Tissue Engineering in Musculoskeletal Tissue: A Review of the Literature
Abstract
:1. Introduction
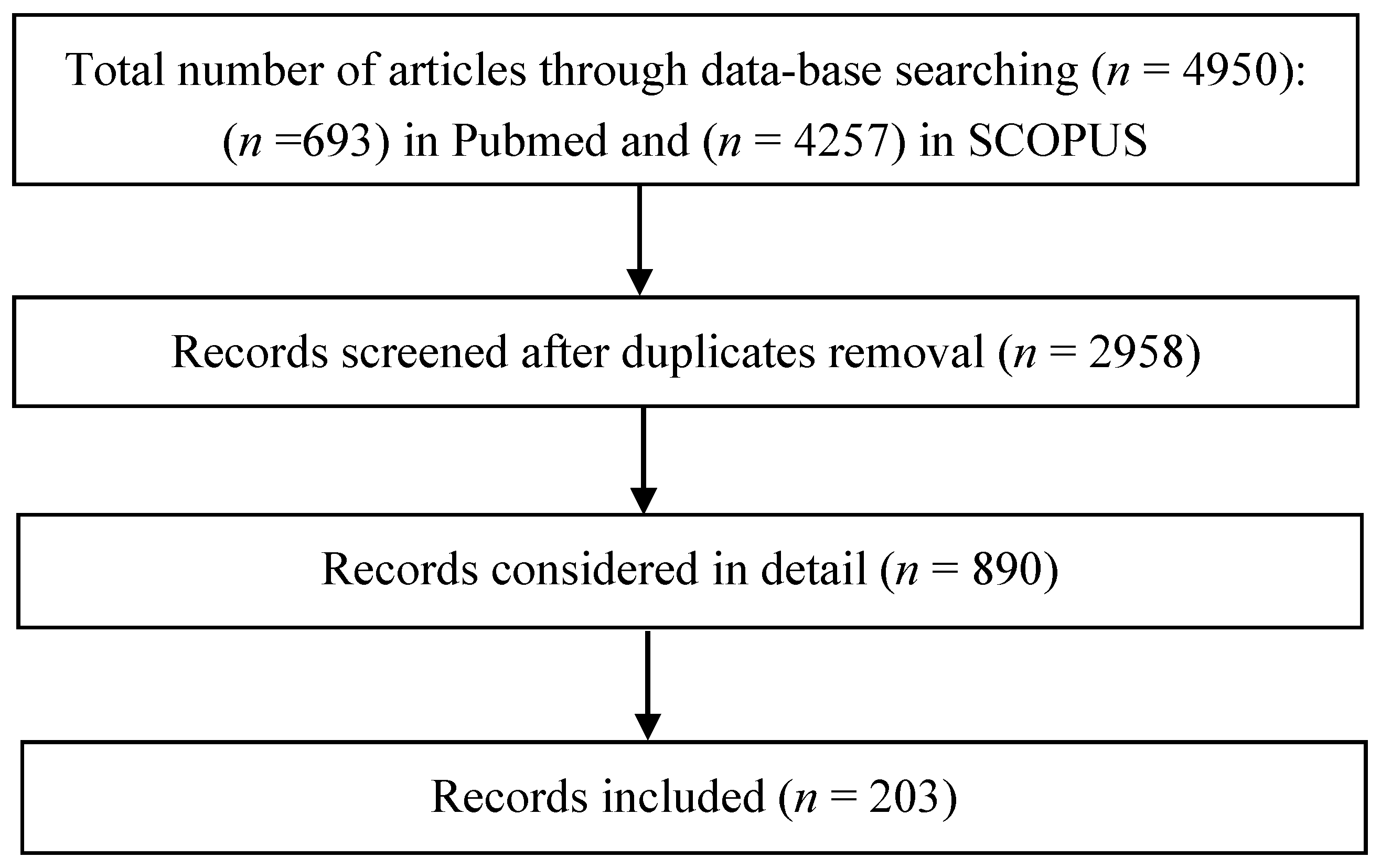
1.1. Methods
1.2. Results
2. Biomaterials
2.1. Natural and Synthetic Polymers
2.2. Inorganic Biomaterials
2.3. Hybrid Biomaterials
3. Biomaterials Modifications
3.1. Laser Treatment
3.2. Ion Implantation
3.3. Plasma Treatment
| Application | Cell Type | Plasma Source | Gas | Substrate | Results | Reference |
|---|---|---|---|---|---|---|
| Bone | Human-induced pluripotent stem cells (iPSCs) | MW | O2 | Polyethersulfone (PES) | Enhanced proliferation and osteogenesis | [89] |
| Human primary osteosarcoma cells (Saos-2) | RF | O2 and Ar | PCL | Improved cell viability and proliferation | [90] | |
| Mouse osteoblast cells (MC3T3-E1) | RF | Ar/O2, NH3/O2 and N2/H2 | PCL | Improved cell attachment and proliferation | [91] | |
| MC3T3 | RF | O2 | PCL | Improved cell adhesion and ALP activity | [92] | |
| Human mesenchymal stem cells (hMSCs) | Not specified | Ar and N2 | PCL | Improved cell attachment. Accelerated differentiation towards osteoblasts | [93] | |
| hMSCs | Not specified | He | PCL/CMC | Enhanced osteoinductivity without external osteogenic differential agent, did not support the proliferation | [94] | |
| hMSCs | RF | O2 | PolyActive | Significant upregulation of bone sialoprotein and osteonectin expression | [95] | |
| hMSCs | Not specified | Air | PLGA | Greatly enhances peptide immobilization which increases the ALP activity, calcium content and expression osteogenic markers of collagen type-I, osteocalcin (OC) and osteopontin (OP) | [96] | |
| hMSCs | RF | O2 | PLLA | Improved expression of genes associated with osteoblast linkage | [97] | |
| hMSCs | Not specified | Air | PLLA | Improved cell proliferation, ALP activity and mineralization | [98] | |
| hMSCs | Not specified | Air | PLLA/PVA | Increases the ALP activity level, protein content and calcium deposition | [99] | |
| Cartilage | Mouse chondrocyte teratocarcinoma-derived cells (ATDC5) | RF | O2 and Ar | PCL | Improved cell viability and proliferation | [90] |
| Neonatal human knee articular chondrocytes (nHAC-kn) | MW | Ar | Silk fibroin | Improved cell attachment, proliferation and glycosaminoglycan synthesis | [100] | |
| Schwann cells (RT4-D6P2T) | RF | Air | PCL | Improved cell proliferation | [101] | |
| MSCs | Not specified | Air | PCL | Improved cell attachment and proliferation, chondro-differentiation in a non-differential medium | [102] | |
| Mouse lung fibroblasts (L929) | RF | O2 and Ar | PCL | Improved cell viability and proliferation | [90] | |
| Human foreskin fibroblasts (HFFs) | DBD | Ar, N2 and He/NH3 | PCL | Improved cell adhesion and proliferation | [103] | |
| HFFs | DBD | Ar, N2 and He/NH3 | Chitosan/PEO | Improved cell adhesion and proliferation | [104] | |
| Normal human epidermal keratinocytes and fibroblasts (NHEKs and NHEFs) | RF | O2 | Silk fibroin | Improved cell attachment | [105] | |
| Epithelial | 3T3 fibroblasts | DBD | O2 and NH3 | PLGA | Improved cell adhesion and proliferation | [101] |
| Mouse embryonic fibroblasts (MEFs) | Corona | N2 | PLLA | More elongated and dendritic cell morphology. Improved cell vitality | [106] | |
| Bovine aorta endothelial cells (BAECs) | RF | Ar and Ar-NH3/H2 | - | Improved cell adhesion, spreading and infiltration | [107] | |
| Stem cells | Porcine mesenchymal stem cells (pMSCs) | RF | O2 | PLLA | Improved cell adhesion | [100] |
| Adipose-derived stem cells (ADSCs) | DBD | Ar and Air | PCL | Improved cell adhesion, proliferation, spreading and viability | [108] | |
| Muscle | Primary porcine smooth muscle cells (SMCs) | RF | Air | PCL | Improved spread-out cell morphology | [100] |
| Bovine smooth muscle cells (BSMCs) | RF | Ar and Ar-NH3/H2 | - | Improved adhesion, spreading and infiltration | [107] | |
| Immune System | Human monocyte | RF | Air | PLLA | Disruption of macrophage polarization balance towards an anti-inflammatory profileImproved cell morphology with filopodia-like and podosome-like structures on plasma-treated samples | [109] |
4. Scaffolding Strategies
4.1. Phase Separation
4.2. 3D Printing
4.2.1. Fused Deposition Modeling
4.2.2. Selective Laser Sintering
4.2.3. Stereolithography
4.2.4. Bioprinting
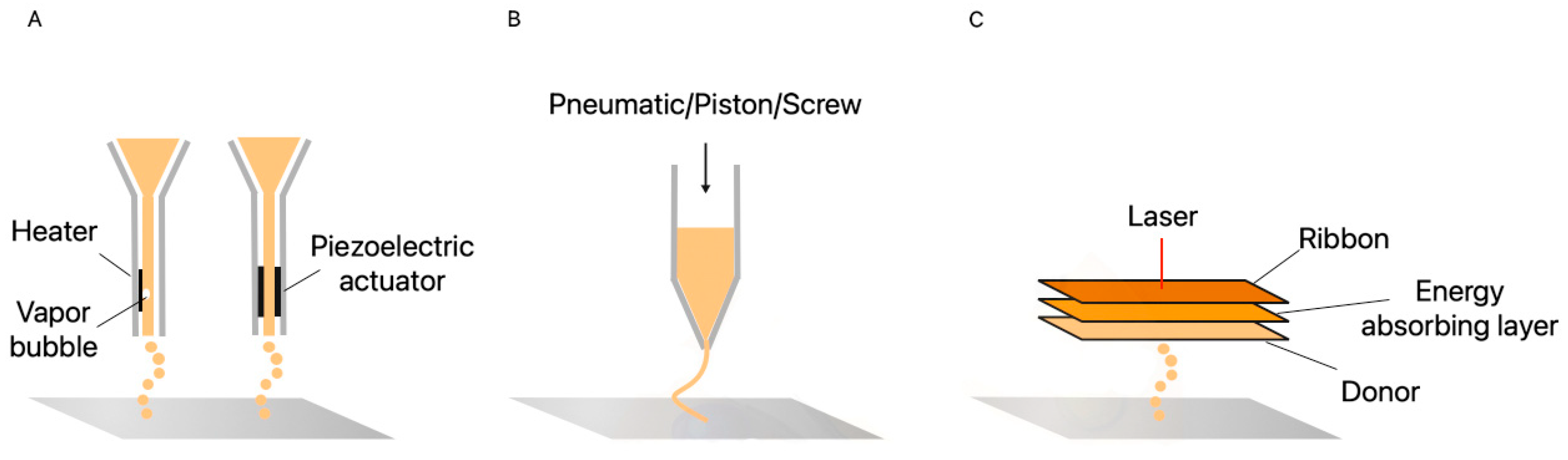
4.2.5. Inkjet Bioprinting
4.2.6. Extrusion
4.2.7. Laser-Assisted Bioprinting
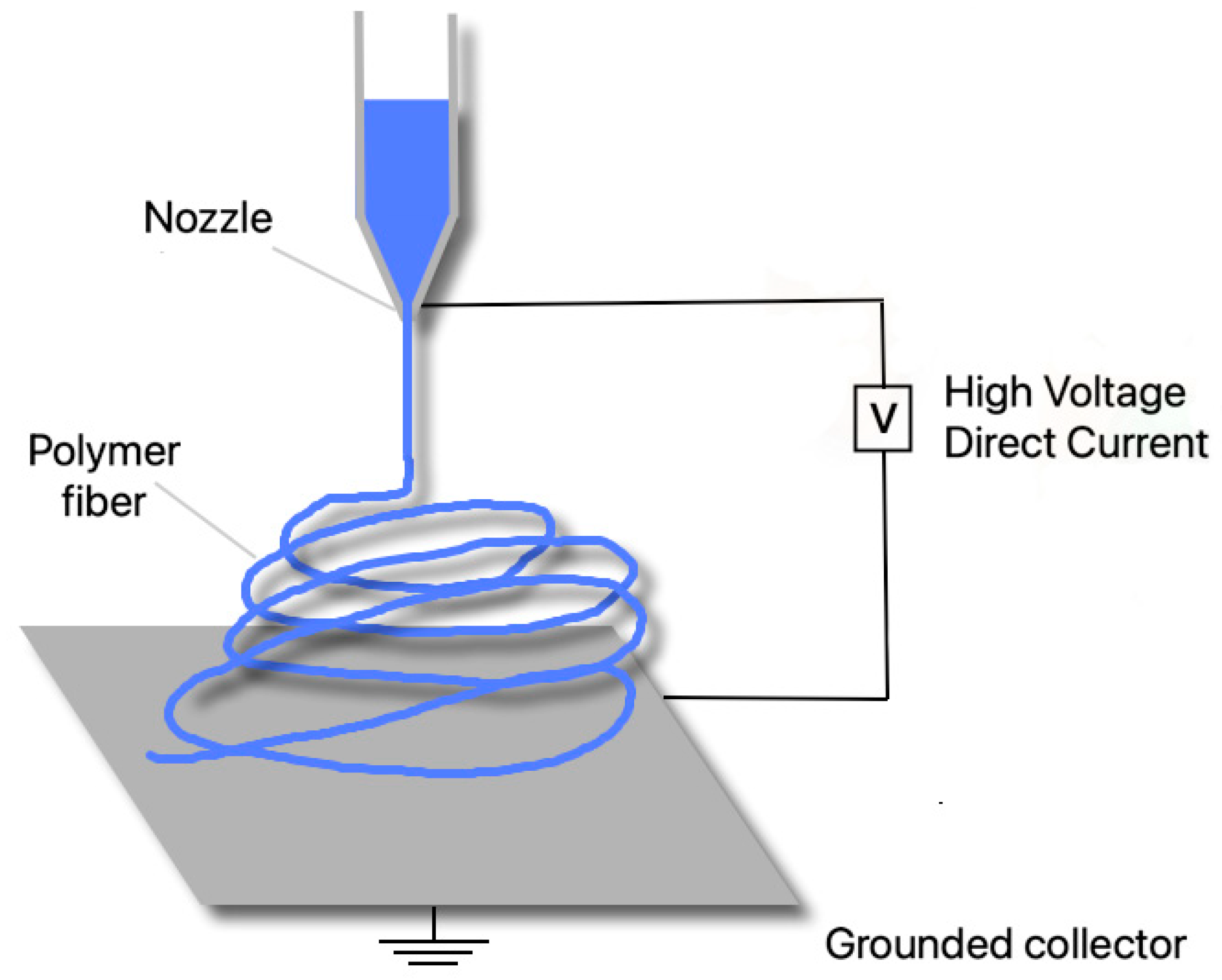
4.3. Electrospinning
5. Scaffold-Free Approaches
5.1. Self-Organization Process
5.1.1. Cell-Sheet Engineering
5.1.2. Pellet Culture
5.1.3. Aggregate Culture
5.2. Self-Assembling Process
6. Clinical Use of Tissue Engineered Products
7. Conclusions and Future Directions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Gingery, A.; Killian, M.L. Special focus issue on strategic directions in musculoskeletal tissue engineering. Tissue Eng. 2017, 23, 873. [Google Scholar] [CrossRef]
- Devore, D.I.; Walters, T.J.; Christy, R.J.; Rathbone, C.R.; Hsu, J.R.; Baer, D.G.; Wenke, J.C. For combat wounded: Extremity trauma therapies from the USAISR. Mil. Med. 2011, 176, 660–663. [Google Scholar]
- Corona, B.T.; Rivera, J.C.; Owens, J.G.; Wenke, J.C.; Rathbone, C.R. Volumetric muscle loss leads to permanent disability following extremity trauma. J. Rehabil. Res. Dev. 2015, 52, 785–792. [Google Scholar] [PubMed]
- Carnes, M.E.; Pins, G.D. Skeletal muscle tissue engineering: Biomaterials-based strategies for the treatment of volumetric muscle loss. Bioengineering 2020, 7, 85. [Google Scholar] [CrossRef]
- Garg, K.; Ward, C.L.; Hurtgen, B.J.; Wilken, J.M.; Stinner, D.J.; Wenke, J.C.; Owens, J.G.; Corona, B.T. Volumetric muscle loss: Persistent functional deficits beyond frank loss of tissue. J. Orthop. Res. 2015, 33, 40–46. [Google Scholar] [PubMed]
- Mase, V.J.; Hsu, J.R.; Wolf, S.E.; Wenke, J.C.; Baer, D.G.; Owens, J.; Badylak, S.F.; Walters, J.T.R. Clinical application of an acellular biologic scaffold for surgical repair of a large, traumatic quadriceps femoris muscle defect. Orthopedics 2010, 33, 511. [Google Scholar] [CrossRef] [PubMed]
- Aurora, A.; Garg, K.; Corona, B.T.; Walters, J.T.R. Physical rehabilitation improves muscle function following volumetric muscle loss injury. BMC Sports Sci. Med. Rehabil. 2014, 6, 41. [Google Scholar] [CrossRef] [Green Version]
- Grogan, B.F.; Hsu, J.R.; Skeletal Trauma Research Consortium. Volumetric muscle loss. J. Am. Acad. Orthop. Surg. 2011, 19, S35–S37. [Google Scholar]
- Doi, K.; Hattori, Y.; Tan, S.-H.; Dhawan, V. Basic science behind functioning free muscle transplantation. Clin. Plast. Surg. 2002, 29, 483–495. [Google Scholar]
- Eckardt, A.; Fokas, K. Microsurgical reconstruction in the head and neck region: An 18-year experience with 500 consecutive cases. J. Cranio Maxillofac. Surg. 2003, 31, 197–201. [Google Scholar]
- Lin, C.-H.; Lin, Y.-T.; Yeh, J.-T.; Chen, C.-T. Free Functioning Muscle Transfer for Lower Extremity Posttraumatic Composite Structure and Functional Defect. Plast. Reconstr. Surg. 2007, 119, 2118–2126. [Google Scholar] [PubMed]
- Chuang, D.C.-C. Free tissue transfer for the treatment of facial paralysis. Facial Plast. Surg. 2008, 24, 194–203. [Google Scholar] [PubMed]
- Dueweke, J.J.; Awan, T.M.; Mendias, C.L. Regeneration of skeletal muscle. Cell Tissue Res. 2011, 347, 759–774. [Google Scholar]
