Influence of Face Masks on the Use of Contact Lenses
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Data Collection
- Frequency of use and hours of wear of contact lenses (CL) before the pandemic (classified as “Daily”, “2–3 days/week”, and “Sporadically”)
- Current frequency of use and hours of use of CL (classified as “Daily”, “2–3 days/week”, and “Sporadically”)
- 2.1
- If the time of use has varied, explain the reasons.
- Frequency of cleaning routine before and after the pandemic (rated as “Improves”, “Worsens”, and “Stays the same”)
- Symptoms of eye discomfort with the use of contact lenses (rated as “Never”, “Sometimes”, and “Often”) and with the mask (rated as “Improves”, “Worsens”, and “Stays the same”)
- Foreign body sensation, dryness, irritation, itching, or burning with the use of contact lenses (rated as “Never”, “Sometimes”, and “Often”) and with the mask (rated as “Improves”, “Worsens”, and “Stays the same”).
- Eye dryness with the use of contact lenses (rated as “Never”, “Sometimes”, and “Often”) and with the mask (rated as “Improves”, “Worsens”, and “Stays the same”)
- Sensation of blurriness with the use of contact lenses (rated as “Never”, “Sometimes”, and “Often”) and with the mask (rated as “Improves”, “Worsens”, and “Stays the same”).
- Need to close the eyes due to ocular discomfort with the use of contact lenses (rated as “Never”, “Sometimes”, and “Often”) and with the mask (rated as “Improves”, “Worsens”, and “Stays the same”)
- Need to remove contact lenses due to eye discomfort (rated as “Never”, “Sometimes”, and “Often”) and with the mask (rated as “Better”, “Worse”, and “Stays the same”)
2.2. Statistical Analysis
3. Results
3.1. Descriptive Analysis
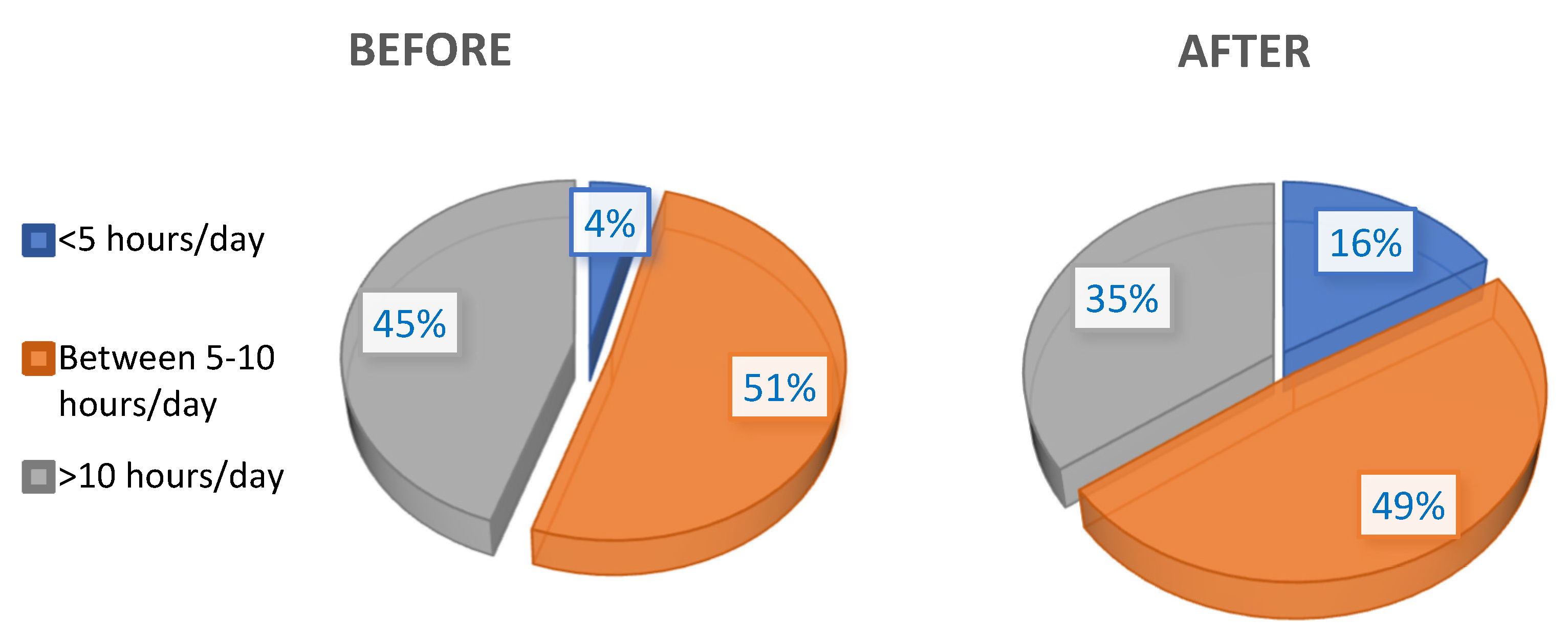
3.2. CL Usage Frequency
3.3. Eye Symptoms
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- WHO Coronavirus (COVID-19) Dashboard. Available online: https://covid19.who.int/ (accessed on 6 May 2021).
