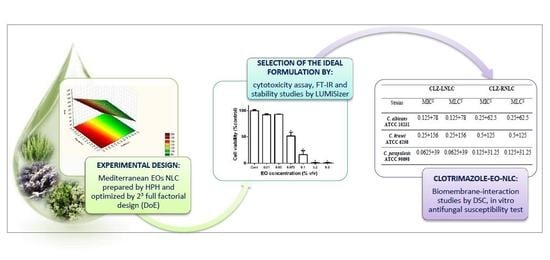
Clotrimazole-Loaded Mediterranean Essential Oils NLC: A Synergic Treatment of Candida Skin Infections
Abstract
:1. Introduction
2. Materials and Methods
2.1. Materials
2.2. Nanoparticles Production
2.3. Design of Experiment (DOE)
2.4. Dynamic Light Scattering
2.5. EOs Encapsulation Efficiency (EE%)
2.6. In Vitro Cell Viability Studies
2.7. Fourier Transform-Infrared (FT-IR) Analysis
2.8. Accelerated Characterization of Formulation Stability
2.9. Drug Encapsulation Efficiency (EE), Loading Capacity (LC) and In Vitro Release
2.10. Biomembrane Model Preparation
2.11. Differential Scanning Calorimetry
2.12. In Vitro Antifungal Susceptibility Test
2.13. Statistical Analysis
3. Results and Discussion
3.1. NLC optimization for EOs Encapsulations (DoE)
3.2. Biocompatibility of EOs and NLC-EO Using Human Cell Lines
3.3. CLZ-Loaded NLC Prepared with the Selected EOs: Lavandula and Rosmarinus
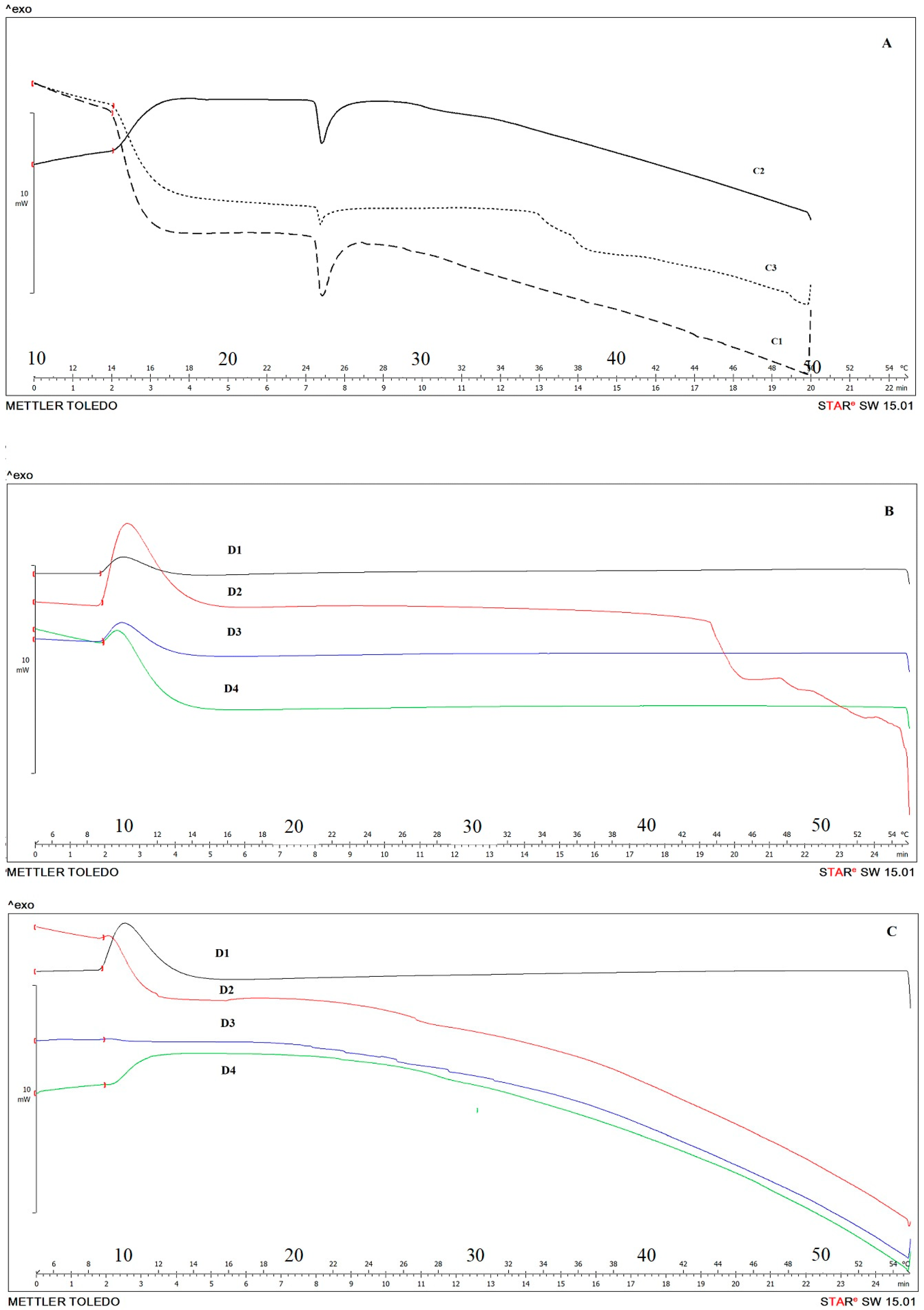
3.4. Pre-Vitro Evaluation of Essential Oils on Biomembrane
3.5. In Vitro Antifungal Susceptibility Test: MIC and MLC Results
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Pfaller, M.A.; Diekema, D.J. Rare and Emerging Opportunistic Fungal Pathogens: Concern for Resistance Beyond Candida albicans and Aspergillus fumigatus. J. Clin. Microbiol. 2004, 42, 4419–4431. [Google Scholar] [CrossRef] [PubMed]
- Williams, D.W.; Kuriyama, T.; Silva, S.; Malic, S.; Lewis, M.A. Candida Biofilms and Oral Candidosis: Treatment and Prevention. Periodontology 2011, 55, 250–265. [Google Scholar] [CrossRef] [PubMed]
- Ben-Ami, R. Treatment of Invasive Candidiasis: A Narrative Review. J. Fungi 2018, 4, 97. [Google Scholar] [CrossRef]
- Costa, C.; Ribeiro, J.; Miranda, I.M.; Silva-Dias, A.; Cavalheiro, M.; Costa-de-Oliveira, S.; Rodrigues, A.G.; Teixeira, M.C. Clotrimazole Drug Resistance in Candida glabrata Clinical Isolates Correlates with Increased Expression of the Drug:H(+) Antiporters Cgaqr1, Cgtpo1_1, Cgtpo3, and Cgqdr2. Front. Microbiol. 2016, 7, 526. [Google Scholar] [CrossRef] [PubMed]
