Periodontal Microbiological Status Influences the Occurrence of Cyclosporine-A and Tacrolimus-Induced Gingival Overgrowth
Abstract
:1. Background
2. Materials and Methods
3. Statistical Analysis
4. Results
5. Discussion
6. Conclusions
Author Contributions
Finding
Conflicts of Interest
References
- Seymour, R.A.; Ellis, J.S.; Thomason, J.M. Risk factors for drug-induced gingival overgrowth. J. Clin. Periodontol. 2000, 27, 217–223. [Google Scholar] [CrossRef]
- Hallmon, W.M.; Rossmann, J.A. The role of drugs in the pathogenesis of gingival overgrowth. A collective review of current concept. Periodontology 2000 1999, 21, 176–196. [Google Scholar] [CrossRef] [PubMed]
- Colvard, M.D.; Bishop, J.; Weissman, D.; Bargiulo, A.V. Cardizem-induced gingival hyperplasia. Periodont. Case Rep. 1986, 8, 67–68. [Google Scholar] [PubMed]
- Seymour, R.A. Calcium channel blockers and gingival overgrowth. Br. J. 1991, 170, 376–379. [Google Scholar] [CrossRef] [PubMed]
- Di Comite, M.; Crincoli, V.; Fatone, L.; Ballini, A.; Mori, G.; Rapone, B.; Boccaccio, A.; Pappalettere, C.; Grassi, F.R.; Favia, A. Quantitative analysis of defects at the dentin-post space in endodontically treated teeth. Materials 2015, 8, 3268–3283. [Google Scholar] [CrossRef]
- Kalemaj, Z.; Scarano, A.; Valbonetti, L.; Rapone, B.; Grassi, F.R. Bone response to four dental implants with different surface topography: A histologic and histometric study in minipigs. Int. J. Periodontics Restor. Dent. 2016, 36, 745–754. [Google Scholar] [CrossRef] [PubMed]
- Rapone, B.; Nardi, G.M.; Di Venere, D.; Pettini, F.; Grassi, F.R.; Corsalini, M. Oral hygiene in patients with oral cancer undergoing chemotherapy and/or radiotherapy after prosthesis rehabilitation: Protocol proposal. Oral Implantol. 2016, 9 (Suppl. 1), 90–97. [Google Scholar] [CrossRef]
- Corsalini, M.; di Venere, D.; Rapone, B.; Stefanachi, G.; Laforgia, A.; Pettini, F. Evidence of signs and symptoms of Craniomandibular Disorders in Fibromyalgia patients. Open Dent. J. 2017, 11, 91–98. [Google Scholar] [CrossRef]
- Di Venere, D.; Pettini, F.; Nardi, G.M.; Laforgia, A.; Stefanachi, G.; Notaro, V.; Rapone, B.; Grassi, F.R.; Corsalini, M. Correlation between parodontal indexes and orthodontic retainers: Prospective study in a group of 16 patients. Oral Implantol. 2017, 10, 78–86. [Google Scholar] [CrossRef] [PubMed]
