Management of Leishmaniases in the Era of Climate Change in Morocco
Abstract
:1. Introduction
2. Climate Change in Morocco
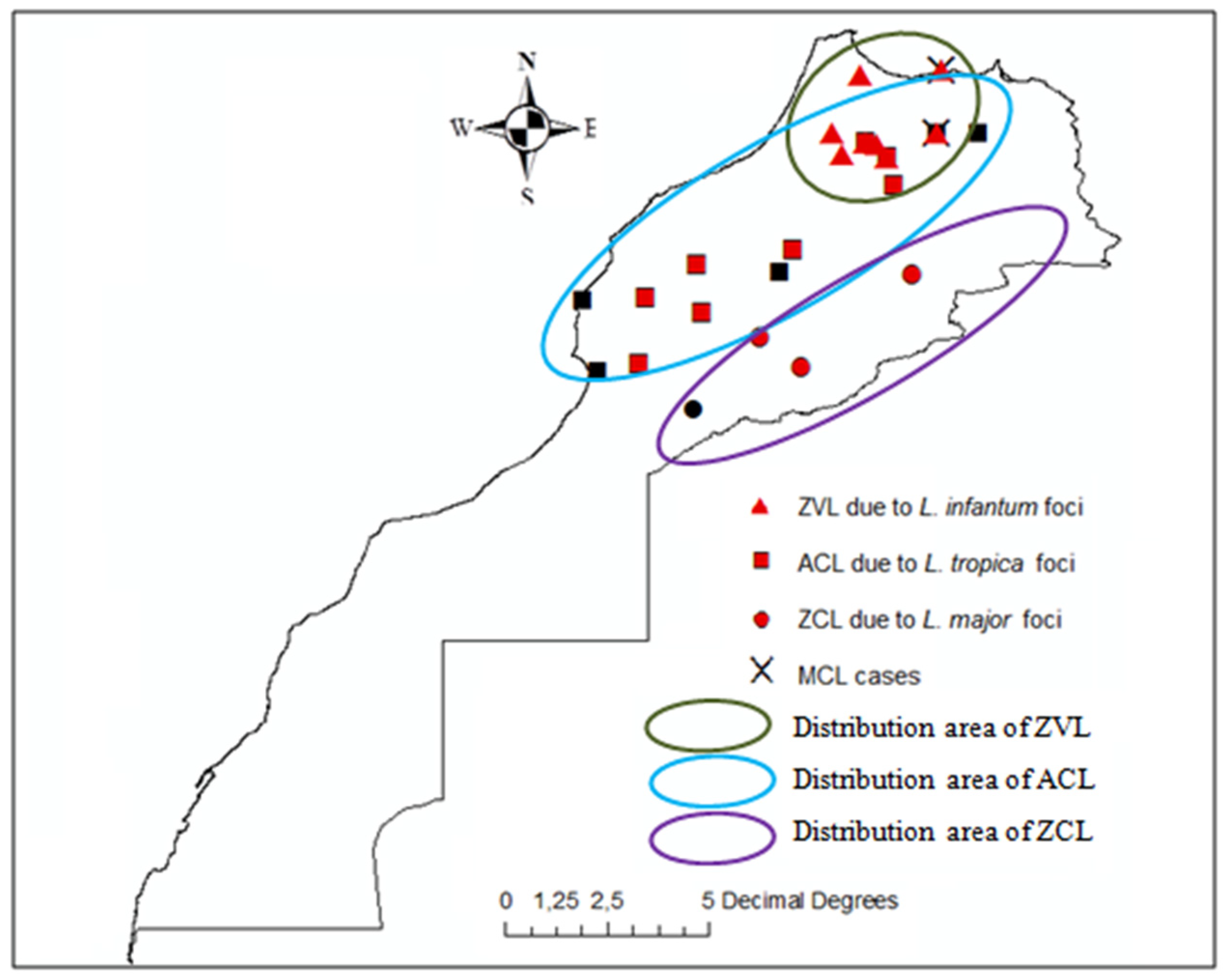
3. Leishmaniases Epidemiology in Morocco: What Is Known and What Can We Anticipate from Climate Change
4. Managing Leishmaniases in Morocco in the Era of Climate Change: A Puzzling Problem
Author Contributions
Funding
Conflicts of Interest
References
- Akhoundi, M.; Downing, T.; Votýpka, J.; Kuhls, K.; Lukeš, J.; Cannet, A.; Ravel, C.; Marty, P.; Delaunay, P.; Kasbari, M.; et al. Leishmania infections: Molecular targets and diagnosis. Mol. Aspects Med. 2017, 57, 1–29. [Google Scholar] [CrossRef] [PubMed]
- Akhoundi, M.; Kuhls, K.; Cannet, A.; Votýpka, J.; Marty, P.; Delaunay, P.; Sereno, D. A Historical Overview of the Classification, Evolution, and Dispersion of Leishmania Parasites and Sandflies. PLoS Negl. Dis. 2016, 10, e0004770. [Google Scholar] [CrossRef] [PubMed]
- Kahime, K.; Boussaa, S.; Bounoua, L.; Ouanaimi, F.; Messouli, M.; Boumezzough, A. Leishmaniasis in Morocco: Diseases and vectors. Asian Pac. J. Trop. Dis. 2014, 4, S530–S534. [Google Scholar] [CrossRef]
- Kahime, K.; Boussaa, S.; Nhammi, H.; Boumezzough, A. Urbanization of human visceral leishmaniasis in Morocco. Parasit. Epidemiol. Control 2017, 2, 16. [Google Scholar] [CrossRef] [PubMed]