- Pelletier, R.; Peter, J.; Antin, C.; Gonzalez, C.; Wood, L.; Walsh, T.J. Emergence of Resistance of Candida Albicans to Clotrimazole in Human Immunodeficiency Virus-Infected Children: In vitro and Clinical Correlations. J. Clin. Microbiol. 2000, 38, 1563–1568. [Google Scholar] [PubMed]
- Pfaller, M.A.; Messer, S.A.; Woosley, L.N.; Jones, R.N.; Castanheira, M. Echinocandin and Triazole Antifungal Susceptibility Profiles for Clinical Opportunistic Yeast and Mold Isolates Collected from 2010 to 2011: Application of New Clsi Clinical Breakpoints and Epidemiological Cutoff Values for Characterization of Geographic and Temporal Trends of Antifungal Resistance. J. Clin. Microbiol. 2013, 51, 2571–2581. [Google Scholar] [CrossRef] [PubMed]
- Bakkali, F.; Averbeck, S.; Averbeck, D.; Idaomar, M. Biological Effects of Essential Oils—A Review. Food Chem. Toxicol. 2008, 46, 446–475. [Google Scholar] [CrossRef] [PubMed]
- Bona, E.; Cantamessa, S.; Pavan, M.; Novello, G.; Massa, N.; Rocchetti, A.; Berta, G.; Gamalero, E. Sensitivity of Candida Albicans to Essential Oils: Are They an Alternative to Antifungal Agents? J. Appl. Microbiol. 2016, 121, 1530–1545. [Google Scholar] [CrossRef]
- Altintas, A.; Tabanca, N.; Tyihak, E.; Ott, P.G.; Moricz, A.M.; Mincsovics, E.; Wedge, D.E. Characterization of Volatile Constituents from Origanum Onites and Their Antifungal and Antibacterial Activity. J. AOAC Int. 2013, 96, 1200–1208. [Google Scholar] [CrossRef]
- Hammer, K.A.; Carson, C.F.; Riley, T.V. In-Vitro Activity of Essential Oils, in Particular Melaleuca Alternifolia (Tea Tree) Oil and Tea Tree Oil Products, against Candida Spp. J. Antimicrob. Chemother. 1998, 42, 591–595. [Google Scholar] [CrossRef]
- Pozzatti, P.; Scheid, L.A.; Spader, T.B.; Atayde, M.L.; Santurio, J.M.; Alves, S.H. In vitro Activity of Essential Oils Extracted from Plants Used as Spices against Fluconazole-Resistant and Fluconazole-Susceptible Candida Spp. Can. J. Microbiol. 2008, 54, 950–956. [Google Scholar] [CrossRef] [PubMed]
- Tampieri, M.P.; Galuppi, R.; Macchioni, F.; Carelle, M.S.; Falcioni, L.; Cioni, P.L.; Morelli, I. The Inhibition of Candida Albicans by Selected Essential Oils and Their Major Components. Mycopathologia 2005, 159, 339–345. [Google Scholar] [CrossRef] [PubMed]