- Di Venere, D.; Nardi, G.M.; Lacarbonara, V.; Laforgia, A.; Stefanachi, G.; Corsalini, M.; Grassi, F.R.; Rapone, B.; Pettini, F. Early mandibular canine-lateral incisor transposition: Case Report. Oral Implantol. 2017, 10, 181–189. [Google Scholar] [CrossRef] [PubMed]
- Di Venere, D.; Corsalini, M.; Nardi, G.M.; Laforgia, A.; Grassi, F.R.; Rapone, B.; Pettini, F. Obstructive site localization in patients with Obstructive Sleep Apnea Syndrome: A comparison between otolaryngologic data and cephalometric values. Oral Implantol. 2017, 10, 295–310. [Google Scholar] [CrossRef] [PubMed]
- Grassi, F.R.; Rapone, B.; Scarano Catanzaro, F.; Corsalini, M.; Kalemaj, Z. Effectiveness of computer-assisted anesthetic delivery system (STA™) in dental implant surgery: A prospective study. Oral Implantol. 2017, 10, 381–389. [Google Scholar] [CrossRef] [PubMed]
- Notaro, V.; Rapone, B.; Cagnetta, G.; Sportelli, P.; Nardi, G.M.; Corsalini, M. Resonance frequency evaluation on immediate loading implants with angled abutments: Case series. Ann. Di Stomatol. 2018, 9, 91–96. [Google Scholar] [CrossRef]
- Quaglia, E.; Moscufo, L.; Corsalini, M.; Coscia, D.; Sportelli, P.; Cantatore, F.; de Rinaldis, C.; Rapone, B.; Carossa, M.; Carossa, S. Polyamide vs silk sutures in the healing of postextraction sockets: A split mouth study. Oral Implantol. 2018, 11, 115–120. [Google Scholar] [CrossRef]
- Nardi, G.M.; Grassi, R.; Grassi, F.R.; Aragona, S.E.; Rapone, B.; Della Vella, F.; Sabatini, S. Use of photobiomodulation induced by polarized polychromatic non-coherent light in the management of adult chronic periodontitis. J. Biol. Regul. Homeost. Agents 2019, 33, 293–297. [Google Scholar] [PubMed]
- Corsalini, M.; di Venere, D.; Carossa, M.; Ripa, M.; Sportelli, P.; Cantatore, F.; de Rinaldis, C.; di Santantonio, G.; Lenoci, G.; Barile, G.; et al. Comparative clinical study between zirconium-ceramic and metal-ceramic fixed rehabilitations. Oral Implantol. 2018, 11, 150–160. [Google Scholar]
- Corsalini, M.; di Venere, D.; Sportelli, P.; Magazzino, D.; Ripa, M.; Cantatore, F.; Cagnetta, C.; de Rinaldis, C.; Montemurro, N.; de Giacomo, A.; et al. Evaluation of prosthetic quality and masticatory efficiency in patients with total removable prosthesis: Study of 12 cases. Oral Implantol. 2018, 11, 230–240. [Google Scholar]
