Herb–Drug Interactions: Worlds Intersect with the Patient at the Center
Abstract: Background
1. Introduction
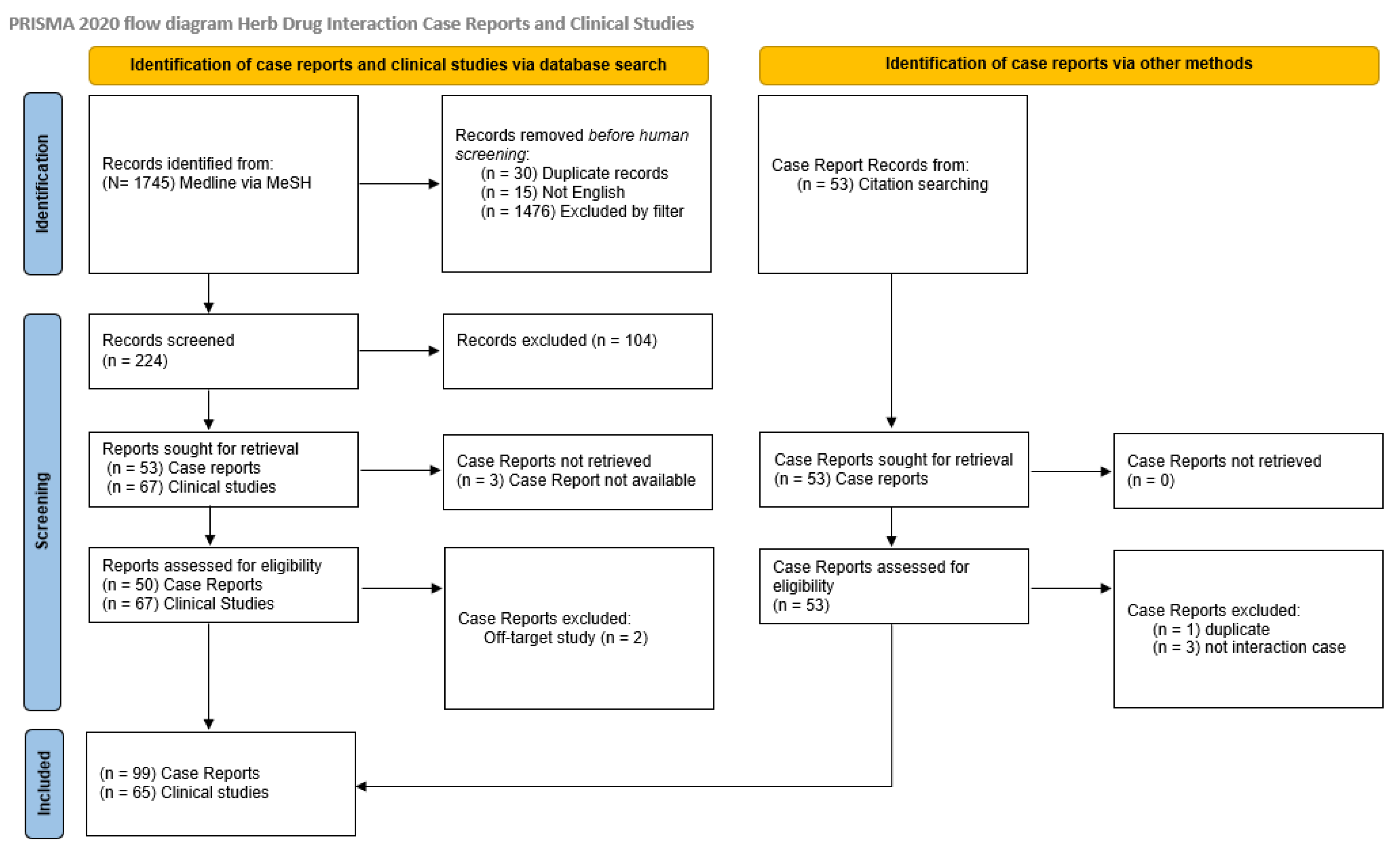
2. Materials and Methods
3. Results
3.1. Case Report Analysis
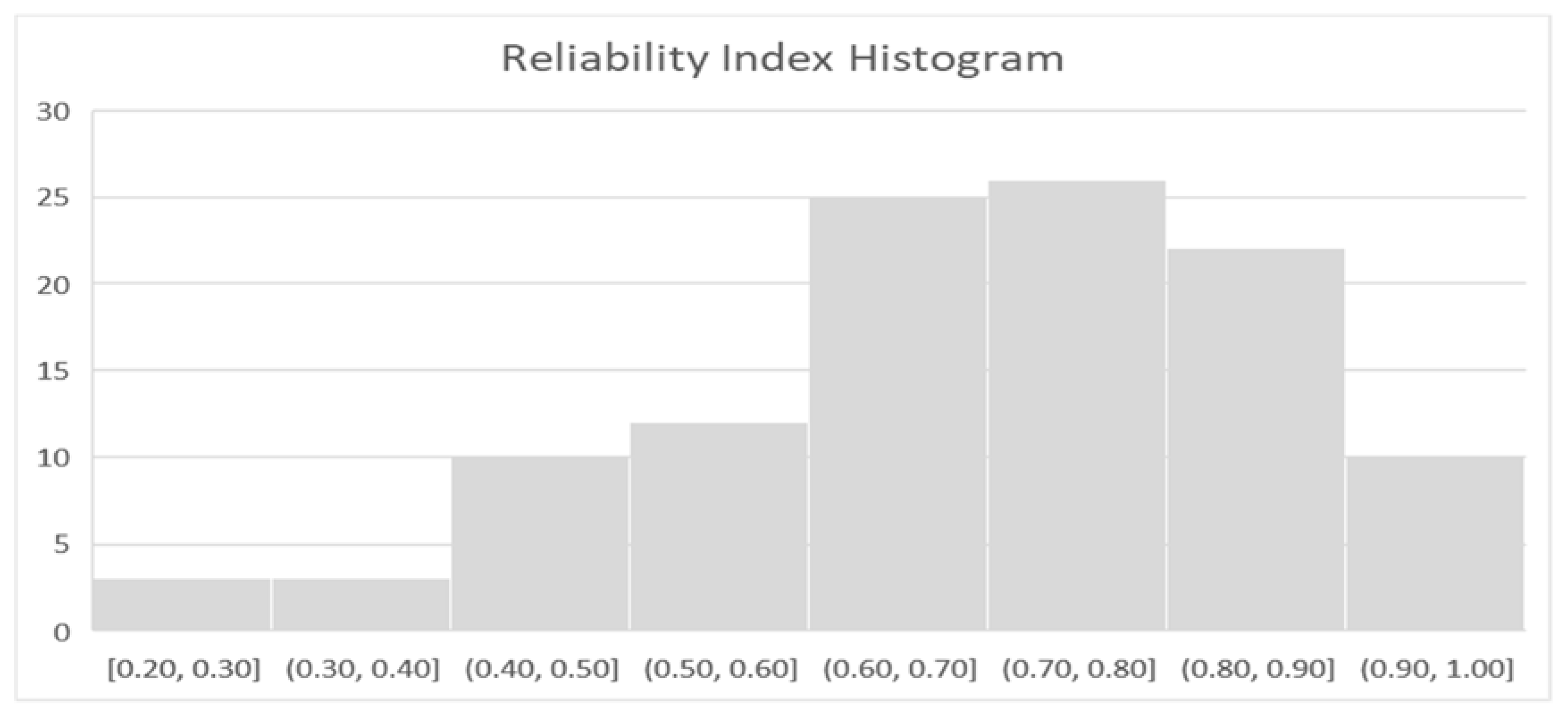
3.1.1. Reliability Index Results
3.1.2. Qualitative Analysis of Case Reports
3.2. Case Report and Study Comparison
3.3. Case Report and Interaction Checker Comparison
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Smith, T.; May, G.; Eckl, V.; Morton Reynolds, C. US Sales of Herbal Supplements Increase by 8.6% in 2019. HerbalGram 2020, 127, 54–69. Available online: http://cms.herbalgram.org/herbalgram/issue127/hg127-mktrpt-2019.html (accessed on 20 December 2020).