- Hosseini, S.F.; Zandi, M.; Rezaei, M.; Farahmandghavi, F. Two-Step Method for Encapsulation of Oregano Essential Oil in Chitosan Nanoparticles: Preparation, Characterization and in vitro Release Study. Carbohydr. Polym. 2013, 95, 50–56. [Google Scholar] [CrossRef]
- Trinetta, V.; Morgan, M.T.; Coupland, J.N.; Yucel, U. Essential Oils against Pathogen and Spoilage Microorganisms of Fruit Juices: Use of Versatile Antimicrobial Delivery Systems. J. Food Sci. 2017, 82, 471–476. [Google Scholar] [CrossRef] [PubMed]
- Carbone, C.; Martins-Gomes, C.; Caddeo, C.; Silva, A.M.; Musumeci, T.; Pignatello, R.; Puglisi, G.; Souto, E.B. Mediterranean Essential Oils as Precious Matrix Components and Active Ingredients of Lipid Nanoparticles. Int. J. Pharm. 2018, 548, 217–226. [Google Scholar] [CrossRef] [PubMed]
- Fazly Bazzaz, B.S.; Khameneh, B.; Namazi, N.; Iranshahi, M.; Davoodi, D.; Golmohammadzadeh, S. Solid Lipid Nanoparticles Carrying Eugenia Caryophyllata Essential Oil: The Novel Nanoparticulate Systems with Broad-Spectrum Antimicrobial Activity. Lett. Appl. Microbiol. 2018, 66, 506–513. [Google Scholar] [CrossRef] [PubMed]
- Moghimipour, E.; Ramezani, Z.; Handali, S. Solid Lipid Nanoparticles as a Delivery System for Zataria Multiflora Essential Oil: Formulation and Characterization. Curr. Drug Deliv. 2013, 10, 151–157. [Google Scholar] [CrossRef]
- Saporito, F.; Sandri, G.; Bonferoni, M.C.; Rossi, S.; Boselli, C.; Icaro Cornaglia, A.; Mannucci, B.; Grisoli, P.; Vigani, B.; Ferrari, F. Essential Oil-Loaded Lipid Nanoparticles for Wound Healing. Int. J. Nanomed. 2018, 13, 175–186. [Google Scholar] [CrossRef]
- Lai, F.; Wissing, S.A.; Muller, R.H.; Fadda, A.M. Artemisia Arborescens L Essential Oil-Loaded Solid Lipid Nanoparticles for Potential Agricultural Application: Preparation and Characterization. AAPS PharmSciTech 2006, 7, E2. [Google Scholar] [CrossRef]
- Granata, G.; Stracquadanio, S.; Leonardi, M.; Napoli, E.; Consoli, G.M.L.; Cafiso, V.; Stefani, S.; Geraci, C. Essential Oils Encapsulated in Polymer-Based Nanocapsules as Potential Candidates for Application in Food Preservation. Food Chem. 2018, 269, 286–292. [Google Scholar] [CrossRef]