- Rioux, J.A.; Petter, F.; Akalay, O.; Lanotte, G.; Ouazani, A.; Seguignes, M.; Mohcine, A. Meriones shawi (Duvernoy, 1842) (Rodentia, Gerbillidae), réservoir de Leishmania major Yakimoff et Shokhor, 1914 dans le Sud Marocain. C. R. Acad Sci III Sci Vie 1982, 294, 515–517. [Google Scholar]
- Guilvard, E.; Rioux, J.A.; Gallego, M.; Pratlong, F.; Mahjour, J.; Martinez-Ortega, E.; Dereure, J.; Saddiki, A.; Martini, A. Leishmania tropica au Maroc III—Rôle de Phlebotomus sergenti. A propos de 89 isolats. Ann. Parasitol. Hum. Comp. 1991, 66, 96–99. [Google Scholar] [CrossRef] [PubMed]
- Echchakery, M.; Boussaa, S.; Kahime, K.; Boumezzough, A. Epidemiological role of a rodent in Morocco: Case of cutaneous leishmaniasis. Asian Pac. J. Trop. Dis. 2015, 5, 589–594. [Google Scholar] [CrossRef]
- Intergovernmental Panel on Climate Change (IPCC) 2014-Fifth Assessment Report—Climate Change: The Synthesis Report: Geneva. Available online: https://www.ipcc.ch/report/ar5/syr/ (accessed on 15 October 2017).
- World Health Organization (WHO). 2015. Leishmaniasis Fact Sheet No 375. Updated February 2015. Available online: http://www.who.int/mediacentre/factsheets/fs375/en/ (accessed on 15 October 2017).
