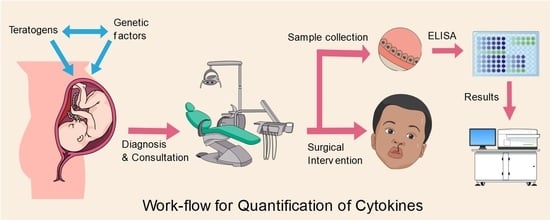
Quantification of Cytokines in Lip Tissue from Infants Affected by Congenital Cleft Lip and Palate
Abstract
:1. Introduction
2. Materials and Methods
2.1. Profile of Study Participants
2.2. Data and Sample Collection
2.3. Sample Preparation and ELISA
2.4. Cytokines Studied and Statistical Analysis
3. Results
3.1. Mean Concentration of Cytokines in Patients
3.2. Concentration of Cytokines in Individual Patients
3.3. Correlation between Cytokines
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Vieira, A.R.; Orioli, I.M. Birth order and oral clefts: A meta-analysis. Teratology 2002, 66, 209–216. [Google Scholar] [CrossRef]
- Robin, N.H.; Baty, H.; Franklin, J.; Guyton, F.C.; Mann, J.; Woolley, A.L.; Waite, P.D.; Grant, J. The multidisciplinary evaluation and management of cleft lip and palate. South. Med. J. 2006, 99, 1111–1120. [Google Scholar] [CrossRef]
- Murray, J.C. Gene/environment causes of cleft lip and/or palate. Clin. Genet. 2002, 61, 248–256. [Google Scholar] [CrossRef]
- Peterson, L.J.; Ellis, E.; Hupp, J.R.; Tucker, M.R. Contemporary Oral and Maxillofacial Surgery, 4th ed.; Mosby Co.: St. Louis, MO, USA, 2003. [Google Scholar]
- Simmerman, E.; Qin, X.; Marshall, B.; Perry, L.; Cai, L.; Wang, T.; Yu, J.; Akbari, O.; Baban, B. Innate lymphoid cells: A paradigm for low SSI in cleft lip repair. J. Surg. Res. 2016, 205, 312–317. [Google Scholar] [CrossRef]
- Panetta, N.J.; Gupta, D.M.; Slater, B.J.; Kwan, M.D.; Liu, K.J.; Longaker, M.T. Tissue engineering in cleft palate and other congenital malformations. Pediatr. Res. 2008, 63, 545–551. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Z.; Fang, S.; Zhang, Q.; Chen, L.; Liu, Y.; Li, K.; Zhao, Y. Analysis of complications in primary cleft lips and palates surgery. J. Craniofac. Surg. 2014, 25, 968–971. [Google Scholar] [CrossRef] [PubMed]
- Yamaguchi, K.; Lonic, D.; Lo, L.J. Complications following orthognathic surgery for patients with cleft lip/palate: A systematic review. J. Formos. Med. Assoc. 2016, 115, 269–277. [Google Scholar] [CrossRef] [Green Version]
- Agency for Healthcare Research and Quality. HCUP 2007 Healthcare Cost and Utilization Project. Available online: http://www.ahrq.gov/data/hcup/ (accessed on 10 October 2020).