- Esmaeili, A.; Asgari, A. In vitro Release and Biological Activities of Carum Copticum Essential Oil (Ceo) Loaded Chitosan Nanoparticles. Int. J. Biol. Macromol. 2015, 81, 283–290. [Google Scholar] [CrossRef] [PubMed]
- Severino, P.; Santana, M.H.; Souto, E.B. Optimizing SLN and NLC by 2(2) Full Factorial Design: Effect of Homogenization Technique. Mater. Sci. Eng. C Mater. Biol. Appl. 2012, 32, 1375–1379. [Google Scholar] [CrossRef] [PubMed]
- Boukamp, P.; Petrussevska, R.T.; Breitkreutz, D.; Hornung, J.; Markham, A.; Fusenig, N.E. Normal Keratinization in a Spontaneously Immortalized Aneuploid Human Keratinocyte Cell Line. J. Cell Biol. 1988, 106, 761–771. [Google Scholar] [CrossRef] [PubMed]
- Andreani, T.; Kiill, C.P.; de Souza, A.L.; Fangueiro, J.F.; Fernandes, L.; Doktorovova, S.; Santos, D.L.; Garcia, M.L.; Gremiao, M.P.; Souto, E.B.; et al. Surface Engineering of Silica Nanoparticles for Oral Insulin Delivery: Characterization and Cell Toxicity Studies. Colloids Surf. B Biointerfaces 2014, 123, 916–923. [Google Scholar] [CrossRef]
- Hosseini, S.M.; Hosseini, H.; Mohammadifar, M.A.; Mortazavian, A.M.; Mohammadi, A.; Khosravi-Darani, K.; Shojaee-Aliabadi, S.; Dehghan, S.; Khaksar, R. Incorporation of Essential Oil in Alginate Microparticles by Multiple Emulsion/Ionic Gelation Process. Int. J. Biol. Macromol. 2013, 62, 582–588. [Google Scholar] [CrossRef] [PubMed]
- Caddeo, C.; Manconi, M.; Fadda, A.M.; Lai, F.; Lampis, S.; Diez-Sales, O.; Sinico, C. Nanocarriers for Antioxidant Resveratrol: Formulation Approach, Vesicle Self-Assembly and Stability Evaluation. Colloids Surf. B Biointerfaces 2013, 111, 327–332. [Google Scholar] [CrossRef]
- Chang, C.W.; Liao, Y.C. Accelerated Sedimentation Velocity Assessment for Nanowires Stabilized in a Non-Newtonian Fluid. Langmuir 2016, 32, 13620–13626. [Google Scholar] [CrossRef]
- Reference Method for Broth Dilution Antifungal Susceptibility Testing of Yeasts. Approved Standard—Third Edition. Available online: https://clsi.org/media/1461/m27a3_sample.pdf (accessed on 9 April 2019).
