Peer Mentoring as a Tool for Developing Soft Skills in Clinical Practice: A 3-Year Study
Abstract
:1. Introduction
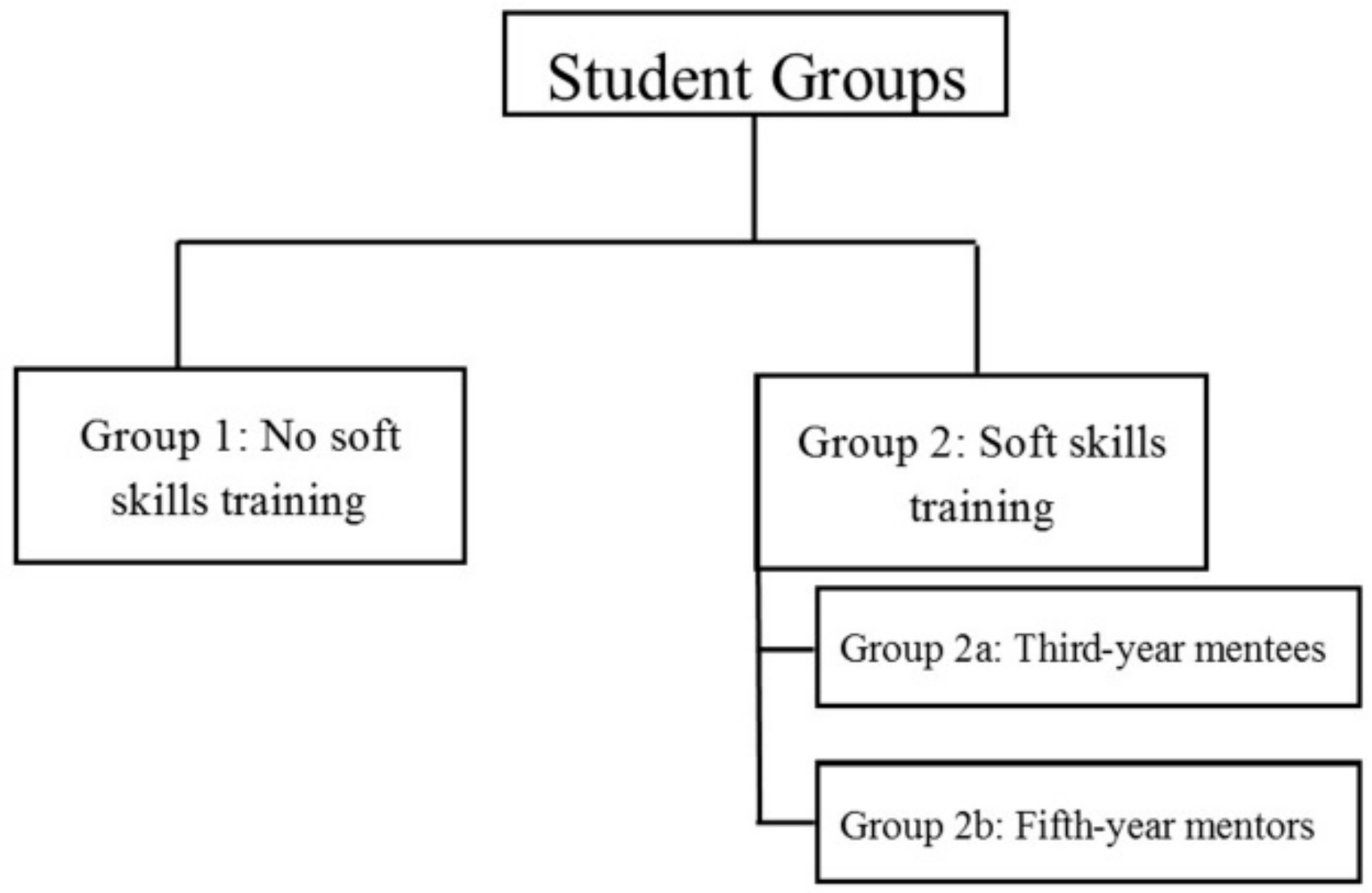
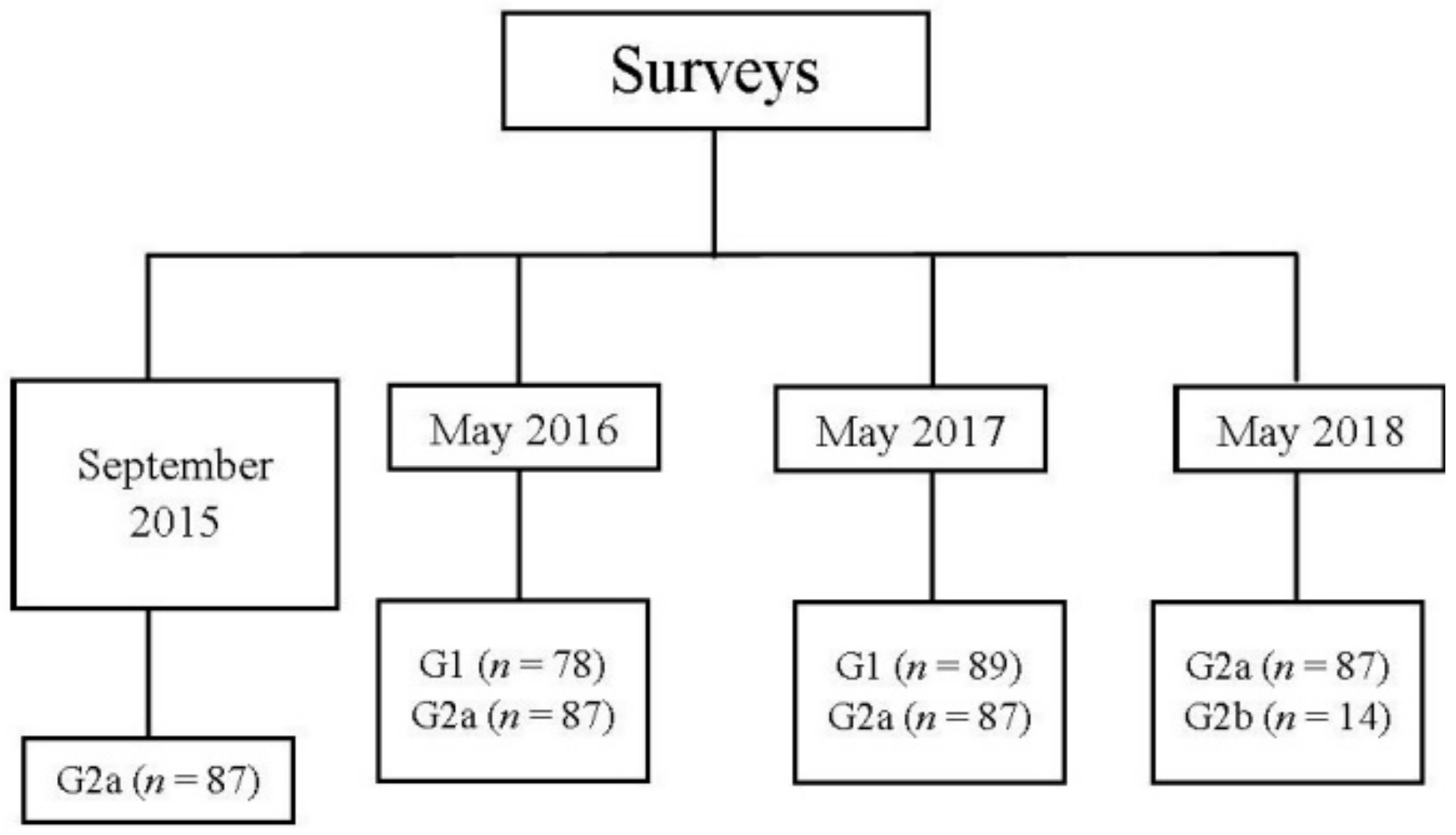
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Succi, C.; Canovi, M. Soft skills to enhance graduate employability: Comparing students and employers’ Perceptions. Stud. High. Educ. 2020, 45, 1834–1847. [Google Scholar] [CrossRef]
- Dalaya, M.; Ishaquddin, S.; Ghadage, M.; Hatte, G. An interesting review on soft skills and dental practice. J. Clin. Diagn. Res. 2015, 9, ZE19–ZE21. [Google Scholar] [CrossRef]
- Bisquerra Alzina, R.; Pérez Escoda, N. Emotional competences. Educ. XX1 2007, 10, 61–82. [Google Scholar]
- Flin, R.; Patey, R.; Glavin, R.; Maran, N. Anaesthetists’ non-technical skills. Br. J. Anaesth. 2010, 105, 38–44. [Google Scholar] [CrossRef] [Green Version]
- Nicolaides, M.; Cardillo, L.; Theodoulou, I.; Hanrahan, J.; Tsoulfas, G.; Athanasiou, T.; Papalois, A.; Sideris, M. Developing a novel framework for non-technical skills learning strategies for undergraduates: A systematic review. Ann. Med. Surg. 2018, 36, 29–40. [Google Scholar] [CrossRef]
- Gonzalez, M.A.; Abu Kasim, N.H.; Naimie, Z. Soft skills and dental education. Eur. J. Dent. Educ. 2013, 17, 73–82. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Salovey, P.; Mayer, J.D. Emotional intelligence. Imagin. Cogn. Personal. 1990, 9, 185–211. [Google Scholar] [CrossRef]
- Victoroff, K.Z.; Boyatzis, R.E. What is the relationship between emotional intelligence and dental student clinical performance? J. Dent. Educ. 2013, 77, 416–426. [Google Scholar] [CrossRef] [PubMed]
- Alzahem, A.M.; van der Molen, H.T.; Alaujan, A.H.; Schmidt, H.G.; Zamakhshary, M.H. Stress amongst dental students: A systematic review. Eur. J. Dent. Educ. 2011, 15, 8–18. [Google Scholar] [CrossRef] [PubMed]
- Carey, J.A.; Madill, A.; Manogue, M. Communications skills in dental education: A systematic research review. Eur. J. Dent. Educ. 2010, 14, 69–78. [Google Scholar] [CrossRef] [PubMed]