- Semenza, J.C.; Menne, B. Climate change and infectious diseases in Europe. Lancet Infect. Dis. 2009, 9, 365–375. [Google Scholar] [CrossRef]
- Yates, T.L.; Mills, J.N.; Parmenter, C.A.; Ksiazek, T.G.; Parmenter, R.R.; Vande Castle, J.R.; Calisher, C.H.; Nichol, S.T.; Abbott, K.D.; Young, J.C.; et al. The ecology and evolutionary history of an emergent disease: Hantavirus pulmonary syndrome. Bioscience 2002, 52, 989–998. [Google Scholar] [CrossRef]
- Toumi, A.; Chlif, S.; Bettaieb, J.; Alaya, N.B.; Boukthir, A.; Ahmadi, Z.E.; Ben Salah, A. Temporal dynamics and impact of climate factors on the cases of zoonotic cutaneous leishmaniasis in central Tunisia. PLoS Negl. Trop. Dis. 2012, 6, e1633. [Google Scholar] [CrossRef] [PubMed]
- Bounoua, L.; Kahime, K.; Houti, L.; Blakey, T.; Ebi, K.L.; Zhang, P.; Imhoff, M.L.; Thome, K.; Dudek, C.; Sahabi, S.A.; et al. Linking Climate to Incidence of Zoonotic Cutaneous Leishmaniasis (L. major) in Pre-Saharan North Africa. Int. J. Environ. Res. Public Health 2013, 10, 3172–3191. [Google Scholar] [CrossRef] [PubMed]
- Kahime, K.; Boussaa, S.; El Mzabi, A.; Boumezzough, A. Spatial relations among environmental factors and phlebotomine sand fly populations (Diptera: Psychodidae) in central and southern Morocco. J Vector Ecol. 2015, 40, 342–354. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Behnassi, M.; Kahime, K.; Boussaa, S.; Messouli, M.; Boumezzough, A. Infectious Diseases and Climate Vulnerability in Morocco: Governance and Adaptation Options. In Examining the Role of Environmental Change on Emerging Infectious Diseases and Pandemics; Bouzid, M., Ed.; IGI Global: Hershey, PA, USA, 2016; pp. 138–162. [Google Scholar]
- Moroccan Ministry of Health. (The CL Data Is Provided by the Directorate of Epidemiology and DiseaseControl). Rabat: Ministry of Health. Available online: http://www.sante.gov.ma/Pages/ADM_Centrale/DELM.aspx (accessed on 25 May 2015).
- World Health Organization (WHO). 2010-Control of the Leishmaniasis: Report of a Meeting of the WHO Expert Committee on the Control of Leishmaniases; World Health Organization Technical Report Series No. 949; WHO: Geneva, Switzerland, March 2010. [Google Scholar]
- Boudrissa, A.; Cherif, K.; Kherrachi, I.; Benbetka, S.; Bouiba, L.; Boubidi, S.C.; Benikhlef, R.; Arrar, L.; Hamrioui, B.; Harrat, Z. Extension de Leishmania major au Nord de l’Algérie. Bull. Soc. Pathol. Exot. 2012, 105, 30–35. [Google Scholar] [CrossRef] [PubMed]
- Salomón, O.D.; Quintana, M.G.; Mastrángelo, A.V.; Fernández, M.S. Leishmaniasis and Climate Change-Case Study: Argentina. J. Trop. Med. 2012, 601242. [Google Scholar] [CrossRef] [PubMed]
- Oshaghi, M.A.; Ravasan, N.M.; Javadian, E.; Rassi, Y.; Sadraei, J.; Enayati, A.A.; Vatandoost, H.; Zare, Z.; Emami, S.N. Application of predictive degree day model for field development of sandfly vectors of visceral leishmaniasis in northwest of Iran. J. Vector. 2009, 46, 247–255. [Google Scholar]
- Ready, P.D. Leishmaniasis emergence and climate change. Rev. Sci. Tech. 2008, 27, 399–412. [Google Scholar] [CrossRef] [PubMed]
- SNC-Second National Communication. Ministère de l’Aménagement du territoire de l’habitat et de l’environnement, Royaume du Maroc. In Second National Communication à la Convention Cadre des Nations Unis sur les CC; SNC-Second National Communication: Rabat, Morocco, 2009. [Google Scholar]