- Carbone, C.; Tomasello, B.; Ruozi, B.; Renis, M.; Puglisi, G. Preparation and Optimization of Pit Solid Lipid Nanoparticles Via Statistical Factorial Design. Eur. J. Med. Chem. 2012, 49, 110–117. [Google Scholar] [CrossRef]
- Severino, P.; Andreani, T.; Jager, A.; Chaud, M.V.; Santana, M.H.; Silva, A.M.; Souto, E.B. Solid Lipid Nanoparticles for Hydrophilic Biotech Drugs: Optimization and Cell Viability Studies (Caco-2 & Hepg-2 Cell Lines). Eur. J. Med. Chem. 2014, 81, 28–34. [Google Scholar] [CrossRef]
- Joseph, E.; Reddi, S.; Rinwa, V.; Balwani, G.; Saha, R. Design and in Vivo Evaluation of Solid Lipid Nanoparticulate Systems of Olanzapine for Acute Phase Schizophrenia Treatment: Investigations on Antipsychotic Potential and Adverse Effects. Eur. J. Pharm. Sci. 2017, 104, 315–325. [Google Scholar] [CrossRef]
- Wang, J.J.; Liu, K.S.; Sung, K.C.; Tsai, C.Y.; Fang, J.Y. Lipid Nanoparticles with Different Oil/Fatty Ester Ratios as Carriers of Buprenorphine and Its Prodrugs for Injection. Eur. J. Pharm. Sci. 2009, 38, 138–146. [Google Scholar] [CrossRef]
- Schubert, M.A.; Muller-Goymann, C.C. Solvent Injection as a New Approach for Manufacturing Lipid Nanoparticles--Evaluation of the Method and Process Parameters. Eur. J. Pharm. Biopharm. 2003, 55, 125–131. [Google Scholar] [CrossRef]
- Vitorino, C.; Carvalho, F.A.; Almeida, A.J.; Sousa, J.J.; Pais, A.A. The Size of Solid Lipid Nanoparticles: An Interpretation from Experimental Design. Colloids Surf. B Biointerfaces 2011, 84, 117–130. [Google Scholar] [CrossRef]
- Zhang, S.; Tang, C.; Yin, C. Effects of Poly(Ethylene Glycol) Grafting Density on the Tumor Targeting Efficacy of Nanoparticles with Ligand Modification. Drug Deliv. 2015, 22, 182–190. [Google Scholar] [CrossRef]
- Patravale, V.B.; Date, A.A.; Kulkarni, R.M. Nanosuspensions: A Promising Drug Delivery Strategy. J. Pharm. Pharmacol. 2004, 56, 827–840. [Google Scholar] [CrossRef]
- Cavanagh, H.; Wilkinson, J. Biological Activities of Lavender Essential Oil. Phytother. Res. 2002, 16, 301–308. [Google Scholar] [CrossRef]
- Sivropoulou, A.; Papanikolaou, E.; Nikolaou, C.; Kokkini, S.; Lanaras, T.; Arsenakis, M. Antimicrobial and Cytotoxic Activities of Origanum Essential Oils. J. Agric. Food Chem. 1996, 44, 1202–1205. [Google Scholar] [CrossRef]