- Ács, L.; Bányai, D.; Nemes, B.; Nagy, K.; Ács, N.; Bánhidy, F.; Rózsa, N. Maternal-related factors in the origin of isolated cleft palate-A population-based case-control study. Orthod. Craniofac. Res. 2020, 23, 174–180. [Google Scholar] [CrossRef] [PubMed]
- Prabhu, S.; Krishnapillai, R.; Jose, M.; Prabhu, V. Etiopathogenesis of orofacial clefting revisited. J. Oral Maxillofac. Pathol. 2012, 16, 228–232. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Muhamad, A.H.; Azzaldeen, A.; Watted, N. Cleft lip and palate; A comprehensive review. Int. J. Basic Appl. Med Sci. 2014, 4, 338–355. [Google Scholar]
- Prescott, N.J.; Winter, R.M.; Malcolm, S. Nonsyndromic cleft lip and palate: Complex genetics and environmental effects. Ann. Hum. Genet. 2001, 65 Pt 6, 505–515. [Google Scholar] [CrossRef]
- Cohen, M.M. Etiology and pathogenesis of orofacial clefting. Oral Maxillofac. Surg. Clin. N. Am. 2000, 12, 379–396. [Google Scholar] [CrossRef]
- Diehl, S.R.; Erickson, R.P. Genome scan for teratogen-induced clefting susceptibility loci in the mouse: Evidence of both allelic and locus heterogeneity distinguishing cleft lip and cleft palate. Proc. Natl. Acad. Sci. USA 1997, 94, 5231–5236. [Google Scholar] [CrossRef] [Green Version]
- Ferguson, M.W. Palate development. Development 1988, 103, 41–60. [Google Scholar]
- Moore, G.; Ivens, A.; Chambers, J.; Bjornsson, A.; Arnason, A.; Jensson, O.; Williamson, R. The application of molecular genetics to detection of craniofacial abnormality. Development 1988, 103, 233–239. [Google Scholar] [PubMed]
- Kerrigan, J.J.; Mansell, J.P.; Sengupta, A.; Brown, N.; Sandy, J.R. Palatogenesis and potential mechanisms for clefting. J. R. Coll. Surg. Edinb. 2000, 45, 351–358. [Google Scholar] [PubMed]
- Gulati, K.; Guhathakurta, S.; Joshi, J.; Rai, N.; Ray, A. Cytokines and their role in health and disease: A brief overview. MOJ Immunol. 2016, 4, 1–9. [Google Scholar] [CrossRef] [Green Version]
- Steinke, J.W.; Borish, L. 3. Cytokines and chemokines. J. Allergy Clin. Immunol. 2006, 117, S441–S445. [Google Scholar] [CrossRef]
- Turner, M.D.; Nedjai, B.; Hurst, T.; Pennington, D.J. Cytokines and chemokines: At the crossroads of cell signalling and inflammatory disease. Biochim. Biophys. Acta 2014, 1843, 2563–2582. [Google Scholar] [CrossRef] [Green Version]
- Leng, S.X.; McElhaney, J.E.; Walston, J.D.; Xie, D.; Fedarko, N.S.; Kuchel, G.A. ELISA and multiplex technologies for cytokine measurement in inflammation and aging research. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2008, 63, 879–884. [Google Scholar] [CrossRef] [Green Version]
- Inoyatov, A.; Abdurakhmanov, M.; Sharopov, S.; Azimov, M. The levels of mediators of immune response in infants with congenital cleft lip and palate. Med. Health Sci. J. 2012, 10, 30–36. [Google Scholar] [CrossRef]
- Musakhodjaeva, D.A.; Sharopov, S.G. Cytokine profile in children with congenital cleft lip and palate. Eur. J. Pharm. Med. Res. 2019, 6, 335–339. [Google Scholar]
- Burdi, A.R. Cleft lip and palate research: An updated state of the art. Section I. Epidemiology, etiology, and pathogenesis of cleft lip and palate. Cleft Palate J. 1977, 14, 261–269. [Google Scholar] [PubMed]
