Chemical Composition and Antimicrobial Activity of Selected Essential Oils against Staphylococcus spp. Isolated from Human Semen
Abstract
:1. Introduction
2. Results and Discussion
2.1. Isolated Species of Staphylococci
2.2. Chemical Composition of Essential Oils
2.3. Antibacterial Effect of Antimicrobials
2.4. Antimicrobial Assay
3. Materials and Methods
3.1. Essential Oil Samples
3.2. Chemical Composition of EOs
3.3. Microorganisms
3.4. Antimicrobial Susceptibility Testing
3.5. Disc Diffusion Method
3.6. Determination of Minimum Inhibitory Concentration
3.7. Statistical Analysis
4. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Pellati, D.; Mylonakis, I.; Bertoloni, G.; Fiore, C.; Andrisani, A.; Ambrosini, G.; Armanini, D. Genital tract infections and infertility. Eur. J. Obstet. Gynecol. Reprod. Biol. 2008, 140, 3–11. [Google Scholar] [CrossRef]
- Henkel, R.; Schill, W.-B. Sperm separation in patients with urogenital infections. Andrologia 2009, 30, 91–97. [Google Scholar] [CrossRef] [PubMed]
- Urata, K.; Narahara, H.; Tanaka, Y.; Egashira, T.; Takayama, F.; Miyakawa, I. Effect of endotoxin-induced reactive oxygen species on sperm motility. Fertil. Steril. 2001, 76, 163–166. [Google Scholar] [CrossRef]
- Sanocka-Maciejewska, D.; Ciupińska, M.; Kurpisz, M. Bacterial infection and semen quality. J. Reprod. Immunol. 2005, 67, 51–56. [Google Scholar] [CrossRef] [PubMed]
- Purvis, K.; Christiansen, E. Infection in the male reproductive tract. Impact, diagnosis and treatment in relation to male infertility. Int. J. Androl. 1993, 16, 1–13. [Google Scholar] [CrossRef]
- Marconi, M.; Pilatz, A.; Wagenlehner, F.; Diemer, T.; Weidner, W. Impact of infection on the secretory capacity of the male accessory glands. Int. Braz. J. Urol. 2009, 35, 299–309. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Greive, K.A.; Barnes, T.M. The efficacy of Australian essential oils for the treatment of head lice infestation in children: A randomised controlled trial. Australas. J. Dermatol. 2018, 59, e99–e105. [Google Scholar] [CrossRef] [Green Version]
- Brochot, A.; Guilbot, A.; Haddioui, L.; Roques, C. Antibacterial, antifungal, and antiviral effects of three essential oil blends. Microbiologyopen 2017, 6, e00459. [Google Scholar] [CrossRef]
- Man, A.; Gâz, A.Ş.; Mare, A.D.; Berţa, L. Effects of low-molecular weight alcohols on bacterial viability. Rev. Rom. Med. Lab. 2017, 25, 335–343. [Google Scholar] [CrossRef] [Green Version]
- Kačániová, M.; Ivanišová, E.; Ondrejovič, M.; Chmelová, D.; Terentjeva, M.; Kunová, S.; Tvrdá, E. BIological activity of essential oils against Staphylococcus spp. isolated from human semen. J. Microbiol. Biotechnol. Food Sci. 2019, 9, 404–408. [Google Scholar] [CrossRef] [Green Version]
- Salari, M.H.; Amine, G.; Shirazi, M.H.; Hafezi, R.; Mohammadypour, M. Antibacterial effects of Eucalyptus globulus leaf extract on pathogenic bacteria isolated from specimens of patients with respiratory tract disorders. Clin. Microbiol. Inf. 2006, 12, 194–196. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fraczek, M.; Kurpisz, M. Mechanisms of the harmful effects of bacterial semen infection on ejaculated human spermatozoa: Potential inflammatory markers in semen. Folia Histochem. Cytobiol. 2015, 53, 201–217. [Google Scholar] [CrossRef] [PubMed]
- Wallach, E.E.; Wolff, H. The biologic significance of white blood cells in semen. Fertil. Steril. 1995, 63, 1143–1157. [Google Scholar] [CrossRef]
- Khalili, M.; Sharifi-Yazdi, M. The effect of bacterial infection on the quality of human’s spermatozoa. Iran. J. Public Health 2001, 35, 62–67. [Google Scholar]
- Barra, A. Factors affecting chemical variability of essential oils: A review of recent developments. Nat. Prod. Commun. 2009, 4. [Google Scholar] [CrossRef] [Green Version]
- Kloucek, P.; Smid, J.; Flesar, J.; Havlik, J.; Titera, D.; Rada, V.; Drabek, O.; Kokoska, L. In vitro inhibitory activity of essential oil vapors against Ascosphaera apis. Nat. Prod. Commun. 2012, 7. [Google Scholar] [CrossRef] [Green Version]
- Camarda, L.; Dayton, T.; Di Stefano, V.; Pitonzo, R.; Schillaci, D. Chemical composition and antimicrobial activity of some oleogum resin essential oils from Boswellia spp. (Burseraceae). Ann. Chim. 2007, 97, 837–844. [Google Scholar] [CrossRef]
- Villanueva, M.A.; Torres, R.C.; Başer, K.H.C.; Özek, T.; Kürkçüoǧlu, M. The composition of Manila elemi oil. Flavour Fragr. J. 1993, 8, 35–37. [Google Scholar] [CrossRef]
- Liang, G.Y.; Qiu, D.W.; Wei, H.F.; Li, H.Y.; Zhao, S.; He, Z.Y.; Liu, N. The essential oil of the fruits from Cinnamomum camphora. J. Guiyang Coll. Tradit. Chin. Med. 1994, 16, 59–60. [Google Scholar]
- Li, S.L.; Luo, Y. The analysis of essential oil from camphor tree fruits in Jinggangshan. J. Jiangxi Univ. Tradit. Chin. Med. 2005, 17, 36–37. [Google Scholar]
- Frizzo, C.D.; Santos, A.C.; Paroul, N.; Serafini, L.A.; Dellacassa, E.; Lorenzo, D.; Moyna, P. Essential oils of camphor tree (Cinnamomum camphora nees & eberm) cultivated in Southern Brazil. Braz. Arch. Biol. Technol. 2000, 43, 313–316. [Google Scholar] [CrossRef] [Green Version]
- Macleod, A.J.; Macleod, G.; Subramanian, G. Volatile aroma constituents of orange. Phytochemistry 1988, 27, 2185–2188. [Google Scholar] [CrossRef]
- Kabouche, Z.; Benkiki, N.; Seguin, E.; Bruneau, C. A new dicoumarinyl ether and two rare furocoumarins from Ruta montana. Fitoterapia 2003, 74, 194–196. [Google Scholar] [CrossRef]
- Nikolić, M.; Marković, T.; Mojović, M.; Pejin, B.; Savić, A.; Perić, T.; Marković, D.; Stević, T.; Soković, M. Chemical composition and biological activity of Gaultheria procumbens L. essential oil. Ind. Crops Prod. 2013, 49, 561–567. [Google Scholar] [CrossRef]
- Thielmann, J.; Muranyi, P. Review on the chemical composition of Litsea cubeba essential oils and the bioactivity of its major constituents citral and limonene. J. Essent. Oil Res. 2019, 31, 361–378. [Google Scholar] [CrossRef]
- Pujiarti, R.; Ohtani, Y.; Ichiura, H. Physicochemical properties and chemical compositions of Melaleuca leucadendron leaf oils taken from the plantations in Java, Indonesia. J. Wood Sci. 2011, 57, 446–451. [Google Scholar] [CrossRef]
- An, N.T.G.; Huong, L.T.; Satyal, P.; Tai, T.A.; Dai, D.N.; Hung, N.H.; Ngoc, N.T.B.; Setzer, W.N. Mosquito larvicidal activity, antimicrobial activity, and chemical compositions of essential oils from four species of myrtaceae from Central Vietnam. Plants 2020, 9, 544. [Google Scholar] [CrossRef] [Green Version]
- Silva, C.J.; Barbosa, L.C.A.; Maltha, C.R.A.; Pinheiro, A.L.; Ismail, F.M.D. Comparative study of the essential oils of seven Melaleuca (Myrtaceae) species grown in Brazil. Flavour Fragr. J. 2007, 22, 474–478. [Google Scholar] [CrossRef]
- Farag, R.S.; Shalaby, A.S.; El-Baroty, G.A.; Ibrahim, N.A.; Ali, M.A.; Hassan, E.M. Chemical and biological evaluation of the essential oils of different Melaleuca species. Phyther. Res. 2004, 18, 30–35. [Google Scholar] [CrossRef]
- Sakasegawa, M.; Hori, K.; Yatagai, M. Composition and antitermite activities of essential oils from Melaleuca species. J. Wood Sci. 2003, 49, 181–187. [Google Scholar] [CrossRef]
- Murugan, R.; Mallavarapu, G.R.; Padmashree, K.V.; Rao, R.R.; Livingstone, C. Volatile oil composition of Pogostemon heyneanus and comparison of its composition with patchouli oil. Nat. Prod. Commun. 2010, 5. [Google Scholar] [CrossRef] [Green Version]
- Paw, M.; Begum, T.; Gogoi, R.; Pandey, S.K.; Lal, M. Chemical composition of Citrus limon L. burmf peel essential oil from North East India. J. Essent. Oil Bear. Plants 2020, 23, 337–344. [Google Scholar] [CrossRef]
- Subasinghe, U.; Gamage, M.; Hettiarachchi, D.S. Essential oil content and composition of Indian sandalwood (Santalum album) in Sri Lanka. J. For. Res. 2013, 24, 127–130. [Google Scholar] [CrossRef]
- Teixeira da Silva, J.A.; Kher, M.M.; Soner, D.; Page, T.; Zhang, X.; Nataraj, M.; Ma, G. Sandalwood: Basic biology, tissue culture, and genetic transformation. Planta 2016, 243, 847–887. [Google Scholar] [CrossRef]
- David, A.; Wang, F.; Sun, X.; Li, H.; Lin, J.; Li, P.; Deng, G. Chemical composition, antioxidant, and antimicrobial activities of Vetiveria zizanioides (L.) nash essential oil extracted by carbon dioxide expanded ethanol. Molecules 2019, 24, 1897. [Google Scholar] [CrossRef] [Green Version]
- EUCAST. The European Committee on Antimicrobial Susceptibility Testing. Available online: http://www.eucast.org/fileadmin/src/media/PDFs/EUCAST_files/Breakpoint_tables/v_9.0_Breakpoint_Tables.pdf (accessed on 13 September 2020).