- Martin, K.J.; Jordan, T.R.; Vassar, A.D.; White, D.B. Herbal and Nonherbal Alternative Medicine Use in Northwest Ohio. Ann. Pharmacother. 2002, 36, 1862–1869. [Google Scholar] [CrossRef] [PubMed]
- Clarke, T.C.; Black, L.I.; Stussman, B.J.; Barnes, P.M.; Nahin, R.L. Trends in the Use of Complementary Health Approaches among Adults: United States, 2002–2012 National Health Statistics Reports No. 79; National Center for Health Statistics: Hyattsville, MD, USA, 2015. [Google Scholar]
- Rashrash, M.; Schommer, J.C.; Brown, L.M. Prevalence and Predictors of Herbal Medicine Use Among Adults in the United States. J. Patient Exp. 2017, 4, 108–113. [Google Scholar] [CrossRef]
- Low Dog, T. The use of botanicals during pregnancy and lactation. Altern. Ther. Health Med. 2009, 15, 54–58. [Google Scholar] [PubMed]
- Percha, B.; Altman, R.B. Informatics confronts drug–drug interactions. Trends Pharmacol. Sci. 2013, 34, 178–184. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Su, Q.; Li, Y. Interaction between Warfarin and the Herbal Product Shengmai-Yin: A Case Report of Intracerebral Hematoma. Yonsei Med. J. 2010, 51, 793–796. [Google Scholar] [CrossRef] [Green Version]
- Becker, B.; Greene, J.; Evanson, J.; Chidsey, G.; Stone, W. Ginseng-induced diuretic resistance. JAMA 1996, 276, 606–607. [Google Scholar] [CrossRef]
- Costa, M.L.; Rodrigues, J.A.; Azevedo, J.; Vasconcelos, V.; Eiras, E.; Campos, M.G. Hepatotoxicity induced by paclitaxel interaction with turmeric in association with a microcystin from a contaminated dietary supplement. Toxicon 2018, 150, 207–211. [Google Scholar] [CrossRef] [PubMed]
- Fasinu, P.S.; Bouic, P.J.; Rosenkranz, B. An Overview of the Evidence and Mechanisms of Herb–Drug Interactions. Front. Pharmacol. 2012, 3, 69. [Google Scholar] [CrossRef] [Green Version]
- Kupiec, T.; Raj, V. Fatal Seizures Due to Potential Herb-Drug Interactions with Ginkgo biloba. J. Anal. Toxicol. 2005, 29, 755–758. [Google Scholar] [CrossRef]
- Lee, A.; Chui, P.T.; Aun, C.S.T.; Gin, T.; Lau, A.S.C. Possible interaction between sevoflurane and Aloe vera. Ann. Pharmacother. 2004, 38, 1651–1654. [Google Scholar] [CrossRef] [PubMed]
- Mergenhagen, K.A.; Sherman, O. Elevated International Normalized Ratio after concurrent ingestion of cranberry sauce and warfarin. Am. J. Health Pharm. 2008, 65, 2113–2116. [Google Scholar] [CrossRef] [PubMed]
- Shaw, D.; Graeme, L.; Pierre, D.; Elizabeth, W.; Kelvin, C. Pharmacovigilance of herbal medicine. J. Ethnopharmacol. 2012, 140, 513–518. [Google Scholar] [CrossRef]
- Shetti, S.; Kumar, C.D.; Sriwastava, N.K.; Sharma, I.P. Pharmacovigilance of herbal medicines: Current state and future directions. Pharmacogn. Mag. 2011, 7, 69–73. [Google Scholar] [CrossRef] [Green Version]
- Williamson, E.; Driver, S.; Baxter, K. (Eds.) Stockley’s Herbal Medicines Interactions; Pharmaceutical Press: London, UK, 2009. [Google Scholar]
- Russo, E.B. Taming THC: Potential cannabis synergy and phytocannabinoid-terpenoid entourage effects. Br. J. Pharmacol. 2011, 163, 1344–1364. [Google Scholar] [CrossRef] [PubMed]
- Weathers, P.J.; Arsenault, P.; Covello, P.S.; McMickle, A.; Teoh, K.H.; Reed, D. Artemisinin production in Artemisia annua: Studies in planta and results of a novel delivery method for treating malaria and other neglected diseases. Phytochem. Rev. 2010, 10, 173–183. [Google Scholar] [CrossRef] [Green Version]
- Sobieraj, D.M.; Freyer, C.W. Probable Hypoglycemic Adverse Drug Reaction Associated with Prickly Pear Cactus, Glipizide, and Metformin in a Patient with Type 2 Diabetes Mellitus. Ann. Pharmacother. 2010, 44, 1334–1337. [Google Scholar] [CrossRef] [PubMed]
- Al-Jenoobi, F.I.; Al-Thukair, A.A.; Alam, M.A.; Abbas, F.A.; Al-Mohizea, A.M.; Alkharfy, K.M.; Al-Suwayeh, S.A. Effect of Curcuma longa on CYP2D6- and CYP3A4-mediated metabolism of dextromethorphan in human liver microsomes and healthy human subjects. Eur. J. Drug Metab. Pharmacokinet. 2014, 40, 61–66. [Google Scholar] [CrossRef]
- Awortwe, C.; Makiwane, M.; Reuter, H.; Muller, C.; Louw, J.; Rosenkranz, B. Critical evaluation of causality assessment of herb-drug interactions in patients. Br. J. Clin. Pharmacol. 2018, 84, 679–693. [Google Scholar] [CrossRef] [Green Version]
- Chen, X.-W.; Sneed, K.B.; Pan, S.-Y.; Cao, C.; Kanwar, J.R.; Chew, H.; Zhou, S.-F. Herb-Drug Interactions and Mechanistic and Clinical Considerations. Curr. Drug Metab. 2012, 13, 640–651. [Google Scholar] [CrossRef]
- Aronson, J.K. Toward standardized reporting of drug interactions: The READI checklist for anecdotal reports. Expert Rev. Clin. Pharmacol. 2015, 8, 399–409. [Google Scholar] [CrossRef] [PubMed]
- Ng, J.Y.; Munford, V.; Thakar, H. Web-based online resources about adverse interactions or side effects associated with complementary and alternative medicine: A systematic review, summarization and quality assessment. BMC Med. Inform. Decis. Mak. 2020, 20, 1–20. [Google Scholar] [CrossRef]
- World Health Organization. The WHO Programme for International Drug Monitoring. In Essential Medicines and Health Products; WHO Website; 2015; Available online: who.int/medicines/areas/quality_safety/safety_efficacy/National_PV_Centres_Map/en/ (accessed on 7 January 2021).
- United States Food and Drug Administration. FDA Adverse Event Reporting System (FAERS) Public Dashboard. 2021. Available online: https://fis.fda.gov/sense/app/d10be6bb-494e-4cd2-82e4-0135608ddc13/sheet/7a47a261-d58b-4203-a8aa-6d3021737452/state/analysis (accessed on 28 October 2020).
- Uppsala Monitoring Center. Vigibase. 2012. Available online: https://www.who-umc.org/vigibase/vigibase/ (accessed on 3 March 2021).
- Awortwe, C.; Bruckmueller, H.; Cascorbi, I. Interaction of herbal products with prescribed medications: A systematic review and meta-analysis. Pharmacol. Res. 2019, 141, 397–408. [Google Scholar] [CrossRef]
- Borse, S.P.; Singh, D.P.; Nivsarkar, M. Understanding the relevance of herb–drug interaction studies with special focus on interplays: A prerequisite for integrative medicine. Porto Biomed. J. 2019, 4, e15. [Google Scholar] [CrossRef]
- Liu, D.; Zhang, L.; Duan, L.X.; Wu, J.J.; Hu, M.; Liu, Z.Q.; Wang, C.Y. Potential of herb-drug / herb interactions between substrates and inhibitors of UGTs derived from herbal medicines. Pharmacol. Res. 2019, 150, 104510. [Google Scholar] [CrossRef] [PubMed]
- Rombolà, L.; Scuteri, D.; Marilisa, S.; Watanabe, C.; Morrone, L.A.; Bagetta, G.; Corasaniti, M.T. Pharmacokinetic Interactions between Herbal Medicines and Drugs: Their Mechanisms and Clinical Relevance. Life 2020, 10, 106. [Google Scholar] [CrossRef] [PubMed]
- Fugh-Berman, A.; Ernst, E. Herb-drug interactions: Review and assessment of report reliability. Br. J. Clin. Pharmacol. 2001, 52, 587–595. [Google Scholar] [CrossRef] [Green Version]
- VERBI Software. MAXQDA 2020; VERBI Software: Berlin, Germany, 2019. [Google Scholar]
- Gnjidic, D.; Hilmer, S.; Blyth, F.M.; Naganathan, V.; Waite, L.; Seibel, M.; McLachlan, A.; Cumming, R.; Handelsman, D.J.; Le Couteur, D. Polypharmacy cutoff and outcomes: Five or more medicines were used to identify community-dwelling older men at risk of different adverse outcomes. J. Clin. Epidemiol. 2012, 65, 989–995. [Google Scholar] [CrossRef]
- Turner, J.P.; Jamsen, K.M.; Shakib, S.; Singhal, N.; Prowse, R.; Bell, J.S. Polypharmacy cut-points in older people with cancer: How many medications are too many? Support. Care Cancer 2016, 24, 1831–1840. [Google Scholar] [CrossRef] [PubMed]
- Lexicomp Online Database; Lexicomp Inc.: Hudson, OH, USA, 2021; Available online: http://online.lexi.com (accessed on 15 May 2021).
- Whirl-Carrillo, M.; McDonagh, E.M.; Hebert, J.M.; Gong, L.; Sangkuhl, K.; Thorn, C.F.; Altman, R.B.; Klein, T.E. Pharmacogenomics Knowledge for Personalized Medicine. Clin. Pharmacol. Ther. 2012, 92, 414–417. [Google Scholar] [CrossRef]
- IntegrativePro Drug-Nutrient Interaction Checker; Integrative Therapeutics, LLC: Green Bay, WI, USA, 2021; Available online: https://www.integrativepro.com/drug-nutrient-interaction-checker (accessed on 15 May 2021).
- Medscape Drug Interaction Checker. 2021. Available online: https://reference.medscape.com/drug-interactionchecker (accessed on 15 May 2021).
- Memorial Sloan Kettering Cancer Center Search About Herbs. 2021. Available online: https://www.mskcc.org/cancer-care/diagnosis-treatment/symptom-management/integrative-medicine/herbs/search (accessed on 15 May 2021).
- Natural Medicines Online Database; Therapeutic Research Center: San Francisco, CA, USA, 2021; Available online: https://naturalmedicines.therapeuticresearch.com (accessed on 15 May 2021).