- Bell, R.B.; Feng, Z.; Bifulco, C.B.; Leidner, R.; Weinberg, A.; Fox, B.A. 15—Immunotherapy. In Oral, Head and Neck Oncology and Reconstructive Surgery; Bell, R.B., Fernandes, P.P., Andersen, P.E., Eds.; Elsevier: Amsterdam, The Netherlands, 2018; pp. 314–340. [Google Scholar] [CrossRef]
- Li, M.; Li, R. IL-2 regulates oral mucosa inflammation through inducing endoplasmic reticulum stress and activating the NF-ĸB pathway. J. Recept. Signal Transduct. 2020, 40, 187–193. [Google Scholar] [CrossRef] [PubMed]
- Katsikis, P.D.; Cohen, S.B.; Londei, M.; Feldmann, M. Are CD4+ Th1 cells pro-inflammatory or anti-inflammatory? The ratio of IL-10 to IFN-gamma or IL-2 determines their function. Int. Immunol. 1995, 7, 1287–1294. [Google Scholar] [CrossRef]
- Jewett, A.; Arasteh, A.; Tseng, H.C.; Behel, A.; Arasteh, H.; Yang, W.; Cacalano, N.A.; Paranjpe, A. Strategies to rescue mesenchymal stem cells (MSCs) and dental pulp stem cells (DPSCs) from NK cell mediated cytotoxicity. PLoS ONE 2010, 5, e9874. [Google Scholar] [CrossRef]
- Mooney, M.P.; Siegel, M.I.; Kimes, K.R.; Todhunter, J.; Janosky, J. Multivariate analysis of second trimester midfacial morphology in normal and cleft lip and palate human fetal specimens. Am. J. Phys. Anthropol. 1992, 88, 203–209. [Google Scholar] [CrossRef]
- Siegel, M.I.; Mooney, M.P.; Kimes, K.R.; Gest, T.R. Traction, prenatal development, and the labioseptopremaxillary region. Plast. Reconstr. Surg. 1985, 76, 25–28. [Google Scholar] [CrossRef]
- Siegel, M.I.; Mooney, M.P.; Kimes, K.R.; Todhunter, J. Developmental correlates of midfacial components in a normal and cleft lip and palate human fetal sample. Cleft Palate C. J. 1991, 28, 408–412. [Google Scholar] [CrossRef]
- Moqbel, R.; Ying, S.; Barkans, J.; Newman, T.M.; Kimmitt, P.; Wakelin, M.; Taborda-Barata, L.; Meng, Q.; Corrigan, C.J.; Durham, S.R.; et al. Identification of messenger RNA for IL-4 in human eosinophils with granule localization and release of the translated product. J. Immunol. 1995, 155, 4939–4947. [Google Scholar]
- Neill, D.R.; Wong, S.H.; Bellosi, A.; Flynn, R.J.; Daly, M.; Langford, T.K.; Bucks, C.; Kane, C.M.; Fallon, P.G.; Pannell, R.; et al. Nuocytes represent a new innate effector leukocyte that mediates type-2 immunity. Nature 2010, 464, 1367–1370. [Google Scholar] [CrossRef] [Green Version]
- Saenz, S.A.; Siracusa, M.C.; Perrigoue, J.G.; Spencer, S.P.; Urban, J.F., Jr.; Tocker, J.E.; Budelsky, A.L.; Kleinschek, M.A.; Kastelein, R.A.; Kambayashi, T.; et al. IL25 elicits a multipotent progenitor cell population that promotes T(H)2 cytokine responses. Nature 2010, 464, 1362–1366. [Google Scholar] [CrossRef]
- Brown, M.A.; Pierce, J.H.; Watson, C.J.; Falco, J.; Ihle, J.N.; Paul, W.E. B cell stimulatory factor-1/interleukin-4 mRNA is expressed by normal and transformed mast cells. Cell 1987, 50, 809–818. [Google Scholar] [CrossRef]
- Gabrielsson, S.; Söderlund, A.; Nilsson, C.; Lilja, G.; Nordlund, M.; Troye-Blomberg, M. Influence of atopic heredity on IL-4-, IL-12- and IFN-gamma-producing cells in in vitro activated cord blood mononuclear cells. Clin. Exp. Immunol. 2001, 126, 390–396. [Google Scholar] [CrossRef]