- Schwarz, S.; Kehrenberg, C.; Doublet, B.; Cloeckaert, A. Molecular basis of bacterial resistance to chloramphenicol and florfenicol. FEMS Microbiol. Rev. 2004, 28, 519–542. [Google Scholar] [CrossRef] [Green Version]
- Schwarz, S.; White, D.G. Phenicol resistance. In Frontiers in Antimicrobial Resistance: A Tribute to Stuart B. Levy; White, D.G., Alekshun, M.N., McDermott, P.F., Eds.; ASM Press: Washington, DC, USA, 2005; pp. 124–147. [Google Scholar]
- Witte, W. Biomedicine: Medical consequences of antibiotic use in agriculture. Science 1998, 279, 996–997. [Google Scholar] [CrossRef]
- Falkiner, F. The consequences of antibiotic use in horticulture. J. Antimicrob. Chemother. 1998, 41, 429–431. [Google Scholar] [CrossRef] [Green Version]
- Levy, S.B. The Antibiotic Paradox; Springer: Boston, MA, USA, 1992; ISBN 978-0-306-44331-2. [Google Scholar]
- Roberts, M.C. Tetracycline resistance determinants: Mechanisms of action, regulation of expression, genetic mobility, and distribution. FEMS Microbiol. Rev. 1996, 19, 1–24. [Google Scholar] [CrossRef]
- Biedenbach, D.J.; Beach, M.L.; Jones, R.N. In vitro antimicrobial activity of GAR-936 tested against antibiotic-resistant gram-positive blood stream infection isolates and strains producing extended-spectrum β-lactamases. Diagn. Microbiol. Infect. Dis. 2001, 40, 173–177. [Google Scholar] [CrossRef]
- Edlund, C.; Nord, C.E. In-vitro susceptibility of anaerobic bacteria to gar-936, a new glycylcycline. Clin. Microbiol. Infect. 2000, 6, 159–163. [Google Scholar] [CrossRef] [PubMed]
- Sanfilippo, C.M.; Morrissey, I.; Janes, R.; Morris, T.W. Surveillance of the activity of aminoglycosides and fluoroquinolones against ophthalmic pathogens from Europe in 2010–2011. Curr. Eye Res. 2015, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Dahiya, P.; Manglik, A. Evaluation of antibacterial, antifungal and antioxidant potential of essential oil from Amyris balsamifera against multi drug resistant clinical isolates. Asian J. Pharm. Clin. Res. 2013, 6, 57–60. [Google Scholar]
- Van Vuuren, S.F.; Kamatou, G.P.P.; Viljoen, A.M. Volatile composition and antimicrobial activity of twenty commercial frankincense essential oil samples. S. Afr. J. Bot. 2010, 76, 686–691. [Google Scholar] [CrossRef]
- Screening of the antifungal activity of essential oils against human and plant pathogenic filamentous fungi. Flora Mediterr. 2019, 29. [CrossRef]
- Satyal, P.; Paudel, P.; Poudel, A.; Dosoky, N.S.; Pokharel, K.K.; Setzer, W.N. Bioactivities and compositional analyses of Cinnamomum essential oils from Nepal: C. camphora, C. tamala, and C. glaucescens. Nat. Prod. Commun. 2013, 8, 1777–1784. [Google Scholar] [CrossRef] [Green Version]
- Mishra, A.K.; Dwivedi, S.K.; Kishore, N.; Dubey, N.K. Fungistatic properties of essential oil of Cinnamomum camphora. Int. J. Pharmacogn. 1991, 29, 259–262. [Google Scholar] [CrossRef]
- Liu, C.H.; Mishra, A.K.; He, B.; Tan, R.X. Composition and antifungal activity of essential oils from Artemisia princeps and Cinnamomum camphora. Int. Pest Control 2001, 43, 72–74. [Google Scholar]
- Singh, P.; Srivastava, B.; Kumar, A.; Dubey, N.K. Fungal contamination of raw materials of some herbal drugs and recommendation of Cinnamomum camphora oil as herbal fungitoxicant. Microb. Ecol. 2008, 56, 555–560. [Google Scholar] [CrossRef]
- Ho, C.-L.; Eugene, I.; Wang, C.; Su, Y.-C. Essential oil compositions and bioactivities of the various parts of Cinnamomum camphora Sieb. var. linaloolifera Fujuta. For. Res. Q. 2009, 31, 77–95. [Google Scholar]
- Rangari, P. Screening of antibacterial sensitivty of essential oils of camphor and cinnamon. Shodh Anusandhan Samachar 2011, 1, 22–26. [Google Scholar]
- Kačániová, M.; Terentjeva, M.; Galovičová, L.; Ivanišová, E.; Štefániková, J.; Valková, V.; Borotová, P.; Kowalczewski, P.Ł.; Kunová, S.; Felšöciová, S.; et al. Biological activity and antibiofilm molecular profile of Citrus aurantium essential oil and its application in a food model. Molecules 2020, 25, 3956. [Google Scholar] [CrossRef] [PubMed]
- Teneva, D.; Denkova-Kostova, R.; Goranov, B.; Hristova-Ivanova, Y.; Slavchev, A.; Denkova, Z.; Kostov, G. Chemical composition, antioxidant activity and antimicrobial activity of essential oil from Citrus aurantium L. zest against some pathogenic microorganisms. Z. Nat. C 2019, 74, 105–111. [Google Scholar] [CrossRef] [Green Version]
- Hammer, K.A.; Carson, C.F.; Riley, T.V. Antimicrobial activity of essential oils and other plant extracts. J. Appl. Microbiol. 1999, 86, 985–990. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Li, W.-R.; Shi, Q.-S.; Liang, Q.; Xie, X.-B.; Huang, X.-M.; Chen, Y.-B. Antibacterial activity and kinetics of Litsea cubeba oil on Escherichia coli. PLoS ONE 2014, 9, e110983. [Google Scholar] [CrossRef]
- Liu, T.-T.; Yang, T.-S. Antimicrobial impact of the components of essential oil of Litsea cubeba from Taiwan and antimicrobial activity of the oil in food systems. Int. J. Food Microbiol. 2012, 156, 68–75. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; Jiang, J.; Qimei, L.; Yan, X.; Zhao, J.; Yuan, H.; Qin, Z.; Wang, M. The fungicidal terpenoids and essential oil from Litsea cubeba in Tibet. Molecules 2010, 15, 7075–7082. [Google Scholar] [CrossRef]
- Cui, H.; Li, W.; Li, C.; Vittayapadung, S.; Lin, L. Liposome containing cinnamon oil with antibacterial activity against methicillin-resistant Staphylococcus aureus biofilm. Biofouling 2016, 32, 215–225. [Google Scholar] [CrossRef]
- Hu, W.; Li, C.; Dai, J.; Cui, H.; Lin, L. Antibacterial activity and mechanism of Litsea cubeba essential oil against methicillin-resistant Staphylococcus aureus (MRSA). Ind. Crops Prod. 2019, 130, 34–41. [Google Scholar] [CrossRef]
- Siddique, S.; Parveen, Z.; Firdaus-e-Bareen; Mazhar, S. Chemical composition, antibacterial and antioxidant activities of essential oils from leaves of three Melaleuca species of Pakistani flora. Arab. J. Chem. 2020, 13, 67–74. [Google Scholar] [CrossRef]
- Dryden, M.; Dailly, S.; Crouch, M. A randomized, controlled trial of tea tree topical preparations versus a standard topical regimen for the clearance of MRSA colonization. J. Hosp. Infect. 2004, 56, 283–286. [Google Scholar] [CrossRef] [PubMed]
- Messager, S.; Hammer, K.A.; Carson, C.F.; Riley, T.V. Effectiveness of hand-cleansing formulations containing tea tree oil assessed ex vivo on human skin and in vivo with volunteers using European standard EN 1499. J. Hosp. Infect. 2005, 59, 220–228. [Google Scholar] [CrossRef]