- IBM Corp. IBM SPSS Statistics for Windows; Version 27.0.; IBM Corp: Armonk, NY, USA, 2020. [Google Scholar]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef]
- Ben Abacha, A.; Chowdhury, F.M.; Karanasiou, A.; Mrabet, Y.; Lavelli, A.; Zweigenbaum, P. Text mining for pharmacovigilance: Using machine learning for drug name recognition and drug–drug interaction extraction and classification. J. Biomed. Inform. 2015, 58, 122–132. [Google Scholar] [CrossRef] [Green Version]
- Thompson, P.; Daikou, S.; Ueno, K.; Batista-Navarro, R.; Tsujii, J.; Ananiadou, S. Annotation and detection of drug effects in text for pharmacovigilance. J. Cheminform. 2018, 10, 1–33. [Google Scholar] [CrossRef]
- Naranjo, C.A.; Busto, U.; Sellers, E.M.; Sandor, P.; Ruiz, I.; Roberts, E.A.; Janecek, E.; Domecq, C.; Greenblatt, D.J. A method for estimating the probability of adverse drug reactions. Clin. Pharmacol. Ther. 1981, 30, 239–245. [Google Scholar] [CrossRef]
- Horn, J.R.; Hansten, P.D.; Chan, L.-N. Proposal for a New Tool to Evaluate Drug Interaction Cases. Ann. Pharmacother. 2007, 41, 674–680. [Google Scholar] [CrossRef]
- Council for International Organizations of Medical Sciences. Cumulative Pharmacovigilance Glossary. [Internet Site]. 2021. Available online: https://cioms.ch/wp-content/uploads/2021/03/CIOMS-Cumulative-Glossary_v1.1_3Jun2021.pdf (accessed on 15 June 2001).
- Hill, A.; Van Der Lugt, J.; Sawyer, W.; Boffito, M. How much ritonavir is needed to boost protease inhibitors? Systematic review of 17 dose-ranging pharmacokinetic trials. AIDS 2009, 23, 2237–2245. [Google Scholar] [CrossRef]
- Alcamo, A.M.; Wolf, M.S.; Alessi, L.J.; Chong, H.J.; Green, M.; Williams, J.V.; Simon, D.W. Successful Use of Cidofovir in an Immunocompetent Child With Severe Adenoviral Sepsis. Pediatrics 2020, 145, e20191632. [Google Scholar] [CrossRef] [PubMed]
- Khan, M.; Maryam, A.; Mehmood, T.; Zhang, Y.; Ma, T. Enhancing Activity of Anticancer Drugs in Multidrug Resistant Tumors by Modulating P-Glycoprotein through Dietary Nutraceuticals. Asian Pac. J. Cancer Prev. 2015, 16, 6831–6839. [Google Scholar] [CrossRef] [Green Version]
- Meghwal, M.; Goswami, T.K. Piper nigrum and Piperine: An Update. Phytother. Res. 2013, 27, 1121–1130. [Google Scholar] [CrossRef] [PubMed]
- Jiang, W.; Wang, X.; Xu, X.; Kong, L. Effect of Schisandra sphenanthera extract on the concentration of tacrolimus in the blood of liver transplant patients. Int. J. Clin. Pharmacol. Ther. 2010, 48, 224–229. [Google Scholar] [CrossRef] [PubMed]
- Souirti, Z.; Loukili, M.; Soudy, I.D.; Rtibi, K.; Özel, A.; Limas-Nzouzi, N.; El Ouezzani, S.; Eto, B. Hibiscus sabdariffaincreases hydroxocobalamin oral bioavailability and clinical efficacy in vitamin B12deficiency with neurological symptoms. Fundam. Clin. Pharmacol. 2016, 30, 568–576. [Google Scholar] [CrossRef]
- Berretta, M.; della Pepa, C.; Tralongo, P.; Fulvi, A.; Martellotta, F.; Lleshi, A.; Nasti, G.; Fisichella, R.; Romano, C.; De Divitiis, C.; et al. Use of Complementary and Alternative Medicine (CAM) in cancer patients: An Italian multicenter survey. Oncotarget 2017, 8, 24401–24414. [Google Scholar] [CrossRef] [Green Version]
- Knecht, K.; Kinder, D.; Stockert, A. Biologically-Based Complementary and Alternative Medicine (CAM) Use in Cancer Patients: The Good, the Bad, the Misunderstood. Front. Nutr. 2020, 6, 196. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yeung, K.S.; Gubili, J.; Mao, J.J. Herb-Drug Interactions in Cancer Care. Oncology 2018, 32, 516–520. [Google Scholar] [PubMed]
- Beauchamp, T.L.; Childress, J.F. Principles of Biomedical Ethics, 7th ed.; Oxford University Press: New York, NY, USA, 2019. [Google Scholar]
- Melchardt, T.; Magnes, T.; Weiss, L.; Grundbichler, M.; Strasser, M.; Hufnagl, C.; Moik, M.; Greil, R.; Egle, A. Liver toxicity during temozolomide chemotherapy caused by Chinese herbs. BMC Complement. Altern. Med. 2014, 14, 115. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Spinella, M.; Eaton, L.A. Hypomania induced by herbal and pharmaceutical psychotropic medicines following mild traumatic brain injury. Brain Inj. 2002, 16, 359–367. [Google Scholar] [CrossRef] [PubMed]
- Lee, N.; Fermo, J. Warfarin and royal jelly interaction. Pharmacotherapy 2006, 26, 583–586. [Google Scholar] [CrossRef]
- Khalid, Z.; Osuagwu, F.C.; Shah, B.; Roy, N.; Dillon, J.E.; Bradley, R. Celery root extract as an inducer of mania induction in a patient on venlafaxine and St John’s Wort. Postgrad. Med. 2016, 128, 682–683. [Google Scholar] [CrossRef] [PubMed]
- Al Faraj, S. Antagonism of the anticoagulant effect of warfarin caused by the use of Commiphora molmol as a herbal medication: A case report. Ann. Trop. Med. Parasitol. 2005, 99, 219–220. [Google Scholar] [CrossRef]
- Ernst, E.; Pittler, M. Herbal medicine. Med. Clin. North Am. 2002, 86, 149–161. [Google Scholar] [CrossRef]
- Bruno, J.J.; Ellis, J. Herbal Use among US Elderly: 2002 National Health Interview Survey. Ann. Pharmacother. 2005, 39, 643–648. [Google Scholar] [CrossRef] [PubMed]
- Kelly, J.P.; Kaufman, D.W.; Kelley, K.; Rosenberg, L.; Anderson, T.E.; Mitchell, A.A. Recent Trends in Use of Herbal and Other Natural Products. Arch. Intern. Med. 2005, 165, 281–286. [Google Scholar] [CrossRef] [Green Version]
- McHugh, M.L. Interrater reliability: The kappa statistic. Biochem. Med. 2012, 22, 276–282. [Google Scholar] [CrossRef]
- Ventola, C.L. Big data and pharmacovigilance: Data mining for adverse drug events and interactions. Pharm. Ther. 2018, 43, 340–351. [Google Scholar]
- National Center for Biotechnology Information (NCBI). National Library of Medicine (US), National Center for Biotechnology Information, Bethesda, MD, US. Available online: https://0-www-ncbi-nlm-nih-gov.brum.beds.ac.uk/ (accessed on 18 May 2021).
- Elsevier. Embase®. Available online: https://0-www-elsevier-com.brum.beds.ac.uk/solutions/embase-biomedical-research (accessed on 18 May 2021).
- IBM Micromedex. Truven Health Analytics/IBM Watson Health. 2020. Available online: https://www.micromedexsolutions.com (accessed on 18 May 2021).
- Tatro, D. (Ed.) Drug Interaction Facts: The Authority on Drug Interactions; Wolters Kluwer Health: Philadelphia, PA, USA, 2015. [Google Scholar]
- Walsh, K.M. Getting to Yes. J. Am. Geriatr. Soc. 2005, 53, 1072. [Google Scholar] [CrossRef]
- Mazaleuskaya, L.L.; Theken, K.; Gong, L.; Thorn, C.F.; Fitzgerald, G.A.; Altman, R.; Klein, T.E. PharmGKB summary: Ibuprofen pathways. Pharm. Genom. 2015, 25, 96–106. [Google Scholar] [CrossRef] [Green Version]
- Gurley, B.J.; Gardner, S.F.; Hubbard, M.A.; Williams, D.K.; Gentry, W.B.; Khan, I.A.; Shah, A. In Vivo Effects of Goldenseal, Kava Kava, Black Cohosh, and Valerian on Human Cytochrome P450 1A2, 2D6, 2E1, and 3A4 Phenotypes. Clin. Pharmacol. Ther. 2005, 77, 415–426. [Google Scholar] [CrossRef] [PubMed]
- Gurley, B.J.; Barone, G.W.; Williams, D.K.; Carrier, J.; Breen, P.; Yates, C.R.; Song, P.-F.; Hubbard, M.A.; Tong, Y.; Cheboyina, S. Effect of milk thistle (Silybum marianum) and black cohosh (Cimicifuga racemosa) supplementation on digoxin pharmacokinetics in humans. Drug Metab. Dispos. 2006, 34, 69–74. [Google Scholar] [CrossRef] [Green Version]
- Abdul, M.I.M.; Jiang, X.; Williams, K.M.; Day, R.; Roufogalis, B.; Liauw, W.S.; Xu, H.; McLachlan, A.J. Pharmacodynamic interaction of warfarin with cranberry but not with garlic in healthy subjects. Br. J. Pharmacol. 2008, 154, 1691–1700. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gurley, B.J.; Gardner, S.F.; Hubbard, M.A.; Williams, D.K.; Gentry, W.B.; Cui, Y.; Ang, C.Y. Cytochrome P450 phenotypic ratios for predicting herb-drug interactions in humans. Clin. Pharmacol. Ther. 2002, 72, 276–287. [Google Scholar] [CrossRef] [PubMed]