- Wegmann, T.G.; Lin, H.; Guilbert, L.; Mosmann, T.R. Bidirectional cytokine interactions in the maternal-fetal relationship: Is successful pregnancy a TH2 phenomenon? Immunol. Today 1993, 14, 353–356. [Google Scholar] [CrossRef]
- Raghupathy, R.; Makhseed, M.; Azizieh, F.; Hassan, N.; Al-Azemi, M.; Al-Shamali, E. Maternal Th1- and Th2-type reactivity to placental antigens in normal human pregnancy and unexplained recurrent spontaneous abortions. Cell. Immunol. 1999, 196, 122–130. [Google Scholar] [CrossRef]
- Kondo, N.; Kobayashi, Y.; Shinoda, S.; Kasahara, K.; Kameyama, T.; Iwasa, S.; Orii, T. Cord blood lymphocyte responses to food antigens for the prediction of allergic disorders. Arch. Dis. Child. 1992, 67, 1003–1007. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sopo, S.M.; Pesaresi, M.A.; Guerrini, B.; Federico, G.; Stabile, A. Mononuclear cell reactivity to food allergens in neonates, children and adults. Pediatr. Allergy Immunol. 1999, 10, 249–252. [Google Scholar] [CrossRef]
- Landor, M. Maternal-fetal transfer of immunoglobulins. Ann. Allergy Asthma Immunol. 1995, 74, 279–283. [Google Scholar] [PubMed]
- Casas, R.; Böttcher, M.F.; Duchén, K.; Björkstén, B. Detection of IgA antibodies to cat, beta-lactoglobulin, and ovalbumin allergens in human milk. J. Allergy Clin. Immunol. 2000, 105 Pt 1, 1236–1240. [Google Scholar] [CrossRef]
- Böttcher, M.F.; Jenmalm, M.C.; Garofalo, R.P.; Björkstén, B. Cytokines in breast milk from allergic and nonallergic mothers. Pediatr. Res. 2000, 47, 157–162. [Google Scholar] [CrossRef] [Green Version]
- Perrier, S.; Kherratia, B.; Deschaumes, C.; Ughetto, S.; Kemeny, J.L.; Baudet-Pommel, M.; Sauvezie, B. IL-1ra and IL-1 production in human oral mucosal epithelial cells in culture: Differential modulation by TGF-beta1 and IL-4. Clin. Exp. Immunol. 2002, 127, 53–59. [Google Scholar] [CrossRef] [PubMed]
- Sporn, M.B.; Roberts, A.B.; Wakefield, L.M.; Assoian, R.K. Transforming growth factor-beta: Biological function and chemical structure. Science 1986, 233, 532–534. [Google Scholar] [CrossRef] [PubMed]
- Min, B.M.; Woo, K.M.; Lee, G.; Park, N.H. Terminal differentiation of normal human oral keratinocytes is associated with enhanced cellular TGF-beta and phospholipase C-gamma 1 levels and apoptotic cell death. Exp. Cell Res. 1999, 249, 377–385. [Google Scholar] [CrossRef] [PubMed]
- Phillips, W.G.; Feldmann, M.; Breathnach, S.M.; Brennan, F.M. Modulation of the IL-1 cytokine network in keratinocytes by intracellular IL-1 alpha and IL-1 receptor antagonist. Clin. Exp. Immunol. 1995, 101, 177–182. [Google Scholar] [CrossRef] [PubMed]
- Okamoto, Y.; Gotoh, Y.; Uemura, O.; Tanaka, S.; Ando, T.; Nishida, M. Age-dependent decrease in serum transforming growth factor (TGF)-beta 1 in healthy Japanese individuals; population study of serum TGF-beta 1 level in Japanese. Dis. Markers 2005, 21, 71–74. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ogawa, N.; Dang, H.; Lazaridis, K.; McGuff, H.S.; Aufdemorte, T.B.; Talal, N. Analysis of transforming growth factor beta and other cytokines in autoimmune exocrinopathy (Sjögren’s syndrome). J. Interferon Cytokine Res. 1995, 15, 759–767. [Google Scholar] [CrossRef] [PubMed]
