The Nursing Stress Scale-Spanish Version: An Update to Its Psychometric Properties and Validation of a Short-form Version in Acute Care Hospital Settings
Abstract
:1. Introduction
Background
2. Materials and Methods
2.1. Study Design
2.2. Setting and Sample
2.3. Data Collection
2.4. Measures
2.5. Data Analyses
2.6. Ethical Considerations
3. Results
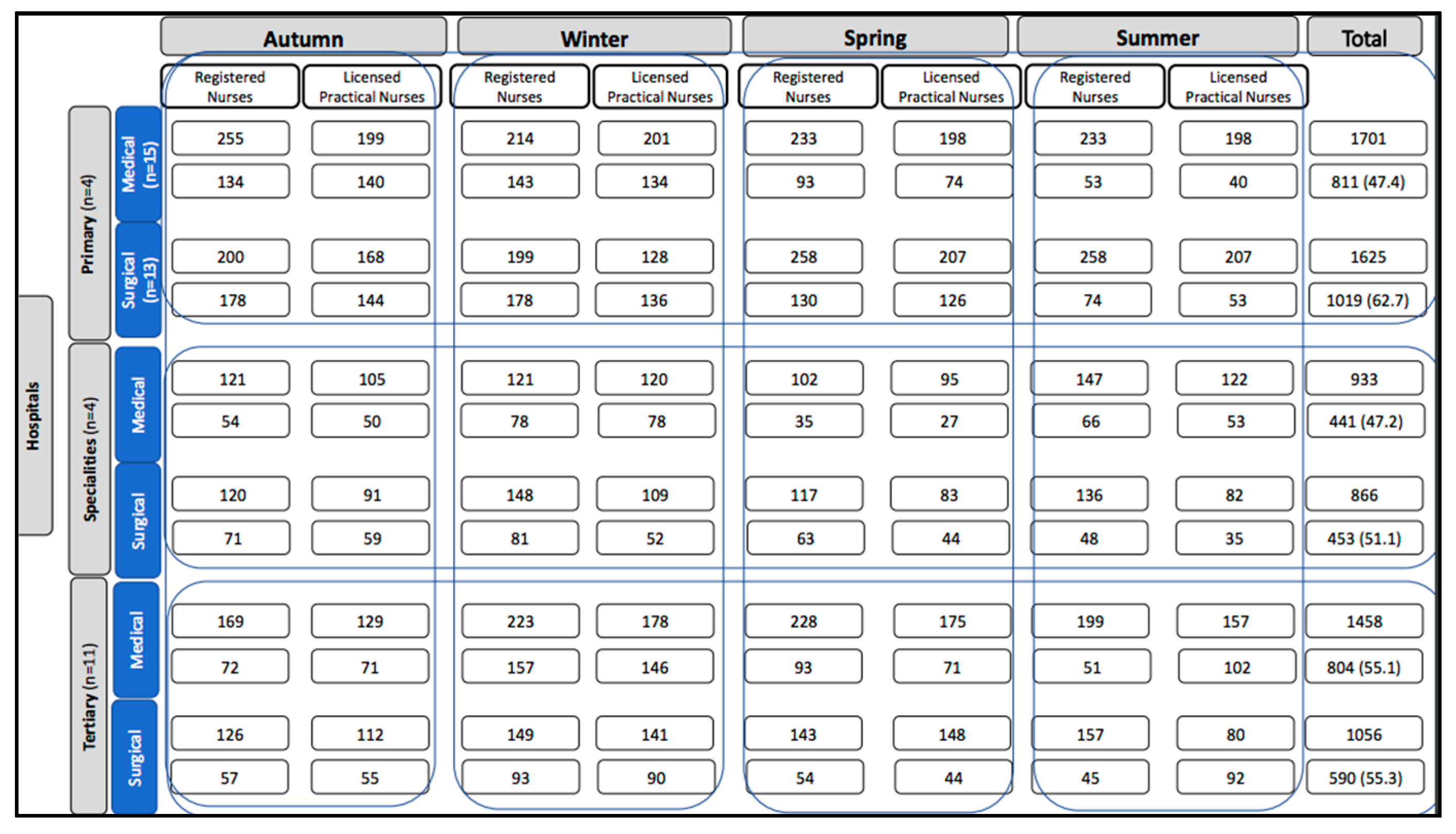
3.1. Sample Characteristics
3.2. Descriptive Analysis of NSS-34
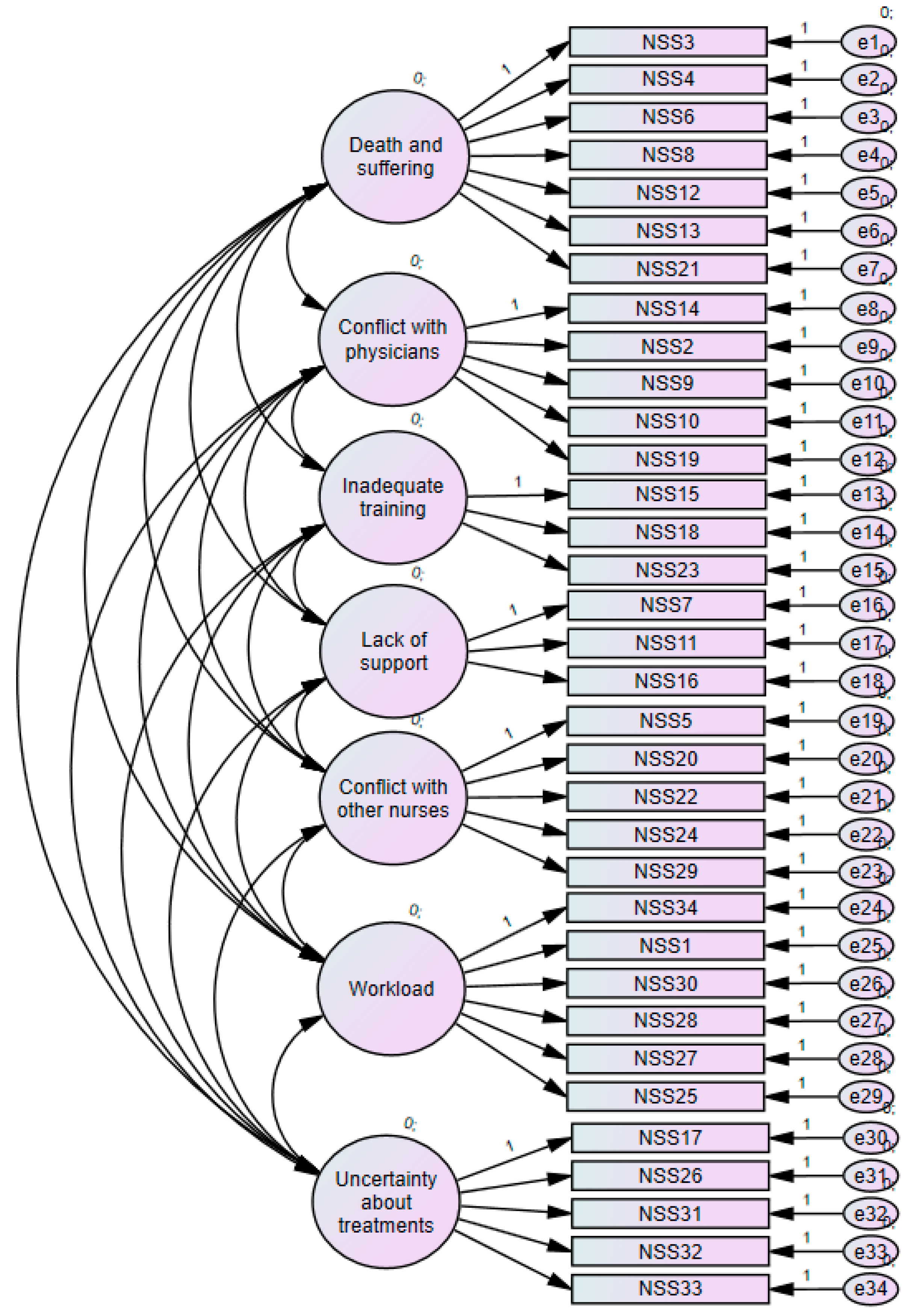
3.3. Validation of NSS-34
3.4. Validation of Short-form NSS-11
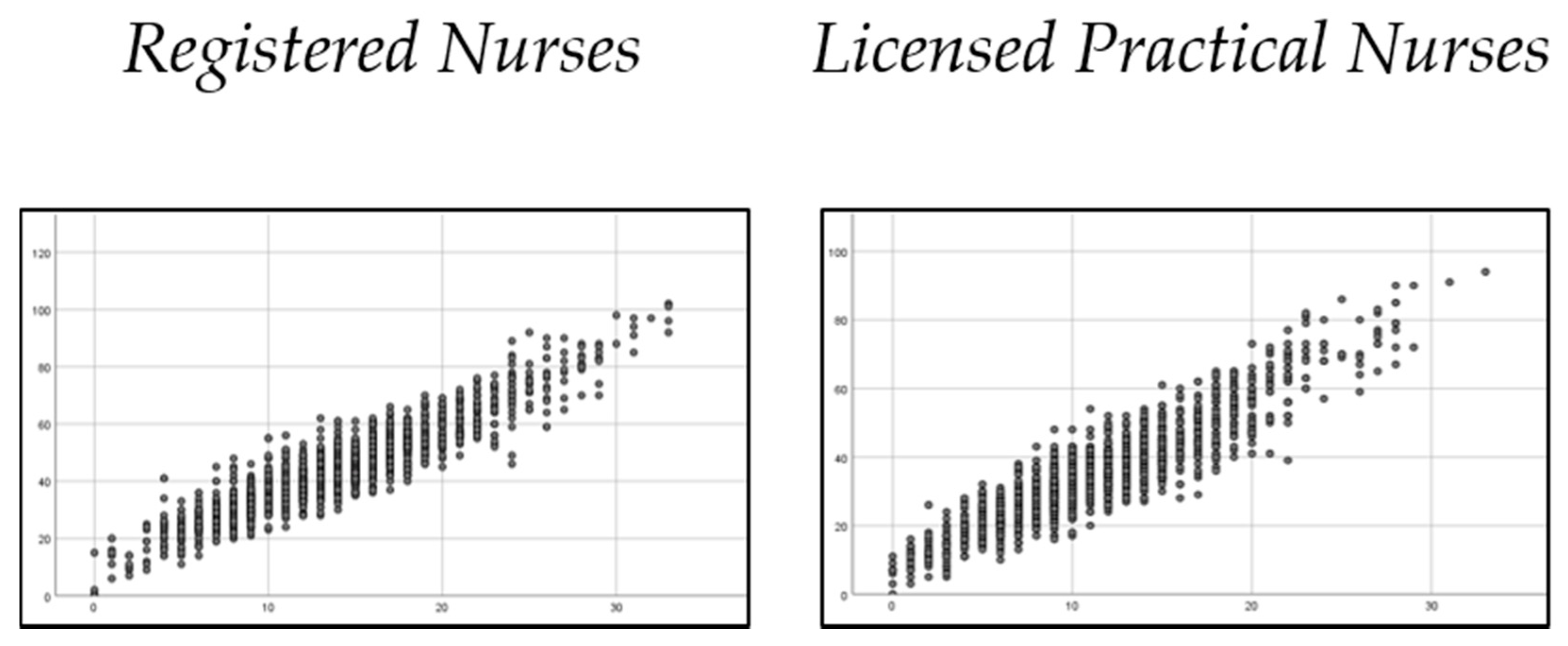
3.5. Comparison of the 34-Item NSS and NSS-11 (Short-Form)
3.6. COSMIN Checklist
4. Discussion
Limitations and Strengths
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Lee, M.H.; Holzemer, W.L.; Faucett, J. Psychometric Evaluation of the Nursing Stress Scale (NSS) Among Chinese Nurses in Taiwan. J. Nurs. Meas. 2007, 15, 133–144. [Google Scholar] [CrossRef]
- Rosnawati, M.R.; Moe, H.; Masilamani, R.; Darus, A. The Bahasa Melayu version of the Nursing Stress Scale among nurses: A reliability study in Malaysia. Asia Pac. J. Public Health 2010, 22, 501–506. [Google Scholar] [CrossRef]
- Pathak, V.; Chakraborty, T.; Mukhopadhyay, S. Reliability and validity analysis of modified nursing stress scale for indian population. J. Nurs. Meas. 2013, 2, 224–245. [Google Scholar] [CrossRef]
- Más-Pons, R.; Escribà-Agüir, V. The Spanish Version of the Nursing Stress Scale, a Cross-cultural Adaptation Process. Rev. Esp. Salud Públ. 1998, 72, 529–538. [Google Scholar]
- Escribà-Agüir, V.; Más-Pons, R.; Cardenas, M.; Pérez, S. Validación de la escala de estresores laborales en personal de enfermería: «the nursing stress scale». Gac. Sanit. 1999, 13, 191–200. [Google Scholar] [CrossRef] [Green Version]
- Gray, P.T.; Anderson, J.G. The Nursing Stress Scale: Development of an instrument. J. Psychopathol. Behav. Assess 1981, 3, 11–23. [Google Scholar] [CrossRef]
- Appley, M.H.; Trumbull, R. On the Concept of Psychological Stress. In Psychological Stress: Issues in Research; Appleton-Century-Crofts: New York, NY, USA, 1967. [Google Scholar]
- Sarafis, P.; Rousaki, E.; Tsounis, A.; Malliarou, M.; Lahana, L.; Bamidis, P.; Niakas, D.; Papastavrou, E. The impact of occupational stress on nurses’ caring behaviors and their health related quality of life. BMC Nurs. 2016, 15, 56. [Google Scholar] [CrossRef] [Green Version]