- Seah, I.Y.J.; Anderson, D.E.; Kang, A.E.Z.; Wang, L.; Rao, P.; Young, B.E.; Lye, D.C.; Agrawal, R. Assessing Viral Shedding and Infectivity of Tears in Coronavirus Disease 2019 (COVID-19) Patients. Ophthalmology 2020, 127, 977–979. [Google Scholar] [CrossRef]
- Zhou, Y.; Duan, C.; Zeng, Y.; Tong, Y.; Nie, Y.; Yang, Y.; Chen, Z.; Chen, C. Ocular Findings and Proportion with Conjunctival SARS-COV-2 in COVID-19 Patients. Ophthalmology 2020, 127, 982–983. [Google Scholar] [CrossRef]
- Zhou, L.; Xu, Z.; Castiglione, G.M.; Soiberman, U.S.; Eberhart, C.G.; Duh, E.J. ACE2 and TMPRSS2 are expressed on the human ocular surface, suggesting susceptibility to SARS-CoV-2 infection. Ocul. Surf. 2020, 18, 537–544. [Google Scholar] [CrossRef] [PubMed]
- Grixti, A.; Sadri, M.; Datta, A.V. Uncommon ophthalmologic disorders in intensive care unit patients. J. Crit. Care 2012, 27, 746–e9. [Google Scholar] [CrossRef] [PubMed]
- Alansari, M.A.; Hijazi, M.H.; Maghrabi, K.A. Making a Difference in Eye Care of the Critically Ill Patients. J Intensive Care Med. 2015, 30, 311–317. [Google Scholar] [CrossRef] [PubMed]
- Fraunfelder, F.W.; Rosenbaum, J.T. Drug-induced uveitis. Incidence, prevention and treatment. Drug Saf. 1997, 17, 197–207. [Google Scholar] [CrossRef] [PubMed]
- Wang, Q.; Yu, C. Letter to editor: Role of masks/respirator protection against 2019-novel coronavirus (COVID-19). Infect. Control. Hosp. Epidemiol. 2020, 1–2. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Feng, S.; Shen, C.; Xia, N.; Song, W.; Fan, M.; Cowling, B. Rational use of face masks in the COVID-19 pandemic. Lancet Respir. Medicine. 2020, 5, 434–436. [Google Scholar] [CrossRef]
- Schünemann, H.J.; Akl, E.A.; Chou, R.; Chu, D.K.; Loeb, M.; Lotfi, T.; Mustafa, R.A.; Neumann, I.; Saxinger, L.; Sultan, S.; et al. Use of facemasks during the COVID-19 pandemic. Lancet Respir. Med. 2020, 8, 954–955. [Google Scholar] [CrossRef]
- Koh, S.; Rhee, M.K. COVID-19 and Dry Eye. Eye Contact Lens. 2021, 47, 317–322. [Google Scholar] [CrossRef]
- Giannaccare, G.; Vaccaro, S.; Mancini, A.; Scorcia, V. Dry eye in the COVID-19 era: How the measures for controlling pandemic might harm ocular surface. Graefes Arch. Clin. Exp. Ophthalmol. 2020, 258, 2567–2568, PMID: 32561978PMCID: PMC7304378. [Google Scholar] [CrossRef]
- Moshirfar, M.; West, W.B.; Marx, D.P. Face mask-associated ocular irritation and dryness. Ophthalmol Ther. 2020, 9, 397–400. [Google Scholar] [CrossRef] [PubMed]
- MADE: A New Coronavirus-Associated Eye Disease. Available online: https://0-www-healio-com.brum.beds.ac.uk/news/ophthalmology/20200622/ blog-a-new-coronavirusassociated-eye-disease (accessed on 6 May 2021).