- Hilkens, C.M.; Kalinski, P.; de Boer, M.; Kapsenberg, M.L. Human dendritic cells require exogenous interleukin-12-inducing factors to direct the development of naive T-helper cells toward the Th1 phenotype. Blood 1997, 90, 1920–1926. [Google Scholar] [CrossRef]
- Kaliński, P.; Smits, H.H.; Schuitemaker, J.H.; Vieira, P.L.; van Eijk, M.; de Jong, E.C.; Wierenga, E.A.; Kapsenberg, M.L. IL-4 is a mediator of IL-12p70 induction by human Th2 cells: Reversal of polarized Th2 phenotype by dendritic cells. J. Immunol. 2000, 165, 1877–1881. [Google Scholar] [CrossRef] [Green Version]
- Wu, C.Y.; Demeure, C.; Kiniwa, M.; Gately, M.; Delespesse, G. IL-12 induces the production of IFN-gamma by neonatal human CD4 T cells. J. Immunol. 1993, 151, 1938–1949. [Google Scholar]
- Heufler, C.; Koch, F.; Stanzl, U.; Topar, G.; Wysocka, M.; Trinchieri, G.; Enk, A.; Steinman, R.M.; Romani, N.; Schuler, G. Interleukin-12 is produced by dendritic cells and mediates T helper 1 development as well as interferon-gamma production by T helper 1 cells. Eur. J. Immunol. 1996, 26, 659–668. [Google Scholar] [CrossRef]
- Lalani, T.; Simmons, R.K.; Ahmed, A.R. Biology of IL-5 in health and disease. Ann. Allergy Asthma Immunol. 1999, 82, 317–332, quiz 332–333. [Google Scholar] [CrossRef]
- Yamaguchi, Y.; Suda, T.; Shiozaki, H.; Miura, Y.; Hitoshi, Y.; Tominaga, A.; Takatsu, K.; Kasahara, T. Role of IL-5 in IL-2-induced eosinophilia. In vivo and in vitro expression of IL-5 mRNA by IL-2. J. Immunol. 1990, 145, 873–877. [Google Scholar]
- Dubucquoi, S.; Desreumaux, P.; Janin, A.; Klein, O.; Goldman, M.; Tavernier, J.; Capron, A.; Capron, M. Interleukin 5 synthesis by eosinophils: Association with granules and immunoglobulin-dependent secretion. J. Exp. Med. 1994, 179, 703–708. [Google Scholar] [CrossRef] [PubMed]
- Kleiner, G.; Marcuzzi, A.; Zanin, V.; Monasta, L.; Zauli, G. Cytokine levels in the serum of healthy subjects. Mediat. Inflamm. 2013, 2013, 434010. [Google Scholar] [CrossRef]
- Kuwahara, M.; Yamashita, M.; Shinoda, K.; Tofukuji, S.; Onodera, A.; Shinnakasu, R.; Motohashi, S.; Hosokawa, H.; Tumes, D.; Iwamura, C.; et al. The transcription factor Sox4 is a downstream target of signaling by the cytokine TGF-β and suppresses T(H)2 differentiation. Nat. Immunol. 2012, 13, 778–786. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kishimoto, T. IL-6: From its discovery to clinical applications. Int. Immunol. 2010, 22, 347–352. [Google Scholar] [CrossRef] [Green Version]
- Yun, U.J.; Park, S.E.; Jo, Y.S.; Kim, J.; Shin, D.Y. DNA damage induces the IL-6/STAT3 signaling pathway, which has anti-senescence and growth-promoting functions in human tumors. Cancer Lett. 2012, 323, 155–160. [Google Scholar] [CrossRef]
- Scheller, J.; Chalaris, A.; Schmidt-Arras, D.; Rose-John, S. The pro- and anti-inflammatory properties of the cytokine interleukin-6. Biochim. Biophys. Acta 2011, 1813, 878–888. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kyurkchiev, D.; Bochev, I.; Ivanova-Todorova, E.; Mourdjeva, M.; Oreshkova, T.; Belemezova, K.; Kyurkchiev, S. Secretion of immunoregulatory cytokines by mesenchymal stem cells. World J. Stem Cells 2014, 6, 552–570. [Google Scholar] [CrossRef]