- Diwan, A.; Eberlin, K.R.; Smith, R. The principles and practice of open fracture care. Chin. J. Traumatol. 2018, 21, 187–192. [Google Scholar]
- Bianchi, B.; Copelli, C.; Ferrari, S.; Ferri, A.; Sesenna, E. Free flaps: Outcomes and complications in head and neck reconstructions. J. Craniomaxillofac. Surg. 2009, 37, 438–442. [Google Scholar]
- Lawson, R.; Levin, L.S. Principles of free tissue transfer in orthopaedic practice. J. Am. Acad. Orthop. Surg. 2007, 15, 290–299. [Google Scholar]
- Shores, J.T.; Brandacher, G.; Lee, W.P.A. Hand and upper extremity transplantation: An update of outcomes in the worldwide experience. Plast. Reconstr. Surg. 2015, 135, 351e–360e. [Google Scholar]
- Brannstrom, M. Womb transplants with live births: An update and the future. Expert. Opin. Biol. Ther. 2017, 17, 1105–1112. [Google Scholar]
- Dubernard, J.-M.; Lengelé, B.; Morelon, E.; Testelin, S.; Badet, L.; Moure, C.; Beziat, J.-L.; Dakpé, S.; Kanitakis, J.; D’Hauthuille, C.; et al. Outcomes 18 months after the first human partial face transplantation. N. Engl. J. Med. 2007, 357, 2451–2460. [Google Scholar]
- Ma, J.; Smietana, M.J.; Kostrominova, T.Y.; Wojtys, E.M.; Larkin, L.M.; Arruda, E.M. Engineered bone–ligament–bone constructs for anterior cruciate ligament replacement. Tissue Eng. Part A 2012, 18, 103–116. [Google Scholar]
- Lechler, R.I.; Sykes, M.; Thomson, A.W.; Turka, L.A. Organ transplantation—How much of the promise has been realized? Nat. Med. 2005, 11, 605–613. [Google Scholar] [CrossRef] [PubMed]
- Klumpp, D.; Horch, R.E.; Kneser, U.; Beier, J.P. Engineering skeletal muscle tissue—New perspectives in vitro and in vivo. J. Cell. Mol. Med. 2010, 14, 2622–2629. [Google Scholar] [CrossRef] [PubMed]
- Vacanti, J. Tissue engineering and regenerative medicine: From first principles to state of the art. J. Pediatr. Surg. 2010, 45, 291–294. [Google Scholar] [CrossRef] [PubMed]
- Berthiaume, F.; Maguire, T.J.; Yarmush, M.L. Tissue engineering and regenerative medicine: History, progress, and challenges. Annu. Rev. Chem. Biomol. Eng. 2011, 2, 403–430. [Google Scholar] [CrossRef]
- Gu, B.K.; Choi, D.J.; Park, S.J.; Kim, M.S.; Kang, C.M.; Kim, C.-H. 3-Dimensional Bioprinting for Tissue Engineering Applications. Biomater. Res. 2016, 20, 12. [Google Scholar] [CrossRef] [Green Version]
- Vandenburgh, H.H.; Karlisch, P.; Farr, L. Maintenance of highly contractile tissue-cultured avian skeletal myotubes in collagen gel. In Vitro Cell. Dev. Biol. 1988, 24, 166–174. [Google Scholar] [CrossRef]
- Lanza, R.; Langer, R.; Vacanti, J. Principles of Tissue Engineering, 3rd ed.; Academic Press: Cambridge, MA, USA, 2011. [Google Scholar]
- KKilian, K.A.; Bugarija, B.; Lahn, B.T.; Mrksich, M. Geometric cues for directing the differentiation of mesenchymal stem cells. Proc. Natl. Acad. Sci. USA 2010, 107, 4872–4877. [Google Scholar] [CrossRef] [Green Version]
- Norman, J.J.; Desai, T.A. Methods for fabrication of nanoscale topography for tissue engineering scaffolds. Ann. Biomed. Eng. 2006, 34, 89–101. [Google Scholar] [CrossRef]
- Mano, J.F.; Silva, G.A.; Azevedo, H.S.; Malafaya, P.B.; Sousa, R.A.; Silva, S.S.; Boesel, L.F.; Oliveira, J.M.; Santos, T.C.; Marques, A.P.; et al. Natural origin biodegradable systems in tissue engineering and regenerative medicine: Present status and some moving trends. J. R. Soc. Interface 2007, 4, 999–1030. [Google Scholar] [CrossRef] [Green Version]
- Schenke-Layland, K.; Nerem, R.M. In Vitro human tissue models—Moving towards personalized regenerative medicine. Adv. Drug. Deliv. Rev. 2011, 63, 195–196. [Google Scholar] [CrossRef]
- Porzionato, A.; Sfriso, M.; Pontini, A.; Macchi, V.; Petrelli, L.; Pavan Natali, A.; Bassetto, F.; Vindigni, V.; de Caro, R. Decellularized human skeletal muscle as biologic scaffold for reconstructive surgery. Int. J. Mol. Sci. 2015, 16, 14808–14831. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wilson, K.; Terlouw, A.; Roberts, K.; Wolchok, J.C. The characterization of decellularized human skeletal muscle as a blueprint for mimetic scaffolds. J. Mater. Sci. Mater. Electron. 2016, 27, 125. [Google Scholar] [CrossRef] [PubMed]
- Davari, H.R.; Rahim, M.B.; Tanideh, N.; Sani, M.; Tavakoli, H.R.; Rasekhi, A.R.; Monabati, A.; Koohi-Hosseinabadi, O.; Gholami, S. Partial replacement of left hemidiaphragm in dogs by either cryopreserved or decellularized heterograft patch. Interact. Cardiovasc. Thorac. Surg. 2016, 23, 623–629. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wolf, M.T.; Daly, K.A.; Reing, J.E.; Badylak, S.F. Biologic scaffold composed of skeletal muscle extracellular matrix. Biomaterials 2012, 33, 2916–2925. [Google Scholar] [CrossRef] [Green Version]
- Porzionato, A.; Stocco, E.; Barbon, S.; Grandi, F.; Macchi, V.; de Caro, R. Tissue-engineered grafts from human decellularized extracellular matrices: A systematic review and future perspectives. Int. J. Mol. Sci. 2018, 19, 4117. [Google Scholar] [CrossRef] [Green Version]
- Gunja, N.J.; Athanasiou, K.A. Biodegradable materials in arthroscopy. Sports Med. Arthrosc. Rev. 2006, 14, 112–119. [Google Scholar] [CrossRef]
- Pina, S.; Ferreira, J.M.F. Bioresorbable plates and screws for clinical applications: A review. J. Heal. Eng. 2012, 3, 243–260. [Google Scholar] [CrossRef] [Green Version]
- Katti, D.; Lakshmi, S.; Langer, R.; Laurencin, C.T. Toxicity, biodegradation and elimination of polyanhydrides. Adv. Drug Deliv. Rev. 2002, 54, 933–961. [Google Scholar] [CrossRef]
- Pereira, D.R.; Canadas, R.F.; Silva-Correia, J.; Marques, A.P.; Reis, R.L.; Oliveira, J.M. Gellan gum-based hydrogel bilayered scaffolds for osteochondral tissue engineering. Key Eng. Mater. 2014, 587, 255–260. [Google Scholar] [CrossRef] [Green Version]
- Elowsson, L.; Kirsebom, H.; Carmignac, V.; Durbeej, M.; Mattiasson, B. Porous protein-based scaffolds prepared through freezing as potential scaffolds for tissue engineering. J. Mater. Sci. Mater. Med. 2010, 23, 2489–2498. [Google Scholar] [CrossRef]
- Huang, Y.-C.; Dennis, R.G.; Larkin, L.; Baar, K. Rapid formation of functional musclein vitro using fibrin gels. J. Appl. Physiol. 2005, 98, 706–713. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jenkins, T.L.; Little, D. Synthetic scaffolds for muskoloskeletal tissue engineering: Cellular responses to fiber parameters. Regen. Med. 2019, 4, 15. [Google Scholar] [CrossRef]
- Tseng, L.-F.; Wang, J.; Baker, R.M.; Wang, G.; Mather, P.T.; Henderson, J.H. Osteogenic capacity of human adipose-derived stem cells is preserved following triggering of shape memory scaffolds. Tissue Eng. Part A 2016, 22, 1026–1035. [Google Scholar] [CrossRef] [PubMed]
- Ninagawa, N.T.; Isobe, E.; Hirayama, Y.; Murakami, R.; Komatsu, K.; Nagai, M.; Kobayashi, M.; Kawabata, Y.; Torihashi, S. Transplantated mesenchymal stem cells derived from embryonic stem cells promote muscle regeneration and accelerate functional recovery of injured skeletal muscle. BioRes. Open Access 2013, 2, 295–306. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fraley, S.I.; Wu, P.-H.; He, L.; Feng, Y.; Krisnamurthy, R.; Longmore, G.D.; Wirtz, D. Three-dimensional matrix fiber alignment modulates cell migration and MT1-MMP utility by spatially and temporally directing protrusions. Sci. Rep. 2015, 5, 14580. [Google Scholar] [CrossRef] [Green Version]