- Gnerre, P.; Rivetti, C.; Rossi, A.P.; Tesei, L.; Montemurro, D.; Nardi, R. Work stress and burnout among physicians and nurses in Internal and Emergency Departments. Italian J. Med. 2017, 11, 151–158. [Google Scholar] [CrossRef] [Green Version]
- Blomberg, K.; Isaksson, A.K.; Allvin, R.; Bisholt, B.; Ewertsson, M.; Kullén-Engström, A.; Ohlsson, U.; Sundler-Johansson, A.; Gustafsson, M. Work stress among newly graduated nurses in relation to workplace and clinical group supervision. J. Nurs. Manag. 2016, 24, 80–87. [Google Scholar] [CrossRef] [PubMed]
- Hoeve, Y.; Brouwer, J.; Kunnen, S. Turnover prevention: The direct and indirect association between organizational job stressors, negative emotions and professional commitment in novice nurses. J. Adv. Nurs. 2019, 76, 836–845. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kakemam, E.; Raeissi, P.; Raoofi, S.; Soltani, A.; Sokhanvar, M.; Visentin, D.C.; Cleary, M. Occupational stress and associated risk factors among nurses: A cross-sectional study. Contemp. Nurse 2019, 55, 237–249. [Google Scholar] [CrossRef] [PubMed]
- Halpin, Y.; Terry, L.M.; Curzio, J. A longitudinal, mixed methods investigation of newly qualified nurses’ workplace stressors and stress experiences during transition. J. Adv. Nurs. 2017, 73, 2577–2586. [Google Scholar] [CrossRef] [PubMed]
- Luan, X.; Wang, P.; Hou, W.; Chen, L.; Lou, F. Job stress and burnout: A comparative study of senior and head nurses in China. Nurs. Health Sci. 2017, 19, 163–169. [Google Scholar] [CrossRef] [PubMed]
- Nasu, K.; Sato, K.; Fukahori, H. Rebuilding and guiding a care community: A grounded theory of end-of-life nursing care practice in long-term care settings. J. Adv. Nurs. 2020, 76, 1009–1018. [Google Scholar] [CrossRef] [PubMed]
- Lo, W.Y.; Chien, L.Y.; Hwang, F.M.; Huang, N.; Chiou, S.T. From job stress to intention to leave among hospital nurses: A structural equation modelling approach. J. Adv. Nurs. 2017, 74, 677–688. [Google Scholar] [CrossRef] [PubMed]
- Admi, H.; Eilon, Y.; Renker, P.; Unhasuta, K. Stress measurement among charge nurses: Developing a cross-cultural tool. J. Adv. Nurs. 2016, 72, 926–935. [Google Scholar] [CrossRef]
- Parkitny, L.; McAuley, J. The Depression Anxiety Stress Scale (DASS). J. Physiother. 2010, 56, 204. [Google Scholar] [CrossRef] [Green Version]
- Vieweg, B.W.; Hedlund, J.L. The General Health Questionnaire (GHQ): A comprehensive review. J. Oper. Psychiatry 1983, 14, 74–81. [Google Scholar]
