Inter-Observer and Intra-Observer Variations in the Assessment of Epithelial Dysplasia in Oral Lichenoid Diseases
Abstract
:1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Schlosser, B.J. Lichen planus and lichenoid reactions of the oral mucosa. Dermatol. Ther. 2010, 23, 251–267. [Google Scholar] [CrossRef] [PubMed]
- Silverman, S.; Gorsky, M.; Lozada-Nur, F. A prospective follow-up study of 570 patients with oral lichen planus: Persistence, remission, and malignant association. Oral Surg. Oral Med. Oral Pathol. 1985, 60, 30–34. [Google Scholar] [CrossRef]
- Van den Haute, V.; Antoine, J.L.; Lachapelle, J.M. Histopathological discriminant criteria between lichenoid drug eruption and idiopathic lichen planus: Retrospective study on selected samples. Dermatologica 1989, 179, 10–13. [Google Scholar] [CrossRef] [PubMed]
- Rotim, Z.; Bolanca, Z.; Rogulj, A.A.; Andabak, M.; Boras, V.V.; Vrdoljak, D.V. Oral lichen planus and oral lichenoid reaction—An update. Acta Clin. Croat. 2015, 54, 516–520. [Google Scholar] [PubMed]
- Van der Meij, E.H.; van der Waal, I. Lack of clinicopathologic correlation in the diagnosis of oral lichen planus based on the presently available diagnostic criteria and suggestions for modifications. J. Oral Pathol. Med. 2003, 32, 507–512. [Google Scholar] [CrossRef] [PubMed]
- Warnakulasuriya, S.; Reibel, J.; Bouquot, J.; Dabelsteen, E. Oral epithelial dysplasia classification systems: Predictive value, utility, weaknesses and scope for improvement. J. Oral Pathol. Med. 2008, 37, 127–133. [Google Scholar] [CrossRef] [PubMed]
- Van der Meij, E.H.; Reibel, J.; Slootweg, P.J.; van der Wal, J.E.; de Jong, W.F.; van der Waal, I. Interobserver and intraobserver variability in the histologic assessment of oral lichen planus. J. Oral Pathol. Med. 1999, 28, 274–277. [Google Scholar] [CrossRef]
- Kujan, O.; Khattab, A.; Oliver, R.J.; Roberts, S.A.; Thakker, N.; Sloan, P. Why oral histopathology suffers inter-observer variability on grading oral epithelial dysplasia: An attempt to understand the sources of variation. Oral Oncol. 2007, 43, 224–231. [Google Scholar] [CrossRef] [PubMed]
- Speight, P.M.; Abram, T.J.; Floriano, P.N.; James, R.; Vick, J.; Thornhill, M.H.; Murdoch, C.; Freeman, C.; Hegarty, A.M.; D’Apice, K.; et al. Interobserver agreement in dysplasia grading: Toward an enhanced gold standard for clinical pathology trials. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2015, 120, 474–482.e2. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Feldmeyer, L.; Suter, V.; Oeschger, C.; Cazzaniga, S.; Bornstein, M.; Simon, D.; Borradori, L.; Beltraminelli, H. Oral lichen planus and oral lichenoid lesions—An analysis of clinical and histopathological features. J. Eur. Acad. Dermatol. Venereol. 2020, 34, e104–e107. [Google Scholar] [CrossRef] [PubMed]
- El-Naggar, A.; Chan, J.; Grandis, J.; Takata, T.; Slootweg, P. WHO Classification of Head and Neck Tumours [Internet]. Available online: https://publications.iarc.fr/Book-And-Report-Series/Who-Classification-Of-Tumours/WHO-Classification-Of-Head-And-Neck-Tumours-2017 (accessed on 10 February 2021).