- Wang, J.; Quach, A.; Brasch, M.E.; Turner, C.E.; Henderson, J.H. On-command on/off switching of progenitor cell and cancer cell polarized motility and aligned morphology via a cytocompatible shape memory polymer scaffold. Biomaterials 2017, 140, 150–161. [Google Scholar] [CrossRef]
- Guvendiren, M.; Burdick, J.A. Engineering synthetic hydrogel microenvironments to instruct stem cells. Curr. Opin. Biotechnol. 2013, 24, 841–846. [Google Scholar] [CrossRef] [Green Version]
- Kisiel, M.; Martino, M.M.; Ventura, M.; Hubbell, J.A.; Hilborn, J.; Ossipov, D.A. Improving the osteogenic potential of BMP-2 with hyaluronic acid hydrogel modified with integrin-specific fibronectin fragment. Biomaterials 2013, 34, 704–712. [Google Scholar] [CrossRef]
- Shekaran, A.; García, J.R.; Clark, A.Y.; Kavanaugh, T.E.; Lin, A.S.; Guldberg, R.E.; García, A.J. Bone regeneration using an alpha2beta1 integrin-specific hydrogel as a BMP-2 delivery vehicle. Biomaterials 2014, 35, 5453–5461. [Google Scholar] [CrossRef] [Green Version]
- Olvera, D.; Sathy, B.N.; Carroll, S.F.; Kelly, D.J. Modulating microfibrillar alignment and growth factor stimulation to regulate mesenchymal stem cell differentiation. Acta Biomater. 2017, 64, 148–160. [Google Scholar] [CrossRef]
- Cheng, X.; Tsao, C.; Sylvia, V.L.; Cornet, D.; Nicolella, D.P.; Bredbenner, T.L.; Christy, R.J. Platelet-derived growth-factor-releasing aligned collagen–nanoparticle fibers promote the proliferation and tenogenic differentiation of adipose-derived stem cells. Acta Biomater. 2014, 10, 1360–1369. [Google Scholar] [CrossRef] [PubMed]
- Quarta, M.; Brett, J.; DiMarco, R.; de Morree, A.; Boutet, S.; Chacon, R.; Gibbons, M.; Garcia, V.; Su, J.; Shrager, J.; et al. An artificial niche preserves the quiescence of muscle stem cells and enhances their therapeutic efficacy. Nat. Biotechnol. 2016, 34, 752–759. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Konieczny, P.; Swiderski, K.; Chamberlain, J.S. Gene and cell-mediated therapies for muscular dystrophy. Muscle Nerve 2013, 47, 649–663. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Partridge, T. Impending therapies for Duchenne muscular dystrophy. Curr. Opin. Neurol. 2011, 24, 415–422. [Google Scholar] [CrossRef] [PubMed]
- Bohner, M. Calcium orthophosphates in medicine: From ceramics to calcium phosphate cements. Injury 2000, 31, 37–47. [Google Scholar] [CrossRef]
- Pina, S.; Canadas, R.; Jiménez, G.; Perán, M.; Marchal, J.A.; Reis, R.L.; Oliveira, J.M. Biofunctional ionic-doped calcium phosphates—Silk fibroin composites for bone tissue engineering scaffolding. Cells Tissues Organs 2017, 204, 150–163. [Google Scholar] [CrossRef]
- Mestres, G.; Le Van, C.; Ginebra, M.-P. Silicon-stabilized α-tricalcium phosphate and its use in a calcium phosphate cement: Characterization and cell response. Acta Biomater. 2012, 8, 1169–1179. [Google Scholar] [CrossRef]
- Yoshida, T.; Kikuchi, M.; Koyama, Y.; Takakuda, K. Osteogenic activity of MG63 cells on bone-like hydroxyapatite/collagen nanocomposite sponges. J. Mater. Sci. Mater. Electron. 2009, 21, 1263–1272. [Google Scholar] [CrossRef]
- Azami, M.; Samadikuchaksaraei, A.; Poursamar, S.A. Synthesis and characterization of a laminated hydroxyapatite/gelatin nanocomposite scaffold with controlled pore structure for bone tissue engineering. Int. J. Artif. Organs 2010, 33, 86–95. [Google Scholar] [CrossRef]
- Heris, H.K.; Rahmat, M.; Mongeau, L. Characterization of a Hierarchical Network of Hyaluronic Acid/Gelatin Composite for use as a Smart Injectable Biomaterial. Macromol. Biosci. 2012, 12, 202–210. [Google Scholar] [CrossRef] [Green Version]
- Wang, Y.; Cui, W.; Chou, J.; Wen, S.; Sun, Y.; Zhang, H. Electrospun nanosilicates-based organic/inorganic nanofibers for potential bone tissue engineering. Colloids Surf. B Biointerfaces 2018, 172, 90–97. [Google Scholar] [CrossRef] [PubMed]
- Bacakova, L.; Filová, E.; Parizek, M.; Ruml, T.; Švorčík, V. Modulation of cell adhesion, proliferation and differentiation on materials designed for body implants. Biotechnol. Adv. 2011, 29, 739–767. [Google Scholar] [CrossRef] [PubMed]
- Parizek, M.; Kasalkova, N.S.; Bacakova, L.; Svindrych, Z.; Slepička, P.; Bacakova, M.; Lisa, V.; Svorcik, V. Adhesion, Growth, and Maturation of Vascular Smooth Muscle Cells on Low-Density Polyethylene Grafted with Bioactive Substances. BioMed Res. Int. 2013, 2013, 371430. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Granados, E.; Martinez-Calderon, M.; Gomez, M.; Rodriguez, A.; Olaizola, S.M. Photonic structures in diamond based on femtosecond UV laser induced periodic surface structuring (LIPSS). Opt. Express 2017, 25, 15330–15335. [Google Scholar] [CrossRef]
- Kim, H.-C.; Reinhardt, H.; Hillebrecht, P.; Hampp, N.A. Photochemical preparation of sub-wavelength heterogeneous laser-induced periodic surface structures. Adv. Mater. 2012, 24, 1994–1998. [Google Scholar] [CrossRef]
- Rebollar, E.; Frischauf, I.; Olbrich, M.; Peterbauer, T.; Hering, S.; Preiner, J.; Hinterdorfer, P.; Romanin, C.; Heitz, J. Proliferation of aligned mammalian cells on laser-nanostructured polystyrene. J. Biomater. 2008, 29, 1796–1806. [Google Scholar] [CrossRef]
- Neděla, O.; Slepička, P.; Švorčík, V. Surface modification of polymer substrates for biomedical applications. Materials 2017, 10, 1115. [Google Scholar] [CrossRef]
- Tsougeni, K.; Petrou, P.S.; Awsiuk, K.; Marzec, M.M.; Ioannidis, N.; Petrouleas, V.; Tserepi, A.; Kakabakos, S.E.; Gogolides, E. Covalent biomolecule immobilization on plasma-nanotextured chemically stable substrates. ACS Appl. Mater. Interfaces 2015, 7, 14670–14681. [Google Scholar] [CrossRef]
- Bilek, M.M.; Bax, D.V.; Kondyurin, A.; Yin, Y.; Nosworthy, N.J.; Fisher, K.; Waterhouse, A.; Weiss, A.S.; Dos Remedios, C.G.; McKenzie, D.R. Free radical functionalization of surfaces to prevent adverse responses to biomedical devices. Proc. Natl. Acad. Sci. USA 2011, 108, 14405–14410. [Google Scholar] [CrossRef] [Green Version]
- Bourkoula, A.; Constantoudis, V.; Kontziampasis, D.; Petrou, S.; Kakabakos, S.E.; Tserepi, A.; Gogolides, E. Roughness threshold for cell attachment and proliferation on plasma micronanotextured polymeric surfaces: The case of primary human skin skin fibroblasts and mouse immortalized 3T3 fibroblasts. J. Phys. D Appl. Phys. 2016, 49, 304002. [Google Scholar] [CrossRef]
- Kitsara, M.; Blanquer, A.; Murillo, G.; Humblot, V.; De Bragança Vieira, S.; Nogués, C.; Ibáñez, E.; Estevea, J.; Barrios, L. Permanently hydrophilic, piezoelectric pvdf nanofibrous scaffolds promoting unaided electromechanical stimulation on osteoblasts. Nanoscale 2019, 1–3. [Google Scholar] [CrossRef] [PubMed]
- Koning, M.; Harmsen, M.C.; van Luyn, M.J.A.; Werker, P.M.N. Current opportunities and challenges in skeletal muscle tissue engineering. J. Tissue Eng. Regen. Med. 2009, 3, 407–415. [Google Scholar] [CrossRef] [PubMed]
- Larkin, L.M.; van der Meulen, J.H.; Dennis, R.G.; Kennedy, J.B. Functional evaluation of nerve–skeletal muscle constructs engineered in vitro. In Vitro Cell. Dev. Biol. Anim. 2006, 42, 75–82. [Google Scholar] [CrossRef] [PubMed]
- Huang, N.F.; Lee, R.J.; Li, S. Engineering of aligned skeletal muscle by micropatterning. Am. J. Transl. Res. 2010, 2, 43–55. [Google Scholar] [PubMed]