- Corsalini, M.; Rapone, B.; di Venere, D.; Petruzzi, M. Removable prosthetic treatment in oral pemphigus vulgaris: Report of three cases. J. Int. Soc. Prevent. Community Dent. 2019. [Google Scholar] [CrossRef]
- Khoori, A.H.; Einollahi, B.; Ansari, G.; Moozeh, M.B. The effect of cyclosporine with and without nifedipine on gingival overgrowth in renal transplant patients. J. Can. Dent. Assoc. 2003, 69, 236–241. [Google Scholar]
- Ratre, M.S.; Mehta, D.S. Effect of azithromycin on gingival overgrowth induced by cyclosporine A+nifedipine combination therapy: A morphometric analysis in rats. J. Indian Soc. Periodontol. 2016, 20, 396–401. [Google Scholar] [CrossRef]
- Ellis, J.S.; Seymour, R.A.; Steele, J.G.; Robertson, P.; Butler, T.J.; Thomason, J.M. Prevalence of Gingival Overgrowth Induced by Calcium Channel Blockers: A Community-Based Study. J. Periodontol. 1999, 70, 63–67. [Google Scholar] [CrossRef] [PubMed]
- Seymour, R.A.; Smith, D.G. The effect of a plaque control programme on the incidence and severity of cyclosporininduced gingival changes. J. Clin. Periodontol. 1991, 18, 107–110. [Google Scholar] [CrossRef] [PubMed]
- Thomason, J.M.; Seymour, R.A.; Rawlins, M.D. Incidence and severity of phenytoin-induced gingival overgrowth in epileptic patients in general medical practice. Community Dent. Oral Epidemiol. 1992, 20, 288–291. [Google Scholar] [CrossRef]
- Marshall, R.I.; Bartold, P.M. Medication induced gingival overgrowth. Oral Dis. 1998, 4, 130–151. [Google Scholar] [PubMed]
- Benveniste, K.; Bitar, M. Effects of Phenytoin on Cultured Human Gingival Fibroblasts, Phenytoin-Induced Teratology and Gingival Pathology; Hassell, T., Johnston, M., Dudley, K., Eds.; Raven Press: New York, NY, USA, 1980; pp. 199–214. [Google Scholar]
- Hassell, T.M. Stimulation and inhibition of fibroblast subpopulations by phenytoin and phenytoin metabolites: Pathogenetic role in gingival enlargement. Pediatr. Dent. 1981, 3, 137–153. [Google Scholar]
- A study of the histopathology of gingival hyperplasia in mental patients receiving sodium diphenylhydantoinate. Oral Surg. 1967, 23, 774–786. [CrossRef]
