The Evidence-Based Development of an Intervention to Improve Clinical Health Literacy Practice
Abstract
:1. Introduction
2. Materials and Methods
2.1. Ensuring the Intervention Was Evidence Based
2.2. Intervention
2.3. Undertaking Feasibility Testing of the Intervention and Study Components
2.3.1. Practice Recruitment
2.3.2. Post-Hoc Improvement of the Intervention
2.4. Ethical Issues
2.5. Analysis
- The outcome of the rapid evidence scans of (a) health professional training and (b) factors facilitating the impact of clinical system alerts on clinical practice;
- Practice recruitment;
- Qualitative thematic analysis of the post-hoc focus groups of (a) primary care practitioners and (b) patients and carers.
3. Results
3.1. Rapid Evidence Scans
3.1.1. Approaches to Health Professional Training Shown to Improve Clinical Practice
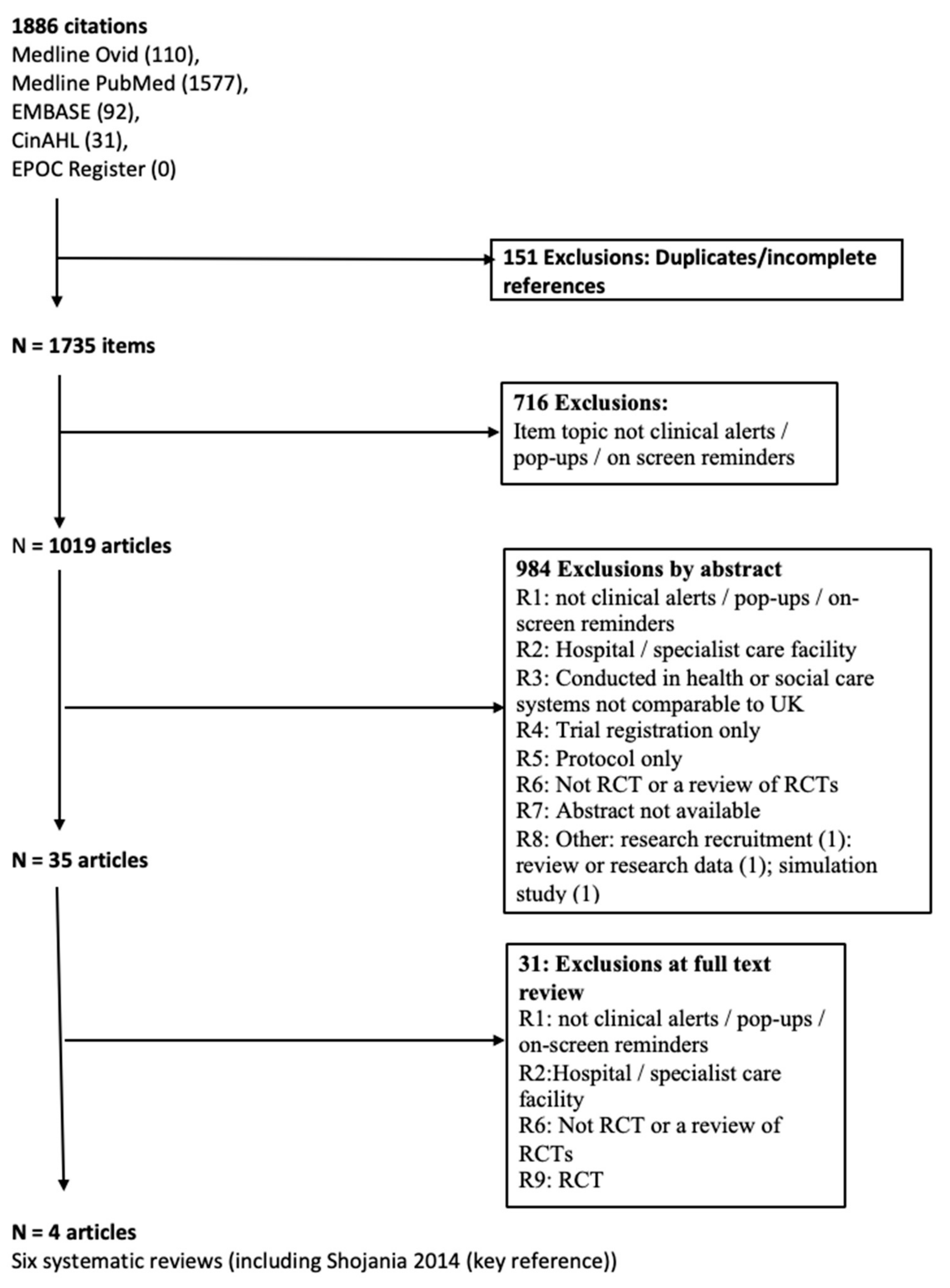
3.1.2. Factors Facilitating the Impact of Clinical System Alerts on Clinical Practice
3.2. Integration of Rapid Review Findings into the Intervention
3.3. Practice Recruitment and Delivery of the Intervention
3.3.1. Post-Hoc Improvement of the Intervention
Feedback from the General Practice Staff
Issues Identified by Practitioners
3.4. Practitioner Suggestions for Addressing the Issues Identified
Feedback from Voice Research Support Group
4. Discussion
4.1. Key Results
4.2. Strengths and Limitations
4.3. How This Research Links to Current Knowledge
4.4. Interpretation
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Appendix A
| Individual Search Component | Search Term | Number Recorded |
|---|---|---|
| 1 | Education title | 48,027 |
| 2 | Training title | 53,237 |
| 3 | Teaching title | 18,689 |
| 4 | 1 or 2 or 3 | 116,609 |
| 5 | systematic review | 0 |
| 6 | randomised controlled trial | 0 |
| 7 | Experiment | 0 |
| 8 | meta-analysis | 75,239 |
| 9 | 5 or 6 or 7 or 8 | 75,239 |
| 10 | 4 and 9 | 739 |
| 11 | Limit 10 English language and yr = 2008–current | 597 |