- Born, K.; Fink, A.; Paeth, H. Dry and wet periods in the northwestern Maghreb for present day and future climate conditions. Meterol. Z. 2009, 17, 533–551. [Google Scholar] [CrossRef]
- Kahime, K.; Bounoua, B.; Messouli, M.; Boussaa, S.; Ouanaimi, F.; Boumezzough, A. Evaluation of EcoAdaptation Strategies of Health to Climate change: Case of Zoonotic Cutaneous Leishmaniasis (ZCL) as Vulnerability Indicator in Pre-Saharan region of Morocco. In Environmental Change and Human Security in the Middle East and Africa; Behnassi, M., Mcglade, K., Eds.; Springer: Dordrecht, The Netherlands, 2016; pp. 117–131. [Google Scholar]
- Bailey, F.; Mondragon-Shem, K.; Hotez, P.; Ruiz-Postigo, J.A.; Al-Salem, W.; Acosta-Serrano, Á.; Molyneux, D.H. A new perspective on cutaneous leishmaniasis-Implications for global prevalence and burden of disease estimates. PLoS Negl. Trop. Dis. 2017, 11, e0005739. [Google Scholar] [CrossRef] [PubMed]
- Kahime, K.; Boussaa, S.; Laamrani-El Idrissi, A.; Nhammi, H.; Boumezzough, A. Epidemiological study on acute cutaneous leishmaniasis in Morocco. J. Acute Dis. 2016, 5, 41–45. [Google Scholar] [CrossRef]
- Moroccan Ministry of Health. 2011-Etat D’avancement des Programmes de Lutte Contre les Maladies Parasitaires. Direction de L’épidémiologie et de Lutte Contre les Maladies; Ministère de la Santé, Rabat, Morocco, 2011. Available online: http://www.sante.gov.ma/departements/delm/index-delm.htm (accessed on 15 October 2017).
- Hmamouch, A.; Amarir, F.; Fellah, H.; Karzaz, M.; Bekhti, K.; Rhajaoui, M. 208 Sebti F. Coexistence of Leishmania tropica and Leishmania infantum in Sefrou province, Morocco. Acta Trop. 2014, 130, 94–99. [Google Scholar] [CrossRef]
- Hlavacova, J.; Votypka, J.; Volf, P. The effect of temperature on Leishmania (Kinetoplastida:Trypanosomatidae) development in sand flies. J. Med. Entomol. 2013, 50, 955–958. [Google Scholar] [CrossRef] [PubMed]
- Lawyer, P.G.; Perkins, P.V. Leishmaniasis and Trypanosomiasis. In Medical Entomology; Eldridge, B.F., Edman, J.D., Eds.; Kluwer Academic Publishers: Dordrecht, The Netherlands, 2000; pp. 231–298. [Google Scholar]
- Medlock, J.M.; Hansford, K.M.; Van Bortel, W.; Zeller, H.; Alten, B. A summary of the evidence for the change in European distribution of phlebotomine sand flies (Diptera: Psychodidae) of public health importance. J Vector Ecol. 2014, 39, 72–77. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Benkova, I.; Volf, P. Effect of temperature on metabolism of Phlebotomus papatasi (Diptera: Psychodidae). J Med. Entomol. 2007, 44, 150–154. [Google Scholar] [CrossRef] [PubMed]
- Ready, P.D. Epidemiology of visceral leishmaniasis. Clin. Epidemiol. 2014, 6, 147–154. [Google Scholar] [CrossRef] [PubMed]
- Rioux, J.A.; Aboulker, J.P.; Lanotte, G.; Killick–Kendrick, R.; Martini–Dumas, A. Ecology of leishmaniasisin the south of France. 21. Influence of temperature on the development of Leishmania infantum Nicolle, 1908 in Phlebotomus ariasi Tonnoir, 1921. Experimental study. Ann. Parasitol. Hum. Comp. 1985, 60, 221–229. [Google Scholar] [CrossRef] [PubMed]
- Sakthianandeswaren, A.; Foote, S.J.; Handman, E. The role of host genetics in leishmaniasis. Trends Parasitol. 2009, 25, 383–391. [Google Scholar] [CrossRef] [PubMed]