- Edmondson, M.; Newall, N.; Carville, K.; Smith, J.; Riley, T.V.; Carson, C.F. Uncontrolled, open-label, pilot study of tea tree (Melaleuca alternifolia) oil solution in the decolonisation of methicillin-resistant Staphylococcus aureus positive wounds and its influence on wound healing. Int. Wound J. 2011, 8, 375–384. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Blackwood, B.; Thompson, G.; McMullan, R.; Stevenson, M.; Riley, T.V.; Alderdice, F.A.; Trinder, T.J.; Lavery, G.G.; McAuley, D.F. Tea tree oil (5%) body wash versus standard care (Johnson’s Baby Softwash) to prevent colonization with methicillin-resistant Staphylococcus aureus in critically ill adults: A randomized controlled trial. J. Antimicrob. Chemother. 2013, 68, 1193–1199. [Google Scholar] [CrossRef] [Green Version]
- Hussein, S.A.M.; Hashim, A.N.M.; El-Sharawy, R.T.; Seliem, M.A.; Linscheid, M.; Lindequist, U.; Nawwar, M.A.M. Ericifolin: An eugenol 5-O-galloylglucoside and other phenolics from Melaleuca ericifolia. Phytochemistry 2007, 68, 1464–1470. [Google Scholar] [CrossRef]
- Das, P.; Dutta, S.; Begum, J.; Anwar, M.N. Antibacterial and antifungal activity analysis of essential oil of Pogostemon cablin (Blanco) benth. Bangladesh J. Microbiol. 2016, 30, 7–10. [Google Scholar] [CrossRef] [Green Version]
- Saeb, S.; Amin, M.; Seyfi Gooybari, R.; Aghel, N. Evaluation of antibacterial activities of Citrus limon, Citrus reticulata, and Citrus grandis against pathogenic bacteria. Int. J. Enteric Pathog. 2016, 4, 11–15. [Google Scholar] [CrossRef] [Green Version]
- Dhiman, A.; Ahmad, S.; Nanda, A.; Narasimhan, B. In vitro antimicrobial status of methanolic extract of Citrus sinensis Linn. fruit peel. Chron. Young Sci. 2012, 3, 204. [Google Scholar] [CrossRef]
- Hamdan, D.; Ashour, M.L.; Mulyaningsih, S.; El-Shazly, A.; Wink, M. Chemical composition of the essential oils of variegated pink-fleshed lemon (Citrus × limon L. Burm. f.) and their anti-inflammatory and antimicrobial activities. Z. Nat. C 2013, 68, 0275. [Google Scholar] [CrossRef]
- Misra, B.B.; Dey, S. Comparative phytochemical analysis and antibacterial efficacy of in vitro and in vivo extracts from East Indian sandalwood tree (Santalum album L.). Lett. Appl. Microbiol. 2012, 55, 476–486. [Google Scholar] [CrossRef]
- Jirovetz, L.; Buchbauer, G.; Denkova, Z.; Stoyanova, A.; Murgov, I.; Gearon, V.; Birkbeck, S.; Schmidt, E.; Geissler, M. Comparative study on the antimicrobial activities of different sandalwood essential oils of various origin. Flavour Fragr. J. 2006, 21, 465–468. [Google Scholar] [CrossRef]
- Gupta, R.; Sharma, K.K.; Afzal, M.; Damanhouri, Z.A.; Ali, B.; Kaur, R.; Kazmi, I.; Anwar, F. Anticonvulsant activity of ethanol extracts of Vetiveria zizanioides roots in experimental mice. Pharm. Biol. 2013, 51, 1521–1524. [Google Scholar] [CrossRef] [PubMed]
- Champagnat, P.; Sidibé, L.; Forestier, C.; Carnat, A.; Chalchat, J.-C.; Lamaison, J.-L. Antimicrobial activity of essential oils from Vetiveria nigritana and Vetiveria zizanioides roots. J. Essent. Oil Bear. Plants 2007, 10, 519–524. [Google Scholar] [CrossRef]
- Kačániová, M.; Galovičová, L.; Ivanišová, E.; Vukovic, N.L.; Štefániková, J.; Valková, V.; Borotová, P.; Žiarovská, J.; Terentjeva, M.; Felšöciová, S.; et al. Antioxidant, antimicrobial and antibiofilm activity of coriander (Coriandrum sativum L.) essential oil for its application in foods. Foods 2020, 9, 282. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kačániová, M.; Kunová, S.; Sabo, J.; Ivanišová, E.; Žiarovská, J.; Felšöciová, S.; Fatrcová-Šramková, K.; Terentjeva, M. Isolation and identification of lactic acid bacteria in wine production by MALDI-TOF MS biotyper. Acta Hortic. Regiotect. 2020, 23, 21–24. [Google Scholar] [CrossRef]
- Zheljazkov, V.D.; Sikora, V.; Semerdjieva, I.B.; Kačániová, M.; Astatkie, T.; Dincheva, I. Grinding and fractionation during distillation alter hemp essential oil profile and its antimicrobial activity. Molecules 2020, 25, 3943. [Google Scholar] [CrossRef]
- Xiangwei, Z.; Xiaodong, W.; Peng, N.; Yang, Z.; JiaKuan, C. Chemical composition and antimicrobial activity of the essential oil of Sagittaria trifolia. Chem. Nat. Compd. 2006, 42, 520–522. [Google Scholar] [CrossRef]
- Rota, M.C.; Herrera, A.; Martínez, R.M.; Sotomayor, J.A.; Jordán, M.J. Antimicrobial activity and chemical composition of Thymus vulgaris, Thymus zygis and Thymus hyemalis essential oils. Food Control 2008, 19, 681–687. [Google Scholar] [CrossRef]
- Lv, F.; Liang, H.; Yuan, Q.; Li, C. In vitro antimicrobial effects and mechanism of action of selected plant essential oil combinations against four food-related microorganisms. Food Res. Int. 2011, 44, 3057–3064. [Google Scholar] [CrossRef]
- National Committee for Clinical Laboratory Standards. Performance Standards for Antimicrobial Susceptibility Testing; 9th International Supplement, M100-S9; NCCLS: Wayne, PA, USA, 1999. [Google Scholar]

| Essential Oil | Components | RT (min.) | Percentage of Components (n = 3) |
|---|---|---|---|
| Amyris balsamifera L. | Amorpha-4,11-diene | 24.20 | 2.58 |
| β-cadinene | 25.04 | 1.33 | |
| Dihydroagarofuran | 26.43 | 1.53 | |
| β-dihydroagarofuran | 26.56 | 1.05 | |
| α-zingiberene | 27.06 | 2.21 | |
| Cedrene | 28.72 | 4.91 | |
| α-curcumen | 28.89 | 2.44 | |
| Nerolidol | 35.64 | 1.57 | |
| Elemol | 39.25 | 9.62 | |
| β-eudesmol | 39.75 | 1.13 | |
| γ-eudesmol | 40.50 | 2.49 | |
| Guaiol | 40.94 | 19.40 | |
| 10-epi-γ-eudesmol | 41.75 | 14.80 | |
| Valerianol | 43.16 | 23.20 | |
| Drim-7-en-11-ol | 50.65 | 1.84 | |
| Boswelia carterii Birdw. | Sabinene | 4.33 | 5.51 |
| 3-Carene | 5.05 | 1.39 | |
| α-phellandrene | 5.54 | 2.81 | |
| β-myrcene | 5.65 | 3.91 | |
| D-limonene | 6.68 | 26.40 | |
| 4-Thujanol | 6.70 | 1.49 | |
| prehnitene | 9.25 | 8.65 | |
| Copaene | 17.96 | 1.59 | |
| Bornyl acetate | 21.6 | 1.00 | |
| 2-methylene-4,8,8-trimethyl-4-vinyl-bicyclo[5.2.0]nonane | 21.93 | 7.83 | |
| Farnesol | 24.6 | 2.24 | |
| trans-verbenol | 25.65 | 1.55 | |
| β-selinene | 26.39 | 2.18 | |
| γ-selinene | 26.63 | 1.24 | |
| γ-cadinene | 28.02 | 1.67 | |
| δ-cadinene | 28.12 | 2.05 | |
| Carveol | 31.32 | 1.03 | |
| Caryophyllene oxide | 35.28 | 2.41 | |
| tau-cadinol | 41.74 | 2.13 | |
| Canarium luzonicum (Blume) A. Gray | β-Phellandrene | 4.34 | 4.54 |
| α-Phellandrene | 5.54 | 12.20 | |
| D-limonene | 6.68 | 36.40 | |
| cis-Sabinene | 6.90 | 3.06 | |
| o-cymene | 9.25 | 3.35 | |
| α-terpinolen | 9.75 | 1.59 | |
| Terpinen-4-ol | 22.71 | 1.15 | |
| α-terpineol | 26.41 | 3.83 | |
| Elemol | 39.25 | 16.70 | |
| 10-epi-γ-eudesmol | 41.75 | 1.59 | |