| Individual Search Component | Search Term | Number Recorded |
|---|---|---|
| 1 | Forms and records control in title or abstract | 4841 |
| 2 | “Appointments and schedules” in title or abstract | 4733 |
| 3 | Medical records systems, computerized/ | 16,146 |
| 4 | Decision making, computer assisted/ | 1918 |
| 5 | Pop-up$.mp. or * medical order entry systems/ | 1592 |
| 6 | exp artificial intelligence/ | 64,858 |
| 7 | 1 or 2 or 3 or 4 or 5 or 6 | 91,781 |
| 8 | Reminder systems/ | 2672 |
| 9 | (reminder$ or prompt$ or cue).tw. | 93,329 |
| 10 | 8 or 9 | 94,547 |
| 11 | 7 and 10 | 1391 |
| 12 | 8 or 11 | 3428 |
| 13 | computer$.tw,hw. | 527,898 |
| 14 | 12 and 13 | 1188 |
| 15 | (computer$ adj3 reminder$).tw. | 211 |
| 16 | 14 or 15 | 1255 |
| 17 | randomized controlled trial.pt. | 341,782 |
| 18 | controlled clinical trial.pt. | 46,251 |
| 19 | randomized controlled trials/ | 101,431 |
| 20 | random allocation/ | 55,981 |
| 21 | double blind method/ | 95,407 |
| 22 | single blind method/ | 20,902 |
| 23 | clinical trial.pt. | 304,286 |
| 24 | (clinical adj trial ?).tw. | 208,944 |
| 25 | ((singl$ or doubl$ or trebl$ or tripl$) adj25 (blind$ or mask$)).tw. | 97,489 |
| 26 | (random$ or placebo ?).tw. | 696,566 |
| 27 | exp clinical trial/ | 563,997 |
| 28 | 17 or 18 or 19 or 20 or 21 or 22 or 23 or 24 or 25 or 26 or 27 | 1,166,567 |
| 29 | limit 28 to animals | 187,341 |
| 30 | limit 29 to humans | 64,168 |
| 31 | 29 not (29 and 30) | 123,173 |
| 32 | 28 not 31 | 1,043,394 |
| 33 | 16 and 32 | 289 |
| 34 | limit 33 to yr = “2009–current” | 112 |
| 35 | limit to English Language | 110 |

References
- Sorensen, K.; Van den Broucke, S.; Fullam, J.; Doyle, G.; Pelikan, J.; Slonska, Z.; Brand, H.; Consortium Health Literacy Project European. Health literacy and public health: A systematic review and integration of definitions and models. BMC Public Health 2012, 12, 80. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nutbeam, D. Health literacy as a public health goal: A challenge for contemporary health education and communication strategies into the 21st century. Health Promot. Int. 2000, 15, 259–267. [Google Scholar] [CrossRef] [Green Version]