- Gurley, B.J.; Gardner, S.F.; Hubbard, M.A.; Williams, D.K.; Gentry, W.B.; Cui, Y.; Ang, C.Y. Clinical assessment of botanical supplementation on cytochrome P450 phenotypes in the elderly: St. John’s wort, garlic oil, Panax ginseng, and Ginkgo biloba. Drugs Aging 2005, 22, 525–539. [Google Scholar] [CrossRef]
- Zhou, Q.; Ye, Z.; Ruan, Z.; Zeng, S. Investigation on modulation of human P-gp by multiple doses of Radix Astragali extract granules using fexofenadine as a phenotyping probe. J. Ethnopharmacol. 2013, 146, 744–749. [Google Scholar] [CrossRef]
- Fan, L.; Zhang, W.; Guo, D.; Tan, Z.-R.; Xu, P.; Li, Q.; Liu, Y.-Z.; Zhang, L.; He, T.-Y.; Hu, D.-L.; et al. The Effect of Herbal Medicine Baicalin on Pharmacokinetics of Rosuvastatin, Substrate of Organic Anion-transporting Polypeptide 1B1. Clin. Pharmacol. Ther. 2008, 83, 471–476. [Google Scholar] [CrossRef]
- Hu, M.; Mak, V.W.L.; Yin, O.Q.P.; Chu, T.T.W.; Tomlinson, B. Effects of Grapefruit Juice and SLCO1B1 388A>G Polymorphism on the Pharmacokinetics of Pitavastatin. Drug Metab. Pharmacokinet. 2013, 28, 104–108. [Google Scholar] [CrossRef] [Green Version]
- Nicandro, J.P.; Tsourounis, C.; Frassetto, L.; Guglielmo, B.J. In vivo effect of I’m-Yunity on hepatic cytochrome P450 3A4. J. Herb. Pharmacother. 2007, 7, 39–56. [Google Scholar] [CrossRef]
- Tankanow, R.; Tamer, H.R.; Streetman, D.S.; Smith, S.G.; Welton, J.L.; Annesley, T.; Aaronson, K.D.; Bleske, B.E. Interaction Study between Digoxin and a Preparation of Hawthorn (Crataegus oxyacantha). J. Clin. Pharmacol. 2003, 43, 637–642. [Google Scholar] [CrossRef] [Green Version]
- Walker, A.F.; Marakis, G.; Simpson, E.; Hope, J.L.; Robinson, P.A.; Hassanein, M.; Simpson, H.C. Hypotensive effects of hawthorn for patients with diabetes taking prescription drugs: A randomized controlled trial. Br. J. Gen. Pract. 2006, 56, 437–443. [Google Scholar]
- Ikehata, M.; Ohnishi, N.; Egami, S.; Kishi, H.; Shin, Y.; Takara, K.; Tsuchishita, Y.; Tokuda, N.; Hori, S.; Yatani, Y.; et al. Effects of Turmeric Extract on the Pharmacokinetics of Nifedipine After a Single Oral Administration in Healthy Volunteers. J. Diet. Suppl. 2008, 5, 401–410. [Google Scholar] [CrossRef]
- Kim, T.-E.; Ha, N.; Kim, Y.; Kim, H.; Lee, J.W.; Jeon, J.-Y.; Kim, M.-G. Effect of epigallocatechin-3-gallate, major ingredient of green tea, on the pharmacokinetics of rosuvastatin in healthy volunteers. Drug Des. Dev. Ther. 2017, 11, 1409–1416. [Google Scholar] [CrossRef] [Green Version]
- Moltó, J.; Valle, M.; Miranda, C.; Cedeño, S.; Negredo, E.; Clotet, B. Herb-Drug Interaction between Echinacea purpurea and Etravirine in HIV-Infected Patients. Antimicrob. Agents Chemother. 2012, 56, 5328–5331. [Google Scholar] [CrossRef] [Green Version]
- Salman, S.A.B.; Amrah, S.; Wahab, M.S.A.; Ismail, Z.; Ismail, R.; Yuen, K.H.; Gan, S.H.; Msc, S.A.B.S.; Mpharm, R.I. Modification of propranolol’s bioavailability by Eurycoma longifolia water-based extract. J. Clin. Pharm. Ther. 2010, 35, 691–696. [Google Scholar] [CrossRef]
- Xiao, C.-Q.; Chen, R.; Lin, J.; Wang, G.; Chen, Y.; Tan, Z.-R.; Zhou, H.-H. Effect of genistein on the activities of cytochrome P450 3A and P-glycoprotein in Chinese healthy participants. Xenobiotica 2011, 42, 173–178. [Google Scholar] [CrossRef]
- Aruna, D.; Naidu, M.U.R. Pharmacodynamic interaction studies of Ginkgo biloba with cilostazol and clopidogrel in healthy human subjects. Br. J. Clin. Pharmacol. 2007, 63, 333–338. [Google Scholar] [CrossRef] [Green Version]
- Dai, L.-L.; Fan, L.; Wu, H.-Z.; Tan, Z.-R.; Chen, Y.; Peng, X.-D.; Shen, M.-X.; Yang, G.-P.; Zhou, H.-H. Assessment of a pharmacokinetic and pharmacodynamic interaction between simvastatin and Ginkgo biloba extracts in healthy subjects. Xenobiotica 2013, 43, 862–867. [Google Scholar] [CrossRef]
- Fan, L.; Tao, G.-Y.; Wang, G.; Chen, Y.; Zhang, W.; He, Y.-J.; Li, Q.; Lei, H.-P.; Jiang, F.; Hu, D.-L.; et al. Effects of Ginkgo biloba Extract Ingestion on the Pharmacokinetics of Talinolol in Healthy Chinese Volunteers. Ann. Pharmacother. 2009, 43, 944–949. [Google Scholar] [CrossRef]
- Guo, C.-X.; Pei, Q.; Yin, J.-Y.; Peng, X.; Zhou, B.-T.; Zhao, Y.-C.; Wu, L.-X.; Meng, X.-G.; Wang, G.; Li, Q.; et al. Effects of Ginkgo biloba extracts on pharmacokinetics and efficacy of atorvastatin based on plasma indices. Xenobiotica 2012, 42, 784–790. [Google Scholar] [CrossRef] [PubMed]
- Jiang, X.; Blair, E.Y.L.; McLachlan, A.J. Investigation of the Effects of Herbal Medicines on Warfarin Response in Healthy Subjects: A Population Pharmacokinetic-Pharmacodynamic Modeling Approach. J. Clin. Pharmacol. 2006, 46, 1370–1378. [Google Scholar] [CrossRef]
- Kim, B.-H.; Kim, K.-P.; Lim, K.S.; Kim, J.-R.; Yoon, S.H.; Cho, J.-Y.; Lee, Y.-O.; Lee, K.-H.; Jang, I.-J.; Shin, S.-G.; et al. Influence of Ginkgo biloba extract on the pharmacodynamic effects and pharmacokinetic properties of ticlopidine: An open-label, randomized, two-period, two-treatment, two-sequence, single-dose crossover study in healthy Korean male volunteers. Clin. Ther. 2010, 32, 380–390. [Google Scholar] [CrossRef]
- Mohutsky, M.A.; Anderson, G.D.; Miller, J.W.; Elmer, G.W. Ginkgo biloba: Evaluation of CYP2C9 Drug Interactions In Vitro and In Vivo. Am. J. Ther. 2006, 13, 24–31. [Google Scholar] [CrossRef]
- Zadoyan, G.; Rokitta, D.; Klement, S.; Dienel, A.; Hoerr, R.; Gramatté, T.; Fuhr, U. Effect of Ginkgo biloba special extract EGb 761® on human cytochrome P450 activity: A cocktail interaction study in healthy volunteers. Eur. J. Clin. Pharmacol. 2012, 68, 553–560. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Van Breemen, R.B.; Chen, L.; Tonsing-Carter, A.; Banuvar, S.; Barengolts, E.; Viana, M.; Chen, S.-N.; Pauli, G.F.; Bolton, J.L. Pharmacokinetic Interactions of a Hop Dietary Supplement with Drug Metabolism in Perimenopausal and Postmenopausal Women. J. Agric. Food Chem. 2020, 68, 5212–5220. [Google Scholar] [CrossRef]
- Gurley, B.J.; Swain, A.; Barone, G.W.; Williams, D.K.; Breen, P.; Yates, C.R.; Stuart, L.B.; Hubbard, M.A.; Tong, Y.; Cheboyina, S.; et al. Effect of Goldenseal (Hydrastis canadensis) and Kava Kava (Piper methysticum) Supplementation on Digoxin Pharmacokinetics in Humans. Drug Metab. Dispos. 2006, 35, 240–245. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gurley, B.J.; Swain, A.; Hubbard, M.A.; Hartsfield, F.; Thaden, J.; Williams, D.K.; Gentry, W.B.; Tong, Y. Supplementation With Goldenseal (Hydrastis canadensis), but not Kava Kava (Piper methysticum), Inhibits Human CYP3A Activity In Vivo. Clin. Pharmacol. Ther. 2008, 83, 61–69. [Google Scholar] [CrossRef] [PubMed]
- Andrén, L.; Andreasson, A.; Eggertsen, R. Interaction between a commercially available St. John’s wort product (Movina) and atorvastatin in patients with hypercholesterolemia. Eur. J. Clin. Pharmacol. 2007, 63, 913–916. [Google Scholar] [CrossRef]
- Bell, E.C.; Ravis, W.R.; Chan, H.M.; Lin, Y.-J. Lack of Pharmacokinetic Interaction Between St. John’s Wort and Prednisone. Ann. Pharmacother. 2007, 41, 1819–1824. [Google Scholar] [CrossRef]
- Bell, E.C.; Ravis, W.R.; Lloyd, K.B.; Stokes, T.J. Effects of St. John’s Wort Supplementation on Ibuprofen Pharmacokinetics. Ann. Pharmacother. 2007, 41, 229–234. [Google Scholar] [CrossRef] [PubMed]
- Nieminen, T.H.; Hagelberg, N.M.; Saari, T.I.; Neuvonen, M.; Laine, K.; Neuvonen, P.; Olkkola, K.T. St John’s wort greatly reduces the concentrations of oral oxycodone. Eur. J. Pain 2010, 14, 854–859. [Google Scholar] [CrossRef]