- Ko, S.D.; Page, R.C.; Narayanan, A.S. Fibroblast heterogeneity and prostaglandin regulation of subpopulations. Proc. Natl. Acad. Sci. USA 1977, 74, 3429–3432. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dongari, A. Research, Science and Therapy Committee, American Academy of Periodontology. Drug-associated gingival enlargement. J. Periodontol. 2004, 75, 1424–1431. [Google Scholar]
- Cota, L.O.; Viana, M.B.; Moreira, P.R.; Gomez, R.S.; Cortelli, J.R.; Cortelli, S.C.; Costa, F.O. Gingival overgrowth in cyclosporine, tacrolimus, or sirolimus-based immunosuppressive regimens and the single nucleotide IL-6 (-174 G/C) gene polymorphism. Arch. Oral Biol. 2010, 55, 494–501. [Google Scholar] [CrossRef] [PubMed]
- Marshall, R.I.; Bartold, P.M. A clinical review of drug-induced gingival overgrowths. Aust. Dent. J. 1999, 44, 219–232. [Google Scholar] [CrossRef]
- Ikawa, K.; Ikawa, M.; Shimauchi, H.; Iwakura, M.; Sakamoto, S. Treatment of gingival overgrowth induced by manidipine administration: A case report. J. Periodontol. 2002, 73, 115–122. [Google Scholar] [CrossRef] [PubMed]
- Tipton, D.A.; Stricklin, G.P.; Dabbous, M.K. Fibroblast heterogeneity in collagenolytic response to cyclosporine. J. Cell. Biochem. 1991, 46, 152–165. [Google Scholar] [CrossRef] [PubMed]
- Kaur, G.; Verhamme, K.M.; Dieleman, J.P.; Vanrolleghem, A.; van Soest, E.M.; Stricker, B.H.; Sturkenboom, M.C. Association between calcium channel blockers and gingival hyperplasia. J. Clin. Periodontol. 2010, 37, 625–630. [Google Scholar] [CrossRef] [PubMed]
- Cupp, M.J.; Tracy, T.S. Cytochrome P450: New nomenclature and clinical implications. Am. Fam. Physician 1998, 57, 107–116. [Google Scholar] [PubMed]
- Belpaire, F.M.; Bogaert, M.G. Cytochrome P450: Genetic polymorphism and drug interactions. Acta Clin. Belg. 1996, 51, 254–260. [Google Scholar] [CrossRef]
- Nishikawa, S.; Nagata TMorisaki, I.; Oka, T.; Ishida, H. Pathogenesis of Drug-Induced Gingival Overgrowth. A Review of Studies in the Rat Model. J. Periodontol. 1996, 67, 463–471. [Google Scholar] [CrossRef]
- Margiotta, V.; Pizzo, I.; Pizzo, G.; Barbaro, A. Cyclosporin-and nifedipine-induced gingival overgrowth in renal transplant patients: Correlations with periodontal and pharmacological parameters, and HLA-antigens. J. Oral Pathol. Med. 1996, 25, 128–134. [Google Scholar] [CrossRef]