- Berkman, N.D.; Sheridan, S.L.; Donahue, K.E.; Halpern, D.J.; Viera, A.; Crotty, K.; Viswanathan, M. Health Literacy Interventions and Outcomes: An Updated Systematic Review; Agency for Healthcare Research and Quality: Rockville, MD, USA, 2011. [Google Scholar]
- Sorensen, K.; Pelikan, J.M.; Rothlin, F.; Ganahl, K.; Slonska, Z.; Doyle, G.; Fullam, J.; Kondilis, B.; Agrafiotis, D.; Uiters, E.; et al. Health literacy in Europe: Comparative results of the European health literacy survey (HLS-EU). Eur. J. Public Health 2015, 25, 1053–1058. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rowlands, G.; Protheroe, J.; Winkley, J.; Richardson, M.; Seed, P.T.; Rudd, R. A mismatch between population health literacy and the complexity of health information: An observational study. Br. J. Gen. Pract. 2015, 65, e379–e386. [Google Scholar] [CrossRef]
- Parker, R. Measuring health literacy: What? So what? Now what? In Measures of Health Literacy: Workshop Summary, Roundtable on Health Literacy; Hernandez, L., Ed.; National Academies Press: Washington, DC, USA, 2009; pp. 91–98. [Google Scholar]
- Pelikan, J.M. Health-literate healthcare organisations. In International Handbook of Health Literacy. Research, Policy and Practice Across the Lifespan; Okan, O., Bauer, U., Levin-Zamir, D., Pinheiro, P., Sørensen, K., Eds.; Policy Press: Bristol, UK, 2019; pp. 539–553. [Google Scholar]
- Protheroe, J.; Nutbeam, D.; Rowlands, G. Health literacy: A necessity for increasing participation in health care. Br. J. Gen. Pract. 2009, 59, 721–723. [Google Scholar] [CrossRef]
- Personalised Health and Care Framework. Available online: https://www.england.nhs.uk/personalised-health-and-care-framework/ (accessed on 13 July 2019).