- Chan, S.F.; La Greca, A.M. Perceived Stress Scale (PSS). Encycl. Behav. Med. 2013, 1454–1455. [Google Scholar] [CrossRef]
- Karasek, R.; Brisson, C.; Kawakami, N.; Houtman, I.; Bongers, P.; Amick, B. The Job Content Questionnaire (JCQ): An instrument for internationally comparative assessments of psychosocial job characteristics. J. Occup. 1998, 3, 322–355. [Google Scholar] [CrossRef]
- Campillo-Cruz, M.; González-Gutiérrez, J.L.; Ardoy-Cuadros, J.; Fernández-Muñoz, J.J. The Development and Exploratory Psychometric Properties of the Traumatic and Routine Stressors Scale on Emergency Nurses (TRSS-EN). Int. J. Environ. Res. Public Health 2020, 17, 1963. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Opie, T.; Dollard, M.; Lenthall, S.; Knight, S. Occupational Stress in Remote Area Nursing: Development of the Remote Area Nursing Stress Scale (RANSS). J. Nurs. Meas. 2013, 21, 246–263. [Google Scholar] [CrossRef] [PubMed]
- Benoliel, J.Q.; McCorkle, R.; Georgiadou, F.; Denton, T.; Spitzer, A. Measurement of stress in clinical nursing. Cancer Nurs. 1990, 13, 221–228. [Google Scholar] [CrossRef] [PubMed]
- Harris, P.E. The Nursing Stress Index. Work Stress 1989, 3, 335–346. [Google Scholar] [CrossRef]
- Ko, W.; Kiser, N.L. Stress Levels of Nurses in Oncology Outpatient Units. Clin. J. Oncol. Nurs. 2016, 20, 158–164. [Google Scholar] [CrossRef] [PubMed]
- Lavoie, T.M.; Feeley, N.; Lavigne, G.L.; Genest, C.; Robins, S.; Fréchette, J. Neonatal Intensive Care Unit Nurses Working in an Open Ward: Stress and Work Satisfaction. Health Care Manag. 2016, 35, 205–216. [Google Scholar] [CrossRef] [PubMed]
- Gauthier, T.; Meyer, R.M.; Grefe, D.; Gold, J.I. An on-the-job mindfulness-based intervention for pediatric ICU nurses: A pilot. J. Pediatr. Nurs. 2015, 30, 402–409. [Google Scholar] [CrossRef]
- Yang, J.; Tang, S.; Zhou, W. Effect of Mindfulness-Based Stress Reduction Therapy on Work Stress and Mental Health of Psychiatric Nurses. Psychiatr. Danub. 2018, 30, 189–196. [Google Scholar] [CrossRef]
- Romano, M.; Festini, F.; Bronner, L. Cross-sectional study on the determinants of work stress for nurses and intention of leaving the profession. Prof. Inferm. 2015, 68, 203–210. [Google Scholar] [CrossRef]
- Carrillo, C.; Ríos, M.I.; Escudero, L.; Martínez, M. Factores de estrés laboral en el personal de Enfermería hospitalario del equipo volante según el modelo demanda-control-apoyo. Enferm. Glob. 2018, 17, 304–324. [Google Scholar] [CrossRef]