- Fan, L.; Zhou, G.; Guo, D.; Liu, Y.-L.; Chen, W.-Q.; Liu, Z.; Tan, Z.-R.; Sheng, D.; Zhou, H.-H.; Zhang, W. The Pregnane X Receptor Agonist St Johnʼs Wort Has No Effects on the Pharmacokinetics and Pharmacodynamics of Repaglinide. Clin. Pharmacokinet. 2011, 50, 605–611. [Google Scholar] [CrossRef]
- Goey, A.K.L.; Meijerman, I.; Rosing, H.; Marchetti, S.; Mergui-Roelvink, M.; Keessen, M.; Burgers, J.A.; Beijnen, J.H.; Schellens, J.H.M. The Effect of St John’s Wort on the Pharmacokinetics of Docetaxel. Clin. Pharmacokinet. 2013, 53, 103–110. [Google Scholar] [CrossRef]
- Hennessy, M.; Kelleher, D.; Spiers, P.; Barry, M.; Kavanagh, P.; Back, D.; Mulcahy, F.; Feely, J. St John’s Wort increases expression of P-glycoprotein: Implications for drug interactions. Br. J. Clin. Pharmacol. 2002, 53, 75–82. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jiang, X.; Williams, K.M.; Liauw, W.S.; Ammit, A.; Roufogalis, B.; Duke, C.C.; Day, R.; McLachlan, A.J. Effect of St John’s wort and ginseng on the pharmacokinetics and pharmacodynamics of warfarin in healthy subjects. Br. J. Clin. Pharmacol. 2004, 57, 592–599. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Loughren, M.J.; Kharasch, E.D.; Kelton-Rehkopf, M.C.; Syrjala, K.L.; Shen, D.D. Influence of St. John’s Wort on Intravenous Fentanyl Pharmacokinetics, Pharmacodynamics, and Clinical Effects. Anesthesiology 2020, 132, 491–503. [Google Scholar] [CrossRef]
- Markert, C.; Kastner, I.M.; Hellwig, R.; Kalafut, P.; Schweizer, Y.; Hoffmann, M.M.; Burhenne, J.; Weiss, J.; Mikus, G.; Haefeli, W.E. The Effect of Induction of CYP3A4 by St John’s Wort on Ambrisentan Plasma Pharmacokinetics in Volunteers of knownCYP2C19Genotype. Basic Clin. Pharmacol. Toxicol. 2014, 116, 423–428. [Google Scholar] [CrossRef] [PubMed]
- Mueller, S.C.; Majcher-Peszynska, J.; Uehleke, B.; Klammt, S.; Mundkowski, R.G.; Miekisch, W.; Sievers, H.; Bauer, S.; Frank, B.; Kundt, G.; et al. The extent of induction of CYP3A by St. John’s wort varies among products and is linked to hyperforin dose. Eur. J. Clin. Pharmacol. 2006, 62, 29–36. [Google Scholar] [CrossRef] [PubMed]
- Mueller, S.C.; Majcher-Peszynska, J.; Mundkowski, R.G.; Uehleke, B.; Klammt, S.; Sievers, H.; Lehnfeld, R.; Frank, B.; Thurow, K.; Kundt, G.; et al. No clinically relevant CYP3A induction after St. John’s wort with low hyperforin content in healthy volunteers. Eur. J. Clin. Pharmacol. 2008, 65, 81–87. [Google Scholar] [CrossRef] [Green Version]
- Murphy, P.A.; Kern, S.E.; Stanczyk, F.Z.; Westhoff, C.L. Interaction of St. John’s Wort with oral contraceptives: Effects on the pharmacokinetics of norethindrone and ethinyl estradiol, ovarian activity and breakthrough bleeding. Contracept. 2005, 71, 402–408. [Google Scholar] [CrossRef] [PubMed]
- Piscitelli, S.C.; Burstein, A.H.; Chaitt, D.; Alfaro, R.M.; Falloon, J. Indinavir concentrations and St John’s wort. Lancet 2000, 355, 547–548. [Google Scholar] [CrossRef]
- Portolés, A.; Terleira, A.; Calvo, A.; Martínez, M.I.; Resplandy, G. Effects of Hypericum perforatum on Ivabradine Pharmacokinetics in Healthy Volunteers: An Open-Label, Pharmacokinetic Interaction Clinical Trial. J. Clin. Pharmacol. 2006, 46, 1188–1194. [Google Scholar] [CrossRef]
- Xie, R.; Tan, L.H.; Polasek, E.C.; Hong, C.; Teillol-Foo, M.; Gordi, T.; Sharma, A.; Ms, D.J.N.; Arakawa, T.; Knuth, D.W.; et al. CYP3A and P-Glycoprotein Activity Induction With St. John’s Wort in Healthy Volunteers From 6 Ethnic Populations. J. Clin. Pharmacol. 2005, 45, 352–356. [Google Scholar] [CrossRef]
- Xu, H.; Williams, K.M.; Liauw, W.S.; Murray, M.; Day, R.; McLachlan, A.J. Effects of St John’s wort and CYP2C9 genotype on the pharmacokinetics and pharmacodynamics of gliclazide. Br. J. Pharmacol. 2008, 153, 1579–1586. [Google Scholar] [CrossRef] [Green Version]
- Heger-Mahn, D.; Pabst, G.; Dienel, A.; Schlafke, S.; Klipping, C. No interacting influence of lavender oil preparation silexan on oral contraception using an ethinyl estradiol/levonorgestrel combination. Drugs R&D 2014, 14, 265–272. [Google Scholar] [CrossRef] [Green Version]
- Chen, Y.; Ouyang, D.-S.; Kang, Z.; Yang, G.-P.; Tan, Z.-R.; Zhou, G.; Yan, J. Effect of a traditional Chinese medicine Liu Wei Di Huang Wan on the activities of CYP2C19, CYP2D6 and CYP3A4 in healthy volunteers. Xenobiotica 2011, 42, 596–602. [Google Scholar] [CrossRef]
- Fan, L.; Wang, G.; Wang, L.-S.; Chen, Y.; Zhang, W.; Huang, Y.-F.; Huang, R.-X.; Hu, D.-L.; Wang, D.; Zhou, H.-H. Herbal medicine Yin Zhi Huang induces CYP3A4-mediated sulfoxidation and CYP2C19-dependent hydroxylation of omeprazole. Acta Pharmacol. Sin. 2007, 28, 1685–1692. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kim, H.; Bae, S.K.; Park, S.-J.; Shim, E.-J.; Kim, H.-S.; Shon, J.-H.; Liu, K.-H.; Shin, J.-G. Effects of woohwangcheongsimwon suspension on the pharmacokinetics of bupropion and its active metabolite, 4-hydroxybupropion, in healthy subjects. Br. J. Clin. Pharmacol. 2010, 70, 126–131. [Google Scholar] [CrossRef] [PubMed]
- Nakao, M.; Muramoto, Y.; Hisadome, M.; Yamano, N.; Shoji, M.; Fukushima, Y.; Saruwatari, J.; Nakagawa, K. The effect of Shoseiryuto, a traditional Japanese medicine, on cytochrome P450s, N-acetyltransferase 2 and xanthine oxidase, in extensive or intermediate metabolizers of CYP2D6. Eur. J. Clin. Pharmacol. 2007, 63, 345–353. [Google Scholar] [CrossRef] [PubMed]
- Park, S.-I.; Park, J.-Y.; Park, M.-J.; Yim, S.-V.; Kim, B.-H. Effects of Ojeok-san on the Pharmacokinetics of Celecoxib at Steady-state in Healthy Volunteers. Basic Clin. Pharmacol. Toxicol. 2018, 123, 51–57. [Google Scholar] [CrossRef] [Green Version]
- Saruwatari, J.; Takaishi, C.; Yoshida, K.; Takashima, A.; Fujimura, Y.; Umemoto, Y.; Abe, T.; Kitamado, M.; Shimomasuda, M.; Muramoto, Y.; et al. A herbal-drug interaction study of keishi-bukuryo-gan, a traditional herbal preparation used for menopausal symptoms, in healthy female volunteers. J. Pharm. Pharmacol. 2012, 64, 670–676. [Google Scholar] [CrossRef]
- Wang, P.; Sun, H.; Yang, L.; Li, L.-Y.; Hao, J.; Ruff, D.; Guo, Z.-X. Absence of an effect of T89 on the steady-state pharmacokinetics and pharmacodynamics of warfarin in healthy volunteers. J. Clin. Pharmacol. 2014, 54, 234–239. [Google Scholar] [CrossRef]
- Lee, Y.H.; Lee, B.K.; Choi, Y.J.; Yoon, I.K.; Chang, B.C.; Gwak, H.S. Interaction between warfarin and Korean red ginseng in patients with cardiac valve replacement. Int. J. Cardiol. 2010, 145, 275–276. [Google Scholar] [CrossRef]
- Malati, C.Y.; Robertson, S.M.; Hunt, J.D.; Chairez, C.; Alfaro, R.M.; Kovacs, J.A.; Penzak, S.R. Influence of Panax ginseng on Cytochrome P450 (CYP)3A and P-glycoprotein (P-gp) Activity in Healthy Participants. J. Clin. Pharmacol. 2012, 52, 932–939. [Google Scholar] [CrossRef] [Green Version]
- Fatima, N.; Pingali, U.; Muralidhar, N. Study of pharmacodynamic interaction of Phyllanthus emblica extract with clopidogrel and ecosprin in patients with type II diabetes mellitus. Phytomedicine 2014, 21, 579–585. [Google Scholar] [CrossRef]
- Bedada, S.K.; Neerati, P. Resveratrol Pretreatment Affects CYP2E1 Activity of Chlorzoxazone in Healthy Human Volunteers. Phytotherapy Res. 2016, 30, 463–468. [Google Scholar] [CrossRef]
- Fuhr, U.; Beckmann-Knopp, S.; Jetter, A.; Lück, H.; Mengs, U. The Effect of Silymarin on Oral Nifedipine Pharmacokinetics. Planta Medica 2007, 73, 1429–1435. [Google Scholar] [CrossRef] [PubMed]