- Khosravi, A.R.; Sharifzadeh, A.; Nikaein, D.; Almaie, Z.; Gandomi Nasrabadi, H. Chemical Composition, Antioxidant Activity and Antifungal Effects of Five Iranian Essential Oils against Candida Strains Isolated from Urine Samples. J. Mycol. Med. 2018. [Google Scholar] [CrossRef]
- Sabzevari, O.; Hatcher, M.; Kentish, P.; OSullivan, M.; Gibson, G.G. Bifonazole, but Not the Structurally-Related Clotrimazole, Induces Both Peroxisome Proliferation and Members of the Cytochrome P4504a Sub-Family in Rat Liver. Toxicology 1996, 106, 19–26. [Google Scholar] [CrossRef]
- Ibrahim, W.M.; AlOmrani, A.H.; Yassin, A.E. Novel Sulpiride-Loaded Solid Lipid Nanoparticles with Enhanced Intestinal Permeability. Int. J. Nanomed. 2014, 9, 129–144. [Google Scholar] [CrossRef]
- Tonglairoum, P.; Ngawhirunpat, T.; Rojanarata, T.; Panomsuk, S.; Kaomongkolgit, R.; Opanasopit, P. Fabrication of Mucoadhesive Chitosan Coated Polyvinylpyrrolidone/Cyclodextrin/Clotrimazole Sandwich Patches for Oral Candidiasis. Carbohydr. Polym. 2015, 132, 173–179. [Google Scholar] [CrossRef]
- Xu, D.; Qi, Y.; Wang, X.; Li, X.; Wang, S.; Cao, Y.; Wang, C.; Sun, B.; Decker, E.; Panya, A. The Influence of Flaxseed Gum on the Microrheological Properties and Physicochemical Stability of Whey Protein Stabilized Beta-Carotene Emulsions. Food Funct. 2017, 8, 415–423. [Google Scholar] [CrossRef] [PubMed]
- Carbone, C.; Campisi, A.; Musumeci, T.; Raciti, G.; Bonfanti, R.; Puglisi, G. Fa-Loaded Lipid Drug Delivery Systems: Preparation, Characterization and Biological Studies. Eur. J. Pharm. Sci. 2014, 52, 12–20. [Google Scholar] [CrossRef] [PubMed]
- Montenegro, L.; Carbone, C.; Puglisi, G. Vehicle Effects on in vitro Release and Skin Permeation of Octylmethoxycinnamate from Microemulsions. Int. J. Pharm. 2011, 405, 162–168. [Google Scholar] [CrossRef] [PubMed]
- Borghi, E.; Borgo, F.; Morace, G. Fungal Biofilms: Update on Resistance. Adv. Exp. Med. Biol. 2016, 931, 37–47. [Google Scholar] [CrossRef] [PubMed]
- Cristani, M.; D’Arrigo, M.; Mandalari, G.; Castelli, F.; Sarpietro, M.G.; Micieli, D.; Venuti, V.; Bisignano, G.; Saija, A.; Trombetta, D. Interaction of Four Monoterpenes Contained in Essential Oils with Model Membranes: Implications for Their Antibacterial Activity. J. Agric. Food Chem. 2007, 55, 6300–6308. [Google Scholar] [CrossRef] [PubMed]