- Ponte-Sucre, A.; Gamarro, F.; Dujardin, J.C.; Barrett, M.P.; López-Vélez, R.; García-Hernández, R.; Pountain, A.W.; Mwenechanya, R.; Papadopoulou, B. Drug resistance and treatment failure in leishmaniasis: A 21st century challenge. PLoS Negl. Trop. Dis. 2017, 11, e0006052. [Google Scholar] [CrossRef] [PubMed]
- Yanik, M.; Gurel, M.S.; Simsek, Z.; Kati, M. The psychological impact of cutaneous leishmaniasis. Clin. Exp. Dermatol. 2004, 29, 464–467. [Google Scholar] [CrossRef] [PubMed]
- Wilson, A.L.; Dhiman, P.C.; Kitron, U.; Scot, T.W.; van den Berg, H.; Lindsay, S.W. Benefit of insecticide-treated nets, curtains and screening on vector borne diseases, excluding malaria: A systematic review and meta-analysis. PLoS Negl. Trop. Dis. 2014, 8, e3228. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bates, P.A.; Depaquit, J.; Galati, E.A.; Kamhawi, S.; Maroli, M.; McDowell, M.A.; Picado, A.; Ready, P.D.; Salomón, O.D.; Shaw, J.J.; et al. Recent advances in phlebotomine sand fly research related to leishmaniasis control. Parasit. Vectors 2015, 8, 131. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Courtenay, O.; Peters, N.C.; Rogers, M.E.; Bern, C. Combining epidemiology with basicbiology of sand flies, parasites, and hosts to inform leishmaniasis transmission dynamics and control. PLoS Pathog. 2017, 13, e1006571. [Google Scholar] [CrossRef] [PubMed]
| Foci | CLinical Presentation | Leishmania Cycle | Underlying Causes of Expansion | References |
|---|---|---|---|---|
| Governorate of Sidi Bouzid, central Tunisia | Zoonotic Cutaneous Leishmaniasis | Species: Leishmania major Reservoirs: Psammomys obesus, Meriones shawi and Meriones libycus Vector: Phlebotomus papatasi |
| [12] |
| Village of El M’hir, North of Algeria | Zoonotic Cutaneous Leishmaniasis | Species: Leishmania major Reservoirs: Psammomys obesus Vector: Phlebotomus papatasi |
| [18] |
| Errachidia province, South-Est of Morocco | Zoonotic Cutaneous Leishmaniasis | Species: Leishmania major Reservoirs: Meriones shawi Vector: Phlebotomus papatasi |
| [13] |
| Old world | Cutaneous Leishmaniasis | Species: L. infantum, L. tropica, L. major, L. aethiopica and L. donovani Reservoirs: Humans, rodents, Canids, Hyraxes, … Vector: Phlebotomus papatasi, P. sergenti, P. caucasicus, P. duboscqi, P. Bergeroti, … |
| [17] |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kholoud, K.; Denis, S.; Lahouari, B.; El Hidan, M.A.; Souad, B. Management of Leishmaniases in the Era of Climate Change in Morocco. Int. J. Environ. Res. Public Health 2018, 15, 1542. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph15071542
Kholoud K, Denis S, Lahouari B, El Hidan MA, Souad B. Management of Leishmaniases in the Era of Climate Change in Morocco. International Journal of Environmental Research and Public Health. 2018; 15(7):1542. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph15071542
Chicago/Turabian StyleKholoud, Kahime, Sereno Denis, Bounoua Lahouari, Moulay Abdelmonaim El Hidan, and Bouhout Souad. 2018. "Management of Leishmaniases in the Era of Climate Change in Morocco" International Journal of Environmental Research and Public Health 15, no. 7: 1542. https://0-doi-org.brum.beds.ac.uk/10.3390/ijerph15071542