- Ranganathan, K.; Kavitha, L. Oral epithelial dysplasia: Classifications and clinical relevance in risk assessment of oral potentially malignant disorders. J. Oral Maxillofac. Pathol. 2019, 23, 19–27. [Google Scholar] [CrossRef] [PubMed]
- Van der Meij, E.H.; Mast, H.; van der Waal, I. The possible premalignant character of oral lichen planus and oral lichenoid lesions: A prospective five-year follow-up study of 192 patients. Oral Oncol. 2007, 43, 742–748. [Google Scholar] [CrossRef] [PubMed]
- Krutchkoff, D.J.; Eisenberg, E. Lichenoid dysplasia: A distinct histopathologic entity. Oral Surg. Oral Med. Oral Pathol. 1985, 60, 308–315. [Google Scholar] [CrossRef]
- Lodi, G.; Scully, C.; Carrozzo, M.; Griffiths, M.; Sugerman, P.B.; Thongprasom, K. Current controversies in oral lichen planus: Report of an international consensus meeting. Part 1. Viral infections and etiopathogenesis. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2005, 100, 40–51. [Google Scholar] [CrossRef] [PubMed]
- Ranganathan, K.; Kavitha, L.; Sharada, P.; Bavle, R.M.; Rao, R.S.; Pattanshetty, S.M.; Hazarey, V.K.; Madhura, M.G.; Nagaraj, T.; Lingappa, A.; et al. Intra-observer and inter-observer variability in two grading systems for oral epithelial dysplasia: A multi-centre study in India. J. Oral Pathol. Med. 2020, 49, 948–955. [Google Scholar] [CrossRef] [PubMed]
- Kujan, O.; Oliver, R.J.; Khattab, A.; Roberts, S.A.; Thakker, N.; Sloan, P. Evaluation of a new binary system of grading oral epithelial dysplasia for prediction of malignant transformation. Oral Oncol. 2006, 42, 987–993. [Google Scholar] [CrossRef]
- Küffer, R.; Lombardi, T. Premalignant lesions of the oral mucosa. A discussion about the place of oral intraepithelial neoplasia (OIN). Oral Oncol. 2002, 38, 125–130. [Google Scholar] [CrossRef]
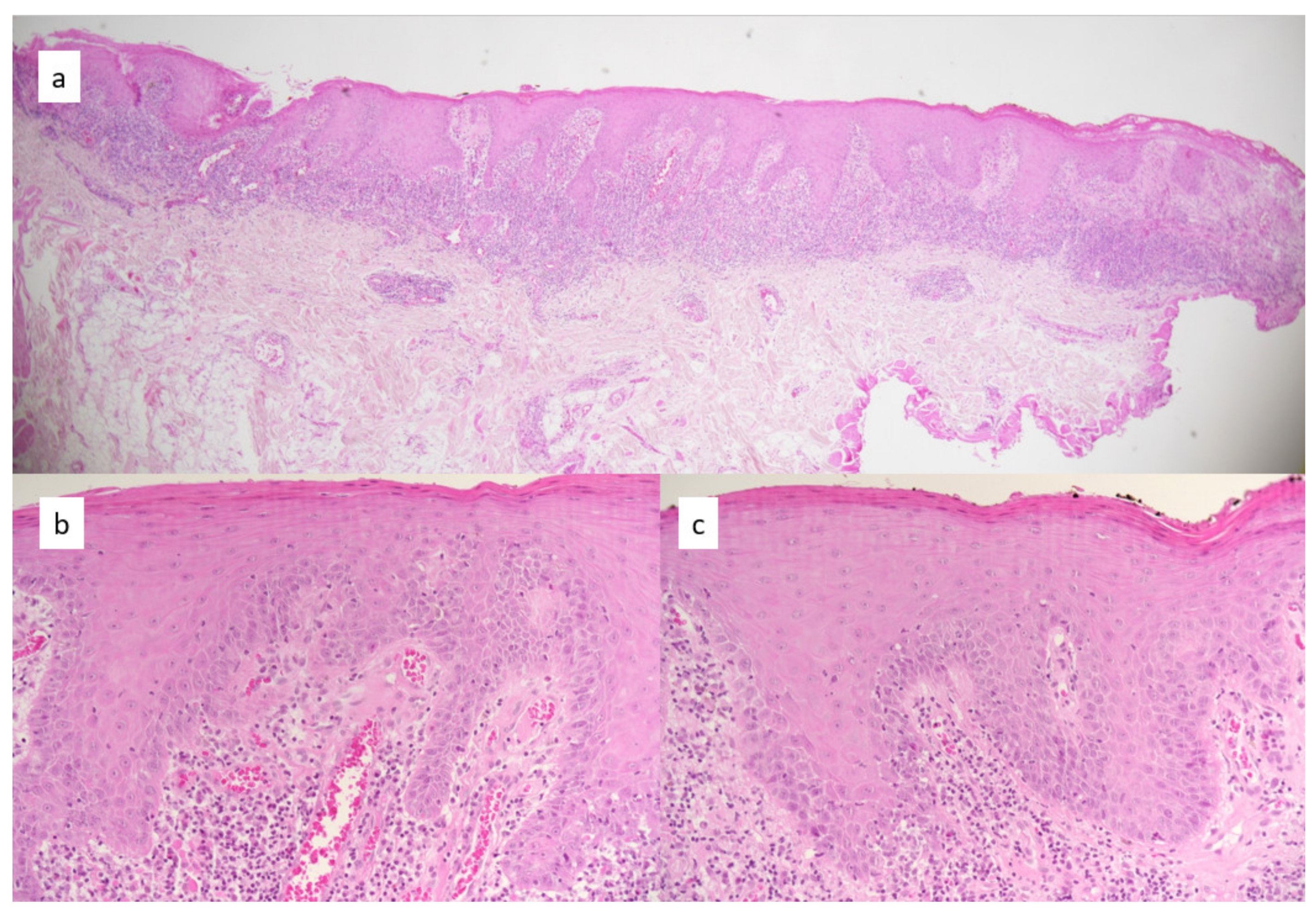
| First Assessment | Second Assessment | Weighted Kappa * (95% CI) | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| None | I | II | III | |||||||
| N | Row% | N | Row% | N | Row% | N | Row% | |||
| Rater: Pathologist 1 | None | 65 | 73.0% | 24 | 27.0% | 0 | 0.0% | 0 | 0.0% | 0.36 (0.19, 0.53) |
| I | 7 | 31.8% | 14 | 63.6% | 1 | 4.5% | 0 | 0.0% | ||
| II | 0 | 0.0% | 1 | 100.0% | 0 | 0.0% | 0 | 0.0% | ||
| III | 0 | 0.0% | 0 | 0.0% | 0 | 0.0% | 0 | 0.0% | ||
| Rater: Pathologist 2 | None | 68 | 75.6% | 15 | 16.7% | 7 | 7.8% | 0 | 0.0% | 0.34 (0.14, 0.54) |
| I | 7 | 35.0% | 9 | 45.0% | 4 | 20.0% | 0 | 0.0% | ||
| II | 0 | 0.0% | 1 | 50.0% | 0 | 0.0% | 1 | 50.0% | ||