- Chan, C.K.; Wu, K.H.; Lee, Y.S.; Hwang, S.M.; Lee, M.S.; Liao, S.K.; Cheng, E.H.; See, L.C.; Tsai, C.N.; Kuo, M.L.; et al. The comparison of interleukin 6-associated immunosuppressive effects of human ESCs, fetal-type MSCs, and adult-type MSCs. Transplantation 2012, 94, 132–138. [Google Scholar] [CrossRef] [PubMed]
- Kimura, A.; Kishimoto, T. IL-6: Regulator of Treg/Th17 balance. Eur. J. Immunol. 2010, 40, 1830–1835. [Google Scholar] [CrossRef]
- Acosta-Rodriguez, E.V.; Napolitani, G.; Lanzavecchia, A.; Sallusto, F. Interleukins 1beta and 6 but not transforming growth factor-beta are essential for the differentiation of interleukin 17-producing human T helper cells. Nat. Immunol. 2007, 8, 942–949. [Google Scholar] [CrossRef] [PubMed]
- Manel, N.; Unutmaz, D.; Littman, D.R. The differentiation of human T(H)-17 cells requires transforming growth factor-beta and induction of the nuclear receptor RORgammat. Nat. Immunol. 2008, 9, 641–649. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mantovani, A.; Cassatella, M.A.; Costantini, C.; Jaillon, S. Neutrophils in the activation and regulation of innate and adaptive immunity. Nat. Rev. Immunol. 2011, 11, 519–531. [Google Scholar] [CrossRef]
- Mojsilović, S.; Jauković, A.; Santibañez, J.F.; Bugarski, D. Interleukin-17 and its implication in the regulation of differentiation and function of hematopoietic and mesenchymal stem cells. Mediat. Inflamm. 2015, 2015, 470458. [Google Scholar] [CrossRef] [Green Version]
- Fossiez, F.; Banchereau, J.; Murray, R.; Van Kooten, C.; Garrone, P.; Lebecque, S. Interleukin-17. Int. Rev. Immunol. 1998, 16, 541–551. [Google Scholar] [CrossRef] [PubMed]
- Carp, H.; Torchinsky, A.; Fein, A.; Toder, V. Hormones, cytokines and fetal anomalies in habitual abortion. Gynecol. Endocrinol. 2001, 15, 472–483. [Google Scholar] [CrossRef]
- Jaskoll, T.H.; Choy, H.A.; Chen, H.; Melnick, M. Developmental expression and CORT-regulation of TGF-band EGF receptor mRNA during mouse palatal morphogenesis: Correlation between CORT-induced cleft palate and TGF-b2 mRNA expression. Teratology 1996, 54, 34–44. [Google Scholar] [CrossRef]
- Morgan, E.T. Regulation of cytochromes P450 during inflammation and infection. Drug Metab. Rev. 1997, 29, 1129–1188. [Google Scholar] [CrossRef]
- Beaty, T.H.; Ruczinski, I.; Murray, J.C.; Marazita, M.L.; Munger, R.G.; Hetmanski, J.B.; Murray, T.; Redett, R.J.; Fallin, M.D.; Liang, K.Y.; et al. Evidence for gene-environment interaction in a genome wide study of nonsyndromic cleft palate. Genet. Epidemiol. 2011, 35, 469–478. [Google Scholar] [CrossRef]
- Wu, T.; Schwender, H.; Ruczinski, I.; Murray, J.C.; Marazita, M.L.; Munger, R.G.; Hetmanski, J.B.; Parker, M.M.; Wang, P.; Murray, T.; et al. Evidence of gene-environment interaction for two genes on chromosome 4 and environmental tobacco smoke in controlling the risk of nonsyndromic cleft palate. PLoS ONE 2014, 9, e88088. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Moynihan, J.A.; Callahan, T.A.; Kelley, S.P.; Campbell, L.M. Adrenal hormone modulation of type 1 and type 2 cytokine production by spleen cells: Dexamethasone and dehydroepiandrosterone suppress interleukin-2, interleukin-4, and interferon-gamma production in vitro. Cell. Immunol. 1998, 184, 58–64. [Google Scholar] [CrossRef]