- Practitioners Should Be Aware of Mask-Associated Dry Eye (MADE). Available online: https://eyewire.news/articles/ core-alerts-practitioners-to-mask-associated-dry-eye-made/ (accessed on 6 May 2021).
- Pandey, S.K.; Sharma, V. Mask-associated dry eye disease and dry eye due to prolonged screen time: Are we heading towards a new dry eye epidemic during the COVID-19 era? Indian, J. Ophthalmol. 2021, 69, 448–449. [Google Scholar] [CrossRef] [PubMed]
- Margrain, T.H.; Owen, C. The misting characteristics of spectacle lenses. Ophthalmic Physiol. Opt. 1996, 16, 108–114. [Google Scholar] [CrossRef] [PubMed]
- Crebolder, J.M.; Sloan, R.B. Determining the effects of eyewear fogging on visual task performance. Appl. Ergon. 2004, 35, 371–381. [Google Scholar] [CrossRef]
- Matusiak, Ł.; Szepietowska, M.; Krajewski, P.; Białynicki-Birula, R.; Szepietowski, J.C. Inconveniences due to the use of face masks during the COVID-19 pandemic: A survey study of 876 young people. Dermatol Ther. 2020, 33, e13567. [Google Scholar] [CrossRef]
- Lu, P.; Chen, X.; Liu, X.; Yu, L.; Kang, Y.; Xie, Q.; Ke, L.; Wei, X. Dry eye syndrome in elderly Tibetans at high altitude: A population-based study in China. Cornea 2008, 27, 545–551. [Google Scholar] [CrossRef]
- Jie, Y.; Xu, L.; Wu, Y.Y.; Jonas, J.B. Prevalence of dry eye among adult Chinese in the Beijing Eye Study. Eye 2009, 23, 688–693. [Google Scholar] [CrossRef] [Green Version]
- Tian, Y.J.; Liu, Y.; Zou, H.D.; Jiang, Y.J.; Liang, X.Q.; Sheng, M.J.; Li, B.; Xu, X. Epidemiologic study of dry eye in populations equal or over 20 years old in Jiangning District of Shanghai. Zhonghua Yan Ke Za Zhi 2009, 45, 486–491. [Google Scholar] [PubMed]
- Tong, L.; Saw, S.M.; Lamoureux, E.L.; Wang, J.J.; Rosman, M.; Tan, D.T.; Wong, T.Y. A questionnaire-based assessment of symptoms associated with tear film dysfunction and lid margin disease in an Asian population. Ophthalmic Epidemiol. 2009, 16, 31–37. [Google Scholar] [CrossRef]
- Tan, L.L.; Morgan, P.; Cai, Z.Q.; Straughan, R.A. Prevalence of and risk factors for symptomatic dry eye disease in Singapore. Clin Exp Optom. 2015, 98, 45–53. [Google Scholar] [CrossRef] [PubMed]
- Viso, E.; Rodriguez-Ares, M.T.; Gude, F. Prevalence of and associated factors for dry eye in a Spanish adult population (the Salnes Eye Study). Ophthalmic Epidemiol. 2009, 16, 15–21. [Google Scholar] [CrossRef] [PubMed]
- Paulsen, A.J.; Cruickshanks, K.J.; Fischer, M.E.; Huang, G.H.; Klein, B.E.; Klein, R.; Dalton, D.S. Dry eye in the beaver dam offspring study: Prevalence, risk factors, and health-related quality of life. Am. J. Ophthalmol. 2014, 157, 799–806. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vehof, J.; Kozareva, D.; Hysi, P.G.; Hammond, C.J. Prevalence and risk factors of dry eye disease in a British female cohort. Br J. Ophthalmol. 2014, 98, 1712–1717. [Google Scholar] [CrossRef] [PubMed]
- Na, K.S.; Han, K.; Park, Y.G.; Na, C.; Joo, C.K. Depression, Stress, Quality of Life, and Dry Eye Disease in Korean Women: A Population-Based Study. Cornea. 2015, 34, 733–738. [Google Scholar] [CrossRef]
- Malet, F.; Le Goff, M.; Colin, J.; Schweitzer, C.; Delyfer, M.N.; Korobelnik, J.F.; Rougier, M.B.; Radeau, T.; Dartigues, J.F.; Delcourt, C. Dry eye disease in French elderly subjects: The Alienor Study. Acta Ophthalmol. 2014, 92, e429–e436. [Google Scholar] [CrossRef]
- Han, S.B.; Hyon, J.Y.; Woo, S.J.; Lee, J.J.; Kim, T.H.; Kim, K.W. Prevalence of dry eye disease in an elderly Korean population. Arch Ophthalmol. 2011, 129, 633–638. [Google Scholar] [CrossRef] [Green Version]
