1. Introduction
Mindfulness is commonly understood as the ability of being open, accepting, and present in the moment [
1]. Mindfulness trainings such as Mindfulness-Based Stress Reduction (MBSR), Mindfulness-Based Cognitive Therapy (MBCT), Acceptance and Commitment Therapy (ACT), and Dialectical Behavioral Therapy (DBT) are often described as interventions that focus to promote non-judgmental and moment-to-moment awareness of the present experience. The role of mindfulness in encouraging behaviors related to healthy body weight maintenance and reducing overweight and obesity has gained attention among scholars [
2]. This practice has been beneficial to control food cravings, portion size, body mass index, and body weight [
3]. Mindful eating refers to being conscious of physical sensation and emotion while eating or in a food-related environment [
1]. It helps in improving one’s sensitivity to the physical cues of hunger, satiety, eating speed, and the food atmosphere [
3]. These cues are crucial to self-regulate one’s desire to consume high-calorie foods. Studies have shown that mindful eating helps in reducing negative eating behaviors, sweets consumption, and serving sizes of energy-dense foods [
4,
5,
6].
There are many factors associated with eating behaviors, such as physiological (i.e., chronotype), social (i.e., coworker influence), environmental, and psychological (i.e., stress, mood) [
7,
8,
9]. It has been hypothesized that obesity-related eating behaviors are partially associated with the inability to identify and respond to internal cues of hunger and satiety [
10,
11] (pp. 75–91), [
12] (pp. 913–933). This lack of response to internal cues is correlated with increased overeating episodes and a greater risk for weight gain [
13,
14,
15]. In addition, emotional dysregulation has been associated with emotional and stress eating [
16,
17,
18,
19]. Studies have shown that compulsive overeating and higher preference for high calorie, fat, sugar, and/or high sodium foods are the result of negative emotions and acute stress [
20,
21,
22]. Emotional eating has been shown to be a strong indicator of obesity and is negatively associated with weight loss and its maintenance [
23,
24,
25]. Furthermore, a restricted diet and increased physical activity can result in physiological discomforts that may impose an added barrier to long-term weight loss [
24].
There are several tools available in measuring eating behaviors such as Night Eating Syndrome Questionnaire (NEQ), Three-Factor Eating Questionnaire (TFEQ) and Binge Eating Scale (BES). The Mindful Eating Questionnaire (MEQ) is the first scale developed by Framson and colleagues that measures mindful eating [
1]. It is a 28-item self-report instrument that consists of five mindful eating domains: awareness, disinhibition, distraction, emotional response, and external cues. This questionnaire has been validated previously among healthy adults aged 18 to 80 years old. The study showed good internal consistency with a reliability of 0.64 for the MEQ score [
1]. In addition, each subscale had internal consistency ranging from 0.64 to 0.83. It was also reported that there were modest (0.14) to moderate (0.47) correlation among all subscales with the exception of correlation between external cues and emotional response. Another validation study among overweight and obese pregnant women yielded the same five domains of the MEQ [
26]. It was found that the MEQ has poor internal consistency reliability of the summary score (0.56). As for the subscales, only the external cues subscale was not internally consistent with Cronbach’s alpha of 0.31. Its reliability was further supported by test-retest analysis, where the total and subscale scores were ranged between 0.62 to 0.85. To add, positive correlations were also observed between the MEQ subscales and the Mindful Attention Awareness Scale (MAAS) [
26]. Another study of the Persian version of MEQ among women seeking weight loss reported satisfactory internal consistency for the total score and the subscales (0.73–0.81) and satisfactory test-retest reliability ranging from 0.73 to 0.91. [
27]. Its construct validity analysis resulted in five domains which were similar to the original study. Contrary, the Italian version of the MEQ resulted in a 20-item pool where only two domains emerged; awareness and recognition [
28]. Clementi et al. also found that both domains have satisfactory internal and test-retest reliability, and were associated with general mindfulness. Meanwhile, the MAAS is a standard tool used to assess mindfulness in everyday life among the general population [
29]. It consists of a 15-item self-reported single-factor scale that focused on the mindfulness construct’s attention awareness component.