- Hippisley-Cox, J.; Vinogradova, Y. Trends in Consultation Rates in General Practice 1995/1996 to 2007/2008: Analysis of the QRESEARCH Database; QResearch and The Information Centre for Health and Social Care: London, UK, 2008. [Google Scholar]
- McMillan, B.; Eastham, R.; Brown, B.; Fitton, R.; Dickinson, D. Primary Care Patient Records in the United Kingdom: Past, Present, and Future Research Priorities. J. Med. Internet Res. 2018, 20, e11293. [Google Scholar] [CrossRef]
- Dexheimer, J.W.; Talbot, T.R.; Sanders, D.L.; Rosenbloom, S.T.; Aronsky, D. Prompting clinicians about preventive care measures: A systematic review of randomized controlled trials. J. Am. Med. Inform. Assoc. 2008, 15, 311–320. [Google Scholar] [CrossRef] [Green Version]
- Brokel, J.M.; Schwichtenberg, T.J.; Wakefield, D.S.; Ward, M.M.; Shaw, M.G.; Kramer, J.M. Evaluating clinical decision support rules as an intervention in clinician workflows with technology. Comput. Inform. Nurs. 2011, 29, 36–42. [Google Scholar] [CrossRef]
- Hoye, S.; Gjelstad, S.; Lindbaek, M. Effects on antibiotic dispensing rates of interventions to promote delayed prescribing for respiratory tract infections in primary care. Br. J. Gen. Pract. 2013, 63, e777–e786. [Google Scholar] [CrossRef] [Green Version]
- Rowlands, G.; Whitney, D.; Moon, G. Developing and Applying Geographical Synthetic Estimates of Health Literacy in GP Clinical Systems. Int. J. Environ. Res. Public Health 2018, 15, 1709. [Google Scholar] [CrossRef] [Green Version]
- Making the Case for Health Literacy: East Midlands National Demonstrator Site 2016–17. Strategic Report; Health Education England: Leeds, UK, 2017.
- Khangura, S.; Konnyu, K.; Cushman, R.; Grimshaw, J.; Moher, D. Evidence summaries: The evolution of a rapid review approach. Syst. Rev. 2012, 1, 10. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Forsetlund, L.; Bjorndal, A.; Rashidian, A.; Jamtvedt, G.; O’Brien, M.A.; Wolf, F.; Davis, D.; Odgaard-Jensen, J.; Oxman, A.D. Continuing education meetings and workshops: Effects on professional practice and health care outcomes. Cochrane Database Syst. Rev. 2009, CD003030. [Google Scholar] [CrossRef] [PubMed]
- Shojania, K.G.; Jennings, A.; Mayhew, A.; Ramsay, C.R.; Eccles, M.P.; Grimshaw, J. The effects of on-screen, point of care computer reminders on processes and outcomes of care. Cochrane Database Syst. Rev. 2009, CD001096. [Google Scholar] [CrossRef] [PubMed]
- Merlin, T.; Weston, A.; Tooher, R.; Middleton, P.; Salisbury, J.; Coleman, K.; Norris, S.; Grimmer-Somers, K.; Hillier, S. NHMRC Levels of Evidence and Grades for Recommendations for Developers of Clinical Practice Guidelines; National Health and Medical Research Council (Australia): Canberra, Australia, 2009. [Google Scholar]
- SystmOne GP. Available online: https://www.tpp-uk.com/products/systmone/primary-care (accessed on 20 December 2019).
- Voice. About Us. Available online: https://www.voice-global.org/about-us/ (accessed on 3 December 2019).
- Parikh, N.S.; Parker, R.M.; Nurss, J.R.; Baker, D.W.; Williams, M.V. Shame and health literacy: The unspoken connection. Patient Educ. Couns. 1996, 27, 33–39. [Google Scholar] [CrossRef]
- Moore, P.M.; Rivera Mercado, S.; Grez Artigues, M.; Lawrie, T.A. Communication skills training for healthcare professionals working with people who have cancer. Cochrane Database Syst. Rev. 2013, CD003751. [Google Scholar] [CrossRef]
- Perry, M.; Draskovic, I.; Lucassen, P.; Vernooij-Dassen, M.; van Achterberg, T.; Rikkert, M.O. Effects of educational interventions on primary dementia care: A systematic review. Int. J. Geriatr. Psychiatry 2011, 26, 1–11. [Google Scholar] [CrossRef]
- Pulsford, D.; Jackson, G.; O’Brien, T.; Yates, S.; Duxbury, J. Classroom-based and distance learning education and training courses in end-of-life care for health and social care staff: A systematic review. Palliat. Med. 2013, 27, 221–235. [Google Scholar] [CrossRef]