- Johanson, M.; Zhao, X.R.; Huynh-Ba, G.; Villar, C.C. Matrix Metalloproteinases, Tissue Inhibitors of Matrix Metalloproteinases, and Inflammation in Cyclosporine A–Induced Gingival Enlargement: A Pilot In Vitro Study Using a Three-Dimensional Model of the Human Oral Mucosa. J. Periodontol. 2013, 84, 634–640. [Google Scholar] [CrossRef]
- Ballini, A.; Cantore, S.; Farronato, D.; Cirulli, N.; Inchingolo, F.; Papa, F.; Malcangi, G.; Inchingolo, A.D.; Dipalma, G.; Sardaro, N.; et al. Periodontal disease and bone pathogenesis: The crosstalk between cytokines and porphyromonas gingivalis. J. Biol. Regul. Homeost. Agents 2015, 29, 273–281. [Google Scholar]
- Santacroce, L.; Carlaio, R.G.; Bottalico, L. Does it make sense that diabetes is reciprocally associated with periodontal disease? Endocr. Metab. Immune Disord. Drug Targets 2010, 10, 57–70. [Google Scholar] [CrossRef]
- Ballini, A.; Cantore, S.; Dedola, A.; Santacroce, L.; Laino, L.; Cicciu, M.; Mastrangelo, F. IL-1 haplotype analysis in periodontal disease. J. Biol. Regul. Homeost. Agents 2018, 32, 433–437. [Google Scholar]
- Di Serio, F.; Lovero, R.; D’Agostino, D.; Nisi, L.; Miragliotta, G.; Contino, R.; Man, A.; Ciccone, M.M.; Santacroce, L. Evaluation of procalcitonin, Vitamin D and C-reactive protein levels in septic patients with positive emocoltures. Our preliminary experience. Acta Med. Mediterr. 2016, 32, 1911–1914. [Google Scholar] [CrossRef]
- Giudice, G.; Cutrignelli, D.A.; Sportelli, P.; Limongelli, L.; Tempesta, A.; Gioia, G.D.; Santacroce, L.; Maiorano, E.; Favia, G. Rhinocerebral Mucormycosis with Orosinusal Involvement: Diagnostic and Surgical Treatment Guidelines. Endocr. Metab. Immune Disord. Drug Targets 2016, 16, 264–269. [Google Scholar] [CrossRef] [PubMed]
- Vermesan, D.; Vermesan, H.; Dragulescu, S.I.; Bera, I.; di Giovanni, A.; Sabatini, R.; Santacroce, L.; Bottalico, L.; Flace, P.; Cagiano, R. Secondary pathologic fractures in osteosarcoma: Prognosis and evolution. Eur. Rev. Med. Pharmacol. Sci. 2009, 13, 71–76. [Google Scholar] [PubMed]