- Hannah, A.; Lim, B.T.; Ayers, K.M. Emotional intelligence and clinical interview performance of dental students. J. Dent. Educ. 2009, 73, 1107–1117. [Google Scholar] [CrossRef] [PubMed]
- Neumann, M.; Edelhäuser, F.; Tauschel, D.; Fischer, M.R.; Wirtz, M.; Woopen, C.; Haramati, A.; Scheffer, C. Empathy decline and its reasons: A systematic review of studies with medical students and residents. Acad. Med. 2011, 86, 996–1009. [Google Scholar] [CrossRef]
- Quieng, M.C.; Lim, P.P.; Lucas, M.R.D. 21st century-based Soft Skills: Spotlight on non-cognitive skills in a cognitive-laden dentistry Program. Eur. J. Contemp. Educ. 2015, 11, 72–81. [Google Scholar] [CrossRef]
- Field, J.C.; Kavadella, A.; Szep, S.; Davies, J.R.; DeLap, E.; Manzanares Cespedes, M.C. The graduating European dentist-domain III: Patient-centred care. Eur. J. Dent. Educ. 2017, 21, 18–24. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- McLoughlin, J.; Zijlstra-Shaw, S.; Davies, J.R.; Field, J.C. The graduating European dentist-domain I: Professionalism. Eur. J. Dent. Educ. 2017, 21, 11–13. [Google Scholar] [CrossRef] [Green Version]
- Field, J.C.; DeLap, E.; Manzanares Cespedes, M.C. The graduating European dentist-domain II: Safe and effective clinical practice. Eur. J. Dent. Educ. 2017, 21, 14–17. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Azimi, S.; AsgharNejad Farid, A.A.; Kharazi Fard, M.J.; Khoei, N. Emotional intelligence of dental students and patient satisfaction. Eur. J. Dent. Educ. 2010, 14, 129–132. [Google Scholar] [CrossRef]
- Lam, L.T.; Kirby, S.L. Is emotional intelligence an advantage? An exploration of the impact of emotional and general intelligence on individual performance. J. Soc. Psychol. 2002, 142, 133–143. [Google Scholar] [CrossRef]
- Romanelli, F.; Cain, J.; Smith, K.M. Emotional intelligence as a predictor of academic and/or professional success. Am. J. Pharm. Educ. 2006, 70, 69. [Google Scholar] [CrossRef]
- Cowpe, J.; Plasschaert, A.; Harzer, W.; Vinkka-Puhakka, H.; Walmsley, A.D. Profile and competences for the graduating European dentist—Update 2009. Eur. J. Dent. Educ 2010, 14, 193–202. [Google Scholar] [CrossRef]