- Gortzi, O.; Lala, S.; Chinou, I.; Tsaknis, J. Evaluation of the Antimicrobial and Antioxidant Activities of Origanum Dictamnus Extracts before and after Encapsulation in Liposomes. Molecules 2007, 12, 932–945. [Google Scholar] [CrossRef]
- Rao, A.; Zhang, Y.; Muend, S.; Rao, R. Mechanism of Antifungal Activity of Terpenoid Phenols Resembles Calcium Stress and Inhibition of the Tor Pathway. Antimicrob. Agents Chemother. 2010, 54, 5062–5069. [Google Scholar] [CrossRef]
- Djeddi, S.; Bouchenah, N.; Settar, I.; Skaltsa, H.D. Composition and Antimicrobial Activity of the Essential Oil of Rosmarinus Officinalis from Algeria. Chem. Nat. Compd. 2007, 43, 487–490. [Google Scholar] [CrossRef]
- Ksouri, S.; Djebir, S.; Bentorki, A.A.; Gouri, A.; Hadef, Y.; Benakhla, A. Antifungal Activity of Essential Oils Extract from Origanum Floribundum Munby, Rosmarinus Officinalis L. And Thymus Ciliatus Desf. Against Candida Albicans Isolated from Bovine Clinical Mastitis. J. Mycol. Med. 2017, 27, 245–249. [Google Scholar] [CrossRef]
- Langeveld, W.T.; Veldhuizen, E.J.; Burt, S.A. Synergy between Essential Oil Components and Antibiotics: A Review. Crit. Rev. Microbiol. 2014, 40, 76–94. [Google Scholar] [CrossRef] [PubMed]
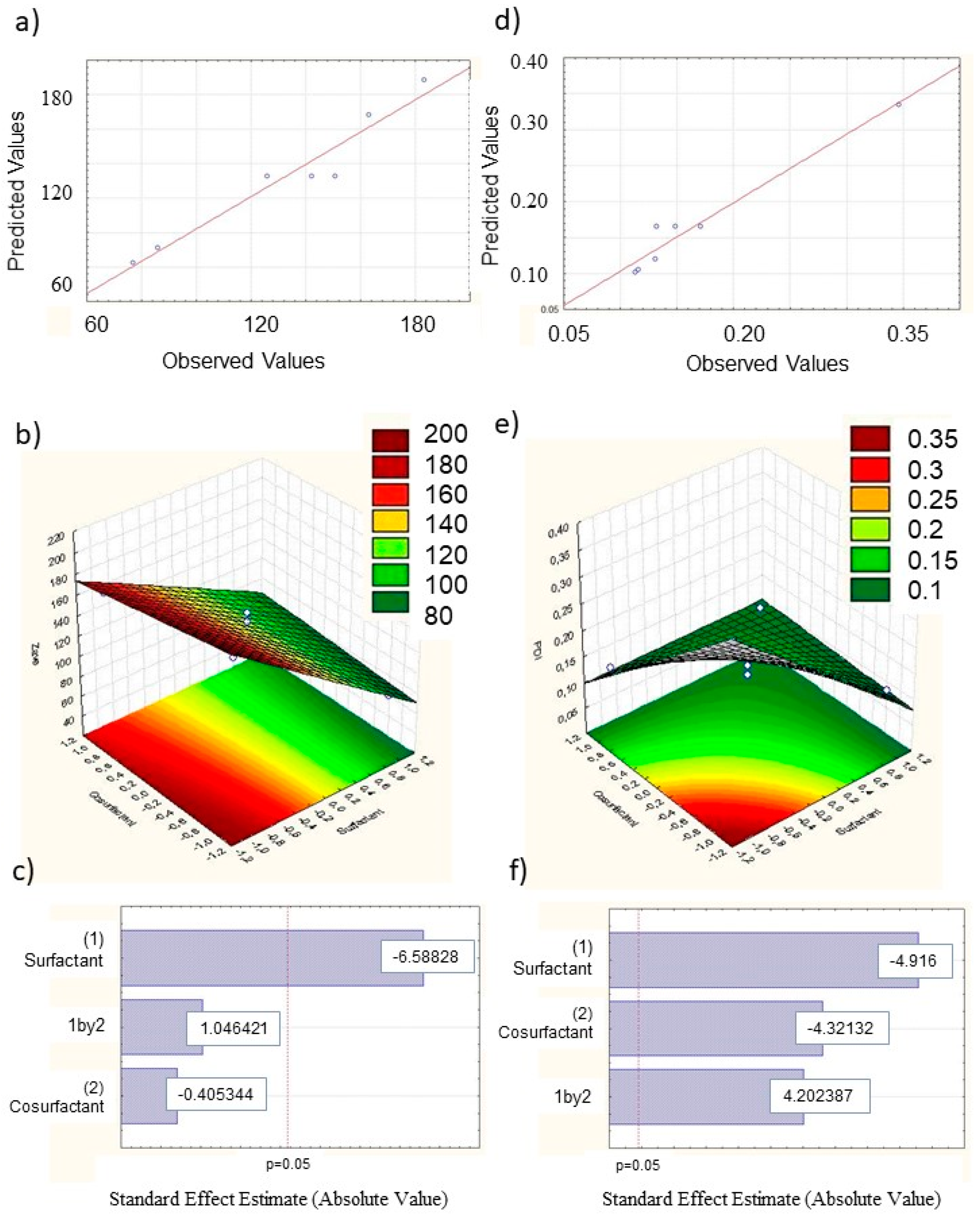






| Investigated Parameters | β0 | β1 | β2 | β12 |
|---|---|---|---|---|
| Zave | ||||
| Effect | 100 | −91.67 | −5.64 | 14.56 |
| Standard error | 5.26 | 13.91 | 13.91 | 13.91 |
| Significance level | 25.21 | −6.59 | −0.41 | 1.05 |
| t value | 0.0001 | 0.007 | 0.71 | 0.37 |
| PDI | ||||
| Effect | 0.16 | −0.12 | 0.11 | 0.11 |
| Standard error | 0.009 | 0.025 | 0.025 | 0.025 |
| Significance level | 17.35 | −4.91 | −4.32 | 4.20 |
| t value | 0.0004 | 0.01 | 0.025 | 0.025 |
| Investigated Parameters | Sum of Squares (SS) | Mean of Squares (MS) | F | Significance p Value |
|---|---|---|---|---|
| Zave | ||||
| A | 84.04 102 | 84.04 102 | 43.40 | 0.007 * |
| B | 31.81 | 31.81 | 0.16 | 0.712 |
| AB | 211.99 | 211.99 | 1.09 | 0.372 |
| Error | 580.81 | 193.60 | ||
| Total SS | 92.28 102 | |||
| PDI | ||||
| A | 1.54 10−2 | 1.54 10−2 | 24.17 | 0.016 * |
| B | 1.19 10−2 | 1.19 10−2 | 18.67 | 0.022 * |
| AB | 1.12 10−2 | 1.12 10−2 | 17.66 | 0.024 * |
| Error | 0.19 10−2 | 0.000636 | ||
| Total SS | 4.04 10−2 |
| Cell Line | Sample | Lavandula | Origanum | Rosmarinus |
|---|---|---|---|---|
| HaCaT | EO | 0.228 ± 0.004 | 0.022 ± 0.001 | 0.258 ± 0.003 |
| NLC | 0.076 ± 0.001 | 0.012 ± 0.001 | 0.075 ± 0.001 | |