- Monea, A.; Santacroce, L.; Marrelli, M.; Man, A. Oral candidiasis and inflammatory response: A potential synergic contribution to the onset of type-2 diabetes mellitus. Australas. Med. J. 2017, 10, 550–556. [Google Scholar] [CrossRef]
- Santacroce, L.; D’agostino, D.; Charitos, I.A.; Bottalico, L.; Ballini, A. A short review about electrophysiology and bioimpedance: History and perspectives. Indian J. Public Health Res. Dev. 2018, 9, 577–591. [Google Scholar] [CrossRef]
- Nardi, G.M.; Sabatini, S.; Guerra, F.; Tatullo, M.; Ottolenghi, L. Tailored brushing method (TBM): An innovative simple protocol to improve the oral care. J. Biomed. 2016, 1, 26–31. [Google Scholar] [CrossRef]
- Kantarci, A.; Augustin, P.; Firatli, E.; Sheff, M.C.; Hasturk, H.; Graves, D.T. Trackman Apoptosis in gingival overgrowth tissues. PCJ Dent. Res. 2007, 86, 888–892. [Google Scholar] [CrossRef] [PubMed]
- Jung, J.Y.; Jeong, Y.J.; Jeong, T.S.; Chung, H.J.; Kim, W.J. Inhibition of apoptotic signals in overgrowth of human gingival fibroblasts by cyclosporin A treatment. Arch. Oral Biol. 2008, 53, 1042–1049. [Google Scholar] [CrossRef] [PubMed]
- Tu, H.P.; Fu, E.; Chen, Y.T.; Wu, M.H.; Cheng, L.C.; Yang, S.F. Expression of p21 and p53 in rat gingival and human oral epithelial cells after cyclosporine A treatment. J. Periodontal Res. 2008, 43, 32. [Google Scholar] [CrossRef]
- Tu, H.P.; Chen, Y.T.; Chiu, H.C.; Chin, Y.T.; Huang, S.M.; Cheng, L.C.; Fu, E.; Chiang, C.Y. Cyclosporine A enhances apoptosis in gingival keratinocytes of rats and in OECM1 cells via the mitochondrial pathway. J. Periodontal Res. 2009, 44, 767–775. [Google Scholar] [CrossRef] [PubMed]
- Hyland, P.L.; McKeown, S.T.; Mackenzie, I.C.; Irwin, C.R. Regulation of keratinocyte growth factor and scatter factor in cyclosporin-induced gingival overgrowth. J. Oral Pathol. Med. 2004, 33, 391–397. [Google Scholar] [CrossRef] [PubMed]






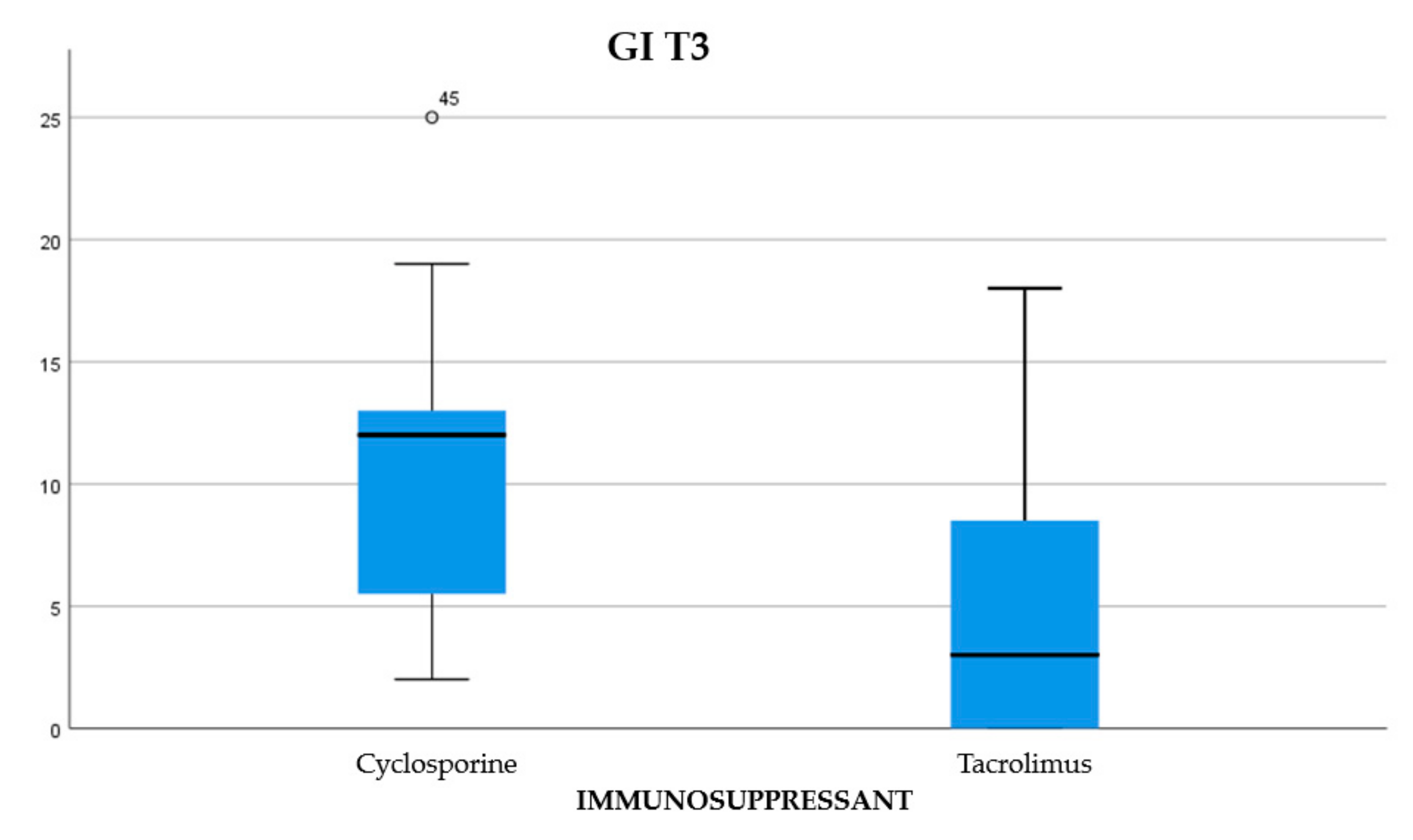


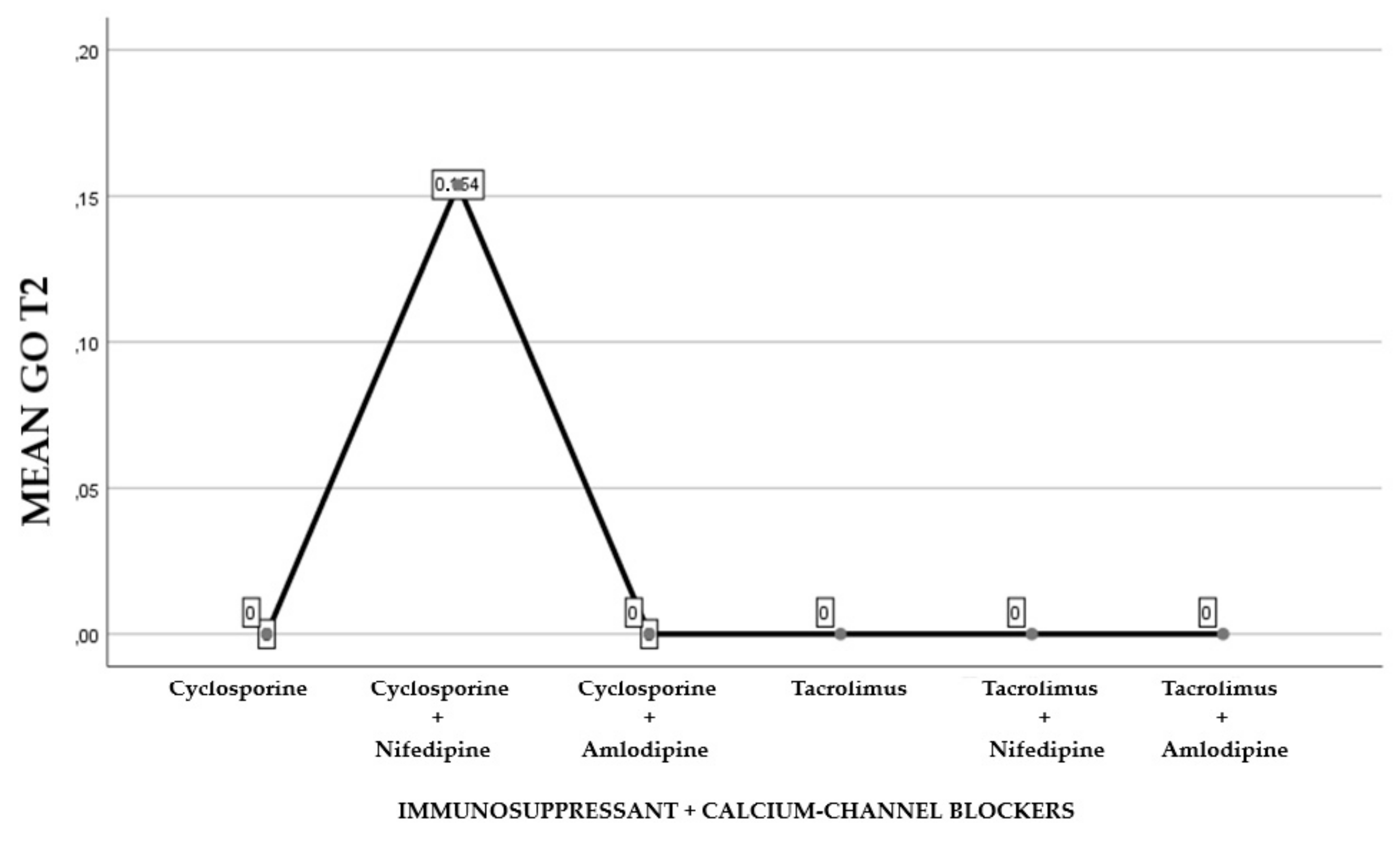

| Statistic Tests a | ||||
|---|---|---|---|---|
| Periodontal Indices | U of Mann-Whitney | W of Wilcoxon | Z | Asymptotic Sign. (with Two Tails) |
| PI T0 | 269,500 | 675,500 | −994 | 0.320 |
| PI T1 | 269,500 | 675,500 | −996 | 0.319 |
| PI T2 | 165,500 | 571,500 | −2974 | 0.003 |
| PI T3 | 189,000 | 595,000 | −2528 | 0.011 |
| GI T0 | 230,000 | 636,000 | −1742 | 0.081 |