- Friedman, P.K.; Arena, C.; Atchison, K.; Beemsterboer, P.L.; Farsai, P.; Giusti, J.B.; Haden, N.K.; Martin, M.E.; Sanders, C.F., Jr.; Sudzina, M.R.; et al. Report of the ADEA President’s Commission on Mentoring. J. Dent. Educ. 2004, 68, 390–396. [Google Scholar] [CrossRef]
- Gironda, M.W.; Bibb, C.A.; Lefever, K.; Law, C.; Messadi, D. A program to recruit and mentor future academic dentists: Successes and challenges. J. Dent. Educ. 2013, 77, 292–299. [Google Scholar] [CrossRef]
- Wilson, N.H.F.; Verma, M.; Nanda, A. Leadership in recruiting and retaining talent in academic dentistry. J. Dent. 2019, 87, 32–35. [Google Scholar] [CrossRef]
- Bagramian, R.A.; Taichman, R.S.; McCauley, L.; Green, T.G.; Inglehart, M.R. Mentoring of dental and dental hygiene faculty: A case study. J. Dent. Educ. 2011, 75, 291–299. [Google Scholar] [CrossRef]
- Lopez, N.; Johnson, S.; Black, N. Does peer mentoring work? Dental students assess its benefits as an adaptive coping strategy. J. Dent. Educ. 2010, 74, 1197–1205. [Google Scholar] [CrossRef]
- Sinkford, J.C.; Valachovic, R.W. Growing our own: Mentoring in the dental academic pipeline. J. Dent. Educ. 2019, 83, 981–987. [Google Scholar] [CrossRef] [Green Version]
- John, V.; Papageorge, M.; Jahangiri, L.; Wheater, M.; Cappelli, D.; Frazer, R.; Sohn, W. Recruitment, development, and retention of dental faculty in a changing environment. J. Dent. Educ. 2011, 75, 82–89. [Google Scholar] [CrossRef]
- Schrubbe, K.F. Mentorship: A critical component for professional growth and academic success. J. Dent. Educ. 2004, 68, 324–328. [Google Scholar] [CrossRef]
- Zerzan, J.T.; Hess, R.; Schur, E.; Phillips, R.S.; Rigotti, N. Making the most of mentors: A guide for mentees. Acad. Med. 2009, 84, 140–144. [Google Scholar] [CrossRef]
- Abu Kasim, N.H.; Abu Kassim, N.L.; Razak, A.A.A.; Abdullah, H.; Bindal, P.; Che’ Abdul Aziz, Z.A.; Sulaiman, E.; Farook, M.S.; Gonzalez, M.A.; Thong, Y.L.; et al. Pairing as an instructional strategy to promote soft skills amongst clinical dental students. Eur. J. Dent. Educ. 2014, 18, 51–57. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Stewart, R.A.; Hauge, L.S.; Stewart, R.D.; Rosen, R.L.; Charnot-Katsikas, A.; Prinz, R.A.; Association for Surgical Education. A CRASH course in procedural skills improves medical students’ self-assessment of proficiency, confidence, and anxiety. Am. J. Surg. 2007, 193, 771–773. [Google Scholar] [CrossRef]