- Blanca-Gutiérrez, J.J.; Arias-Herrera, A. Síndrome de burnout en personal de enfermería: Asociado con estresores del entorno hospitalario, Andalucía, España. Enferm. Univ. 2018, 15. [Google Scholar] [CrossRef]
- Mokkink, L.B.; Prinsen, C.; Patrick, D.L.; Alonso, J.; Bouter, L.M.; de Vet, H.; Terwee, C.B. COSMIN Study Design Checklist for Patient-Reported Outcome Measurement Instruments; Department of Epidemiology and Biostatistics Amsterdam Public Health Research Institute Amsterdam University Medical Centers, Location VUmc: Amsterdam, The Netherlands, 2019; pp. 1–32. [Google Scholar]
- Hu, L.T.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Struct. Equ. Model. 1999, 6, 1–55. [Google Scholar] [CrossRef]
- Kline, R.B. Principles and Practice of Structural Equation Modeling, 4th ed.; Guilford Publications: New York, NY, USA, 2005. [Google Scholar]
- Bentler, P.M. EQS 6 Structural Equations Program Manual; Multivariate Software Inc.: Encino, CA, USA, 2006. [Google Scholar]
- Meyers, L.S.; Gamst, G.; Guarino, A.J. Applied Multivariate Research: Design and Interpretation; SAGE Publications, Inc.: Thousand Oaks, CA, USA, 2006. [Google Scholar]
- Ware, J.E., Jr.; Gandek, B. Methods for testing data quality, scaling assumptions, and reliability: The IQOLA Project approach. International Quality of Life Assessment. J. Clin. Epidemiol. 1998, 51, 945–952. [Google Scholar] [CrossRef]
- Rey, S. Mixité, trajectoires professionnelles et division sexuée du travail dans les équipes infirmières [Mix, career paths and gendered division of work in nursing teams]. Soins 2020, 65, 40–42. [Google Scholar] [CrossRef]
- Cohen, J.; Venter, W.D.F. The integration of occupational- and household-based chronic stress among South African women employed as public hospital nurses. PLoS ONE 2020, 15, e0231693. [Google Scholar] [CrossRef]
- Hatch, D.J.; Freude, G.; Martus, P.; Rose, U.; Müller, G.; Potter, G.G. Age, burnout and physical and psychological work ability among nurses. Occup. Med. 2018, 68, 246–254. [Google Scholar] [CrossRef] [Green Version]
- Tran, T.T.T.; Nguyen, N.B.; Luong, M.A.; Bui, T.H.A.; Phan, T.D.; Tran, V.O.; Ngo, T.H.; Minas, H.; Nguyen, T.Q. Stress, anxiety and depression in clinical nurses in Vietnam: A cross-sectional survey and cluster analysis. Int. J. Ment. Health 2019, 3, 3. [Google Scholar] [CrossRef] [Green Version]