| GI T1 | 235,000 | 641,000 | −1649 | 0.099 |
| GIT2 | 184,500 | 590,500 | −2616 | 0.009 |
| GI T3 | 133,000 | 539,000 | −3597 | 0.000 |
| GO T0 | 250,000 | 656,000 | −1744 | 0.081 |
| GO T1 | 308,000 | 714,000 | −1103 | 0.270 |
| GO T2 | 308,000 | 714,000 | −1103 | 0.270 |
| GO T3 | 308,000 | 714,000 | −1103 | 0.270 |
| PD T0 | 279,500 | 685,500 | −805 | 0.421 |
| PD T1 | 278,500 | 684,500 | −824 | 0.410 |
| PD T2 | 283,000 | 689,000 | −739 | 0.460 |
| PD T3 | 299,500 | 705,500 | −428 | 0.669 |
| CAL T0 | 278,500 | 684,500 | −824 | 0.410 |
| CAL T1 | 272,000 | 678,000 | −947 | 0.343 |
| CAL T2 | 253,000 | 659,000 | −1307 | 0.191 |
| CAL T3 | 259,000 | 665,000 | −1194 | 0.232 |
| Statistic Tests a,b | ||||
|---|---|---|---|---|
| Test | GO T0 | GO T1 | GO T2 | GO T3 |
| H of Kruskal-Wallis | 6434 | 2923 | 2923 | 2923 |
| gl | 5 | 5 | 5 | 5 |
| Asymptotic sign. | 0.266 | 0.712 | 0.712 | 0.712 |
| Statistics Tests a,b | |||
|---|---|---|---|
| Periodontal Indices | H of Kruskal-Wallis | Gl | Asymptotic Sign. |
| PI T0 | 7880 | 5 | 0.163 |
| PI T1 | 5710 | 5 | 0.335 |
| PI T2 | 11,280 | 5 | 0.046 |
| PI T3 | 6776 | 5 | 0.238 |
| GI T0 | 7979 | 5 | 0.157 |
| GI T1 | 6311 | 5 | 0.277 |
| GI T2 | 9126 | 5 | 0.104 |
| GI T3 | 13,809 | 5 | 0.017 |
| PD T0 | 7601 | 5 | 0.180 |
| PD T1 | 6852 | 5 | 0.232 |
| PD T2 | 7661 | 5 | 0.176 |
| PD T3 | 7136 | 5 | 0.211 |
| CAL T0 | 6757 | 5 | 0.239 |
| CAL T1 | 3897 | 5 | 0.564 |
| CAL T2 | 5310 | 5 | 0.379 |
| CAL T3 | 6844 | 5 | 0.232 |
| Correlations | ||
|---|---|---|
| IG T0 | ||
| GO T0 | Pearson’s correlation | 1 |
| N | 51 | |
| PI T0 | Pearson’s correlation | 0.512 |
| Sign. (with two tails) | 0.000 | |
| N | 51 | |
| GI T0 | Pearson’s correlation | 0.621 |
| Sign. (with two tails) | 0.000 | |
| N | 51 | |
| PD T0 | Pearson’s correlation | 0.351 |
| Sign. (with two tails) | 0.012 | |
| N | 51 | |
| CAL T0 | Pearson’s correlation | 0.358 |
| Sign. (with two tails) | 0.010 | |
| N | 51 | |
| Correlations | ||
|---|---|---|
| IG T1 | ||
| GO T1 | Pearson’s correlation | 1 |
| N | 51 | |
| PI T1 | Pearson’s correlation | 0.625 |
| Sign. (with two tails) | 0.000 | |
| N | 51 | |
| GI T1 | Pearson’s correlation | 0.455 |
| Sign. (with two tails) | 0.001 | |
| N | 51 | |
| PD T1 | Pearson’s correlation | 0.243 |