- Ramalingam, M.; Khademhosseini, A.; Fisher, J.; Mikos, A. Micropatterned biomaterials for cell and tissue engineering. In Biomedical Engineering Handbook, 4th ed.; CRC Press: Boca Raton, FL, USA, 2012; pp. 1–17. [Google Scholar]
- Kane, R.S.; Takayama, S.; Ostuni, E.; Ingber, D.E.; Whitesides, G.M. Patterning proteins and cells using soft lithography. Biomaterials 1999, 20, 2363. [Google Scholar] [CrossRef]
- Khademhosseini, A.; Suh, K.Y.; Jon, S.; Eng, G.; Yeh, J.; Chen, G.-J.; Langer, R. A soft lithographic approach to fabricate patterned microfluidic channels. Anal. Chem. 2004, 76, 3675. [Google Scholar] [CrossRef]
- Bajaj, P.; Reddy, B., Jr.; Millet, L.; Wei, C.; Zorlutuna, P.; Bao, G.; Bashir, R. Patterning the differentiation of C2C12 skeletal myoblasts. Integr. Biol. 2011, 3, 897. [Google Scholar] [CrossRef]
- Kaji, H.; Kawashima, A.T.; Nishizawa, M. Patterning cellular motility using an electrochemical technique and a geometrically confined environment. Langmuir 2006, 22, 10784. [Google Scholar] [CrossRef]
- Ahmed, W.W.; Wolfram, T.; Goldyn, A.M.; Bruellhoff, K.; Rioja, B.A.; Möller, M.; Spatz, J.P.; Saif, T.A.; Groll, J.; Kemkemer, R. Myoblast morphology and organization on biochemically micro-patterned hydrogel coatings under cyclic mechanical strain. Biomaterials 2010, 31, 250. [Google Scholar] [CrossRef]
- Shimizu, K.; Fujita, H.; Nagamori, E. Micropatterning of single myotubes on a thermoresponsive culture surface using elastic stencil membranes for single-cell analysis. J. Biosci. Bioeng. 2010, 109, 174. [Google Scholar] [CrossRef]
- Cui, X.; Gao, G.; Qiu, Y. Accelerated myotube formation using bioprinting technology for biosensor applications. Biotechnol. Lett. 2013, 35, 315. [Google Scholar] [CrossRef] [PubMed]
- Nagamine, K.; Kawashima, T.; Ishibashi, T.; Kaji, H.; Kanzaki, M.; Nishizawa, M. Micropatterning contractile C2C12 myotubes embedded in a fibrin gel. Biotechnol. Bioeng. 2010, 105, 1161. [Google Scholar] [CrossRef] [PubMed]
- Fujie, T.; Ahadian, S.; Liu, H.; Chang, H.; Ostrovidov, S.; Wu, H.; Bae, H.; Nakajima, K.; Kaji, H.; Khademhosseini, A. Engineered nanomembranes for directing cellular organization toward flexible biodevices. Nano Lett. 2013, 13, 3185–3192. [Google Scholar] [CrossRef]
- Sasagawa, T.; Shimizu, T.; Sekiya, S.; Shimizu, T.; Yamato, M.; Sawa, Y.; Okano, T. Design of prevascularized three-dimensional cell-dense tissues using a cell sheet stacking manipulation technology. Biomaterials 2010, 31, 1646. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, H.; Shimizu, T.; Nakayama, M.; Yamato, M.; Okano, T. The use of anisotropic cell sheets to control orientation during the self-organization of 3D muscle tissue. Biomaterials 2013, 34, 7372. [Google Scholar] [CrossRef] [Green Version]
- Guillaume-Gentil, O.; Gabi, M.; Zenobi-Wong, M.; Vörös, J. Electrochemically switchable platform for the micro-patterning and release of heterotypic cell sheets. Biomed. Microdevices 2011, 13, 221. [Google Scholar] [CrossRef] [Green Version]
- Nandakumar, A.; Birgani, Z.T.; Santos, D.; Mentink, A.; Auffermann, N.; Van Der Werf, K.; Bennink, M.; Moroni, L.; Van Blitterswijk, C.A.; Habibovic, P. Surface modification of electrospun fibre meshes by oxygen plasma for bone regeneration. Biofabrication 2012, 5, 015006. [Google Scholar] [CrossRef]
- Feng, Z.-Q.; Lu, H.-J.; Leach, M.K.; Huang, N.-P.; Wang, Y.-C.; Liu, C.-J.; Gu, Z.-Z. The influence of type-I collagen-coated PLLA aligned nanofibers on growth of blood outgrowth endothelial cells. Biomed. Mater. 2010, 5, 065011. [Google Scholar] [CrossRef]
- Vesel, A.; Mozetic, M. Modification of PET surface by nitrogen plasma treatment. J. Phys. Conf. Ser. 2008, 100, 012–027. [Google Scholar] [CrossRef] [Green Version]
- Liu, W.; Zhan, J.; Su, Y.; Wu, T.; Wu, C.; Ramakrishna, S.; Mo, X.; Al-Deyab, S.S.; El-Newehy, M. Effectsof plasma treatment to nanofibers on initial cell adhesion and cell morphology. Colloids Surf. B Biointerfaces 2014, 113, 101–106. [Google Scholar] [CrossRef]
- Onak, G.; Şen, M.; Horzum, N.; Ercan, U.K.; Yaralı, Z.B.; Garipcan, B.; Karaman, O. Aspartic and Glutamic Acid Templated Peptides Conjugation on Plasma Modified Nanofibers for Osteogenic Differentiation of Human Mesenchymal Stem Cells: A Comparative Study. Sci. Rep. 2018, 8, 17620. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Paletta, J.R.; Bockelmann, S.; Walz, A.; Theisen, C.; Wendorff, J.H.; Greiner, A.; Fuchs-Winkelmann, S.; Schofer, M.D. RGD-functionalisation of PLLA nanofibers by surface coupling using plasma treatment: Influence on stem cell differentiation. J. Mater. Sci. Mater. Electron. 2009, 21, 1363–1369. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.; Park, H.; Jung, D.; Kim, S. Protein immobilization on plasma-polymerized ethylene diamine-coated glass slides. Anal. Biochem. 2003, 313, 41–45. [Google Scholar] [CrossRef]
- Birhanu, G.; Javar, H.A.; Seyedjafari, E.; Zandi-Karimi, A.; Telgerd, M.D. An improved surfacefor enhanced stem cell proliferation and osteogenic differentiation using electrospun composite PLLA/P123 scaffold. Artif. Cells Nanomed. Biotechnol. 2017, 46, 1274–1281. [Google Scholar] [CrossRef]
- Wang, M.; Zhou, Y.; Shi, D.; Chang, R.; Zhang, J.; Keidar, M.; Webster, T.J. Cold atmospheric plasma (CAP)-modified and bioactive protein-loaded core–shell nanofibers for bone tissue engineering applications. Biomater. Sci. 2019, 7, 2430–2439. [Google Scholar] [CrossRef]
- Meghdadi, M.; Pezeshki-Modaress, M.; Irani, S.; Atyabi, S.M.; Zandi, M. Chondroitin sulfate immobilized PCL nanofibers enhance chondrogenic differentiation of mesenchymal stem cells. Int. J. Biol. Macromol. 2019, 136, 616–624. [Google Scholar] [CrossRef]
- Ghobeira, R.; Philips, C.; De Naeyer, V.; Declercq, H.; Cools, P.; De Geyter, N.; Cornelissen, R.; Morent, R. Comparative study of the surface properties and cytocompatibility of plasma-treated poly-ε-caprolactone nanofibers subjected to different sterilization methods. J. Biomed. Nanotechnol. 2017, 13, 699–716. [Google Scholar] [CrossRef]
- De Valence, S.; Tille, J.-C.; Chaabane, C.; Gurny, R.; Bochaton-Piallat, M.-L.; Walpoth, B.; Möller, M. Plasma treatment for improving cell biocompatibility of a biodegradable polymer scaffold for vascular graft applications. Eur. J. Pharm. Biopharm. 2013, 85, 78–86. [Google Scholar] [CrossRef]
- Ardeshirylajimi, A.; Dinarvand, P.; Seyedjafari, E.; Langroudi, L.; Adegani, F.J.; Soleimani, M. Enhanced reconstruction of rat calvarial defects achieved by plasma-treated electrospun scaffolds and induced pluripotent stem cells. Cell Tissue Res. 2013, 354, 849. [Google Scholar] [CrossRef]
- Correia, C.R.; Gaifem, J.; Oliveira, M.B.; Silvestre, R.; Mano, J.F. The influence of surface modified poly(l-lactic acid) films on the differentiation of human monocytes into macrophages. Biomater. Sci. 2017, 5, 551–560. [Google Scholar] [CrossRef]
- Alves, N.M.; Pashkuleva, I.; Reis, R.L.; Mano, J.F. Controlling cell behavior through the design of polymer surfaces. Small 2010, 6, 2208–2220. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Asadian, M.; Onyshchenko, I.; Thukkaram, M.; Tabaei, P.S.E.; van Guyse, J.; Cools, P.; Declercq, H.; Hoogenboom, R.; Morent, R.; de Geyter, N. Effects of a dielectric barrier discharge (DBD) treatment on chitosan/polyethylene oxide nanofibers and their cellular interactions. Carbohydr. Polym. 2018, 201, 402–415. [Google Scholar] [CrossRef] [PubMed]