| A431 | EO | 0.274 ± 0.006 | 0.012 ± 0.001 | 0.263 ± 0.002 |
| NLC | 0.114 ± 0.003 | 0.016 ± 0.001 | 0.117 ± 0.003 | |
| Effect of significance for skin cell lines | EO vs. NLC for HaCaT Significant | EO vs. NLC for A431 Significant | HaCaT vs. A431 for EO Significant | HaCaT vs. A431 for NLC Significant |
| p < 0.0001 | p < 0.0001 | p < 0.0001 | p < 0.0001 |
| Samples | Zave (nm) ± S.D. | PDI ± S.D. | EE% ± S.D. | LC ± S.D. |
|---|---|---|---|---|
| LNLC | 85.89 ± 0.51 | 0.113 ± 0.018 | - | - |
| RNLC | 76.97 ± 0.51 | 0.116 ± 0.012 | - | - |
| CLZ-LNLC | 163.0 ± 3.32 | 0.164 ± 0.025 | 25.2 ± 1.02 | 96.74 ± 0.5 |
| CLZ-RNLC | 126.8 ± 2.83 | 0.173 ± 0.008 | 16.7 ± 2.06 | 97.89 ± 0.6 |
| Sample | Strains | C. albicans ATCC 10231 | C. krusei ATCC 6258 | C. parapsilosis ATCC 90098 |
|---|---|---|---|---|
| CLZ | MIC+ | >128 | >128 | 64 |
| MLC+ | >128 | >128 | 64 | |
| Pure Lavandula | MIC† | 0.5 | 0.5 | 0.5 |
| MLC† | 0.5 | 0.5 | 0.5 | |
| Pure Rosmarinus | MIC† | 2 | 2 | 0.5 |
| MLC† | 2 | 2 | 0.5 | |
| LNLC | MIC† | 1 | >2 | >2 |
| MLC† | 1 | >2 | >2 | |
| RNLC | MIC† | >2 | >2 | >2 |
| MLC† | >2 | >2 | >2 | |
| CLZ-LNLC | MIC‡ | 0.125 + 78 | 0.25 + 156 | 0.0625 + 39 |
| MLC‡ | 0.125 + 78 | 0.25 + 156 | 0.0625 + 39 | |
| CLZ-RNLC | MIC‡ | 0.25 + 62.5 | 0.5 + 125 | 0.125 + 31.25 |
| MLC‡ | 0.25 + 62.5 | 0.5 + 125 | 0.125 + 31.25 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Carbone, C.; Teixeira, M.d.C.; Sousa, M.d.C.; Martins-Gomes, C.; Silva, A.M.; Souto, E.M.B.; Musumeci, T. Clotrimazole-Loaded Mediterranean Essential Oils NLC: A Synergic Treatment of Candida Skin Infections. Pharmaceutics 2019, 11, 231. https://0-doi-org.brum.beds.ac.uk/10.3390/pharmaceutics11050231
Carbone C, Teixeira MdC, Sousa MdC, Martins-Gomes C, Silva AM, Souto EMB, Musumeci T. Clotrimazole-Loaded Mediterranean Essential Oils NLC: A Synergic Treatment of Candida Skin Infections. Pharmaceutics. 2019; 11(5):231. https://0-doi-org.brum.beds.ac.uk/10.3390/pharmaceutics11050231
Chicago/Turabian StyleCarbone, Claudia, Maria do Céu Teixeira, Maria do Céu Sousa, Carlos Martins-Gomes, Amelia M. Silva, Eliana Maria Barbosa Souto, and Teresa Musumeci. 2019. "Clotrimazole-Loaded Mediterranean Essential Oils NLC: A Synergic Treatment of Candida Skin Infections" Pharmaceutics 11, no. 5: 231. https://0-doi-org.brum.beds.ac.uk/10.3390/pharmaceutics11050231