| Rosifoliol | 43.27 | 1.08 | |
| Elemicin | 43.73 | 9.59 | |
| Cinnamomum camphora (L.) J. Presl. | Sabinene | 4.33 | 6.07 |
| β-pinene | 5.64 | 1.70 | |
| D-limonene | 6.68 | 25.90 | |
| 1,8-cineol | 7.07 | 44.90 | |
| γ-terpinene | 8.35 | 1.43 | |
| o-cymene | 9.25 | 11.70 | |
| Cinnamomum caphora var. linaloolifera Y. Fuita | 1,2-epoxylinalool | 16.46 | 1.27 |
| Linalool | 21.32 | 96.99 | |
| Citrus x aurantium L. | β-myrcene | 5.65 | 2.32 |
| D-limonene | 6.68 | 1.57 | |
| 1,8-cineole | 7.07 | 2.70 | |
| β-ocimene | 8.75 | 2.39 | |
| Linalyl acetate | 21.14 | 63.4 | |
| Caryophyllene | 21.92 | 1.34 | |
| α-terpineol | 26.41 | 8.84 | |
| Neryl acetate | 27.51 | 3.77 | |
| Geranyl acetate | 28.64 | 6.02 | |
| Geraniol | 30.28 | 5.31 | |
| Gaultheria procumbens L. | Methyl salicylate | 28.68 | 98.00 |
| Litsea cubeba (Lour.) Pers. | Sabinene | 4.33 | 2.20 |
| D-limonene | 6.68 | 14.00 | |
| 1,8-cineole | 7.07 | 1.62 | |
| 6-methyl-5-hepten-2-one | 12.11 | 1.35 | |
| Citronellal | 17.86 | 1.00 | |
| Linalool | 21.32 | 1.82 | |
| Caryophyllene | 21.92 | 1.85 | |
| (Z)-citral | 25.56 | 31.00 | |
| α-terpineol | 26.41 | 1.06 | |
| (E)-citral | 27.51 | 35.2 | |
| trans-geraniol | 32.01 | 1.35 | |
| nerolic acid | 45.74 | 1.13 | |
| Melaleuca leucadendron L. | D-limonene | 6.68 | 8.12 |
| 1,8-Cineole | 7.07 | 49.20 | |
| γ-terpinen | 8.35 | 2.91 | |
| o-cymene | 9.25 | 3.16 | |
| α-terpinolen | 9.75 | 1.24 | |
| Linalyl acetate | 21.14 | 1.13 | |
| Caryophyllene | 21.92 | 5.65 | |
| 2,4-dihydroxy-2-methylpentane | 24.12 | 4.11 | |
| Z,Z,Z-1,5,9,9-tetramethyl-1,4,7,-cycloundecatriene | 24.61 | 2.91 | |
| α-terpineol acetate | 26.07 | 1.84 | |
| α-terpineol | 26.41 | 9.92 | |
| α-selinene | 26.64 | 2.09 | |
| Globulol | 38.72 | 1.90 | |
| Melaleuca ericifolia Smith. | D-limonene | 6.68 | 2.97 |
| 1,8-cineol | 7.07 | 23.10 | |
| γ-terpinene | 8.35 | 2.63 | |
| o-cymene | 9.25 | 3.64 | |
| 1,2-epoxylinalool | 16.46 | 2.03 | |
| Ethyl 2-(5-methyl-5-vinyltetrahydrofuran-2-yl)propan-2-yl carbonate | 17.61 | 1.54 | |
| β-linalool | 21.24 | 36.70 | |
| 2-methylene-4,8,8-trimethyl-4-vinyl-bicyclo[5.2.0]nonane | 21.93 | 1.17 | |
| Alloaromadendrene | 22.40 | 4.73 | |
| Terpinen-4-ol | 22.71 | 2.62 | |
| Aromadendrene | 23.75 | 1.86 | |
| Leden | 25.73 | 1.07 | |
| α-terpineol | 26.41 | 4.98 | |
| Pogostemon cabli (Blanco) Benth. | Patchoulene | 17.51 | 3.28 |
| α-guaien | 22.10 | 18.10 | |
| α-patchoulene | 23.23 | 6.09 | |
| 1,1,4a-Trimethyl-5,6-dimethylenedecahydronaphthalene | 23.33 | 7.88 | |
| γ-patchoulene | 23.88 | 1.10 | |
| Aciphyllene | 26.11 | 3.53 | |
| γ-guajene | 26.69 | 18.20 | |
| Patchouli alcohol | 41.48 | 27.30 | |
| Pogostol | 42.74 | 2.65 | |
| Dhelqangin | 51.98 | 2.34 | |
| Citrus limon (L.) Osbeck | (E)-citral | 27.51 | 2.44 |
| Sabinene | 4.33 | 3.45 | |
| β-myrcene | 5.65 | 2.42 | |
| D-limonene | 6.68 | 67.10 | |
| α-terpinolen | 9.75 | 14.20 | |
| α-bergamotene | 21.89 | 1.33 | |
| Neral | 25.45 | 1.50 | |
| β-bisabolene | 27.22 | 1.30 | |
| Santalum album L. | α-santalene | 21.31 | 5.03 |
| α-bergamotene | 21.89 | 9.68 | |
| α-santalal | 41.14 | 2.54 | |
| α-santalol | 41.69 | 59.00 | |
| β-santalol | 50.36 | 9.02 | |
| Lanceol | 51.12 | 1.93 | |
| (E)-nuciferol | 51.87 | 1.74 | |
| 7-(5-hexynyl)-tricyclo[4.2.2.0(2,5)]dec-7-ene | 52.26 | 1.38 | |
| Vetiveria zizanoides (L.) Roberty | 3,3,5,6,8,8-Hexamethyltricyclo[5.1.0.0(2,4)]oct-5-ene | 18.88 | 1.02 |
| Tricyclo[6.3.0.0(1,5)]undec-2-en-4-one, 5,9-dimethyl | 20.76 | 2.00 | |
| 1,2,4,5-tetraethylbenzene | 21.32 | 4.39 | |
| α-muurolene | 25.59 | 1.89 | |
| α-cadinene | 25.78 | 1.74 | |
| Selina-5,11-diene | 26.16 | 1.50 | |
| δ-cadinene | 26.64 | 1.57 | |
| α-vetispirene | 27.16 | 1.77 | |
| β-vetispirene | 27.42 | 2.03 | |
| γ-vetivenene | 30.19 | 3.30 | |
| β-vetivenene | 31.27 | 7.42 | |
| Valencen | 32.39 | 2.19 | |
| 3,5,11-Eudesmatriene | 34.91 | 1.65 | |
| 7,7-dichlorobicyclo[3.2.0]hept-2-en-6-one | 41.06 | 1.22 | |
| γ-himachalene | 41.31 | 2.63 | |
| Ziza-6(13)-en-12-al | 41.99 | 1.02 | |
| Khusiol | 45.27 | 1.12 | |
| β-guaiene | 45.58 | 4.43 | |
| Cyclocopacamphenol | 46.03 | 1.66 | |
| Zizanol | 47.64 | 1.03 | |
| (E)-isovalencenal | 47.76 | 1.37 | |
| Vetiselinenol | 48.57 | 1.41 | |
| Vetiverol | 50.15 | 2.22 | |
| Khusenol | 50.68 | 5.24 | |
| Vetiverone | 51.09 | 3.02 | |
| β-costol | 52.11 | 3.52 | |
| Khusenic acid | 63.32 | 4.17 |
| Name of Bacteria/AMB | C | TET | TIG | TOB |
|---|---|---|---|---|
| Stapyloccocus aureus 18.3 | S | S | S | S |
| Staphyloccous capitis 3.6 | R | S | S | I |
| Staphylococcus epidermidis 2.2 | R | S | S | R |
| Staphylococcus epidermidis 2.4 | S | S | S | R |
| Staphylococcus epidermidis 16.2 | S | S | S | R |
| Staphylococcus epidermidis 18.4 | R | S | S | R |
| Staphylococcus epidermidis 19.5 | S | S | S | R |
| Staphylococcus epidermidis 24.2 | R | S | S | I |
| Staphylococcus epidermidis 27.3 | R | S | S | R |
| Staphylococcus haemoliticus 2.3 | R | S | S | R |
| Staphylococcus haemoliticus 14.5 | R | S | S | R |
| Staphylococcus haemoliticus 14.6 | R | S | S | R |
| Staphylococcus haemoliticus 14.7 | S | S | S | R |
| Staphylococcus haemoliticus 14.8 | R | S | S | R |
| Staphylococcus haemoliticus 17.1 | R | S | S | R |
| Staphylococcus haemoliticus 17.2 | R | S | S | R |
| Staphylococcus haemoliticus 17.3 | R | S | S | R |
| Staphylococcus haemoliticus 17.5 | S | S | S | R |
| Staphylococcus haemoliticus 17.6 | R | S | S | S |
| Staphylococcus haemoliticus 19.7 | R | S | S | R |
| Staphylococcus haemoliticus 19.8 | S | S | S | R |
| Staphylococcus haemoliticus 20.2 | S | S | S | R |
| Staphylococcus haemoliticus 20.4 | R | S | S | I |
| Staphylococcus haemoliticus 20.5 | R | S | S | R |
| Staphylococcus haemoliticus 21.5 | R | S | S | S |
| Staphylococcus haemoliticus 21.6 | S | S | S | I |
| Staphylococcus haemoliticus 21.7 | R | S | S | R |
| Staphylococcus haemoliticus 22.5 | R | S | S | R |
| Staphylococcus haemoliticus 24.1 | R | S | S | S |
| Staphylococcus haemoliticus 24.2 | R | S | S | R |
| Staphylococcus haemoliticus 24.5 | R | S | S | S |
| Staphylococcus haemoliticus 24.6 | S | S | S | I |
| Staphylococcus haemoliticus 24.7 | R | S | S | R |
| Staphylococcus haemoliticus 24.8 | R | S | S | R |
| Staphylococcus haemoliticus | R | S | S | S |
| Staphylococus hominis 3.1 | S | S | S | R |
| Staphylococus hominis 3.2 | R | S | S | R |
| Staphylococus hominis 3.3 | R | S | S | I |
| Staphylococus hominis 3.4 | R | S | S | R |
| Staphylococus hominis 3.5 | S | S | S | R |