- Bai, J.H.; Ravindran, V. Job stress among nurses. Indian J. Contin. Nurs. Educ. 2019, 20, 92. [Google Scholar] [CrossRef]
- Savič, B.S.; Pagon, M. Relationship Between Nurses and Physicians in Terms of Organizational Culture: Who Is Responsible for Subordination of Nurses? Croat. Med. J. 2008, 49, 334–343. [Google Scholar] [CrossRef]
- Siedlecki, S.L.; Hixson, E.D. Relationships Between Nurses and Physicians Matter. J Issues Nurs. 2015, 31, 20. [Google Scholar]
- Alkrisat, M.; Alatrash, M. Psychometric Properties of the Extended Nursing Stress Scale: Measuring Stress in Workplace. J. Nurs. Meas. 2017, 25, 31–45. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.M.; Nam, K.A.; Lee, E.; Jeong, G.H. Validity and Reliability of the Korean Version of the Expanded Nursing Stress Scale. J. Korean Acad. Nurs. Adm. 2015, 21, 542–551. [Google Scholar] [CrossRef]
- Çağan, Ö. Examining psychometric properties of the Turkish version of the Nursing Job Rotation Stress Scale (NJRS). Perspect. Psychiatr. Care. 2019, 55, 773–778. [Google Scholar] [CrossRef] [PubMed]
- Huang, S.; Lin, Y.H.; Kao, C.C.; Yang, H.Y.; Anne, Y.L.; Wang, C.H. Nursing Job Rotation Stress Scale development and psychometric evaluation. Jpn. J. Nurs. Sci. 2016, 13, 114–122. [Google Scholar] [CrossRef] [PubMed]
- Pélissier, C.; Charbotel, B.; Fassier, J.B.; Fort, E.; Fontana, L. Nurses’ Occupational and Medical Risks Factors of Leaving the Profession in Nursing Homes. Int J. Environ. Res. Public Health 2018, 15, 1850. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Barrientos, S.; Vega-Vázquez, L.; De Diego-Cordero, R.; Badanta-Romero, B.; Porcel-Gálvez, A.M. Interventions to improve working conditions of nursing staff in acute care hospitals: Scoping review. J. Nurs. Manag. 2018, 26, 94–107. [Google Scholar] [CrossRef]
| Variables | RN n (%) | LPN n (%) | Total n (%) | Statistics p-Value |
|---|---|---|---|---|
| 2195 (53.4) | 1914 (46.6) | 4109 | ||
| Gender | <0.001 | |||
| Male | 449 (20) | 158 (8) | 607 (15) | |
| Female | 1746 (80) | 1756 (92) | 3502 (85) | |
| Age (years) | ||||
| Mean ± SD | 44.3 (8.7) | 49 (8.5) | 46.5 (8.9) | <0.001 |
| Level of education | <0.001 | |||
| Vocational training | - | 1795 (93.8) | 1795 (43.7) | |
| Registered nurse and Bachelor in nursing sciences | 2003 (91.2) | 113 (5.9) | 2116 (51.5) | |
| Master in nursing sciences | 188 (8.6) | 6 (0.3) | 194 (4.7) | |