- Pombo, A.; Luz, C.; Rodrigues, L.P.; Cordovil, R. Effects of COVID-19 Confinement on the Household Routines of Children in Portugal. J. Child. Fam. Stud. 2021, 1–11. [Google Scholar] [CrossRef]
- Pesudovs, K.; Burr, J.M.; Harley, C.; Elliott, D.B. The development, assessment, and selection of questionnaires. Optom Vis Sci. 2007, 84, 663–674. [Google Scholar] [CrossRef] [Green Version]
- Nichols, J.J.; Willcox, M.D.; Bron, A.J.; Belmonte, C.; Ciolino, J.B.; Craig, J.P.; Dogru, M.; Foulks, G.N.; Jones, L.; Nelson, J.D.; et al. The TFOS International Workshop on Contact Lens Discomfort. The TFOS International Workshop on Contact Lens Discomfort: Executive summary. Invest Ophthalmol. Vis. Sci. 2013, 54, TFOS7–TFOS13. [Google Scholar] [CrossRef] [Green Version]
- Salinas, R.; Puig, M.; Fry, C.L.; Johnson, D.A.; Kheirkhah, A. Floppy eyelid syndrome: A comprehensive review. Ocul. Surf. 2020, 18, 31–39. [Google Scholar] [CrossRef] [PubMed]
- Singh, N.P.; Walker, R.J.; Cowan, F.; Davidson, A.C.; Roberts, D.N. Retrograde air escape via the nasolacrimal system: A previously unrecognized complication of continuous positive airway pressure in the management of obstructive sleep apnea. Ann. Otol. Rhinol. Laryngol. 2014, 123, 321–324. [Google Scholar] [CrossRef] [PubMed]
- Alves, M.; Novaes, P.; Morraye, A.; Reinach, P.S.; Rocha, E.M. Is dry eye an environmental disease? Arq. Bras Oftalmol. 2014, 77, 193–200. [Google Scholar] [CrossRef] [Green Version]
- Wolkoff, P.; Skov, P.; Franck, C.; Petersen, L.N. Eye irritation and environmental factors in the office environment--hypotheses, causes and a physiological model. Scand. J. Work Environ. Health 2003, 29, 411–430. [Google Scholar] [CrossRef] [Green Version]
- Nakamura, S.; Shibuya, M.; Nakashima, H.; Hisamura, R.; Masuda, N.; Imagawa, T.; Uehara, M.; Tsubota, K. Involvement of oxidative stress on corneal epithelial alterations in a blink-suppressed dry eye. Invest Ophthalmol. Vis. Sci. 2007, 48, 1552–1558. [Google Scholar] [CrossRef]
- Chen, X.; Gallar, J.; Pozo, M.A.; Baeza, M.; Belmonte, C. CO2 stimulation of the cornea: A comparison between human sensation and nerve activity in polymodal nociceptive afferents of the cat. Eur. J. Neurosci. 1995, 7, 1154–1163. [Google Scholar] [CrossRef]
- Nichols, J.J.; Mitchell, G.L.; Nichols, K.K. An assessment of self-reported disease classification in epidemiological studies of dry eye. Invest Ophthalmol. Vis. Sci. 2004, 45, 3453–3457. [Google Scholar] [CrossRef] [Green Version]
- Gulati, A.; Sullivan, R.; Buring, J.E.; Sullivan, D.A.; Dana, R.; Schaumberg, D.A. Validation and repeatability of a short questionnaire for dry eye syndrome. Am. J. Ophthalmol. 2006, 142, 125–131. [Google Scholar] [CrossRef] [PubMed]
- Begley, C.G.; Caffery, B.; Chalmers, R.L.; Mitchell, G.L.; Dry Eye Investigation (DREI) Study Group. Use of the dry eye questionnaire to measure symptoms of ocular irritation in patients with aqueous tear deficient dry eye. Cornea 2002, 21, 664–670. [Google Scholar] [CrossRef]
- Grubbs, J., Jr.; Huynh, K.; Tolleson-Rinehart, S.; Weaver, M.A.; Williamson, J.; Lefebvre, C.; Davis, R.M. Instrument development of the UNC Dry Eye Management Scale. Cornea. 2014, 33, 1186–1192. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Simpson, T.L.; Situ, P.; Jones, L.W.; Fonn, D. Dry eye symptoms assessed by four questionnaires. Optom Vis Sci. 2008, 85, 692–699. [Google Scholar] [CrossRef]