- Kawaguchi-Suzuki, M.; Frye, R.F.; Zhu, H.-J.; Brinda, B.J.; Chavin, K.D.; Bernstein, H.J.; Markowitz, J.S. The Effects of Milk Thistle (Silybum marianum) on Human Cytochrome P450 Activity. Drug Metab. Dispos. 2014, 42, 1611–1616. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tocaciu, S.; Oliver, L.J.; Lowenthal, R.M.; Peterson, G.M.; Patel, R.; Shastri, M.; McGuinness, G.; Olesen, I.; Fitton, J.H. The Effect of Undaria pinnatifida Fucoidan on the Pharmacokinetics of Letrozole and Tamoxifen in Patients With Breast Cancer. Integr. Cancer Ther. 2018, 17, 99–105. [Google Scholar] [CrossRef] [Green Version]
- Thronicke, A.; Steele, M.L.; Grah, C.; Matthes, B.; Schad, F. Clinical safety of combined therapy of immune checkpoint inhibitors and Viscum album L. therapy in patients with advanced or metastatic cancer. BMC Complement. Altern. Med. 2017, 17, 534. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Açikgöz, S.K.; Açıkgöz, E. Gastrointestinal bleeding secondary to interaction of Artemisia absinthium with warfarin. Drug Metab. Drug Interact. 2013, 28, 187–189. [Google Scholar] [CrossRef] [PubMed]
- Almeida, J.; Grimsley, E. Coma from the Health Food Store: Interaction between Kava and Alprazolam. Ann. Intern. Med. 1996, 125, 940–941. [Google Scholar] [CrossRef]
- Alscher, D.M.; Klotz, U. Drug interaction of herbal tea containing St. John’s wort with cyclosporine. Transpl. Int. 2003, 16, 543–544. [Google Scholar] [CrossRef]
- Aslam, M.; Stockley, I. Interaction between curry ingredient (karela) and drug (chlorpropamide). Lancet 1979, 313, 607. [Google Scholar] [CrossRef]
- Barbenel, D.M.; Yusufi, B.; Bench, C.J.; O’Shea, D. Mania in a patient receiving testosterone replacement post-orchidectomy taking St John’s wort and sertraline. J. Psychopharmacol. 2000, 14, 84–86. [Google Scholar] [CrossRef]
- Barone, G.W.; Gurley, B.J.; Ketel, B.L.; Lightfoot, M.L.; Abul-Ezz, S.R. Drug Interaction between St. John’s Wort and Cyclosporine. Ann. Pharmacother. 2000, 34, 1013–1016. [Google Scholar] [CrossRef]
- Bilgi, N.; Bell, K.; Ananthakrishnan, A.N.; Atallah, E. Imatinib and Panax ginseng: A Potential Interaction Resulting in Liver Toxicity. Ann. Pharmacother. 2010, 44, 926–928. [Google Scholar] [CrossRef]
- Bolley, R.; Zülke, C.; Kammerl, M.; Fischereder, M.; Krämer, B.K. Tacrolimus-induced nephrotoxicity unmasked by induction of the CYP3A4 system with ST JOHN’S wort. Transplantation 2002, 73, 1009. [Google Scholar] [CrossRef] [PubMed]
- Bossaer, J.B.; Odle, B.L. Probable Etoposide Interaction with Echinacea. J. Diet. Suppl. 2012, 9, 90–95. [Google Scholar] [CrossRef] [PubMed]
- Breidenbach, T.; Hoffmann, M.W.; Becke, T.; Schlitt, H.; Klempnauer, J. Drug interaction of St John’s wort with ciclosporin. Lancet 2000, 355, 1912. [Google Scholar] [CrossRef]
- Buckley, M.S.; Goff, A.D.; Knapp, W.E. Fish Oil Interaction with Warfarin. Ann. Pharmacother. 2004, 38, 50–53. [Google Scholar] [CrossRef] [PubMed]
- Bamgbade, O. The perioperative implications of khat use. Eur. J. Anaesthesiol. 2008, 25, 170–172. [Google Scholar] [CrossRef] [PubMed]
- Campos, M.; Machado, J.; Costa, M.; Lino, S.; Correia, F.; Maltez, F. Case Report: Severe Hematological, Muscle and Liver Toxicity Caused by Drugs and Artichoke Infusion Interaction in an Elderly Polymedicated Patient. Curr. Drug Saf. 2018, 13, 44–50. [Google Scholar] [CrossRef] [PubMed]
- Cappuzzo, K.A. Herbal Product Use in a Patient with Polypharmacy. Consult. Pharm. 2006, 21, 911–915. [Google Scholar] [CrossRef]
- Carbajal, R.; Yisfalem, A.; Pradhan, N.; Baumstein, D.; Chaudhari, A. Case Report: Boldo (Peumus boldus) and Tacrolimus Interaction in a Renal Transplant Patient. Transplant. Proc. 2014, 46, 2400–2402. [Google Scholar] [CrossRef] [PubMed]
- Carr, M.; Klotz, J.; Bergeron, M. Coumadin resistance and the vitamin supplement “noni”. Am. J. Hematol. 2004, 77, 103. [Google Scholar] [CrossRef]
- Carrasco, M.C.; Vallejo, J.R.; Pardo-de-Santayana, M.; Peral, D.; Martín, M.Á.; Altimiras, J. Interactions of Valeriana officinalis L. and Passiflora incarnata L. in a patient treated with lorazepam. Phytother. Res. 2009, 23, 1795–1796. [Google Scholar] [CrossRef] [PubMed]
- Carter, J.; Yeh, R.F.; Braunschweig, I.; Barta, S. Unreported use of an herbal supplement resulting in decreased clearance of intravenous busulfan in a patient undergoing auto-SCT. Bone Marrow Transplant. 2014, 49, 313–314. [Google Scholar] [CrossRef]
- Cattaneo, D.; Fusi, M.; Gervasoni, C. No effects of Hypericum-containing complex on dolutegravir plasma trough concentrations: A case report. Eur. J. Clin. Pharmacol. 2019, 75, 1467–1468. [Google Scholar] [CrossRef] [PubMed]
- Chan, J.C.M.; Ng, M.-H.; Wong, R.S.M.; Tomlinson, B. A case of simvastatin-induced myopathy with SLCO1B1 genetic predisposition and co-ingestion of linagliptin and Stevia rebaudiana. J. Clin. Pharm. Ther. 2019, 44, 381–383. [Google Scholar] [CrossRef]
- Chang, Y.-Y.; Liu, J.-S.; Lai, S.-L.; Wu, H.-S.; Lan, M.-Y. Cerebellar Hemorrhage Provoked by Combined Use of Nattokinase and Aspirin in a Patient with Cerebral Microbleeds. Intern. Med. 2008, 47, 467–469. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Constable, S.; Ham, A.; Pirmohamed, M. Herbal medicines and acute medical emergency admissions to hospital. Br. J. Clin. Pharmacol. 2007, 63, 247–248. [Google Scholar] [CrossRef] [Green Version]
- Cordova, E.; Morganti, L.; Rodriguez, C. Possible Drug–Herb Interaction between Herbal Supplement Containing Horsetail (Equisetum arvense) and Antiretroviral Drugs. J. Int. Assoc. Provid. AIDS Care (JIAPAC) 2017, 16, 11–13. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Damato, A.; Larocca, M.; Rondini, E.; Menga, M.; Pinto, C.; Versari, A. Severe Rhabdomyolysis during Treatment with Trabectedin in Combination with a Herbal Drug in a Patient with Metastatic Synovial Sarcoma: A Case Report. Case Rep. Oncol. 2017, 10, 258–264. [Google Scholar] [CrossRef] [Green Version]
- Dannawi, M. Possible serotonin syndrome after combination of buspirone and St John’s Wort. J. Psychopharmacol. 2002, 16, 401. [Google Scholar] [CrossRef] [PubMed]
- Daveluy, A.; Géniaux, H.; Thibaud, L.; Mallaret, M.; Miremont-Salamé, G.; Haramburu, F. Probable Interaction Between an Oral Vitamin K Antagonist and Turmeric (Curcuma longa). Therapie 2014, 69, 519–520. [Google Scholar] [CrossRef] [PubMed]
- Epstein, R.J.; Leung, T.W.T.; Cheung, P.S.Y. Panmucositis and chemosensitisation associated with betel quid chewing during dose-dense adjuvant breast cancer chemotherapy. Cancer Chemother. Pharmacol. 2006, 58, 835–837. [Google Scholar] [CrossRef]
- Galera, R.M.L.; Pascuet, E.R.; Mur, J.I.E.; Montoro-Ronsano, J.B.; Juarez-Gimenez, J.C. Interaction between cat’s claw and protease inhibitors atazanavir, ritonavir and saquinavir. Eur. J. Clin. Pharmacol. 2008, 64, 1235–1236. [Google Scholar] [CrossRef] [PubMed]
- Galluzzi, S.; Zanetti, O.; Binetti, G.; Trabucchi, M.; Frisoni, G.B. Coma in a patient with Alzheimer’s disease taking low dose trazodone and Ginkgo biloba. J. Neurol. Neurosurg. Psychiatry 2000, 68, 679–680. [Google Scholar] [CrossRef] [Green Version]
- Hamann, G.L.; Campbell, J.D.; George, C.M. Warfarin-Cranberry Juice Interaction. Ann. Pharmacother. 2011, 45, 420. [Google Scholar] [CrossRef]
- Gordon, R.Y.; Becker, D.J.; Rader, D.J. Reduced Efficacy of Rosuvastatin by St. John’s Wort. Am. J. Med. 2009, 122, e1–e2. [Google Scholar] [CrossRef]
- Griffiths, A.; Beddall, A.; Pegler, S. Fatal haemopericardium and gastrointestinal haemorrhage due to possible interaction of cranberry juice with warfarin. J. R. Soc. Promot. Health 2008, 128, 324–326. [Google Scholar] [CrossRef] [PubMed]
- Hanselin, M. INR elevation with maitake extract in combination with warfarin. Ann. Pharmacother. 2010, 44, 223–224. [Google Scholar] [CrossRef]
