 17,760 (61.3) | 20,329 (68.0) | 35,611 (64.4) | 29,545 (63.2) | 45,555 (52.7) |
| In primary school | 7504 (2.7) | 347 (3.6) | 719 (3.6) | 727 (3.5) | 811 (2.8) | 755 (2.5) | 1459 (2.6) | 1161 (2.5) | 1525 (1.8) |
| Others | 5506 (2.3) | 423 (4.4) | 317 (1.6) | 640 (3.1) | 820 (2.8) | 712 (2.4) | 1197 (2.2) | 1086 (2.3) | 311 (0.4) |
| Severe cases | 641 | 14 | 42 | 73 | 30 | 88 | 92 | 192 | 110 |
| Year | Districts/Countries (n) | Cluster Centers/Radius | Time (Month) | Observed Cases (n) | Expected Cases (n) | RR | LLR | p-Value |
|---|---|---|---|---|---|---|---|---|
| 2009 | 13 | (29.87N, 106.49E)/64.12 km | April–June | 4077 | 1039 | 6.16 | 3165.487 | 0.001 |
| 2010 | 9 | (29.45N, 106.72E)/52.31 km | Apr–July | 8667 | 1987 | 6.97 | 7526.839 | 0.001 |
| 2011 | 8 | (31.92N, 108.77E)/170.97 km | Apr–June | 3571 | 1037 | 3.96 | 2055.819 | 0.001 |
| 2012 | 7 | (29.45N, 106.72E)/38.52 km | October–December | 5524 | 1304 | 5.01 | 4098.742 | 0.001 |
| 2013 | 10 | (29.61N, 106.37E)/39.48 km | October–December | 5931 | 2092 | 3.25 | 2599.343 | 0.001 |
| 2014 | 7 | (29.45N, 106.72E)/38.52 km | September–December | 9960 | 3329 | 3.43 | 4729.999 | 0.001 |
| 2015 | 7 | (29.45N, 106.72E)/38.52 km | April–July | 7765 | 2649 | 3.35 | 3567.425 | 0.001 |
| 2016 | 9 | (29.45N, 106.72E)/52.31 km | June–October | 23,788 | 10,227 | 3.14 | 8444.554 | 0.001 |
| Year | Mild Cases | Severe Cases | χ2 | p-Value * | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Specimen | EV71 | CVA16 | Other Enterovirus | Specimen | EV71 | CVA16 | Other Enterovirus | |||
| 2009 | 298 | 155 | 35 | 2 | 14 | 4 | 0 | 1 | 6.1 ** | 0.078 |
| 2010 | 1418 | 246 | 558 | 97 | 42 | 22 | 0 | 0 | 49.9 ** | <0.01 |
| 2011 | 2646 | 717 | 615 | 409 | 73 | 33 | 5 | 3 | 25.4 | <0.01 |
| 2012 | 2284 | 397 | 545 | 633 | 30 | 17 | 1 | 5 | 28.8 | <0.01 |
| 2013 | 2568 | 474 | 222 | 1100 | 88 | 40 | 0 | 19 | 50.6 | <0.01 |
| 2014 | 4102 | 680 | 1084 | 1307 | 92 | 30 | 3 | 23 | 38.1 | <0.01 |
| 2015 | 2734 | 525 | 561 | 887 | 191 | 96 | 4 | 29 | 136.6 | <0.01 |
| 2016 | 2791 | 481 | 608 | 993 | 111 | 19 | 20 | 31 | 0.7 | 0.722 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Qi, L.; Tang, W.; Zhao, H.; Ling, H.; Su, K.; Zhao, H.; Li, Q.; Shen, T. Epidemiological Characteristics and Spatial-Temporal Distribution of Hand, Foot, and Mouth Disease in Chongqing, China, 2009–2016. Int. J. Environ. Res. Public Health 2018, 15, 270. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph15020270
Qi L, Tang W, Zhao H, Ling H, Su K, Zhao H, Li Q, Shen T. Epidemiological Characteristics and Spatial-Temporal Distribution of Hand, Foot, and Mouth Disease in Chongqing, China, 2009–2016. International Journal of Environmental Research and Public Health. 2018; 15(2):270. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph15020270
Chicago/Turabian StyleQi, Li, Wenge Tang, Han Zhao, Hua Ling, Kun Su, Hua Zhao, Qin Li, and Tao Shen. 2018. "Epidemiological Characteristics and Spatial-Temporal Distribution of Hand, Foot, and Mouth Disease in Chongqing, China, 2009–2016" International Journal of Environmental Research and Public Health 15, no. 2: 270. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph15020270