| Staphylococus hominis 3.7 | R | S | S | S |
| Staphylococus hominis 14.4 | R | S | S | R |
| Staphylococus hominis 16.1 | R | S | S | S |
| Staphylococus hominis 16.4 | S | S | S | R |
| Staphylococus hominis 17.4 | R | S | S | R |
| Staphylococus hominis 18.1 | R | S | S | R |
| Staphylococus hominis 18.8 | R | S | S | I |
| Staphylococus hominis 21.1 | R | S | S | S |
| Staphylococus hominis 21.2 | R | S | S | I |
| Staphylococus hominis 27.4 | R | S | S | S |
| Isolate/EOs | 1. | 2. | 3. | 4. | 5. | 6. | 7. |
|---|---|---|---|---|---|---|---|
| Stapyloccocus aureus 18.3 | 16.50 ± 1.32 | 11.00 ± 1.00 | 21.33 ± 1.15 | 7.67 ± 0.58 | 24.67 ± 0.58 | 14.67 ± 0.58 | 7.33 ± 0.58 |
| Staphyloccous capitis 3.6 | 12.33 ± 0.58 | 8.67 ± 0.58 | 24.67 ± 0.58 | 4.67 ± 0.58 | 14.67 ± 0.58 | 7.67 ± 0.58 | 8.33 ± 0.58 |
| Staphylococcus epidermidis 2.2 | 9.33 ± 0.58 | 12.67 ± 0.58 | 20.33 ± 0.58 | 9.00 ± 1.00 | 8.33 ± 0.58 | 15.33 ± 0.58 | 5.67 ± 0.58 |
| Staphylococcus epidermidis 2.4 | 8.67 ± 0.58 | 11.67 ± 0.58 | 22.33 ± 0.58 | 7.67 ± 0.58 | 7.33 ± 0.58 | 15.00 ± 0.00 | 4.67 ± 0.58 |
| Staphylococcus epidermidis 16.2 | 11.67 ± 0.58 | 12.67 ± 0.58 | 21.67 ± 0.58 | 4.67 ± 0.58 | 7.67 ± 0.58 | 16.33 ± 0.58 | 5.67 ± 0.58 |
| Staphylococcus epidermidis 18.4 | 10.67 ± 0.58 | 13.33 ± 1.15 | 19.67 ± 0.58 | 5.33 ± 0.58 | 8.33 ± 0.58 | 15.67 ± 1.15 | 5.50 ± 0.50 |
| Staphylococcus epidermidis 19.5 | 14.67 ± 0.58 | 12.67 ± 0.58 | 20.33 ± 0.58 | 4.67 ± 0.58 | 6.33 ± 1.15 | 16.67 ± 0.58 | 5.00 ± 1.00 |
| Staphylococcus epidermidis 24.2 | 11.33 ± 1.15 | 11.67 ± 1.53 | 19.67 ± 0.58 | 6.33 ± 0.58 | 7.33 ± 1.15 | 16.00 ± 1.00 | 4.33 ± 0.58 |
| Staphylococcus epidermidis 27.3 | 11.67 ± 1.53 | 11.67 ± 1.15 | 20.33 ± 1.15 | 5.67 ± 0.58 | 6.67 ± 0.58 | 17.33 ± 0.58 | 4.67 ± 0.58 |
| Staphylococcus haemoliticus 2.3 | 8.67 ± 0.58 | 8.33 ± 0.58 | 20.67 ± 1.15 | 4.67 ± 0.58 | 4.67 ± 0.58 | 10.33 ± 0.58 | 5.67 ± 0.58 |
| Staphylococcus haemoliticus 14.5 | 7.67 ± 0.58 | 8.67 ± 1.15 | 18.33 ± 0.58 | 6.33 ± 0.58 | 5.67 ± 0.58 | 8.67 ± 0.58 | 5.33 ± 1.15 |
| Staphylococcus haemoliticus 14.6 | 11.00 ± 1.00 | 8.67 ± 1.15 | 19.67 ± 0.58 | 7.67 ± 0.58 | 4.67 ± 0.58 | 8.33 ± 0.58 | 6.33 ± 1.15 |
| Staphylococcus haemoliticus 14.7 | 7.00 ± 1.00 | 7.67 ± 0.58 | 20.33 ± 0.58 | 8.33 ± 0.58 | 4.67 ± 1.15 | 7.67 ± 1.15 | 4.67 ± 0.58 |
| Staphylococcus haemoliticus 14.8 | 11.00 ± 1.00 | 8.67 ± 0.58 | 18.67 ± 0.58 | 9.33 ± 1.15 | 5.33 ± 0.58 | 8.33 ± 0.58 | 6.00 ± 1.00 |
| Staphylococcus haemoliticus 17.1 | 10.67 ± 1.15 | 10.67 ± 1.15 | 18.33 ± 0.58 | 6.33 ± 1.15 | 5.67 ± 0.58 | 6.67 ± 0.58 | 4.67 ± 0.58 |
| Staphylococcus haemoliticus 17.2 | 9.67 ± 1.15 | 10.67 ± 0.58 | 17.33 ± 0.58 | 5.33 ± 0.58 | 6.67 ± 0.58 | 7.33 ± 0.58 | 5.67 ± 1.15 |
| Staphylococcus haemoliticus 17.3 | 9.00 ± 1.00 | 8.67 ± 0.58 | 18.33 ± 0.58 | 5.33 ± 0.58 | 6.33 ± 1.15 | 8.33 ± 0.58 | 5.33 ± 0.58 |
| Staphylococcus haemoliticus 17.5 | 13.33 ± 1.15 | 8.67 ± 0.58 | 17.67 ± 1.15 | 6.33 ± 0.58 | 7.33 ± 0.58 | 6.33 ± 1.15 | 5.67 ± 0.58 |
| Staphylococcus haemoliticus 17.6 | 11.33 ± 1.15 | 9.33 ± 0.58 | 20.33 ± 0.58 | 5.67 ± 1.15 | 6.33 ± 0.58 | 5.67 ± 0.58 | 5.00 ± 1.00 |
| Staphylococcus haemoliticus 19.7 | 14.33 ± 0.58 | 7.67 ± 0.58 | 18.33 ± 1.15 | 6.00 ± 1.73 | 7.67 ± 0.58 | 7.33 ± 0.58 | 4.67 ± 0.58 |
| Staphylococcus haemoliticus 19.8 | 13.67 ± 1.53 | 10.67 ± 0.58 | 18.67 ± 1.15 | 5.67 ± 1.15 | 7.33 ± 0.58 | 8.67 ± 0.58 | 6.33 ± 0.58 |
| Staphylococcus haemoliticus 20.2 | 9.00 ± 1.00 | 10.67 ± 1.15 | 20.33 ± 1.15 | 5.67 ± 0.58 | 5.67 ± 0.58 | 7.33 ± 0.58 | 4.67 ± 1.15 |
| Staphylococcus haemoliticus 20.4 | 10.33 ± 0.58 | 8.67 ± 0.58 | 19.33 ± 1.15 | 5.00 ± 1.00 | 6.33 ± 0.58 | 7.67 ± 1.15 | 5.67 ± 1.15 |
| Staphylococcus haemoliticus 20.5 | 13.00 ± 1.00 | 9.00 ± 1.00 | 18.33 ± 1.15 | 7.33 ± 0.58 | 5.33 ± 0.58 | 7.67 ± 0.58 | 6.00 ± 1.00 |
| Staphylococcus haemoliticus 21.5 | 14.33 ± 0.58 | 8.33 ± 0.58 | 20.33 ± 0.58 | 7.67 ± 0.58 | 6.00 ± 1.00 | 8.33 ± 0.58 | 5.83 ± 0.29 |
| Staphylococcus haemoliticus 21.6 | 9.33 ± 0.58 | 9.67 ± 1.15 | 18.67 ± 0.58 | 7.33 ± 0.58 | 6.67 ± 1.15 | 7.67 ± 0.58 | 6.17 ± 0.29 |
| Staphylococcus haemoliticus 21.7 | 8.33 ± 0.58 | 10.33 ± 0.58 | 17.67 ± 0.58 | 6.67 ± 0.58 | 4.67 ± 1.15 | 6.33 ± 0.58 | 5.17 ± 0.29 |
| Staphylococcus haemoliticus 22.5 | 7.33 ± 0.58 | 8.33 ± 0.58 | 17.33 ± 1.15 | 5.67 ± 0.58 | 4.67 ± 0.58 | 6.33 ± 1.15 | 4.33 ± 0.58 |
| Staphylococcus haemoliticus 24.1 | 11.67 ± 0.58 | 10.33 ± 0.58 | 18.67 ± 0.58 | 6.33 ± 1.15 | 5.33 ± 1.53 | 6.67 ± 1.15 | 5.67 ± 1.15 |
| Staphylococcus haemoliticus 24.2 | 10.33 ± 0.58 | 10.67 ± 0.58 | 19.33 ± 1.15 | 8.67 ± 1.15 | 5.67 ± 1.15 | 6.67 ± 0.58 | 4.67 ± 1.15 |
| Staphylococcus haemoliticus 24.5 | 12.17 ± 0.29 | 9.67 ± 0.58 | 18.67 ± 0.58 | 7.67 ± 0.58 | 6.67 ± 0.58 | 6.00 ± 1.00 | 5.33 ± 0.58 |
| Staphylococcus haemoliticus 24.6 | 10.67 ± 0.58 | 8.33 ± 0.58 | 17.67 ± 0.58 | 8.33 ± 1.15 | 5.67 ± 0.58 | 5.67 ± 0.58 | 4.33 ± 0.58 |
| Staphylococcus haemoliticus 24.7 | 12.00 ± 2.00 | 8.33 ± 0.58 | 19.33 ± 1.15 | 8.00 ± 1.00 | 6.33 ± 1.15 | 4.67 ± 0.58 | 4.67 ± 0.58 |
| Staphylococcus haemoliticus 24.8 | 10.33 ± 0.58 | 8.33 ± 0.58 | 18.33 ± 0.58 | 7.67 ± 0.58 | 6.33 ± 0.58 | 5.33 ± 0.58 | 5.83 ± 0.76 |
| Staphylococcus haemoliticus | 11.33 ± 0.58 | 12.67 ± 0.58 | 20.33 ± 0.58 | 8.33 ± 0.58 | 7.67 ± 0.58 | 6.33 ± 0.58 | 4.67 ± 0.58 |
| Staphylococus hominis 3.1 | 11.33 ± 0.58 | 10.33 ± 0.58 | 21.67 ± 0.58 | 10.67 ± 0.58 | 18.33 ± 0.58 | 8.00 ± 1.73 | 3.33 ± 1.15 |
| Staphylococus hominis 3.2 | 9.33 ± 0.58 | 11.33 ± 1.15 | 22.00 ± 1.73 | 9.33 ± 0.58 | 19.67 ± 0.58 | 8.33 ± 0.58 | 3.67 ± 0.58 |
| Staphylococus hominis 3.3 | 7.67 ± 0.58 | 10.00 ± 1.73 | 21.33 ± 0.58 | 8.33 ± 0.58 | 19.33 ± 0.58 | 8.00 ± 1.73 | 4.33 ± 0.58 |
| Staphylococus hominis 3.4 | 11.67 ± 0.58 | 8.33 ± 0.58 | 21.33 ± 0.58 | 9.00 ± 1.00 | 18.33 ± 0.58 | 7.33 ± 1.15 | 4.67 ± 0.58 |
| Staphylococus hominis 3.5 | 9.67 ± 0.58 | 9.67 ± 0.58 | 21.67 ± 0.58 | 8.33 ± 0.58 | 20.33 ± 0.58 | 8.67 ± 0.58 | 4.33 ± 0.58 |
| Staphylococus hominis 3.7 | 10.33 ± 1.15 | 10.33 ± 1.15 | 18.67 ± 0.58 | 8.67 ± 0.58 | 21.67 ± 0.58 | 8.00 ± 1.00 | 4.33 ± 0.58 |
| Staphylococus hominis 14.4 | 10.67 ± 1.15 | 9.33 ± 1.15 | 20.33 ± 0.58 | 7.33 ± 0.58 | 18.67 ± 1.15 | 7.33 ± 1.15 | 3.67 ± 0.58 |
| Staphylococus hominis 16.1 | 10.67 ± 1.53 | 8.67 ± 0.58 | 18.67 ± 0.58 | 7.67 ± 1.15 | 17.67 ± 1.15 | 7.33 ± 0.58 | 3.67 ± 1.15 |
| Staphylococus hominis 16.4 | 9.33 ± 0.58 | 8.33 ± 0.58 | 20.33 ± 0.58 | 7.33 ± 1.15 | 19.67 ± 0.58 | 9.33 ± 0.58 | 3.67 ± 0.58 |