- Hou, Q.; Han, W.; Fu, X. Pharmacokinetic interaction between tacrolimus and berberine in a child with idiopathic nephrotic syndrome. Eur. J. Clin. Pharmacol. 2013, 69, 1861–1862. [Google Scholar] [CrossRef] [PubMed]
- Hughes, R.L. Fatal combination of mitragynine and quetiapine—A case report with discussion of a potential herb-drug interaction. Forensic Sci. Med. Pathol. 2018, 15, 110–113. [Google Scholar] [CrossRef]
- Hurren, K.M.; Lewis, C.L. Probable interaction between warfarin and bee pollen. Am. J. Health Pharm. 2010, 67, 2034–2037. [Google Scholar] [CrossRef]
- Hwang, S.-W.; Han, H.-S.; Lim, K.Y.; Han, J.-Y. Drug Interaction Between Complementary Herbal Medicines and Gefitinib. J. Thorac. Oncol. 2008, 3, 942–943. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Iida, R.; Otsuka, Y.; Matsumoto, K.; Kuriyama, S.; Hosoya, T. Pseudoaldosteronism due to the concurrent use of two herbal medicines containing glycyrrhizin: Interaction of glycyrrhizin with angiotensin-converting enzyme inhibitor. Clin. Exp. Nephrol. 2006, 10, 131–135. [Google Scholar] [CrossRef] [PubMed]
- Janetzky, K.; Morreale, A.P. Drug Experience Warfarin, and ginseng. Am. J. Healh Pharm. 1997, 54, 692–693. [Google Scholar] [CrossRef] [PubMed]
- Ji, H.; Zhang, G.; Yue, F.; Zhou, X. Adverse event due to a likely interaction between sodium aescinate and Ginkgo biloba extract: A case report. J. Clin. Pharm. Ther. 2017, 42, 237–238. [Google Scholar] [CrossRef]
- Jones, B.D.; Runikis, A.M. Interaction of Ginseng with Phenelzine. J. Clin. Psychopharmacol. 1987, 7, 201–202. [Google Scholar] [CrossRef] [PubMed]
- Kang, Y.-C.; Chen, M.-H.; Lai, S.-L. Potentially Unsafe Herb-drug Interactions Between a Commercial Product of Noni Juice and Phenytoin- A Case Report. Acta Neurol. Taiwanica 2015, 24, 43–46. [Google Scholar]
- Karhova, M.; Trelchel, U.; Malagb, M.; Fnllmg, A.; Gerken, G.; Broelsch, C.E. Interaction of Hypericum perforatum (St. John’s wort) with cycbsporin A metabolism in a patient after liver transplantation. J. Hepatol. 2000, 33, 853. [Google Scholar]
- Cambria-Kiely, J.A. Effect of Soy Milk on Warfarin Efficacy. Ann. Pharmacother. 2002, 36, 1893–1896. [Google Scholar] [CrossRef]
- Krüth, P.; Brosi, E.; Fux, R.; Mörike, K.; Gleiter, C.H. Ginger-Associated Overanticoagulation by Phenprocoumon. Ann. Pharmacother. 2004, 38, 257–260. [Google Scholar] [CrossRef] [PubMed]
- Lam, A.Y.; Elmer, G.W.; Mohutsky, M.A. Possible interaction between warfarin and Lycium barbarum L. Ann. Pharmacother. 2001, 35, 1199–1201. [Google Scholar] [CrossRef]
- Lambert, J.-P.; Cormier, J. Potential Interaction between Warfarin and Boldo-Fenugreek. Pharmacother. J. Hum. Pharmacol. Drug Ther. 2001, 21, 509–512. [Google Scholar] [CrossRef] [PubMed]
- Lantz, M.S.; Buchalter, E.; Giambanco, V. St. John’s wort and antidepressant drug interactions in the elderly. J. Geriatr. Psychiatry Neurol. 1999, 12, 7–10. [Google Scholar] [CrossRef]
- Leung, H.; Hung, A.; Hui, A.; Chan, T. Warfarin overdose due to the possible effects of Lycium barbarum L. Food Chem. Toxicol. 2008, 46, 1860–1862. [Google Scholar] [CrossRef]
- Mai, I.; Krüger, H.; Budde, K.; Johne, A.; Brockmöller, J.; Neumayer, H.-H.; Roots, I. Hazardous pharmacokinetic interaction of Saint John’s wort (Hypericum perforatum) with the immunosuppressant cyclosporin. Int. J. Clin. Pharmacol. Ther. 2000, 38, 500–502. [Google Scholar] [CrossRef] [PubMed]
- Mateo-Carrasco, H.; Gálvez-Contreras, M.C.; Fernández-Ginés, F.D.; Nguyen, T.V. Elevated liver enzymes resulting from an interaction between Raltegravir and Panax ginseng: A case report and brief review. Drug Metab. Drug Interact. 2012, 27, 171–175. [Google Scholar] [CrossRef]
- McGovern, E.; McDonnell, T. Herbal Medicine—Sets the Heart Racing! Ir. Med. J. 2009, 1, 517–538. [Google Scholar]
- McCrae, S. Elevated serum digoxin levels in a patient taking digoxin and Siberian ginseng. CMAJ 1996, 155, 293–295. [Google Scholar]
- Meisel, C. Fatal intracerebral mass bleeding associated with Ginkgo biloba and ibuprofen. Atherosclerosis 2003, 167, 367. [Google Scholar] [CrossRef]
- Mendoza, C.E.; Ferreira, A.C.; De Marchena, E. Warfarin and herbal products interaction causing prosthetic aortic valve thrombosis presenting as acute myocardial infarction. J. Hear. Valve Dis. 2004, 13, 22–24. [Google Scholar]
- Myers, A.P.; Watson, T.A.; Strock, S.B. Drug Reaction with Eosinophilia and Systemic Symptoms Syndrome Probably Induced by a Lamotrigine-Ginseng Drug Interaction. Pharmacother. J. Hum. Pharmacol. Drug Ther. 2015, 35, e9–e12. [Google Scholar] [CrossRef] [PubMed]
- Naccarato, M.; Yoong, D.; Gough, K. A Potential Drug–Herbal Interaction between Ginkgo biloba and Efavirenz. J. Int. Assoc. Physicians AIDS Care 2012, 11, 98–100. [Google Scholar] [CrossRef]
- Nayeri, A.; Wu, S.; Adams, E.; Tanner, C.; Meshman, J.; Saini, I.; Reid, W. Acute Calcineurin Inhibitor Nephrotoxicity Secondary to Turmeric Intake: A Case Report. Transplant. Proc. 2017, 49, 198–200. [Google Scholar] [CrossRef]
- Nebel, A.; Schneider, B.J.; Baker, R.K.; Kroll, D.J. Potential metabolic interaction between St. John’s wort and theophylline. Ann. Pharmacother. 1999, 33, 502. [Google Scholar] [PubMed]
- Nowack, R.; Nowak, B. Herbal teas interfere with cyclosporin levels in renal transplant patients. Nephrol. Dial. Transplant. 2005, 20, 2554–2556. [Google Scholar] [CrossRef] [Green Version]
- Orr, A.; Parker, R. Red clover causing symptoms suggestive of methotrexate toxicity in a patient on high-dose methotrexate. Menopause Int. Integr. J. Postreprod. Health 2013, 19, 133–134. [Google Scholar] [CrossRef] [PubMed]
- Paeng, C.H.; Sprague, M.; Jackevicius, C.A. Interaction between Warfarin and Cranberry Juice. Clin. Ther. 2007, 29, 1730–1735. [Google Scholar] [CrossRef]
- Page, R.L.; Lawrence, J.D. Potentiation of Warfarin by Dong Quai. Pharmacother. J. Hum. Pharmacol. Drug Ther. 1999, 19, 870–876. [Google Scholar] [CrossRef]
- Jacquin-Porretaz, C.; Nardin, C.; Blanc, D.; Aubin, F.; Gérard, B.; Drobacheff-Thiebaut, C.; Jacoulet, P.; Westeel, V. Cutaneous Toxicity Induced by Hibiscus Tea in a Patient Treated with Erlotinib. J. Thorac. Oncol. 2017, 12, e47–e48. [Google Scholar] [CrossRef] [Green Version]
- Prasad, K.; Tharangani, P.; Samaranayake, C. Recurrent relapses of depression in a patient established on sertraline after taking herbal medicinal mixtures—A herb–drug interaction? J. Psychopharmacol. 2008, 23, 216–219. [Google Scholar] [CrossRef]
- Rindone, J.P.; Murphy, T.W. Warfarin-cranberry juice 9nteraction resulting in profound hypoprothrombinemia and bleeding. Am. J. Ther. 2005, 13, 283–284. [Google Scholar] [CrossRef] [PubMed]
- Rivera, C.A.; Ferro, C.L.; Bursua, A.J.; Gerber, B.S. Probable Interaction Between Lycium barbarum (Goji) and Warfarin. Pharmacother. J. Hum. Pharmacol. Drug Ther. 2012, 32, e50–e53. [Google Scholar] [CrossRef] [PubMed]
- Rosado, M.F. Thrombosis of a Prosthetic Aortic Valve Disclosing a Hazardous Interaction between Warfarin and a Commercial Ginseng Product. Cardiol. 2003, 99, 111. [Google Scholar] [CrossRef]
- Rozenfeld, V.; Crain, J.L.; Callahan, A.K. Possible augmentation of warfarin effect by glucosamine-chondroitin. Am. J. Health Pharm. 2004, 61, 306–307. [Google Scholar] [CrossRef]
- Rubin, D.; McGovern, B.; Kopelman, R.I. Back to Basics. Am. J. Med. 2006, 119, 482–483. [Google Scholar] [CrossRef]
- Ruschitzka, F.; Meier, P.J.; Turina, M.; Lüscher, T.F.; Noll, G. Acute heart transplant rejection due to Saint John’s wort. Lancet 2000, 355, 548–549. [Google Scholar] [CrossRef]