- Bibb, C.A.; Lefever, K.H. Mentoring future dental educators through an apprentice teaching experience. J. Dent. Educ. 2002, 66, 703–709. [Google Scholar] [CrossRef]
- Schwartz, B.; Saad, M.N.; Goldberg, D. Evaluating the students’ perspectives of a clinic mentoring programme. Eur. J. Dent. Educ. 2014, 18, 115–120. [Google Scholar] [CrossRef]
- Haist, S.A.; Wilson, J.F.; Fosson, S.E.; Brigham, N.L. Are fourth-year medical students effective teachers of the physical examination to first-year medical students? J. Gen. Intern. Med. 1997, 12, 177–181. [Google Scholar] [CrossRef]
- Stenfors-Hayes, T.; Lindgren, L.E.; Tranaeus, S. Perspectives on being a mentor for undergraduate dental students. Eur. J. Dent. Educ. 2011, 15, 153–158. [Google Scholar] [CrossRef] [PubMed]
- Bianchi, S.; Gatto, R.; Fabiani, L. Effects of the SARS-COV-2 pandemic of medical education in Italy: Considerations and tips. Eur. Biomed. J. 2020, 15, 100–101. [Google Scholar]
- Stoopler, E.T.; Tanaka, T.I.; Sollecito, T.P. Hospital-based dental externship during COVID-19 pandemic: Think virtual! Spec. Care Dent. 2020, 40, 393–394. [Google Scholar] [CrossRef]
- Varvara, G.; Bernardi, S.; Bianchi, S.; Sinjari, B.; Piatelli, M. Dental education challenges during the COVID-19 pandemic period in Italy: Undergraduate student feedback, future perspectives, and the needs of teaching strategies for professional development. Healthcare 2021, 9, 454. [Google Scholar] [CrossRef] [PubMed]

| Non-Technical Skills | Characteristics |
|---|---|
| Cognitive self-management | Data collection |
| Analysis | |
| Synthetic thinking | |
| Logical judgment | |
| Reliability | |
| Emotional self-management | Autonomy |
| Mental resistance | |
| Self-confidence | |
| Perseverance | |
| Connection relationship | Empathy |
| Assertiveness | |