- Roque, F.; Herdeiro, M.T.; Soares, S.; Teixeira Rodrigues, A.; Breitenfeld, L.; Figueiras, A. Educational interventions to improve prescription and dispensing of antibiotics: A systematic review. BMC Public Health 2014, 14, 1276. [Google Scholar] [CrossRef] [Green Version]
- Schichtel, M.; Rose, P.W.; Sellers, C. Educational interventions for primary healthcare professionals to promote the early diagnosis of cancer: A systematic review. Educ. Prim. Care 2013, 24, 274–290. [Google Scholar] [CrossRef]
- Vohringer, P.A.; Castro, A.; Martinez, P.; Tala, A.; Medina, S.; Rojas, G. Healthcare team training programs aimed at improving depression management in primary care: A systematic review. J. Affect. Disord. 2016, 200, 142–147. [Google Scholar] [CrossRef]
- Young, T.; Rohwer, A.; Volmink, J.; Clarke, M. What are the effects of teaching evidence-based health care (EBHC)? Overview of systematic reviews. PLoS ONE 2014, 9, e86706. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sikorski, C.; Luppa, M.; Konig, H.H.; van den Bussche, H.; Riedel-Heller, S.G. Does GP training in depression care affect patient outcome?—A systematic review and meta-analysis. BMC Health Serv. Res. 2012, 12, 10. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Holt, T.A.; Thorogood, M.; Griffiths, F. Changing clinical practice through patient specific reminders available at the time of the clinical encounter: Systematic review and meta-analysis. J. Gen. Intern. Med. 2012, 27, 974–984. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Conn, V.S.; Ruppar, T.M.; Enriquez, M.; Cooper, P.S.; Chan, K.C. Healthcare provider targeted interventions to improve medication adherence: Systematic review and meta-analysis. Int. J. Clin. Pract. 2015, 69, 889–899. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Teach-Back. Available online: http://www.nchealthliteracy.org/toolkit/tool5.pdf (accessed on 16 January 2020).
- Chunck and Check. Available online: http://www.healthliteracyplace.org.uk/tools-and-techniques/techniques/chunk-and-check/ (accessed on 16 January 2020).
- The HLS-EU Consortium. Comparative Report on Health Literacy in Eight EU Member States. The European Health Literacy Project 2009–2012. (Second Extended and Revised Version); The HLS-EU Consortium: Gastein, Austria, 2014. [Google Scholar]
- DeWalt, D.; Callahan, L.F.; Hawk, V.H.; Broucksou, K.A.; Hink, A.; Rudd, R.; Brach, C. Health Literacy Universal Precautions Toolkit; Agency for Healthcare Research and Quality U.S. Department of Health and Human Services: Rockville, MD, USA, 2010.
- GP Patient Survey. Available online: https://gp-patient.co.uk (accessed on 13 August 2019).
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rowlands, G.; Tabassum, B.; Campbell, P.; Harvey, S.; Vaittinen, A.; Stobbart, L.; Thomson, R.; Wardle-McLeish, M.; Protheroe, J. The Evidence-Based Development of an Intervention to Improve Clinical Health Literacy Practice. Int. J. Environ. Res. Public Health 2020, 17, 1513. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph17051513
Rowlands G, Tabassum B, Campbell P, Harvey S, Vaittinen A, Stobbart L, Thomson R, Wardle-McLeish M, Protheroe J. The Evidence-Based Development of an Intervention to Improve Clinical Health Literacy Practice. International Journal of Environmental Research and Public Health. 2020; 17(5):1513. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph17051513
Chicago/Turabian StyleRowlands, Gill, Bimasal Tabassum, Paul Campbell, Sandy Harvey, Anu Vaittinen, Lynne Stobbart, Richard Thomson, Mandy Wardle-McLeish, and Joanne Protheroe. 2020. "The Evidence-Based Development of an Intervention to Improve Clinical Health Literacy Practice" International Journal of Environmental Research and Public Health 17, no. 5: 1513. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph17051513