- Baek, H.S.; Park, Y.H.; Ki, C.S.; Park, J.-C.; Rah, D.K. Enhanced chondrogenic responses of articular chondrocytes onto porous silk fibroin scaffolds treated with microwave-induced argon plasma. Surf. Coat. Technol. 2008, 202, 5794–5797. [Google Scholar] [CrossRef]
- Lee, K.Y.; Lee, S.J.; Park, K.E.; Park, W.H. Plasma-treated poly(lactic-co-glycolicacid) nanofibers for tissue engineering. Macromol. Res. 2007, 15, 238–243. [Google Scholar]
- Cheng, Q.; Lee, B.L.; Komvopoulos, K.; Yan, Z.; Li, S. Plasma surface chemical treatment of electrospun poly(L-lactide) microfibrous scaffolds for enhanced cell adhesion, growth, and infiltration. Tissue Eng. Part A 2013, 19, 1188–1198. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Coad, B.R.; Jasieniak, M.; Griesser, S.S.; Griesser, H.J. Controlled covalent surface immobilization of proteins and peptides using plasma methods. Surf. Coat. Technol. 2013, 233, 169–177. [Google Scholar] [CrossRef]
- Rajabi, M.; Firouzi, M.; Hassannejad, Z.; Haririan, I.; Zahedi, P. Fabrication and characterization of electrospun laminin-functionalized silk fibroin/poly (ethylene oxide) nanofibrous scaffolds for peripheral nerve regeneration. J. Biomed. Mater. Res. Part B Appl. Biomater. 2017, 106, 1595–1604. [Google Scholar] [CrossRef]
- Cardoso, V.F.; Botelho, G.; Lanceros-Méndez, S. Nonsolvent induced phase separation preparation of poly (vinylidene fluoride-co-chlorotrifluoroethylene) membranes with tailored morphology, piezoelectric phase content and mechanical properties. Mater. Des. 2015, 88, 390–397. [Google Scholar] [CrossRef]
- Lloyd, D.R.; Kim, S.S.; Kinzer, K.E. Microporous membrane formation via thermally-induced phase separation. II. Liquid—liquid phase separation. J. Membr. Sci. 1991, 64, 1–11. [Google Scholar] [CrossRef]
- Guillen, G.R.; Pan, Y.; Li, M.; Hoek, E.M.V. Preparation and Characterization of Membranes Formed by Nonsolvent Induced Phase Separation: A Review. Ind. Eng. Chem. Res. 2011, 50, 3798–3817. [Google Scholar] [CrossRef]
- Ma, P.X.; Zhang, R. Synthetic nano-scale fibrous extracellular matrix. J. Biomed. Mater. Res. 1999, 46, 60–72. [Google Scholar] [CrossRef] [Green Version]
- Smith, L.A.; Liu, X.; Ma, P.X. Tissue engineering with nano-fibrous scaffolds. Soft Matter 2008, 4, 2144–2149. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Akbarzadeh, R.; Yousefi, A.-M. Effects of processing parameters in thermally induced phase separation technique on porous architecture of scaffolds for bone tissue engineering. J. Biomed. Mater. Res. Part B Appl. Biomater. 2014, 102, 1304–1315. [Google Scholar] [CrossRef] [PubMed]
- Da, H.; Jia, S.-J.; Meng, G.-L.; Cheng, J.-H.; Zhou, W.; Xiong, Z.; Mu, Y.-J.; Liu, J. The impact of compact layer in biphasic scaffold on osteochondral tissue engineering. PLoS ONE 2013, 8, e54838. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Xu, N.; Ye, X.; Wei, D.; Zhong, J.; Chen, Y.; Xu, G.; He, D. 3D artificial bones for bone repair prepared by computed tomography-guided fused deposition modeling for bone repair. ACS Appl. Mater. Interfaces 2014, 6, 14952–14963. [Google Scholar] [CrossRef]
- Yuan, B.; Zhou, S.-Y.; Chen, X.-S. Rapid prototyping technology and its application in bone tissue engineering. J. Zhejiang Univ. Sci. B 2017, 18, 303–315. [Google Scholar] [CrossRef] [Green Version]
- Wang, X.; Jiang, M.; Zhou, Z.; Gou, J.; Hui, D. 3D printing of polymer matrix composites: A review and prospective. Compos. Part B Eng. 2017, 110, 442–458. [Google Scholar] [CrossRef]
- Thavornyutikarn, B.; Chantarapanich, N.; Sitthiseripratip, K.; Thouas, G.A.; Chen, Q. Bone tissue engineering scaffolding: Computer-aided scaffolding techniques. Prog. Biomater. 2014, 3, 61–102. [Google Scholar] [CrossRef] [Green Version]
- Chia, H.N.; Wu, B.M. Recent advances in 3D printing of biomaterials. J. Biol. Eng. 2015, 9, 4. [Google Scholar] [CrossRef] [Green Version]
- Mazzoli, A.; Ferretti, C.; Gigante, A.; Salvolini, E.; Mattioli-Belmonte, M. Selective laser sintering manufacturing of polycaprolactone bone scaffolds for applications in bone tissue engineering. Rapid. Prototyp. J. 2015, 21, 386–392. [Google Scholar] [CrossRef]
- Bai, J.; Goodridge, R.D.; Yuan, S.; Zhou, K.; Chua, C.K.; Wei, J. Thermal influence of CNT on the polyamide 12 nanocomposite for selective laser sintering. Molecules 2015, 20, 19041–19050. [Google Scholar] [CrossRef] [PubMed]
- Mazzoli, A. Selective laser sintering in biomedical engineering. Med. Biol. Eng. Comput. 2013, 51, 245–256. [Google Scholar] [CrossRef] [PubMed]
- Mondschein, R.J.; Kanitkar, A.; Williams, C.B.; Verbridge, S.S.; Long, T.E. Polymer structure-property requirements for stereolithographic 3D printing of soft tissue engineering scaffolds. Biomaterials 2017, 140, 170–188. [Google Scholar] [CrossRef] [PubMed]
- Wang, M.O.; Vorwald, C.E.; Dreher, M.L.; Mott, E.J.; Cheng, M.-H.; Cinar, A.; Mehdizadeh, H.; Somo, S.; Dean, D.; Brey, E.M.; et al. Evaluating 3D-Printed Biomaterials as Scaffolds for Vascularized Bone Tissue Engineering. Adv. Mater. 2015, 27, 138–144. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ji, K.; Yanen, W.; Wei, Q.; Zhang, K.; Jiang, A.; Rao, Y.; Cai, X. Application of 3D printing technology in bone tissue engineering. Bio-Des. Manuf. 2018, 1, 203–210. [Google Scholar] [CrossRef]
- Colasante, C.; Sanford, Z.; Garfein, E.; Tepper, O. Current trends in 3D printing, bioprosthetics, and tissue engineering in plastic and reconstructive surgery. Curr. Surg. Rep. 2016, 4, 6. [Google Scholar] [CrossRef]
- Cui, X.; Boland, T.; D’Lima, D.D.; Lotz, M.K. Thermal inkjet printing in tissue engineering and regenerative medicine. Recent. Pat. Drug. Deliv. Formul. 2012, 6, 149–155. [Google Scholar] [CrossRef]
- Murphy, S.V.; Atala, A. 3D bioprinting of tissues and organs. Nat. Biotechnol. 2014, 32, 773. [Google Scholar] [CrossRef]
- SKnowlton, S.; Anand, S.; Shah, T.; Tasoglu, S. Bioprinting for neural tissue engineering. Trends Neurosci. 2018, 41, 31–46. [Google Scholar] [CrossRef]
- Ozbolat, I.T.; Hospodiuk, M. Current advances and future perspectives in extrusion-based bioprinting. Biomaterials 2016, 76, 321–343. [Google Scholar] [CrossRef] [Green Version]
- Mandrycky, C.; Wang, Z.; Kim, K.; Kim, D.-H. 3D bioprinting for engineering complex tissues. Biotechnol. Adv. 2016, 34, 422–434. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gruene, M.; Unger, C.; Koch, L.; Deiwick, A.; Chichkov, B.N. Dispensing pico to nanolitre of a natural hydrogel by laser-assisted bioprinting. Biomed. Eng. Online 2011, 10, 19. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pham, Q.P.; Sharma, U.; Mikos, A.G. Electrospinning of polymeric nanofibers for tissue engineering applications: A review. Tissue Eng. 2006, 12, 1197–1211. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Braghirolli, D.I.; Steffens, D.; Pranke, P. Electrospinning for regenerative medicine: A review of the main topics. Drug Discov. Today 2014, 19, 743–753. [Google Scholar] [CrossRef] [PubMed]
- Barker, T. The role of ECM proteins and protein fragments in guiding cell behavior in regenerative medicine. Biomaterials 2011, 32, 4211–4214. [Google Scholar] [CrossRef] [PubMed]