| Active listening | |
| Impact relationship | Conflict management |
| Credibility | |
| Communication | |
| Work management | Problem solving |
| Precision | |
| Planning and organizing | |
| Orientation in the objectives |
| Survey Time | Mean (SD) |
|---|---|
| September 2015 | 67.17 (4.23) a |
| May 2016 | 76.38 (3.14) b |
| May 2017 | 78.57 (2.51) bc |
| May 2018 | 81.20 (1.40) c |
| Non-Technical Skills | September 2015 | May 2016 | May 2017 | May 2018 |
|---|---|---|---|---|
| Cognitive self-management | 60.91 | 72.02 | 75.36 | 79.13 |
| Emotional self-management | 67.62 | 76.57 | 76.83 | 81.09 |
| Connection relationship | 72.14 | 80.09 | 81.78 | 83.07 |
| Impact relationship | 69.49 | 78.4 | 79.48 | 81.41 |
| Work management | 65.71 | 74.82 | 79.38 | 81.28 |
| Total | 67.17 | 76.38 | 78.57 | 81.20 |
| Group | Mean (SD) |
|---|---|
| G1 | 76.99 (3.51) a |
| G2a | 81.20 (1.40) b |
| G2b | 83.86 (1.47) b |
| Non-Technical Skills | G1 2016–2017 | G2a May 2018 | G2b May 2018 |
|---|---|---|---|
| Cognitive self-management | 72.01 | 79.13 | 81.89 |
| Emotional self-management | 76.86 | 81.09 | 84.37 |
| Connection relationship | 81.01 | 83.07 | 83.78 |
| Impact relationship | 79.49 | 81.41 | 83.32 |
| Work management | 75.56 | 81.28 | 85.92 |
| Total | 76.99 | 81.20 | 83.86 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lluch, A.M.; Lluch, C.; Arregui, M.; Jiménez, E.; Giner-Tarrida, L. Peer Mentoring as a Tool for Developing Soft Skills in Clinical Practice: A 3-Year Study. Dent. J. 2021, 9, 57. https://0-doi-org.brum.beds.ac.uk/10.3390/dj9050057
Lluch AM, Lluch C, Arregui M, Jiménez E, Giner-Tarrida L. Peer Mentoring as a Tool for Developing Soft Skills in Clinical Practice: A 3-Year Study. Dentistry Journal. 2021; 9(5):57. https://0-doi-org.brum.beds.ac.uk/10.3390/dj9050057
Chicago/Turabian StyleLluch, Antonio M., Clàudia Lluch, María Arregui, Esther Jiménez, and Luis Giner-Tarrida. 2021. "Peer Mentoring as a Tool for Developing Soft Skills in Clinical Practice: A 3-Year Study" Dentistry Journal 9, no. 5: 57. https://0-doi-org.brum.beds.ac.uk/10.3390/dj9050057