The prevalence of overweight and obesity had significantly increased between 1976 and 2016 globally, in which half of them (52%) were adults over 18 years of age [
30]. In Malaysia, the National Health and Morbidity Survey (NHMS) reported that the prevalence of overweight and obesity among adults increased by 5% from 2011 to 2015 [
31,
32]. Moreover, the prevalence by age in 2015 showed an increasing trend from 34.8% among 18–29 years to 60.2% among 50–59 years. Obesity is associated with increased risk of many non-communicable diseases (NCDs), including diabetes, cardiovascular disease, depression, some cancers, and respiratory disease [
33,
34,
35,
36,
37]. Moreover, it negatively impacts bone health, quality of life, and functional capacity [
38,
39,
40]. Consequently, obesity is also associated with expensive health care costs [
41,
42,
43]. One study suggested that obese adults have difficulty in reflecting on the impact of obesity on their social and relational functioning despite having psychological difficulties [
44]. Considering the increasing trend in obesity prevalence in Malaysia, a locally validated instrument is essential in conducting research and intervention activities. To the best of our knowledge, no measure has been carried out to assess mindful eating behavior in Malaysia’s overweight and obese adults. Moreover, there is currently no instrument measuring mindful eating (in general) in the Malaysian context using its local language. Several studies have shown that eating mindfully was associated with a lower BMI [
45,
46] and reduced body weight [
47]. Thus, the objective of our present study was to determine the reliability and validity of the MEQ-M in a sample of overweight and obese adults. This is the first study to examine the reliability and validity of the Mindful Eating Questionnaire (MEQ) among this population. We hypothesized that the MEQ would have similar results to a previous study [
40] where the questionnaire would be valid and reliable among overweight and obese Malaysian adults. As mindful eating was generally associated with general mindfulness in previous studies, we hypothesized that the MEQ-M total score would be positively correlated with the Mindful Attention Awareness Scale (MAAS).
4. Discussion
The purpose of this study was to analyze the psychometric properties of the MEQ in overweight and obese Malaysian adult samples. This paper reports the translation procedure, validity, and reliability of the Malay-translated MEQ.
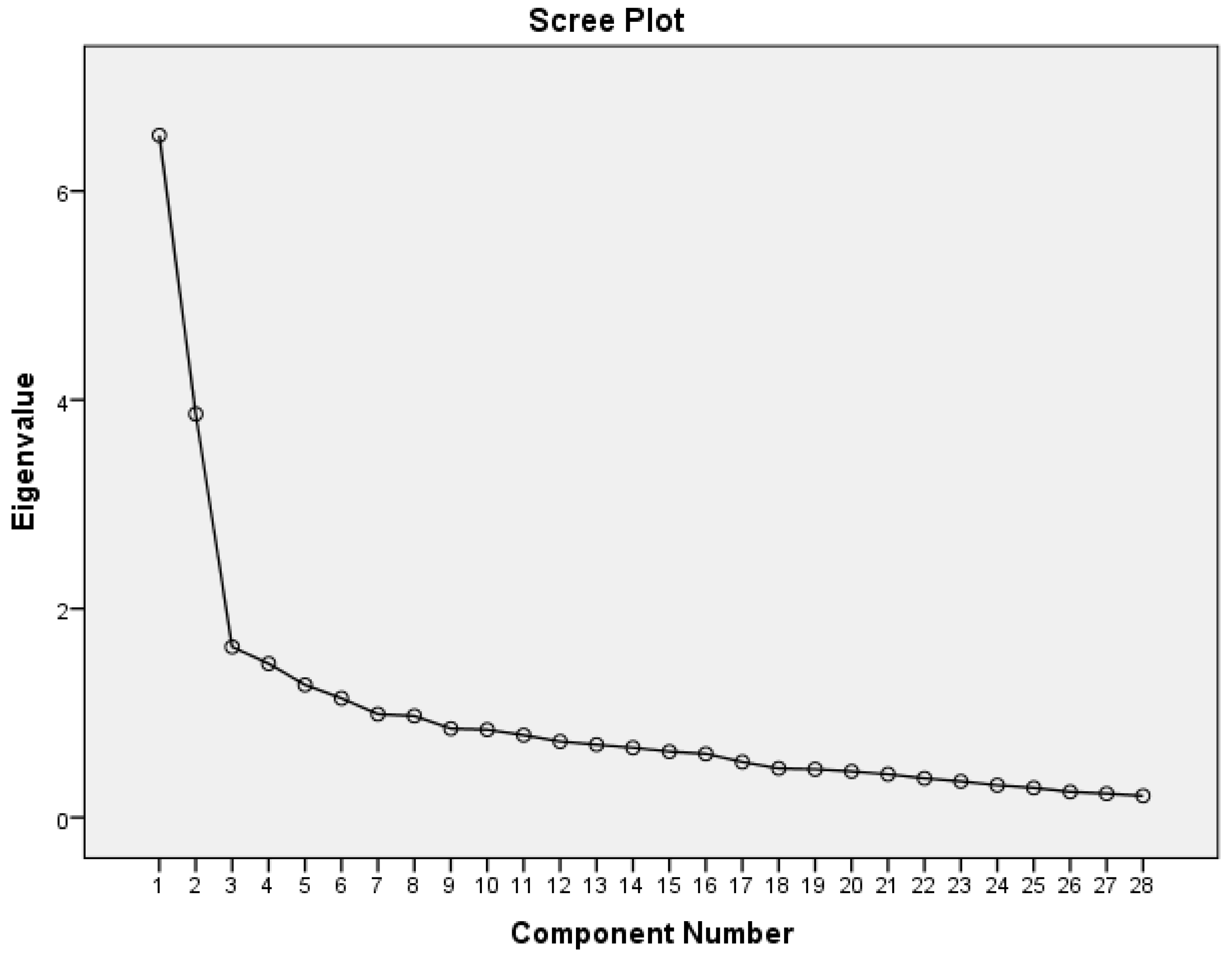
Construct validity (EFA) results were inconsistent with findings reported in previous studies [
1,
27]. These studies found that the 28-item MEQ had a good fit for a five-dimensional factor structure. On the contrary, we found a seven-dimensional model from the exploration. The seven factors were labeled as Factor 1 (environment disinhibition), Factor 2 (emotional response), Factor 3 (taste awareness), Factor 4 (emotion awareness), Factor 5 (portion disinhibition), Factor 6 (external cues of food), and Factor 7 (external cues of place). Each factor was loaded strongly with factor loadings from 0.43 to 0.79. Items 7, 13, and 26 had multiple cross-loading. If a more stringent factor loading was used at the cut-off point of 0.5 (25% shared variances), items 4 and 27 of the MEQ would be dropped and, it would become a 26-item scale. This yielded a six-dimensional model for the Malay-translated MEQ. A possible reason that this study produced a seven-dimensional model, in contrast to other studies, is due to cultural differences. Our population study might have had a different understanding of mindfulness. Studies have shown that cognitive and reasoning styles are different across cultures and may affect how questions are viewed and answered [
56,
57]. Language and cross-cultural variations may influence the respondents’ responses and affect the analysis of the questionnaire’s psychometric properties [
58].