- Rook, G.A.; Hernandez-Pando, R.; Lightman, S.L. Hormones, peripherally activated prohormones and regulation of the Th1/Th2 balance. Immunol. Today 1994, 15, 301–303. [Google Scholar] [CrossRef]
- Piccinni, M.P.; Scaletti, C.; Maggi, E.; Romagnani, S. Role of hormone-controlled Th1- and Th2-type cytokines in successful pregnancy. J. Neuroimmunol. 2000, 109, 30–33. [Google Scholar] [CrossRef]
- Piccinni, M.P.; Bani, D.; Beloni, L.; Manuelli, C.; Mavilia, C.; Vocioni, F.; Bigazzi, M.; Sacchi, T.B.; Romagnani, S.; Maggi, E. Relaxin favors the development of activated human T cells into Th1-like effectors. Eur. J. Immunol. 1999, 29, 2241–2247. [Google Scholar] [CrossRef]
- Hu, S.K.; Mitcho, Y.L.; Rath, N.C. Effect of estradiol on interleukin 1 synthesis by macrophages. Int. J. Immunopharmacol. 1988, 10, 247–252. [Google Scholar] [CrossRef] [PubMed]
| Patient No | Age (in Months) | Gender | Clinical Diagnosis * | Remarks |
|---|---|---|---|---|
| 1 | 7 | M | Cheiloschisis partialis sinistra | Preterm birth in gestational week 37; Rh conflict; mother showed glucose tolerance disturbance |
| 2 | 6 | F | Cheilognathoschisis dextra | Born in the gestational 42nd week; cleft detected in ultrasound in week 22; history of cleft lip and palate in family tree |
| 3 | 4 | M | Cheilognathouranoschisis dextra | Born in the gestational 41st week; cleft detected in the ultrasound in week 22; mother reported urinary tract infection during the pregnancy |
| 4 | 10 | F | Cheiloschisis partialis dextra | Preterm birth in gestational week 39 |
| 5 | 13 | F | Cheilognathoschisis bilateralis | Cleft detected in the ultrasound in week 28; mother used Paracetamol during the pregnancy due to tooth aches |
| 6 | 4 | M | Cheilognathouranoschisis bilateralis | Preterm birth in gestational week 39; both parents were regular smokers |
| 7 | 4 | M | Cheilognathoschisis sinistra | Multiple stigma: dysplastic ears, palm stigma |
| 8 | 4 | M | Uranoschisis partialis sinistra | - |
| 9 | 7 | M | Cheiloschisis partialis sinistra | There was reported high risk of abortion during pregnancy |
| 10 | 4 | M | Cheilognathouranoschisis sinistra | - |
| 11 | 4 | F | Cheilognathouranoschisis dextra | - |
| 12 | 4 | M | Cheiloschisis dextra | Preterm birth in gestational week 39 |
| Cytokine | Mean Concentration | Standard Deviation | Minimum Concentration | Maximum Concentration | Coefficient of Variance (CV%) * |
|---|---|---|---|---|---|
| IL-2 | 1.58 | 1.20 | 0.19 | 4.29 | 75.95 |
| IL-4 | 1.06 | 0.28 | 0.78 | 1.40 | 26.42 |
| IL-5 | - | - | - | - | - |
| IL-6 | 0.59 | 0.18 | 0.32 | 0.87 | 30.51 |
| IL-10 | 1.13 | 0.47 | 0.72 | 1.96 | 41.59 |
| IL-12 | 0.93 | 0.25 | 0.65 | 1.25 | 26.88 |
| IL-13 | 0.57 | 0.17 | 0.26 | 0.99 | 29.82 |
| IL-17A | 1.11 | 0.74 | 0.10 | 2.48 | 66.67 |
| IFN-γ | 0.79 | 0.50 | 0.23 | 1.66 | 63.29 |
| TNF-α | 36.93 | 20.84 | 14.69 | 88.68 | 56.43 |
| G-CSF | 0.70 | 0.47 | 0.11 | 1.70 | 67.14 |
| TGFβ-1 | 152.01 | 69.83 | 90.30 | 248.40 | 45.94 |
| Patient No | IL-2 | IL-4 | IL-6 | IL-10 | IL-12 | IL-13 | IL-17A |
|---|---|---|---|---|---|---|---|
| Cheiloschisis | |||||||
| 1 | 0.185 | 0.776 | 0.361 | 0.723 | 0.739 | 0.412 | 0.100 |