- Schlie-Wolter, S.; Ngezahayo, A.; Chichkov, B.N. The selective role of ECM components on cell adhesion, morphology, proliferation and communication in vitro. Exp. Cell Res. 2013, 319, 1553–1561. [Google Scholar] [CrossRef]
- Alenghat, F.J.; Ingber, D.E. Mechanotransduction: All signals point to cytoskeleton, matrix, and integrins. Sci. Signal. 2002, 2002, 6. [Google Scholar] [CrossRef]
- Aviss, K.J.; Gough, J.E.; Downes, S. Aligned electrospun polymer fibres for skeletal muscle regeneration. Eur. Cell. Mater. 2010, 19, 193–204. [Google Scholar] [CrossRef]
- Townsend-Nicholson, A.; Jayasinghe, S.N. Cell Electrospinning: A Unique Biotechnique for Encapsulating Living Organisms for Generating Active Biological Microthreads/Scaffolds. Biomacromolecules 2006, 7, 3364–3369. [Google Scholar] [CrossRef]
- Jayasinghe, S. Cell electrospinning: A novel tool for functionalising fibres, scaffolds and membranes with living cells and other advanced materials for regenerative biology and medicine. Analyst 2013, 138, 2215–2223. [Google Scholar] [CrossRef]
- Sampson, S.L.; Saraiva, L.; Gustafsson, K.; Jayasinghe, S.N.; Robertson, B.D. Cell electrospinning: An in vitro and in vivo study. Small 2014, 10, 78–82. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chen, H.; Liu, Y.; Hu, Q. A novel bioactive membrane by cell electrospinning. Exp. Cell Res. 2015, 338, 261–266. [Google Scholar] [CrossRef] [PubMed]
- Kitsara, M.; Agbulut, O.; Kontziampasis, D.; Chen, Y.; Menasché, P. Fibers for hearts: A critical review on electrospinning for cardiac tissue engineering. Acta Biomater 2017, 48, 20–40. [Google Scholar] [CrossRef] [PubMed]
- Zimmermann, W.-H.; Didié, M.; Döker, S.; Melnychenko, I.; Naito, H.; Rogge, C.; Tiburcy, M.; Eschenhagen, T. Heart muscle engineering: An update on cardiac muscle replacement therapy. Cardiovasc. Res. 2006, 71, 419–429. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bach, A.D.; Beier, J.P.; Stern-Staeter, J.; Horch, R.E. Skeletal muscle tissue engineering. J. Cell. Mol. Med. 2004, 8, 413–422. [Google Scholar] [CrossRef] [PubMed]
- Chamley-Campbell, J.; Campbell, G.R.; Ross, R. The smooth muscle cell in culture. Physiol. Rev. 1979, 59, 1–61. [Google Scholar] [CrossRef] [PubMed]
- Yeo, M.; Kim, G.H. Anisotropically aligned cell-laden nanofibrous bundle fabricated via cell electrospinning to regenerate skeletal muscle tissue. Small 2018, 14, 1803491. [Google Scholar] [CrossRef]
- Hong, J.; Yeo, M.; Yang, G.H.; Kim, G. Cell-electrospinning and its application for tissue engineering. Int. J. Mol. Sci. 2019, 20, 6208. [Google Scholar] [CrossRef] [Green Version]
- Ladd, M.R.; Lee, S.J.; Stitzel, J.D.; Atala, A.; Yoo, J.J. Co-electrospun dual scaffolding system with potential for muscle–tendon junction tissue engineering. Biomaterials 2011, 32, 1549–1559. [Google Scholar] [CrossRef]
- McKeon-Fischer, K.D.; Freeman, J.W. Characterization of electrospun poly (l-lactide) and gold nanoparticle composite scaffolds for skeletal muscle tissue engineering. J. Tissue Eng. Regen. Med. 2010, 5, 560–568. [Google Scholar] [CrossRef]
- Ma, J.; Holden, K.; Zhu, J.; Pan, H.; Li, Y. The application of collagen-scaffolds seeded with myoblasts to repair skeletal muscle defects. J. Biomed. Biotechnol. 2011, 2011, 812135. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sell, S.A.; McClure, M.J.; Garg, K.; Wolfe, P.S.; Bowlin, G.L. Electrospinning of collagen and elastin for tissue engineering applications. Biomaterials 2006, 27, 724–734. [Google Scholar]
- Ku, S.H.; Lee, S.H.; Park, C.B. Synergic effects of nanofiber alignment and electroactivity on myoblast differentiation. Biomaterials 2012, 33, 6098–6104. [Google Scholar] [CrossRef] [PubMed]
- Abarzúa-Illanes, P.N.; Padilla, C.; Ramos, A.; Isaacs, M.; Ramos-Grez, J.; Olguín, H.C.; Valenzuela, L.M. Improving myoblast differentiation on electrospun poly (epsilon-caprolactone) scaffolds. J. Biomed. Mater. Res. A 2017, 105, 2241–2251. [Google Scholar] [CrossRef]
- De Torre, I.G.; Ibañez-Fonseca, A.; Quintanilla, L.; Alonso, M.; Rodriguez-Cabello, C. Random and oriented electrospun fibers based on a multicomponent, in situ clickable elastin-like recombinamer system for dermal tissue engineering. Acta Biomater. 2018, 72, 137–149. [Google Scholar] [CrossRef] [Green Version]
- Haider, A.; Haider, S.; Kang, I.-K. A comprehensive review summarizing the effect of electrospinning parameters and potential applications of nanofibers in biomedical and biotechnology. Arab. J. Chem. 2015, 11, 1165–1188. [Google Scholar] [CrossRef]
- Tzezana, R.; Zussman, E.; Levenberg, S. A layered ultra-porous scaffold for tissue engineering, created via a hydrospinning method. Tissue Eng. Part C Methods 2008, 14, 281–288. [Google Scholar] [CrossRef] [Green Version]
- Fonseca, D.; Sobreiro-Almeida, R.; Sol, P.C.; Neves, N.M. Development of non-orthogonal 3D-printed scaffolds to enhance their osteogenic performance. Biomater. Sci. 2018, 6, 1569–1579. [Google Scholar] [CrossRef]
- Oliveira, A.; Sampaio, S.; Sousa, R.; Reis, R. Controlled mineralization of nature-inspired silk fibroin/hydroxyapatite hybrid bioactive scafolds for bone tissue engineering applications. In Proceedings of the 20th European Conference on Biomaterials, Nantes, France, 27 September–1 October 2006. [Google Scholar]
- Wenz, A.; Borchers, K.; Tovar, G.E.M.; Kluger, P.J. Bone matrix production in hydroxyapatite-modified hydrogels suitable for bone bioprinting. Biofabrication 2017, 9, 044103. [Google Scholar] [CrossRef]
- Lee, H.; Yang, G.H.; Kim, M.; Lee, J.; Kim, J.H.G. Fabrication of micro/nanoporous collagen/dECM/silk-fibroin biocomposite scaffolds using a low temperature 3D printing process for bone tissue regeneration. Mater. Sci. Eng. C 2018, 84, 140–147. [Google Scholar] [CrossRef]
- Kim, W.J.; Yun, H.-S.; Kim, G.H. An innovative cell-ladenα-TCP/collagen scaffold fabricated using a two-step printing process for potential application in regenerating hard tissues. Sci. Rep. 2017, 7, 3181. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yang, X.; Lu, Z.; Wu, H.; Li, W.; Zheng, L.; Zhao, J. Collagen-alginate as bioink for three-dimensional(3D) cell printing based cartilage tissue engineering. Mater. Sci. Eng. C 2018, 83, 195–201. [Google Scholar] [CrossRef] [PubMed]
- Shen, T.; Dai, Y.; Li, X.; Xu, S.; Gou, Z.; Gao, C. Regeneration of the Osteochondral Defect by a Wollastonite and Macroporous Fibrin Biphasic Scaffold. ACS Biomater. Sci. Eng. 2017, 4, 1942–1953. [Google Scholar] [CrossRef] [PubMed]
- Wu, Y.-H.A.; Chiu, Y.-C.; Lin, Y.-H.; Ho, C.-C.; Shie, M.-Y.; Chen, Y.-W. 3D-printed bioactive calcium silicate/poly-epsilon-caprolactone bioscaffolds modified with biomimetic extracellular matrices for bone regeneration. Int. J. Mol. Sci. 2019, 20, 942. [Google Scholar] [CrossRef] [Green Version]
- Kim, J.-Y.; Ahn, G.; Kim, C.; Lee, J.-S.; Lee, I.-G.; An, S.-H.; Yun, W.-S.; Kim, S.-Y.; Shim, J.-H. Synergistic effectsof beta tri-calcium phosphate and porcine-derived decellularized bone extracellular matrix in 3D-printed polycaprolactone scaffold on bone regeneration. Macromol. Biosci. 2018, 18, 10. [Google Scholar] [CrossRef]
- Heidari, M.; Bahrami, S.H.; Ranjbar-Mohammadi, M.; Milan, P.B. Smart electrospun nanofibers containing PCL/gelatin/graphene oxide for application in nerve tissue engineering. Mater. Sci. Eng. 2018, 103, 109768. [Google Scholar] [CrossRef]