| Sign. (with two tails) | 0.085 | |
| N | 51 | |
| CAL T1 | Pearson’s correlation | 0.333 |
| Sign. (with two tails) | 0.017 | |
| N | 51 | |
| Correlations | ||
|---|---|---|
| IG T2 | ||
| GO T2 | Pearson’s correlation | 1 |
| N | 51 | |
| PI T2 | Pearson’s correlation | 0.183 |
| Sign. (with two tails) | 0.200 | |
| N | 51 | |
| GI T2 | Pearson’s correlation | 0.163 |
| Sign. (with two tails) | 0.253 | |
| N | 51 | |
| PD T2 | Pearson’s correlation | 0.303 |
| Sign. (with two tails) | 0.031 | |
| N | 51 | |
| CAL T2 | Pearson’s correlation | 0.383 |
| Sign. (with two tails) | 0.006 | |
| N | 51 | |
| Correlations | ||
|---|---|---|
| IG T3 | ||
| GO T3 | Pearson’s correlation | 1 |
| N | 51 | |
| PI T3 | Pearson’s correlation | 0.183 |
| Sign. (with two tails) | 0.200 | |
| N | 51 | |
| GI T3 | Pearson’s correlation | 0.163 |
| Sign. (with two tails) | 0.253 | |
| N | 51 | |
| PD T3 | Pearson’s correlation | 0.303 |
| Sign. (with two tails) | 0.031 | |
| N | 51 | |
| CAL T3 | Pearson’s correlation | 0.383 |
| Sign. (with two tails) | 0.006 | |
| N | 51 | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rapone, B.; Ferrara, E.; Santacroce, L.; Cesarano, F.; Arazzi, M.; Di Liberato, L.; Scacco, S.; Grassi, R.; Grassi, F.R.; Gnoni, A.; et al. Periodontal Microbiological Status Influences the Occurrence of Cyclosporine-A and Tacrolimus-Induced Gingival Overgrowth. Antibiotics 2019, 8, 124. https://0-doi-org.brum.beds.ac.uk/10.3390/antibiotics8030124
Rapone B, Ferrara E, Santacroce L, Cesarano F, Arazzi M, Di Liberato L, Scacco S, Grassi R, Grassi FR, Gnoni A, et al. Periodontal Microbiological Status Influences the Occurrence of Cyclosporine-A and Tacrolimus-Induced Gingival Overgrowth. Antibiotics. 2019; 8(3):124. https://0-doi-org.brum.beds.ac.uk/10.3390/antibiotics8030124
Chicago/Turabian StyleRapone, Biagio, Elisabetta Ferrara, Luigi Santacroce, Francesca Cesarano, Marta Arazzi, Lorenzo Di Liberato, Salvatore Scacco, Roberta Grassi, Felice Roberto Grassi, Antonio Gnoni, and et al. 2019. "Periodontal Microbiological Status Influences the Occurrence of Cyclosporine-A and Tacrolimus-Induced Gingival Overgrowth" Antibiotics 8, no. 3: 124. https://0-doi-org.brum.beds.ac.uk/10.3390/antibiotics8030124