| 4 | 0.277 | 0.790 | 0.315 | 0.722 | 0.648 | 0.453 | - |
| 9 | 1.650 | - | 0.608 | - | - | 0.565 | 1.305 |
| 12 | 1.618 | - | 0.516 | - | - | 0.501 | 1.011 |
| Cheilognathoschisis | |||||||
| 2 | 0.798 | 1.401 | 0.678 | 1.290 | 1.248 | 0.576 | 0.777 |
| 5 | 0.554 | 1.248 | 0.867 | 1.150 | 1.118 | 0.615 | 0.660 |
| 7 | 1.715 | - | 0.573 | - | - | 0.600 | 0.939 |
| Cheilognathouranoschisis | |||||||
| 3 | 0.839 | 1.104 | 0.428 | 0.945 | 0.912 | 0.605 | 0.573 |
| 6 | 4.292 | - | - | 1.960 | - | 0.261 | - |
| 10 | 2.435 | - | 0.620 | - | - | 0.583 | 2.480 |
| 11 | 2.912 | - | 0.868 | - | - | 0.992 | 2.248 |
| Uranoschisis | |||||||
| 8 | 1.684 | - | 0.608 | - | - | 0.643 | 0.974 |
| Patient No | IFN-γ | TNF-α | G-CSF | TGFβ-1 |
|---|---|---|---|---|
| Cheiloschisis | ||||
| 1 | 0.230 | 28.935 | 0.199 | * |
| 4 | 0.300 | 30.264 | 0.108 | * |
| 9 | 0.768 | 25.838 | 0.755 | 248.400 |
| 12 | 0.757 | 19.947 | 0.582 | 120.224 |
| Cheilognathoschisis | ||||
| 2 | - | 88.683 | 0.333 | 90.798 |
| 5 | 0.443 | 55.631 | 0.758 | * |
| 7 | 0.758 | 14.816 | 0.696 | 100.920 |
| Cheilognathouranoschisis | ||||
| 3 | 0.369 | 39.422 | 0.441 | * |
| 6 | - | 51.098 | - | 90.300 |
| 10 | 1.585 | 32.550 | 1.695 | 215.720 |
| 11 | 1.664 | 41.300 | 1.320 | 120.224 |
| Uranoschisis | ||||
| 8 | 0.982 | 14.687 | 0.794 | 109.402 |
| Cytokines | IL-2 | IL-4 | IL-6 | IL-10 | IL-12 | IL-13 | IL-17A | IFN-γ | TNF-α | G-CSF | TGFβ-1 |
|---|---|---|---|---|---|---|---|---|---|---|---|
| IL-2 | 1.000 | 0.700 | 0.515 | 0.771 | 0.600 | 0.231 | 0.842 ** | 0.952 ** | −0.056 | 0.809 ** | −0.071 |
| IL-4 | - | 1.000 | 0.800 | 0.900 * | 0.900 * | 0.700 | 1.000 ** | 1.000 ** | 1.000 ** | 0.600 | N.D. |
| IL-6 | - | - | 1.000 | 0.900 * | 0.900 * | 0.674 * | 0.480 | 0.802 ** | 0.478 | 0.729 * | 0.072 |
| IL-10 | - | - | - | 1.000 | 1.000 ** | −0.086 | 1.000 ** | 0.800 | 0.771 | 0.700 | −1.000 |
| IL-12 | - | - | - | - | 1.000 | 0.600 | 1.000 ** | 0.800 | 0.900 * | 0.700 | N.D. |
| IL-13 | - | - | - | - | - | 1.000 | 0.176 | 0.624 | 0.007 | 0.709 * | 0.238 |
| IL-17A | - | - | - | - | - | - | 1.000 | 0.900 ** | −0.188 | 0.770 ** | 0.893 ** |
| IFN-γ | - | - | - | - | - | - | - | 1.000 | −0.067 | 0.903 ** | 0.371 |
| TNF-α | - | - | - | - | - | - | - | - | 1.000 | −0.036 | −0.262 |
| G-CSF | - | - | - | - | - | - | - | - | - | 1.000 | 0.643 |
| TGFβ-1 | - | - | - | - | - | - | - | - | - | - | 1.000 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pilmane, M.; Jain, N.; Jain, S.; Akota, I.; Kroiča, J. Quantification of Cytokines in Lip Tissue from Infants Affected by Congenital Cleft Lip and Palate. Children 2021, 8, 140. https://0-doi-org.brum.beds.ac.uk/10.3390/children8020140
Pilmane M, Jain N, Jain S, Akota I, Kroiča J. Quantification of Cytokines in Lip Tissue from Infants Affected by Congenital Cleft Lip and Palate. Children. 2021; 8(2):140. https://0-doi-org.brum.beds.ac.uk/10.3390/children8020140
Chicago/Turabian StylePilmane, Māra, Nityanand Jain, Shivani Jain, Ilze Akota, and Juta Kroiča. 2021. "Quantification of Cytokines in Lip Tissue from Infants Affected by Congenital Cleft Lip and Palate" Children 8, no. 2: 140. https://0-doi-org.brum.beds.ac.uk/10.3390/children8020140