- Sharif, S.; Ai, J.; Azami, M.; Verdi, J.; Atlasi, M.A.; Shirian, S.; Samadikuchaksaraei, A. Collagen-coated nano-electrospun PCL seeded with human endometrial stem cells for skin tissue engineering applications. J. Biomed. Mater. Res. Part B Appl. Biomater. 2018, 106, 1578–1586. [Google Scholar] [CrossRef]
- Kouhi, M.; Fathi, M.; Reddy, V.J.; Ramakrishna, S. bredigite reinforced electrospun nanofibers for bone tissue engineering. Mater. Today Proc. 2019, 7, 449–454. [Google Scholar] [CrossRef]
- Lee, S.; Joshi, M.K.; Tiwari, A.P.; Maharjan, B.; Kim, K.S.; Yun, Y.-H.; Park, C.H.; Kim, C.S. Lactic acid assisted fabrication of bioactive three-dimensional PLLA/beta-TCP fibrous scaffold for biomedical application. Chem. Eng. J. 2018, 347, 771–781. [Google Scholar] [CrossRef]
- Gao, Q.; Gua, H.; Zhao, P.; Zhang, C.; Cao, M.; Fu, J.; He, Y. Fabrication of electrospun nanofibrous scaffolds with 3D controllable geometric shapes. Mater. Des. 2018, 157, 159–169. [Google Scholar] [CrossRef]
- Garcia, A.G.; Hébraud, A.; Duval, J.-L.; Wittmer, C.R.; Gaut, L.; Duprez, D.; Egles, C.; Bedoui, F.; Schlatter, G.; Legallais, C. Poly (epsilon-caprolactone)/hydroxyapatite 3d honeycomb scaffolds for a cellular microenvironment adapted to maxillofacial bone reconstruction. ACS Biomater. Sci. Eng. 2018, 4, 3317–3326. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zadehnajar, P.; Akbari, B.; Karbasi, S.; Mirmusavi, M.H. Preparation and characterization of poly ε-caprolactone-gelatin/multi-walled carbon nanotubes electrospun scaffolds for cartilage tissue engineering applications. Int. J. Polym. Mater. 2019, 69, 326–337. [Google Scholar] [CrossRef]
- Vunjak-Novakovic, G.; Martin, I.; Obradovic, B.; Treppo, S.; Grodzinsky, A.J.; Langer, R.; Freed, L.E. Bioreactorcultivation conditions modulate the composition and mechanical properties of tissue-engineered cartilage. J. Orthop. Res. 1999, 17, 130–138. [Google Scholar] [CrossRef] [PubMed]
- Meredith, J.C.; Sormana, J.-L.; Keselowsky, B.G.; García, A.J.; Tona, A.; Karim, A.; Amis, E.J. Combinatorial characteri-zation of cell interactions with polymer surfaces. J. Biomed. Mater. Res. A 2003, 66, 483–490. [Google Scholar] [CrossRef] [PubMed]
- Yoon, D.M.; Fisher, J.P. Chondrocyte signaling and artificial matrices for articular cartilage engi-neering. Adv. Exp. Med. Biol. 2006, 585, 67–86. [Google Scholar] [PubMed]
- Barbero, A.; Grogan, S.P.; Mainil-Varlet, P.; Martin, I. Expansion on specific substrates regulates the phenotype and differentiation capacity of human articular chondrocytes. J. Cell Biochem. 2006, 98, 1140–1149. [Google Scholar] [CrossRef]
- Elder, S.H.; Sanders, S.W.; McCulley, W.R.; Marr, M.L.; Shim, J.W.; Hasty, K.A. Chondrocyte response to cyclic hydrostatic pressure in alginate versus pellet culture. J. Orthop. Res. 2006, 24, 740–747. [Google Scholar] [CrossRef]
- Anderson, J.M. Biological responses to materials. Annu. Rev. Mater. Res. 2001, 31, 81–110. [Google Scholar] [CrossRef]
- Jakab, K.; Norotte, C.; Marga, F.; Murphy, K.; Vunjak-Novakovic, G.; Forgacs, G. Tissue engineering by self-assembly and bio-printing of living cells. Biofabrication 2010, 2, 022001. [Google Scholar] [CrossRef]
- Nishida, K.; Yamato, M.; Hayashida, Y.; Watanabe, K.; Yamamoto, K.; Adachi, E.; Nagai, S.; Kikuchi, A.; Maeda, N.; Watanabe, H.; et al. Corneal reconstruction with tissue-engineered cell sheets composed of autologous oral mucosal epithelium. N. Engl. J. Med. 2004, 351, 1187–1196. [Google Scholar] [CrossRef] [Green Version]
- Nishida, K.; Yamato, M.; Hayashida, Y.; Watanabe, K.; Maeda, N.; Watanabe, H.; Yamamoto, K.; Nagai, S.; Kikuchi, A.; Tano, Y.; et al. Functional bioengineered corneal epithelial sheet grafts from corneal stem cells expanded ex vivo on a temperature-responsive cell vivo on a temperature-responsive cell culture surface. Transplantation 2004, 77, 379–385. [Google Scholar] [CrossRef] [PubMed]
- Pérez-Pomares, J.M.; Foty, R.A. Tissue fusion and cell sorting in embryonic development and disease: Biomedical implications. Bioessays 2006, 28, 809–821. [Google Scholar] [CrossRef] [PubMed]
- Shimizu, T.; Sekine, H.; Yang, J.; Isoi, Y.; Yamato, M.; Kikuchi, A.; Kobayashi, E.; Okano, T. Polysurgery of cell sheet grafts overcomes diffusion limits to produce thick, vascularized myocardial tissues. FASEB J. 2006, 20, 708–710. [Google Scholar] [CrossRef] [PubMed]
- Ong, S.-Y.; Dai, H.; Leong, K.W. Inducing hepatic differentiation of human mesenchymal stem cells in pellet culture. Biomaterials 2006, 27, 4087–4097. [Google Scholar] [CrossRef] [PubMed]
- Diekman, B.O.; Christoforou, N.; Willard, V.P.; Sun, H.; Sanchez-Adams, J.; Leong, K.W.; Guilak, F. Cartilage tissue engineering using differentiated and purified induced pluripotent stem cells. Proc. Natl. Acad. Sci. USA 2012, 109, 19172–19177. [Google Scholar] [CrossRef] [Green Version]
- Murphy, M.K.; Masters, T.E.; Hu, J.C.; Athanasiou, K.A. Engineering a fibrocartilage spectrum through modulation of aggregate redifferentiation. Cell Transpl. 2013, 24, 235–245. [Google Scholar] [CrossRef] [Green Version]
- Bhumiratana, S.; Eton, R.E.; Oungoulian, S.R.; Wan, L.Q.; Ateshian, G.A.; Vunjak-Novakovic, G. Large, stratified, and mechanically functional human cartilage grown in vitro by mesenchymal condensation. Proc. Natl. Acad. Sci. USA 2014, 11, 6940–6945. [Google Scholar] [CrossRef] [Green Version]
- Syed-Picard, F.N.; Larkin, L.M.; Shaw, C.M.; Arruda, E.M. Three-dimensional engineered bone from bone marrow stromal cells and their autogenous extracellular matrix. Tissue Eng. Part A 2009, 15, 187–195. [Google Scholar] [CrossRef] [Green Version]
- Pirraco, R.P.; Obokata, H.; Iwata, T.; Marques, A.P.; Tsuneda, S.; Yamato, M.; Reis, R.L.; Okano, T. Development of osteogenic cell sheets for bone tissue engineering applications. Tissue Eng. Part A 2009, 17, 1507–1515. [Google Scholar] [CrossRef] [Green Version]
- Donnelly, K.; Khodabukus, A.; Philp, A.; Deldicque, L.; Dennis, R.G.; Baar, K. A novel bioreactor for stimulating skeletal muscle in vitro. Tissue Eng. Part C Methods 2010, 16, 711–718. [Google Scholar] [CrossRef]
- Athanasiou, K.A.; Eswaramoorthy, R.; Hadidi, P.; Hu, J.C. Self-organization and the self-assembling process in tissue engineering. Annu. Rev. Biomed. Eng. 2013, 15, 115–136. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hu, J.C.; Athanasiou, K.A. A self-assembling process in articular cartilage tissue engineering. Tissue Eng. 2006, 12, 969–979. [Google Scholar] [CrossRef] [PubMed]
- Williams, M.L.; Kostrominova, T.Y.; Arruda, E.M.; Larkin, L.M. Effect of implantation on engineered skeletal muscle constructs. J. Tissue Eng. Regen. Med. 2013, 7, 434–442. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dennis, R.G.; Kosnik, P.E., 2nd. Excitability and isometric contractile properties of mammalian skeletal muscle constructs engineered in vitro. In Vitro Cell. Dev. Biol. Anim. 2000, 36, 1–10. [Google Scholar] [CrossRef]
- Carosio, S.; Barberi, L.; Rizzuto, E.; Nicoletti, C.; del Prete, Z.; Musarò, A. Generation of ex vivo-vascularized muscle engineered tissue (X-MET). Sci. Rep. 2013, 3, 1420. [Google Scholar] [CrossRef]
- Zhang, B.; Yang, S.; Sun, Z.; Zhang, Y.; Xia, T.; Xu, W.; Ye, S. Human mesenchymal stem cells induced by growth differentiation factor 5: An improved self-assembly tissue engineering method for cartilage repair. Tissue Eng. Part C Methods 2011, 17, 1189–1199. [Google Scholar] [CrossRef]