- Oden, N.L.; Lilienfeld, D.E.; Lemp, M.A.; Nelson, J.D.; Ederer, F. Sensitivity and specificity of a screening questionnaire for dry eye. Adv. Exp. Med. Biol. 1998, 438, 807–820. [Google Scholar] [CrossRef]
- Ngo, W.; Situ, P.; Keir, N.; Korb, D.; Blackie, C.; Simpson, T. Psychometric properties and validation of the Standard Patient Evaluation of Eye Dryness questionnaire. Cornea 2013, 32, 1204–1210. [Google Scholar] [CrossRef]
- Sun, C.B.; Wang, Y.Y.; Liu, G.H.; Liu, Z. Role of the Eye in Transmitting Human Coronavirus: What We Know and What We Do Not Know. Front Public Health 2020, 8, 155. [Google Scholar] [CrossRef] [Green Version]
- Li, J.O.; Lam, D.S.C.; Chen, Y.; Ting, D.S.W. Novel Coronavirus disease 2019 (COVID-19): The importance of recognising possible early ocular manifestation and using protective eyewear. Br. J. Ophthalmol. 2020, 104, 297–298. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wu, P.; Duan, F.; Luo, C.; Liu, Q.; Qu, X.; Liang, L.; Wu, K. Characteristics of Ocular Findings of Patients with Coronavirus Disease 2019 (COVID-19) in Hubei Province, China. JAMA Ophthalmol. 2020, 138, 575–578. [Google Scholar] [CrossRef] [PubMed]
- Pritchard, N.; Fonn, D.; Brazeau, D. Discontinuation of contact lens wear: A survey. Int. Contact Lens. Clin. 1999, 26, 157–162. [Google Scholar] [CrossRef]
- Begley, C.G.; Chalmers, R.L.; Mitchell, G.L.; Nichols, K.K.; Caffery, B.; Simpson, T.; DuToit, R.; Portello, J.; Davis, L. Characterization of ocular surface symptoms from optometric practices in North America. Cornea 2001, 20, 610–618. [Google Scholar] [CrossRef]
- Riley, C.; Young, G.; Chalmers, R. Prevalence of ocular surface symptoms, signs, and uncomfortable hours of wear in contact lens wearers: The effect of refitting with daily-wear silicone hydrogel lenses (senofilcon a). Eye Contact Lens. 2006, 32, 281–286. [Google Scholar] [CrossRef] [Green Version]
- Kaštelan, S.; Lukenda, A.; Salopek-Rabatić, J.; Pavan, J.; Gotovac, M. Dry eye symptoms and signs in long-term contact lens wearers. Coll Antropol. 2013, 37, 199–203. [Google Scholar] [PubMed]
- Boccardo, L. Self-reported symptoms of mask-associated dry eye: A survey study of 3,605 people. Cont Lens Anterior Eye. 2021, 101408. [Google Scholar] [CrossRef] [PubMed]
- Nasiri, N.; Sharifi, H.; Bazrafshan, A.; Noori, A.; Karamouzian, M.; Sharifi, A. Ocular Manifestations of COVID-19: A Systematic Review and Meta-analysis. J. Ophthalmic. Vis. Res. 2021, 16, 103–112. [Google Scholar] [CrossRef] [PubMed]



Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Martinez-Perez, C.; Monteiro, B.; Soares, M.; Portugues, F.; Matos, S.; Ferreira, A.; Alvarez-Peregrina, C.; Sánchez-Tena, M.Á. Influence of Face Masks on the Use of Contact Lenses. Int. J. Environ. Res. Public Health 2021, 18, 7407. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph18147407
Martinez-Perez C, Monteiro B, Soares M, Portugues F, Matos S, Ferreira A, Alvarez-Peregrina C, Sánchez-Tena MÁ. Influence of Face Masks on the Use of Contact Lenses. International Journal of Environmental Research and Public Health. 2021; 18(14):7407. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph18147407
Chicago/Turabian StyleMartinez-Perez, Clara, Bruno Monteiro, Mafalda Soares, Fatima Portugues, Sonia Matos, Ana Ferreira, Cristina Alvarez-Peregrina, and Miguel Ángel Sánchez-Tena. 2021. "Influence of Face Masks on the Use of Contact Lenses" International Journal of Environmental Research and Public Health 18, no. 14: 7407. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph18147407