| Staphylococus hominis 17.4 | 11.33 ± 1.15 | 9.00 ± 1.00 | 21.67 ± 0.58 | 8.33 ± 0.58 | 19.33 ± 0.58 | 7.67 ± 0.58 | 5.33 ± 0.58 |
| Staphylococus hominis 18.1 | 12.67 ± 1.15 | 10.67 ± 0.58 | 20.67 ± 0.58 | 8.67 ± 0.58 | 18.33 ± 0.58 | 8.67 ± 0.58 | 5.67 ± 0.58 |
| Staphylococus hominis 18.8 | 9.00 ± 1.00 | 11.67 ± 0.58 | 21.67 ± 0.58 | 8.67 ± 1.15 | 17.33 ± 0.58 | 7.67 ± 0.58 | 4.33 ± 0.58 |
| Staphylococus hominis 21.1 | 11.33 ± 0.58 | 11.67 ± 0.58 | 20.50 ± 0.50 | 8.55 ± 0.50 | 18.33 ± 0.58 | 8.33 ± 0.58 | 4.67 ± 0.58 |
| Staphylococus hominis 21.2 | 11.00 ± 1.00 | 11.00 ± 1.00 | 21.33 ± 0.58 | 7.67 ± 0.58 | 19.33 ± 1.15 | 8.67 ± 1.15 | 4.00 ± 0.00 |
| Staphylococus hominis 27.4 | 10.67 ± 1.15 | 9.33 ± 0.58 | 22.33 ± 0.58 | 7.67 ± 0.58 | 19.33 ± 1.53 | 7.67 ± 0.58 | 4.33 ± 1.15 |
| Isolate/EOs | 8. | 9. | 10. | 11. | 12. | 13. | 14. |
|---|---|---|---|---|---|---|---|
| Stapyloccocus aureus 18.3 | 23.33 ± 0.58 | 4.67 ± 0.58 | 14.67 ± 0.58 | 9.00 ± 1.00 | 10.67 ± 1.15 | 5.33 ± 0.58 | 11.33 ± 0.58 |
| Staphyloccous capitis 3.6 | 25.33 ± 0.58 | 3.67 ± 1.15 | 8.67 ± 0.58 | 8.33 ± 0.58 | 12.67 ± 1.15 | 7.33 ± 0.58 | 12.67 ± 0.58 |
| Staphylococcus epidermidis 2.2 | 14.66 ± 0.58 | 4.33 ± 0.58 | 6.67 ± 0.58 | 7.33 ± 0.58 | 8.33 ± 0.58 | 4.33 ± 0.58 | 6.67 ± 1.15 |
| Staphylococcus epidermidis 2.4 | 12.67 ± 0.58 | 4.00 ± 1.00 | 5.67 ± 0.58 | 6.33 ± 0.58 | 8.67 ± 1.15 | 4.33 ± 0.58 | 6.67 ± 1.15 |
| Staphylococcus epidermidis 16.2 | 14.33 ± 0.58 | 3.67 ± 0.58 | 6.33 ± 1.15 | 6.00 ± 1.00 | 9.00 ± 1.00 | 5.00 ± 1.00 | 6.67 ± 0.58 |
| Staphylococcus epidermidis 18.4 | 14.50 ± 0.87 | 4.67 ± 0.58 | 7.33 ± 0.58 | 5.67 ± 1.15 | 9.67 ± 1.15 | 5.33 ± 0.58 | 7.00 ± 1.73 |
| Staphylococcus epidermidis 19.5 | 11.67 ± 0.58 | 3.67 ± 0.58 | 6.33 ± 0.58 | 5.67 ± 0.58 | 8.33 ± 0.58 | 4.33 ± 1.15 | 7.67 ± 0.58 |
| Staphylococcus epidermidis 24.2 | 12.67 ± 1.53 | 3.33 ± 0.58 | 7.33 ± 0.58 | 6.67 ± 0.58 | 9.33 ± 0.58 | 5.33 ± 0.58 | 8.33 ± 0.58 |
| Staphylococcus epidermidis 27.3 | 11.33 ± 1.15 | 4.67 ± 0.58 | 5.67 ± 0.58 | 5.33 ± 0.58 | 8.67 ± 0.58 | 4.67 ± 0.58 | 8.33 ± 0.58 |
| Staphylococcus haemoliticus 2.3 | 12.33 ± 0.58 | 4.67 ± 1.15 | 5.33 ± 0.58 | 10.67 ± 1.15 | 10.33 ± 0.58 | 5.33 ± 0.58 | 8.67 ± 0.58 |
| Staphylococcus haemoliticus 14.5 | 9.33 ± 0.58 | 3.67 ± 1.15 | 5.33 ± 0.58 | 10.33 ± 0.58 | 9.00 ± 1.00 | 4.00 ± 1.00 | 7.33 ± 0.58 |
| Staphylococcus haemoliticus 14.6 | 9.33 ± 1.15 | 3.33 ± 0.58 | 6.33 ± 0.58 | 11.00 ± 1.00 | 8.33 ± 0.58 | 4.67 ± 0.58 | 7.00 ± 1.73 |
| Staphylococcus haemoliticus 14.7 | 9.67 ± 1.15 | 4.67 ± 1.15 | 5.67 ± 1.15 | 11.33 ± 1.15 | 9.33 ± 1.15 | 5.00 ± 1.00 | 7.33 ± 0.58 |
| Staphylococcus haemoliticus 14.8 | 9.33 ± 1.53 | 4.67 ± 0.58 | 5.67 ± 0.58 | 10.33 ± 2.08 | 9.67 ± 1.15 | 4.67 ± 0.58 | 6.33 ± 0.58 |
| Staphylococcus haemoliticus 17.1 | 10.67 ± 1.15 | 3.67 ± 0.58 | 5.67 ± 1.53 | 12.33 ± 0.58 | 8.33 ± 1.53 | 4.67 ± 1.15 | 7.67 ± 1.53 |
| Staphylococcus haemoliticus 17.2 | 10.00 ± 1.73 | 3.67 ± 0.58 | 5.33 ± 0.58 | 10.67 ± 0.58 | 10.00 ± 2.00 | 5.00 ± 0.00 | 6.33 ± 0.58 |
| Staphylococcus haemoliticus 17.3 | 10.33 ± 1.53 | 4.33 ± 0.58 | 5.33 ± 1.15 | 11.67 ± 0.58 | 9.67 ± 1.53 | 5.50 ± 0.50 | 8.33 ± 0.58 |
| Staphylococcus haemoliticus 17.5 | 8.00 ± 1.00 | 4.67 ± 0.58 | 6.33 ± 0.58 | 12.67 ± 1.15 | 8.33 ± 0.58 | 4.67 ± 0.58 | 8.33 ± 1.53 |
| Staphylococcus haemoliticus 17.6 | 6.67 ± 1.53 | 4.33 ± 0.58 | 5.67 ± 0.58 | 11.33 ± 1.15 | 9.00 ± 1.00 | 5.17 ± 0.76 | 8.67 ± 0.58 |
| Staphylococcus haemoliticus 19.7 | 6.33 ± 1.15 | 3.33 ± 1.15 | 6.33 ± 0.58 | 9.33 ± 1.15 | 7.67 ± 0.58 | 5.67 ± 1.15 | 7.67 ± 0.58 |
| Staphylococcus haemoliticus 19.8 | 7.33 ± 0.58 | 4.33 ± 1.15 | 5.67 ± 0.58 | 10.67 ± 0.58 | 8.33 ± 0.58 | 5.33 ± 0.58 | 6.67 ± 1.15 |
| Staphylococcus haemoliticus 20.2 | 6.67 ± 1.15 | 3.67 ± 1.15 | 6.33 ± 1.15 | 10.33 ± 2.08 | 9.33 ± 1.15 | 3.67 ± 0.58 | 6.67 ± 0.58 |
| Staphylococcus haemoliticus 20.4 | 8.33 ± 1.15 | 4.00 ± 0.00 | 6.00 ± 1.73 | 10.67 ± 1.15 | 10.67 ± 1.53 | 6.00 ± 1.00 | 5.33 ± 0.58 |
| Staphylococcus haemoliticus 20.5 | 8.67 ± 0.58 | 3.67 ± 1.15 | 5.33 ± 0.58 | 12.33 ± 0.58 | 10.67 ± 0.58 | 4.67 ± 0.58 | 5.67 ± 0.58 |
| Staphylococcus haemoliticus 21.5 | 8.33 ± 0.58 | 3.83 ± 0.76 | 6.67 ± 1.53 | 11.67 ± 0.58 | 10.67 ± 1.15 | 5.33 ± 1.15 | 4.66 ± 1.15 |
| Staphylococcus haemoliticus 21.6 | 9.33 ± 0.58 | 4.33 ± 0.58 | 8.67 ± 0.58 | 11.33 ± 1.15 | 9.00 ± 1.00 | 4.67 ± 0.58 | 6.33 ± 1.15 |
| Staphylococcus haemoliticus 21.7 | 8.00 ± 1.73 | 4.33 ± 0.58 | 8.67 ± 1.15 | 11.33 ± 0.58 | 10.67 ± 1.15 | 5.33 ± 0.58 | 6.67 ± 1.15 |
| Staphylococcus haemoliticus 22.5 | 7.33 ± 0.58 | 3.67 ± 0.58 | 8.33 ± 1.15 | 10.67 ± 1.15 | 9.00 ± 1.00 | 5.00 ± 1.73 | 6.33 ± 0.58 |
| Staphylococcus haemoliticus 24.1 | 10.00 ± 1.00 | 4.33 ± 0.58 | 8.00 ± 1.00 | 10.67 ± 0.58 | 9.00 ± 1.73 | 5.00 ± 0.87 | 7.00 ± 1.73 |
| Staphylococcus haemoliticus 24.2 | 10.33 ± 1.53 | 4.67 ± 0.58 | 8.67 ± 1.15 | 10.67 ± 1.15 | 9.00 ± 1.00 | 5.33 ± 0.58 | 6.33 ± 0.58 |
| Staphylococcus haemoliticus 24.5 | 9.67 ± 1.15 | 4.67 ± 1.15 | 8.33 ± 1.15 | 12.67 ± 1.15 | 10.67 ± 1.15 | 5.67 ± 1.15 | 7.33 ± 0.58 |
| Staphylococcus haemoliticus 24.6 | 7.67 ± 0.58 | 4.67 ± 0.58 | 9.67 ± 0.58 | 10.67 ± 0.58 | 9.33 ± 1.15 | 5.33 ± 0.58 | 6.67 ± 1.15 |
| Staphylococcus haemoliticus 24.7 | 8.00 ± 1.00 | 5.67 ± 0.58 | 8.33 ± 0.58 | 12.33 ± 0.58 | 9.33 ± 1.53 | 4.33 ± 0.58 | 6.67 ± 1.53 |
| Staphylococcus haemoliticus 24.8 | 8.33 ± 0.58 | 4.33 ± 0.58 | 9.33 ± 0.58 | 10.67 ± 0.58 | 8.67 ± 1.15 | 4.67 ± 0.58 | 5.67 ± 0.58 |
| Staphylococcus haemoliticus | 6.67 ± 0.58 | 4.67 ± 0.58 | 8.67 ± 1.15 | 12.67 ± 1.15 | 9.67 ± 0.58 | 5.33 ± 0.58 | 5.33 ± 0.58 |
| Staphylococus hominis 3.1 | 21.33 ± 1.15 | 6.67 ± 0.58 | 15.33 ± 0.58 | 8.67 ± 1.15 | 8.33 ± 0.58 | 7.67 ± 0.58 | 10.67 ± 1.15 |
| Staphylococus hominis 3.2 | 20.67 ± 0.58 | 5.67 ± 0.58 | 14.33 ± 0.58 | 8.33 ± 0.58 | 7.33 ± 0.58 | 6.67 ± 0.58 | 11.33 ± 0.58 |
| Staphylococus hominis 3.3 | 19.33 ± 0.58 | 6.33 ± 1.15 | 15.33 ± 0.58 | 10.33 ± 0.58 | 8.33 ± 0.58 | 7.67 ± 0.58 | 11.67 ± 0.58 |
| Staphylococus hominis 3.4 | 21.00 ± 1.73 | 6.67 ± 1.15 | 14.33 ± 0.58 | 10.67 ± 1.15 | 7.67 ± 0.58 | 8.67 ± 0.58 | 11.67 ± 1.53 |
| Staphylococus hominis 3.5 | 21.67 ± 1.15 | 5.67 ± 0.58 | 13.33 ± 0.58 | 9.67 ± 0.58 | 7.67 ± 1.15 | 7.67 ± 0.58 | 11.67 ± 0.58 |
| Staphylococus hominis 3.7 | 20.67 ± 1.15 | 5.33 ± 1.53 | 14.33 ± 0.58 | 12.33 ± 0.58 | 8.33 ± 0.58 | 7.67 ± 0.58 | 12.33 ± 0.58 |
| Staphylococus hominis 14.4 | 21.67 ± 0.58 | 4.67 ± 0.58 | 13.67 ± 1.53 | 10.33 ± 0.58 | 7.67 ± 0.58 | 8.33 ± 0.58 | 12.67 ± 1.15 |