- Schwarz, U.I.; Büschel, B.; Kirch, W. Unwanted pregnancy on self-medication with St John’s wort despite hormonal contraception. Br. J. Clin. Pharmacol. 2003, 55, 112–113. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Segal, R. Warfarin interaction with Matricaria chamomilla. Can. Med. Assoc. J. 2006, 174, 1281–1282. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Strippoli, S.; Lorusso, V.; Albano, A.; Guida, M. Herbal-drug interaction induced rhabdomyolysis in a liposarcoma patient receiving trabectedin. BMC Complement. Altern. Med. 2013, 13, 199. [Google Scholar] [CrossRef] [Green Version]
- Suvarna, R.; Pirmohamed, M.; Henderson, L. Possible interaction between warfarin and cranberry juice. BMJ 2003, 327, 1454. [Google Scholar] [CrossRef] [Green Version]
- Tam, L.S.; Chan, T.Y.K.; Leung, W.K.; Critchley, J.A.J.H. Warfarin interactions with Chinese traditional medicines: Danshen and methyl salicylate medicated oil. Aust. N. Z. J. Med. 1995, 25, 258. [Google Scholar] [CrossRef]
- Tamura, S.; Warabi, Y.; Matsubara, S. Severe liver dysfunction possibly caused by the combination of interferon beta-1b therapy and melilot (sweet clover) supplement. J. Clin. Pharm. Ther. 2012, 37, 724–725. [Google Scholar] [CrossRef] [PubMed]
- Taylor, J.; Wilt, V. Probably antagonism of warfarin by green tea. Ann. Pharmacother. 1999, 33, 426–428. [Google Scholar] [CrossRef]
- van den Bout, C.J.; Bosch, M.E.; Burger, D.M.; Koopmans, P.P.; van der Ven, A.J. Toxic lopinavir concentrations in an HIV-1 infected patient taking herbal medications. AIDS 2008, 22, 1243–1244. [Google Scholar] [CrossRef]
- Van Strater, A.C.; Bogers, J.P. Interaction of St John’s wort (Hypericum perforatum) with clozapine. Int. Clin. Psychopharmacol. 2012, 27, 121–124. [Google Scholar] [CrossRef]
- Welch, J.; Forster, K. Probably elevation in international normalized ratio from cranberry juice. J. Pharm. Technol. 2007, 23, 104–107. [Google Scholar] [CrossRef]
- Werba, J.P.; Misaka, S.; Giroli, M.G.; Shimomura, K.; Amato, M.; Simonelli, N.; Vigo, L.; Tremoli, E. Update of green tea interactions with cardiovascular drugs and putative mechanisms. J. Food Drug Anal. 2018, 26, S72–S77. [Google Scholar] [CrossRef] [Green Version]
- Wiegman, D.-J.; Brinkman, K.; Franssen, E.J.F. Interaction of Ginkgo biloba with efavirenz. AIDS 2009, 23, 1184–1185. [Google Scholar] [CrossRef] [PubMed]
- Wong, A.L.N.; Chan, T.Y.K. Interaction between warfarin and the herbal product quilinggao. Ann. Pharmacother. 2003, 37, 836–838. [Google Scholar] [CrossRef]
- Yu, C.M.; Chan, J.; Sanderson, J.E. Chinese herbs and warfarin potentiation by ’Danshen’. J. Intern. Med. 1997, 241, 337–339. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kim, H.-S.; Kim, G.-Y.; Yeo, C.-W.; Oh, M.; Ghim, J.-L.; Shon, J.-H.; Kim, E.-Y.; Kim, D.H.; Shin, J.-G. The effect of Ginkgo biloba extracts on the pharmacokinetics and pharmacodynamics of cilostazol and its active metabolites in healthy Korean subjects. Br. J. Clin. Pharmacol. 2014, 77, 821–830. [Google Scholar] [CrossRef] [PubMed] [Green Version]
| Measure | Scoring |
|---|---|
| Is reporting of relevant demographics (sex, age, relevant conditions) adequate? | Y = +1 N = 0 |
| Are concomitant diseases and other medications associated with adverse events included (including dosing)? | |
| Are concomitant medications and other herbals/supplements documented (including dosing)? | |
| Are interactors adequately described, including scientific name of botanicals? | |
| Have alternate explanations been excluded? | |
| Is chronology complete? | |
| Is chronology sequence reasonable? | |
| Is adverse reaction adequately described? | |
| Is interaction pharmacologically feasible? | |
| Does event cease upon stopping herb? | |
| Does event recur upon rechallenge? | Y = +1 N = 0 N/A = 0 and remove from denominator |
| Latin Name, Common Name | Drug(s) or Class | N Reports | Severity (N) | Reaction |
|---|---|---|---|---|
| Curcuma longa, turmeric | Fluindione | 1 | Minor | Increased INR |
| Tacrolimus | 1 | Severe | Increased tacrolimus level | |
| contaminated with microcystin | Paclitaxel | 1 | Severe | Hepatotoxicity |
| Equisetum arvense, horsetail | Antiretrovirals | 2 | Minor | Increased viral load |
| Gingko biloba, ginkgo | Antiretrovirals | 1 | Severe | Treatment failure |
| Ibuprofen | 1 | Fatal | Intracerebral bleed | |
| Trazodone | 1 | Severe | Altered mental status | |
| Aescinate | 1 | Severe | Acute kidney injury | |
| Ginkgo biloba in multiherbal | Divalproate, phenytoin | 1 | Fatal | Seizures |
| Efavirenz | 1 | Mild | Increased viral load | |
| G biloba and H perforatum | Buspirone, fluoxetine | 1 | Mild | Serotonin syndrome |
| Hypericum perforatum, St. John’s wort | Serotoninergics | 6 | Mild (4) Severe (2) | Serotonin syndrome |
| Calcineurin inhibitors | 6 | Mild (3) Severe (3) | Decreased drug levels | |
| Clozapine | 1 | Mild | Schizophrenia | |
| Sertraline | 1 | Severe | Mania | |
| Oral contraceptive | 1 | Severe | Pregnancy | |
| H. perforatum in multiherbal | Cyclosporin | 1 | Mild | Decreased drug level |
| Lycium barbarum, goji | Warfarin | 3 | Mild (2) Severe | Increased INR Bleeding |
| Mitragyna speciosa, kratom | Quetiapine | 1 | Fatal | Increased drug level, neuroleptic malignant syndrome |
| Panax ginseng, ginseng | Phenelzine | 1 | Mild | Mania |
| Imatinib | 1 | Severe | Hepatotoxicity | |
| Raltegravir | 1 | Severe | Increased drug level | |
| contaminated with germanium | Furosemide | 1 | Severe | Treatment failure |
| P ginseng in multiherbal | Warfarin | 1 | Severe | Intracerebral bleeding |
| Vaccinium spp, cranberry | Warfarin | 8 | Mild (6) Fatal (2) | 6 Increased INR, 2 GI and pericardial bleeding |
| Clinical Studies | N Studies | N Case Reports | Top Selling Herb Lists Ranks |
|---|---|---|---|
| Hypericum perforatum St. John’s wort | 17 | 17 | 0, 0 |
| Ginkgo biloba, ginkgo | 11 | 7 | 17, 21 |
| Panax ginseng, ginseng | 6 | 4 plus 3 NOS | 30, 30 |
| Allium sativum, garlic | 3 | 1 (multiherb) | 8, 15 |
| Hydrastis canadensis, goldenseal | 3 | 0 | 0, 0 |
| Piper methysticum, kava-kava | 3 | 2 (multiherb) | 0, 28 |
| Silybum marianum, milk thistle | 3 | 0 | 23, 10 |
| Actea racemosa, black cohosh | 2 | 0 | 15, 0 |
| Curcuma longa, turmeric | 2 | 3 | 4, 3 |
| Crataegus spp, hawthorne | 2 | 0 | 0, 38 |
| Interaction Checker | Kappa | 95% CI |
|---|---|---|
| Integrative pro [38] | 0.011 | (−0.013, 0.035) |
| Lexicomp [36] | 0.012 | (−0.012, 0.035) |
| Medscape [39] | 0.018 | (−0.007, 0.043) |
| MSKCC [40] | 0.017 | (−0.008, 0.042) |
| Natural Medicine Database [41] | 0.014 | (−0.008, 0.036) |
| Stockley’s Herb Drug Interaction [16] | 0.009 | (−0.015, 0.033) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Babos, M.B.; Heinan, M.; Redmond, L.; Moiz, F.; Souza-Peres, J.V.; Samuels, V.; Masimukku, T.; Hamilton, D.; Khalid, M.; Herscu, P. Herb–Drug Interactions: Worlds Intersect with the Patient at the Center. Medicines 2021, 8, 44. https://0-doi-org.brum.beds.ac.uk/10.3390/medicines8080044
Babos MB, Heinan M, Redmond L, Moiz F, Souza-Peres JV, Samuels V, Masimukku T, Hamilton D, Khalid M, Herscu P. Herb–Drug Interactions: Worlds Intersect with the Patient at the Center. Medicines. 2021; 8(8):44. https://0-doi-org.brum.beds.ac.uk/10.3390/medicines8080044
Chicago/Turabian StyleBabos, Mary Beth, Michelle Heinan, Linda Redmond, Fareeha Moiz, Joao Victor Souza-Peres, Valerie Samuels, Tarun Masimukku, David Hamilton, Myra Khalid, and Paul Herscu. 2021. "Herb–Drug Interactions: Worlds Intersect with the Patient at the Center" Medicines 8, no. 8: 44. https://0-doi-org.brum.beds.ac.uk/10.3390/medicines8080044