| PhD in nursing sciences | 6 (0.3) | 0 | 6 (0.1) | |
| Years of professional experience | <0.001 | |||
| Current job (Mean± SD) | 19.4 (8.9) | 16.7 (9.3) | 18 (9.2) | |
| Current service (Mean± SD) | 8.3 (8.1) | 6.7 (6.7) | 7.6 (7.5) | |
| Hospital admission | ||||
| Primary | 977 (44.5) | 842 (44) | 1819 (44.2) | |
| Specialist | 494 (22.5) | 402 (21) | 896 (21.8) | 0.230 |
| Tertiary | 724 (33) | 670 (35) | 1394 (34) | |
| Health Unit/Service | ||||
| Surgical | 1128 (51.4) | 928 (48.5) | 2056 (50) | 0.066 |
| Medical | 1067 (48.6) | 986 (51.5) | 2053 (50) | |
| Contract | <0.001 | |||
| Permanent | 1010 (46) | 657 (34.3) | 1667 (40) | |
| Temporary | 1185 (54) | 1257 (65.7) | 2442 (60) | |
| Workday | ||||
| Full-time (35–40 h/week) | 1821 (83) | 1780 (93) | 3601 (88) | <0.001 |
| Part-time | 374 (17) | 134 (7) | 508 (12) | |
| Shift hours | ||||
| Mean ± SD | 9 (2.7) | 9.2 (2.7) | 9.1 (2.7) | 0.349 |
| 34-ITEM NSS | MEAN ± SD | |
|---|---|---|
| 1. Frequent job interruptions. | 2.41 | 0.785 |
| 2. Criticism by physician. | 0.73 | 0.724 |
| 3. Performing procedures that patients experience as painful. | 1.45 | 0.775 |
| 4. Feeling helpless when patients fail to improve. | 1.23 | 0.915 |
| 5. Conflict with supervisor. | 0.32 | 0.610 |
| 6. Listening or talking to a patient about his/her approaching death. | 1.02 | 0.794 |
| 7. Lack of opportunity to talk openly with other unit personnel about problems on the unit. | 1.13 | 0.886 |
| 8. The death of a patient. | 1.47 | 0.850 |
| 9. Conflict with physician. | 0.50 | 0.694 |
| 10. Fear of making a mistake in treating a patient. | 1.14 | 0.805 |
| 11. Lack of an opportunity to share experiences and feelings with other personnel in the ward/unit. | 1.15 | 0.851 |
| 12. The death of a patient with whom you develop a close relationship. | 1.30 | 0.808 |
| 13. Physician not being present when patient dies. | 1.48 | 0.988 |
| 14. Disagreement concerning the treatment of a patient. | 0.92 | 0.744 |
| 15. Feeling inadequately prepared to help with the emotional needs of a patient’s family. | 1.02 | 0.732 |
| 16. Lack of opportunity to express to other personnel in the ward/unit my negative feelings towards patient. | 0.91 | 0.766 |
| 17. Inadequate information from a physician regarding the medical condition of a patient. | 1.31 | 0.884 |
| 18. Being asked a question by a patient for which I do not have a satisfactory answer. | 1.11 | 0.641 |