| Staphylococus hominis 16.1 | 22.67 ± 1.15 | 5.67 ± 0.58 | 11.33 ± 1.15 | 12.67 ± 1.15 | 6.67 ± 1.15 | 6.67 ± 1.15 | 11.33 ± 1.15 |
| Staphylococus hominis 16.4 | 20.33 ± 1.15 | 6.67 ± 0.58 | 14.33 ± 0.58 | 10.33 ± 1.15 | 6.33 ± 0.58 | 7.33 ± 0.58 | 10.33 ± 0.58 |
| Staphylococus hominis 17.4 | 22.33 ± 0.58 | 6.33 ± 0.58 | 12.67 ± 1.15 | 11.33 ± 1.15 | 5.33 ± 1.15 | 8.67 ± 0.58 | 10.67 ± 0.58 |
| Staphylococus hominis 18.1 | 22.67 ± 0.58 | 6.00 ± 1.00 | 11.33 ± 1.15 | 9.33 ± 0.58 | 6.33 ± 1.15 | 7.33 ± 0.58 | 9.33 ± 0.58 |
| Staphylococus hominis 18.8 | 19.33 ± 0.58 | 7.00 ± 1.73 | 11.67 ± 1.15 | 11.67 ± 1.53 | 5.67 ± 1.15 | 8.67 ± 0.58 | 11.33 ± 0.58 |
| Staphylococus hominis 21.1 | 18.67 ± 0.58 | 6.33 ± 0.58 | 12.67 ± 0.50 | 13.67 ± 1.53 | 7.33 ± 1.15 | 6.33 ± 1.53 | 11.67 ± 0.58 |
| Staphylococus hominis 21.2 | 18.33 ± 0.58 | 7.67 ± 0.58 | 12.00 ± 1.73 | 11.33 ± 1.53 | 6.33 ± 0.58 | 7.00 ± 1.73 | 12.33 ± 0.58 |
| Staphylococus hominis 27.4 | 19.00 ± 1.73 | 7.67 ± 1.15 | 11.67 ± 0.58 | 12.67 ± 0.58 | 7.33 ± 0.58 | 8.33 ± 0.58 | 12.33 ± 0.58 |
| Microorganism/EOs | 1. | 2. | 3. | 4. | 5. | 6. | 7. |
|---|---|---|---|---|---|---|---|
| Stapyloccocus aureus 18.3 | 1.56 | 1.56 | 0.39 | 25.00 | 0.39 | 3.12 | 12.50 |
| Staphyloccous capitis 3.6 | 1.56 | 3.12 | 0.78 | 25.00 | 1.56 | 12.50 | 12.50 |
| Staphylococcus epidermidis 2.2 | 3.12 | 1.56 | 0.78 | 12.50 | 3.12 | 3.12 | 25.00 |
| Staphylococcus epidermidis 2.4 | 3.12 | 1.56 | 0.78 | 25.00 | 3.12 | 3.12 | 25.00 |
| Staphylococcus epidermidis 16.2 | 3.12 | 1.56 | 0.39 | 25.00 | 3.12 | 3.12 | 25.00 |
| Staphylococcus epidermidis 18.4 | 3.12 | 1.56 | 1.56 | 25.00 | 3.12 | 3.12 | 25.00 |
| Staphylococcus epidermidis 19.5 | 1.56 | 1.56 | 0.78 | 25.00 | 3.12 | 3.12 | 25.00 |
| Staphylococcus epidermidis 24.2 | 3.12 | 1.56 | 1.56 | 25.00 | 3.12 | 3.12 | 25.00 |
| Staphylococcus epidermidis 27.3 | 3.12 | 1.56 | 0.78 | 25.00 | 3.12 | 3.12 | 25.00 |
| Staphylococcus haemoliticus 2.3 | 6.25 | 6.25 | 0.78 | 25.00 | 12.50 | 6.25 | 25.00 |
| Staphylococcus haemoliticus 14.5 | 6.25 | 6.25 | 1.56 | 25.00 | 12.50 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 14.6 | 3.12 | 6.25 | 1.56 | 25.00 | 12.50 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 14.7 | 12.50 | 6.25 | 0.78 | 3.12 | 12.50 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 14.8 | 3.12 | 6.25 | 1.56 | 3.12 | 12.50 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 17.1 | 3.12 | 3.12 | 1.56 | 25.00 | 12.50 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 17.2 | 3.12 | 3.12 | 1.56 | 25.00 | 12.50 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 17.3 | 3.12 | 6.25 | 1.56 | 25.00 | 12.50 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 17.5 | 1.56 | 6.25 | 1.56 | 25.00 | 6.25 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 17.6 | 3.12 | 6.25 | 0.78 | 25.00 | 6.25 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 19.7 | 1.56 | 6.25 | 1.56 | 25.00 | 6.25 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 19.8 | 1.56 | 3.12 | 1.56 | 25.00 | 6.25 | 12.50 | 12.50 |
| Staphylococcus haemoliticus 20.2 | 6.25 | 3.12 | 0.78 | 25.00 | 12.50 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 20.4 | 6.25 | 6.25 | 1.56 | 25.00 | 12.50 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 20.5 | 1.56 | 6.25 | 1.56 | 25.00 | 25.00 | 12.50 | 12.50 |
| Staphylococcus haemoliticus 21.5 | 1.56 | 6.25 | 0.78 | 25.00 | 12.50 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 21.6 | 3.12 | 6.25 | 1.56 | 25.00 | 12.50 | 12.50 | 12.50 |
| Staphylococcus haemoliticus 21.7 | 6.25 | 3.12 | 1.56 | 25.00 | 25.00 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 22.5 | 6.25 | 6.25 | 1.56 | 25.00 | 25.00 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 24.1 | 3.12 | 1.56 | 1.56 | 25.00 | 12.50 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 24.2 | 3.12 | 1.56 | 1.56 | 25.00 | 12.50 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 24.5 | 1.56 | 3.12 | 1.56 | 25.00 | 12.50 | 12.50 | 25.00 |
| Staphylococcus haemoliticus 24.6 | 1.56 | 3.12 | 1.56 | 25.00 | 12.50 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 24.7 | 1.56 | 3.12 | 1.56 | 25.00 | 12.50 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 24.8 | 1.56 | 3.12 | 1.56 | 25.00 | 12.50 | 25.00 | 25.00 |
| Staphylococcus haemoliticus | 1.56 | 1.56 | 0.78 | 25.00 | 12.50 | 12.50 | 25.00 |
| Staphylococus hominis 3.1 | 1.56 | 1.56 | 0.78 | 12.50 | 3.12 | 12.50 | 25.00 |
| Staphylococus hominis 3.2 | 3.12 | 1.56 | 0.78 | 12.50 | 3.12 | 12.50 | 25.00 |
| Staphylococus hominis 3.3 | 6.25 | 1.56 | 0.78 | 12.50 | 3.12 | 12.50 | 25.00 |
| Staphylococus hominis 3.4 | 3.12 | 3.12 | 0.78 | 12.50 | 3.12 | 12.50 | 25.00 |
| Staphylococus hominis 3.5 | 3.12 | 3.12 | 0.78 | 12.50 | 1.56 | 12.50 | 25.00 |
| Staphylococus hominis 3.7 | 3.12 | 1.56 | 1.56 | 12.50 | 0.78 | 12.50 | 25.00 |
| Staphylococus hominis 14.4 | 3.12 | 3.12 | 0.78 | 12.50 | 1.56 | 12.50 | 25.00 |
| Staphylococus hominis 16.1 | 3.12 | 3.12 | 1.56 | 6.25 | 1.56 | 12.50 | 25.00 |
| Staphylococus hominis 16.4 | 3.12 | 3.12 | 0.78 | 12.50 | 3.12 | 12.50 | 25.00 |
| Staphylococus hominis 17.4 | 1.56 | 3.12 | 0.78 | 25.00 | 3.12 | 12.50 | 25.00 |
| Staphylococus hominis 18.1 | 1.56 | 3.12 | 0.78 | 25.00 | 3.12 | 12.50 | 25.00 |
| Staphylococus hominis 18.8 | 3.12 | 3.12 | 0.78 | 12.50 | 1.56 | 12.50 | 25.00 |
| Staphylococus hominis 21.1 | 3.12 | 3.12 | 0.78 | 12.50 | 1.56 | 12.50 | 25.00 |
| Staphylococus hominis 21.2 | 3.12 | 3.12 | 0.78 | 25.00 | 1.56 | 12.50 | 25.00 |
| Staphylococus hominis 27.4 | 3.12 | 6.25 | 0.39 | 25.00 | 3.12 | 12.50 | 25.00 |
| Name of bacteria/EOs | 8. | 9. | 10. | 11. | 12. | 13. | 14. |
|---|---|---|---|---|---|---|---|
| Stapyloccocus aureus 18.3 | 0.39 | 25.00 | 3.12 | 3.12 | 3.12 | 12.50 | 3.12 |
| Staphyloccous capitis 3.6 | 0.39 | 25.00 | 6.25 | 3.12 | 3.12 | 6.25 | 3.12 |
| Staphylococcus epidermidis 2.2 | 1.56 | 25.00 | 12.50 | 6.25 | 6.25 | 12.50 | 25.00 |
| Staphylococcus epidermidis 2.4 | 1.56 | 25.00 | 12.50 | 6.25 | 6.25 | 12.50 | 25.00 |
| Staphylococcus epidermidis 16.2 | 1.56 | 25.00 | 12.50 | 6.25 | 6.25 | 12.50 | 25.00 |
| Staphylococcus epidermidis 18.4 | 1.56 | 25.00 | 12.50 | 6.25 | 6.25 | 12.50 | 25.00 |
| Staphylococcus epidermidis 19.5 | 1.56 | 25.00 | 12.50 | 6.25 | 6.25 | 12.50 | 12.50 |
| Staphylococcus epidermidis 24.2 | 1.56 | 25.00 | 12.50 | 6.25 | 6.25 | 12.50 | 12.50 |
| Staphylococcus epidermidis 27.3 | 1.56 | 25.00 | 12.50 | 6.25 | 6.25 | 12.50 | 12.50 |
| Staphylococcus haemoliticus 2.3 | 1.56 | 25.00 | 12.50 | 3.12 | 3.12 | 12.50 | 12.50 |
| Staphylococcus haemoliticus 14.5 | 3.12 | 25.00 | 12.50 | 3.12 | 3.12 | 12.50 | 12.50 |