The Cronbach’s alpha and McDonald’s omega analysis showed that the Malay-translated MEQ was a reliable tool to be used among this group. The internal consistencies of the MEQ-M factors ranged from 0.54 to 0.70 for Cronbach’s alpha and 0.58 to 0.80 for McDonald’s omega, except for the External Cues subscales. This indicates that each factor’s items are moderately cohesive with each other in measuring specific mindful eating behavior. The low internal consistency of Factor 6 may be due to the small number of items. The internal consistency of Factor 7 could not be tested as there was only one item (Item 8) extracted. When item 8 was analyzed together with items 4 and 23 from Factor 6, the Cronbach’s alpha produced was 0.441. Exclusion of item 4, 8, and 23 (External Cues subscales) from the analysis has improved the reliability of the MEQ-M. Similarly, the external cues subscale was found to be invalid in a study among overweight and obese pregnant women [
26]. The MEQ-M summary scale was 0.64, which is comparable to that reported by Abbaspoor (0.66) and Framson (0.64). In contrast, our findings showed better reliability compared to Apolzan and colleagues [
26].
The test-retest reliability of the MEQ with an eight-week interval showed only a small agreement between the items. Three subscales (environmental disinhibition, emotional response, and taste awareness) achieved a fair correlation (0.26 to 0.45). In contrast, emotional awareness, portion disinhibition, external cues of food, and external cues of place subscales had a small correlation coefficient. We also found that portion disinhibition and external cues subscales had a negative ICC value due to a negative average covariance among items. This may have affected the overall ICC of the MEQ (0.10). A small ICC means that the items’ measurement was not stable over time. The Iranian version of the MEQ test-retest reliability had a high level of correlation, where all subscales’ ICC was ≥0.7 [
27]. This discrepancy may be due to the different sample populations tested only among women with normal BMI. The ICC could be improved if a sizeable heterogeneous sample in terms of BMI was included. Moreover, they retested the questionnaire in a shorter period (four weeks) compared to the present study.
In correlation to MAAS, the MEQ correlated positively except for Factor 3, 6, and 7. However, the correlation was weak. This may suggest that individuals with higher mindfulness may or may not tend to eat mindfully. In contrast, MEQ was significantly correlated with MAAS among pregnant women [
26]. The differences may be due to the new factors or domains produced from our study compared to the original MEQ which consists of only five factors. Other than that, the MAAS questionnaire focused exclusively on the attention awareness component of the mindfulness construct, whereas the MEQ includes constructs of eating behaviors and mindfulness. In our cultural context, this may reflect that these measures are not related to each other. Our study also found that there was no significant correlation between BMI and the MEQ-M’s subscales, except for the inverse relationship with the Environmental disinhibition subscale. This suggests that higher BMI was correlated with lower ability to stop eating even though they already feel full. Similarly, the subscales of the Iranian version of the MEQ also showed no correlation with BMI apart from the Awareness subscale [
27]. In contrast, Framson et al. found that the overall scores of the MEQ was negatively associate with BMI [
1].
This study was the first to establish the validity and reliability of the MEQ-M among overweight and obese healthy working adults. Since this study was conducted among overweight and obese adults, this limits the generalizability of the results to the general population. Furthermore, this instrument was a self-reported questionnaire. The respondents might have had difficulties with being aware of their eating experience when that questionnaire was given. They might have provided answers describing what they should do instead. In addition, there was no concurrent validation of the MEQ-M with other eating psychopathology, such as the binge eating scale and three-factor eating questionnaire, which may provide additional support for MEQ-M’s validation.