| III | 0 | 0.0% | 0 | 0.0% | 0 | 0.0% | 0 | 0.0% | ||
| Rater: Pathologist 3 | None | 84 | 94.4% | 5 | 5.6% | 0 | 0.0% | 0 | 0.0% | 0.52 (0.30, 0.75) |
| I | 14 | 73.7% | 2 | 10.5% | 3 | 15.8% | 0 | 0.0% | ||
| II | 1 | 25.0% | 1 | 25.0% | 1 | 25.0% | 1 | 25.0% | ||
| III | 0 | 0.0% | 0 | 0.0% | 0 | 0.0% | 0 | 0.0% | ||
| Rater: Pathologist 4 | None | 0 | 0.0% | 0 | 0.0% | 0 | 0.0% | 0 | 0.0% | 0.65 (0.50, 0.80) |
| I | 0 | 0.0% | 7 | 38.9% | 10 | 55.6% | 1 | 5.6% | ||
| II | 0 | 0.0% | 4 | 5.9% | 57 | 83.8% | 7 | 10.3% | ||
| III | 0 | 0.0% | 1 | 3.8% | 1 | 3.8% | 24 | 92.3% | ||
| Dysplasia Assessement | Path. 1 | Path. 2 | Path. 3 | Path. 4 | Weighted Kappa * (95% CI) | Weighted Kappa (w/o Path. 4) (95% CI) | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| N | Col% | N | Col% | N | Col% | N | Col% | ||||
| First dysplasia assessment | None | 89 | 79.5% | 90 | 80.4% | 89 | 79.5% | 0 | 0.0% | 0.05 (−0.005, 0.13) | 0.13 (0.02, 0.25) |
| I | 22 | 19.6% | 20 | 17.9% | 19 | 17.0% | 18 | 16.1% | |||
| II | 1 | 0.9% | 2 | 1.8% | 4 | 3.6% | 68 | 60.7% | |||
| III | 0 | 0.0% | 0 | 0.0% | 0 | 0.0% | 26 | 23.2% | |||
| Second dysplasia assessment | None | 72 | 64.3% | 75 | 67.0% | 99 | 88.4% | 0 | 0.0% | 0.11 (0.002, 0.25) | 0.37 (0.25, 0.49) |
| I | 39 | 34.8% | 25 | 22.3% | 8 | 7.1% | 12 | 10.7% | |||
| II | 1 | 0.9% | 11 | 9.8% | 4 | 3.6% | 68 | 60.7% | |||
| III | 0 | 0.0% | 1 | 0.9% | 1 | 0.9% | 32 | 28.6% | |||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zohdy, M.; Cazzaniga, S.; Nievergelt, H.; Blum, R.; Suter, V.G.A.; Feldmeyer, L.; Beltraminelli, H. Inter-Observer and Intra-Observer Variations in the Assessment of Epithelial Dysplasia in Oral Lichenoid Diseases. Dermatopathology 2021, 8, 84-88. https://0-doi-org.brum.beds.ac.uk/10.3390/dermatopathology8020013
Zohdy M, Cazzaniga S, Nievergelt H, Blum R, Suter VGA, Feldmeyer L, Beltraminelli H. Inter-Observer and Intra-Observer Variations in the Assessment of Epithelial Dysplasia in Oral Lichenoid Diseases. Dermatopathology. 2021; 8(2):84-88. https://0-doi-org.brum.beds.ac.uk/10.3390/dermatopathology8020013
Chicago/Turabian StyleZohdy, Marwa, Simone Cazzaniga, Helga Nievergelt, Roland Blum, Valérie G. A. Suter, Laurence Feldmeyer, and Helmut Beltraminelli. 2021. "Inter-Observer and Intra-Observer Variations in the Assessment of Epithelial Dysplasia in Oral Lichenoid Diseases" Dermatopathology 8, no. 2: 84-88. https://0-doi-org.brum.beds.ac.uk/10.3390/dermatopathology8020013