- Gálvez, P.; Clares, B.; Hmadcha, A.; Ruiz, A.; Soria, B. Development of a cell-based medicinal product: Regulatory structures in the European Union. Br. Med. Bull. 2012, 105, 85. [Google Scholar] [CrossRef] [Green Version]
- Oberweis, C.V.; Marchal, J.A.; López-Ruiz, E.; Gálvez-Martín, P. A worldwide overview of regulatory frameworks for tissue-based products. Tissue Eng. Part B Rev. 2020, 26, 181–196. [Google Scholar] [CrossRef] [Green Version]

| Technique | Advantages | Disadvantages |
|---|---|---|
| Phase separation |
|
|
| 3D printing |
|
|
| Electrospinning |
|
|
| Advantages and Disadvantages | Electrospinning | Cell-Electrospinning |
|---|---|---|
| Advantages |
|
|
| Disadvantages |
|
|
| Technology | Materials | Cells/Growth Factors | Outcomes | Application | References |
|---|---|---|---|---|---|
| 3D bioprinting | Polycaprolactone (PCL) | Saos-2 cell seeding | positive influence on the biological performance of the cells; higher values for the mineralization, activity of osteogenic-related genes, and deposition of the mineralized matrix. | Bone tissue engineering | [160] |
| Alginate/alginate-sulfate | MC3T3-E1 cells/BMP-2 | Alginate/alginate sulfate bioinks allowed good 3D cell printing. Improvement of the release of BMP-2 was achieved using alginate sulfate. Proliferation and differentiation of the printed osteoblasts were enhanced | Bone tissue engineering | [161] | |
| GelMA and methacrylated hyaluronic acid (HA) modified with HAp | hASCs | Positive effects on bone matrix production and remodelling | Bone tissue engineering | [162] | |
| Collagen/dECM/silk fibroin (SF) | MC3T3-E1 cells | High compressive modulus mainly due to the methanol-treated SF; high cellular activities in in vitro tests using MC3T3-E1 cells, induced by Collagen and dECM. | Bone tissue engineering | [163] | |
| α-TCP/collagen | MC3T3-E1 cells | The scaffold showed good mechanical properties and cellular activities | Bone tissue engineering | [164] | |
| collagen type I/agarose with sodium alginate | Primary chondrocytes | Addition of collagen or agarose had an impact on gelling behavior and improving mechanical strength. The collagen facilitated cell adhesion, accelerated cell proliferation, and enhanced the expression of cartilage-specific genes, (Acan, Sox9, and Col2a1) | Bone tissue engineering | [165] | |
| Fibrin and wollastonite | Loaded with rabbit BMSCs | Possible extensive regeneration of both cartilage and subchondral bone induced by in vivo transplantation of the scaffolds | Osteochondral tissue | [166] | |
| CS/PCL | dECM coating/WJMSCs seeding | Improved osteogenic differentiation in vitro and bone regenerative potential in vivo | Bone | [167] | |
| PCL/β-TCP | dECM coating/MC3T3-E1 seeding | Improved osteogenic differentiation in vitro and bone regenerative potential in vivo | Bone | [168] | |
| Electrospinning | Graphene-incorporated electrospun PCL/gelatin | PC12 cells | Good cell attachment and proliferation | Nerve tissue engineering | [169] |
| PCL/collagen | Human endometrial stem cells seeding | Good cell attachment and proliferation Higher wettability, attachment, and proliferation rates of hEnSCs on the PCL/collagen scaffold | Skin | [170] | |
| Polyhydroxybutyrate-co-hydroxyvaletare (PHBV) containing bredigite | - | Bredigite nanoparticles increased the mechanical properties, biodegradability, and bioactivity of the scaffolds | Bone tissue | [171] | |
| PLLA/β-TCP | hMSCs seeding | Enhanced water uptake ability, in vitro bio-mineralization, and bioactivity promoted by the incorporation of β-TCP | Bone | [172] | |
| Electrospinning combined with 3D bioprinting | PCL | Laden with L929 mouse fibroblasts | Multi-layered structures—3D scaffolds—with loosely packed nanofibers, with better surface wettability (when compared to the 2D scaffolds) | Not defined | [173] |
| Electrospinning electro-spraying | PCL/HAp | Murine embryonic cell seeding | High capacity to guide the migration of differentiated bone cells throughout the cavities and the ridge of the scaffolds | Bone regeneration | [174] |
| PCL/gelatin and multi-walled carbon nanotubes (MWNTs) | Adult rabbit chondrocytes seeding | Increased hydrophilicity and tensile strength, and higher bioactivity and slower degradation rate due to presence of MWNTs; 99% antibacterial properties against gram-positive and gram-negative bacteria. | Cartilage tissue | [175] | |
| Phase separation process | Cartilage ECM-derived/PLGA-β-TCP-collagen type I | BMSCs seeding | Enhanced OC regeneration. Chondro and osteogenic-induced BMSCs with independent environments | Osteochondral tissue | [116] |
| Name (MA Holder) | Therapeutic Indication | Jurisdiction |
|---|---|---|
| Spherox (CO. DON AG) | Articular cartilage defects of the femoral condyle and the patella of the knee up to 10 cm2 | European Union |
| MACI (Vericel Denmark ApS.) | Full-thickness cartilage defects of the knee of 3–20 cm2 | European Union |
| CHONDROCELECT (TiGenix N.V.) | Cartilage defects of the femoral condyle of the knee of 1–5 cm2. | European Union |
| Holoclar (Holostem Terapie Avanzate S.R.L) | Moderate to severe limbal stem cell deficiency due to physical or chemical ocular burns. | European Union |
| MACI (Vericel Denmark ApS) | Full-thickness cartilage defects of the knee with or without bone involvement in adults. | Unied States of America |
| GINTUIT (Organogenesis, Inc.) | Topical treatment for vascular wound bed postsurgery with mucogingival conditions in adults | United States of America |
| Carticel (Vericel Denmark ApS) | Cartilage defects of the femoral condyle, in patients who have had an inadequate response to a prior surgical repair procedure | United States of America |
| HeartSheet (TerumoCorporation, Ltd.) | Severe heart failure | Japan |
| JACC (Japan Tissue Engineering Co., Ltd.) | Osteochondritis and traumatic cartilage defects | Japan |
| JACE (Japan Tissue Engineering Co., Ltd.) | Treatment for severe burns Giant congenital melanocytic nevus Dystrophic and junctional epidermolysis bullosa | Japan |
| Kaloderm (Tego Science, Inc.) | Second-degree burn Diabetic foot ulcer | South Korea |
| Holoderm (Tego Science, Inc.) | Second- and third-degree burns | South Korea |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bove, M.; Carlucci, A.; Natale, G.; Freda, C.; Noro, A.; Ferrara, V.; Opromolla, G.; Martone, M.; Cascone, R.; Messina, G.; et al. Tissue Engineering in Musculoskeletal Tissue: A Review of the Literature. Surgeries 2021, 2, 58-82. https://0-doi-org.brum.beds.ac.uk/10.3390/surgeries2010005
Bove M, Carlucci A, Natale G, Freda C, Noro A, Ferrara V, Opromolla G, Martone M, Cascone R, Messina G, et al. Tissue Engineering in Musculoskeletal Tissue: A Review of the Literature. Surgeries. 2021; 2(1):58-82. https://0-doi-org.brum.beds.ac.uk/10.3390/surgeries2010005
Chicago/Turabian StyleBove, Mary, Annalisa Carlucci, Giovanni Natale, Chiara Freda, Antonio Noro, Vincenzo Ferrara, Giorgia Opromolla, Mario Martone, Roberto Cascone, Gaetana Messina, and et al. 2021. "Tissue Engineering in Musculoskeletal Tissue: A Review of the Literature" Surgeries 2, no. 1: 58-82. https://0-doi-org.brum.beds.ac.uk/10.3390/surgeries2010005