| 19. Making a decision concerning a patient when the physician is unavailable | 0.94 | 0.881 |
| 20. Covering other units that are short-staffed. | 1.00 | 1.005 |
| 21. Watching a patient suffer. | 1.76 | 0.856 |
| 22. Difficulty in working with a particular nurse (or nurse) on the unit. | 0.61 | 0.742 |
| 23. Feeling inadequately prepared to help with the emotional needs of a patient. | 0.93 | 0.705 |
| 24. Criticism by a superior. | 0.56 | 0.718 |
| 25. Unpredictable staffing and scheduling. | 1.01 | 0.874 |
| 26. A physician ordering what appears to be inappropriate treatment for a patient. | 0.87 | 0.746 |
| 27. Too many non-nursing tasks required (such as administrative tasks). | 1.58 | 0.972 |
| 28. Not enough time to provide emotional support to a patient. | 1.72 | 0.876 |
| 29. Difficulty in working with a particular nurse (or nurses) within the ward. | 0.64 | 0.747 |
| 30. Not enough time to complete all of my nursing tasks. | 1.59 | 0.874 |
| 31. A physician not being present in a medical emergency. | 1.22 | 0.893 |
| 32. Not knowing what a patient or a patient’s family ought to be told about the patient’s condition and treatment. | 1.11 | 0.774 |
| 33. Uncertainty regarding the operation and functioning of specialised equipment. | 1.04 | 0.725 |
| 34. Not enough staff to adequately cover the unit. | 1.77 | 0.936 |
| Registered Nurses | Licensed Practical Nurses | |||||||
|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | 1 | 2 | 3 | 4 | |
| 7. Lack of an opportunity to talk openly with other unit personnel about problems on the unit. | 0.787 | 0.614 | ||||||
| 11. Lack of an opportunity to share experiences and feelings with other personnel in the ward/unit. | 0.771 | 0.666 | ||||||
| 14. Disagreement concerning the treatment of a patient. | 0.570 | 0.731 | ||||||
| 15.Feeling inadequately prepared to help with the emotional needs of a patient’s family. | 0.889 | 0.869 | ||||||
| 22. Difficulty in working with a particular nurse (or nurses) on the unit. | 0.763 | 0.812 | ||||||
| 23.Feeling inadequately prepared to help with the emotional needs of a patient. | 0.837 | 0.769 | ||||||
| 26. A physician ordering what appears to be inappropriate treatment for a patient. | 0.672 | 0.712 | ||||||
| 28. Not enough time to provide emotional support to a patient. | 0.769 | 0.738 | ||||||
| 29. Difficulty in working with a particular nurse (or nurses) within the ward. | 0.756 | 0.841 | ||||||