| Staphylococcus haemoliticus 14.6 | 3.12 | 25.00 | 12.50 | 3.12 | 3.12 | 12.50 | 12.50 |
| Staphylococcus haemoliticus 14.7 | 3.12 | 25.00 | 12.50 | 3.12 | 3.12 | 12.50 | 12.50 |
| Staphylococcus haemoliticus 14.8 | 3.12 | 25.00 | 12.50 | 3.12 | 3.12 | 12.50 | 12.50 |
| Staphylococcus haemoliticus 17.1 | 3.12 | 25.00 | 12.50 | 3.12 | 3.12 | 12.50 | 12.50 |
| Staphylococcus haemoliticus 17.2 | 3.12 | 25.00 | 12.50 | 3.12 | 3.12 | 12.50 | 12.50 |
| Staphylococcus haemoliticus 17.3 | 3.12 | 25.00 | 12.50 | 3.12 | 3.12 | 12.50 | 12.50 |
| Staphylococcus haemoliticus 17.5 | 6.25 | 25.00 | 12.50 | 3.12 | 3.12 | 25.00 | 12.50 |
| Staphylococcus haemoliticus 17.6 | 6.25 | 25.00 | 12.50 | 3.12 | 3.12 | 25.00 | 12.50 |
| Staphylococcus haemoliticus 19.7 | 6.25 | 25.00 | 12.50 | 3.12 | 6.25 | 25.00 | 12.50 |
| Staphylococcus haemoliticus 19.8 | 6.25 | 25.00 | 12.50 | 3.12 | 6.25 | 25.00 | 12.50 |
| Staphylococcus haemoliticus 20.2 | 6.25 | 25.00 | 12.50 | 3.12 | 6.25 | 25.00 | 12.50 |
| Staphylococcus haemoliticus 20.4 | 6.25 | 25.00 | 12.50 | 3.12 | 3.12 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 20.5 | 6.25 | 25.00 | 12.50 | 3.12 | 3.12 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 21.5 | 6.25 | 25.00 | 12.50 | 3.12 | 3.12 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 21.6 | 6.25 | 25.00 | 6.25 | 3.12 | 3.12 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 21.7 | 6.25 | 25.00 | 6.25 | 3.12 | 3.12 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 22.5 | 6.25 | 25.00 | 6.25 | 3.12 | 3.12 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 24.1 | 3.12 | 25.00 | 6.25 | 3.12 | 3.12 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 24.2 | 3.12 | 25.00 | 6.25 | 3.12 | 3.12 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 24.5 | 3.12 | 25.00 | 6.25 | 3.12 | 3.12 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 24.6 | 6.25 | 25.00 | 6.25 | 3.12 | 3.12 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 24.7 | 6.25 | 25.00 | 6.25 | 3.12 | 3.12 | 25.00 | 25.00 |
| Staphylococcus haemoliticus 24.8 | 6.25 | 25.00 | 6.25 | 3.12 | 3.12 | 25.00 | 25.00 |
| Staphylococcus haemoliticus | 6.25 | 25.00 | 6.25 | 3.12 | 3.12 | 25.00 | 25.00 |
| Staphylococus hominis 3.1 | 0.78 | 12.50 | 3.12 | 6.25 | 3.12 | 6.25 | 3.12 |
| Staphylococus hominis 3.2 | 0.78 | 12.50 | 3.12 | 6.25 | 6.25 | 6.25 | 3.12 |
| Staphylococus hominis 3.3 | 0.78 | 12.50 | 3.12 | 3.12 | 3.12 | 6.25 | 3.12 |
| Staphylococus hominis 3.4 | 0.78 | 12.50 | 3.12 | 3.12 | 3.12 | 6.25 | 3.12 |
| Staphylococus hominis 3.5 | 0.78 | 25.00 | 3.12 | 3.12 | 3.12 | 6.25 | 3.12 |
| Staphylococus hominis 3.7 | 0.78 | 25.00 | 3.12 | 3.12 | 3.12 | 6.25 | 3.12 |
| Staphylococus hominis 14.4 | 0.78 | 25.00 | 3.12 | 3.12 | 3.12 | 6.25 | 3.12 |
| Staphylococus hominis 16.1 | 0.78 | 25.00 | 3.12 | 3.12 | 3.12 | 6.25 | 3.12 |
| Staphylococus hominis 16.4 | 0.78 | 12.50 | 3.12 | 3.12 | 3.12 | 6.25 | 3.12 |
| Staphylococus hominis 17.4 | 0.78 | 12.50 | 3.12 | 3.12 | 3.12 | 6.25 | 3.12 |
| Staphylococus hominis 18.1 | 0.78 | 12.50 | 3.12 | 6.25 | 3.12 | 6.25 | 3.12 |
| Staphylococus hominis 18.8 | 0.78 | 12.50 | 3.12 | 3.12 | 3.12 | 6.25 | 3.12 |
| Staphylococus hominis 21.1 | 0.78 | 12.50 | 3.12 | 3.12 | 6.25 | 6.25 | 3.12 |
| Staphylococus hominis 21.2 | 0.78 | 12.50 | 3.12 | 3.12 | 6.25 | 6.25 | 3.12 |
| Staphylococus hominis 27.4 | 0.78 | 12.50 | 3.12 | 3.12 | 6.25 | 6.25 | 3.12 |
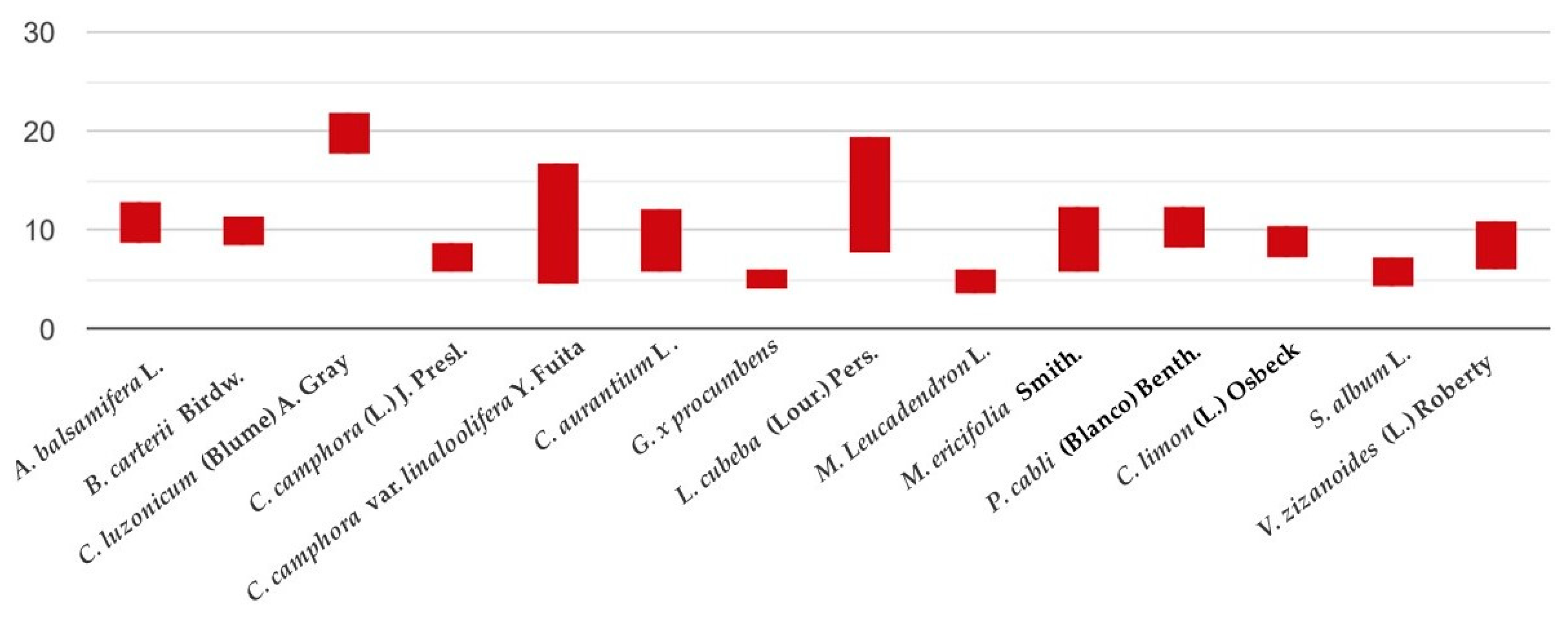
| Essential Oil | Average/Standard Deviation/Statistical Difference |
|---|---|
| A. balsamifera L. | 10.82 ± 2.09 a |
| B. carterii Birdw. | 9.95 ± 1.64 b,a |
| C. luzonicum (Blume) A. Gray | 19.84 ± 1.94 c,a,b |
| C. camphora (L.) J. Presl. | 7.18 ± 1.60 d,a,b,c |
| C. camphora var. linaloolifera Y. Fuita | 10.65 ± 6.30 e,c,d |
| C. x aurantium L. | 8.84 ± 3.33 f,a,b,c,d,e |
| G. procumbens L. | 5.07 ± 1.13 g,a,b,c,d,e,f |
| L. cubeba (Lour.) Pers. | 13.54 ± 5.90 h,a,b,c,d,e,g |
| M. leucadendron L. | 4.82 ± 1.34 i,a,b,c,d,e,f,h |
| M. ericifolia Smith. | 8.93 ± 3.40 j,a,b,c,d,e,g,h,i |
| P. cabli (Blanco) Benth. | 10.29 ± 2.20 k,c,d,g,h,i,j |
| C. limon (L.) Osbeck | 8.71 ± 1.66 l,a,b,c,d,e,g,h,i,k |
| S. album L. | 5.81 ± 1.53 m,a,b,c,d,e,g,h,i,j,k,l |
| V. zizanoides (L.) Roberty | 8.47 ± 2.49 n,a,b,c,d,e,g,h,i,k,m |
| Botanical Species | Common Name | Family | Part |
|---|---|---|---|
| Amyris balsamifera L. | amyris | Rutaceae | crushed wood |
| Boswellia carterii Birdw. | frankincense | Burseraceae | resin |
| Canarium luzonicum (Blume) A. Gray | elemi | Burseraceae | resin |
| Cinnamomum camphora (L.) J. Presl. | camphor three bark | Lauraceae | wood, branches |
| Cinnamomum camphora var. linaloolifera Y. Fuita | ho leaf | Lauraceae | leaves |
| Citrus x aurantium L. | petitgrain | Rutaceae | leaves |
| Gaultheria procumbens L. | wintergreen | Ericaceae | leaves |
| Litsea cubeba (Lour.) Pers. | litsea cubeba fruit | Lauraceae | fruits |
| Melaleuca leucadendron L. | cajeput | Myrtaceae | shoots of leaves |
| Melaleuca ericifolia Smith. | rosalina | Myrtaceae | branches |
| Pogostemon cabli (Blanco) Benth. | patchouli | Lamiaceae | fermented leaves |
| Citrus limon (L.) Osbeck | lemon | Rutaceae | fruits |
| Santalum album L. | sandalwood | Santalaceae | crushed wood |
| Vetiveria zizanoides (L.) Roberty | vetiver | Poaceae | dried roots |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kačániová, M.; Terentjeva, M.; Štefániková, J.; Žiarovská, J.; Savitskaya, T.; Grinshpan, D.; Kowalczewski, P.Ł.; Vukovic, N.; Tvrdá, E. Chemical Composition and Antimicrobial Activity of Selected Essential Oils against Staphylococcus spp. Isolated from Human Semen. Antibiotics 2020, 9, 765. https://0-doi-org.brum.beds.ac.uk/10.3390/antibiotics9110765
Kačániová M, Terentjeva M, Štefániková J, Žiarovská J, Savitskaya T, Grinshpan D, Kowalczewski PŁ, Vukovic N, Tvrdá E. Chemical Composition and Antimicrobial Activity of Selected Essential Oils against Staphylococcus spp. Isolated from Human Semen. Antibiotics. 2020; 9(11):765. https://0-doi-org.brum.beds.ac.uk/10.3390/antibiotics9110765
Chicago/Turabian StyleKačániová, Miroslava, Margarita Terentjeva, Jana Štefániková, Jana Žiarovská, Tatsiana Savitskaya, Dmitrij Grinshpan, Przemysław Łukasz Kowalczewski, Nenad Vukovic, and Eva Tvrdá. 2020. "Chemical Composition and Antimicrobial Activity of Selected Essential Oils against Staphylococcus spp. Isolated from Human Semen" Antibiotics 9, no. 11: 765. https://0-doi-org.brum.beds.ac.uk/10.3390/antibiotics9110765