| 30. Not enough time to complete all of my nursing tasks. | 0.802 | 0.730 | ||||||
| 34. Not enough staff to adequately cover the unit. | 0.745 | 0.729 | ||||||
| Items | Nursing Stress Scale–Spanish Version |
|---|---|
| General recommendations for the design of a study on measurement properties | +++ |
| Content validity | NR |
| Structural validity | ++ |
| Internal consistency | +++ |
| Cross-cultural validity/measurement invariance | NR |
| Measurement error and reliability | +++ |
| Criterion validity | +++ |
| Hypotheses testing for construct validity A. Comparison with other outcome measurement instruments (convergent validity) B. Comparison between subgroups (discriminative or known-groups validity) | +++ +++ |
| Responsiveness A. Criterion approach (i.e., comparison to a ‘gold standard’) B. Construct approach (i.e., hypotheses testing; comparison with other outcome measurement instruments) C. Construct approach: (i.e., hypotheses testing: comparison between subgroups) D. Construct approach: (i.e., hypotheses testing: before and after intervention) | +++ +++ +++ NR |
| Translation process | NR |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Porcel-Gálvez, A.M.; Barrientos-Trigo, S.; Bermúdez-García, S.; Fernández-García, E.; Bueno-Ferrán, M.; Badanta, B. The Nursing Stress Scale-Spanish Version: An Update to Its Psychometric Properties and Validation of a Short-form Version in Acute Care Hospital Settings. Int. J. Environ. Res. Public Health 2020, 17, 8456. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph17228456
Porcel-Gálvez AM, Barrientos-Trigo S, Bermúdez-García S, Fernández-García E, Bueno-Ferrán M, Badanta B. The Nursing Stress Scale-Spanish Version: An Update to Its Psychometric Properties and Validation of a Short-form Version in Acute Care Hospital Settings. International Journal of Environmental Research and Public Health. 2020; 17(22):8456. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph17228456
Chicago/Turabian StylePorcel-Gálvez, Ana María, Sergio Barrientos-Trigo, Sara Bermúdez-García, Elena Fernández-García, Mercedes Bueno-Ferrán, and Bárbara Badanta. 2020. "The Nursing Stress Scale-Spanish Version: An Update to Its Psychometric Properties and Validation of a Short-form Version in Acute Care Hospital Settings" International Journal of Environmental Research and Public Health 17, no. 22: 8456. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph17228456






